on US orders over $100
on all US orders over $100

Some instances of breast cancer are genetic, part of a syndrome called Hereditary Breast and Ovarian Cancer. Read on to learn how this happens, and how you can investigate your family health history for signs of the syndrome.

Tumor Suppressor Genes: Most inherited breast cancers are caused by mutations, abnormal changes, in two particular genes, BRCA1 and BRCA2 (BReast CAncer genes 1 and 2), having been passed on from a parent. Everyone carries these two tumor suppressor genes, which repair cell damage and maintain proper growth of breast and ovarian cells. Every cell has two copies of every gene, one from each parent. A gene mutation only has to occur in one of these copies to be passed along, meaning that a child has a 50% chance of inheriting a mutated gene from a parent who has one.
Mutations in BRCA1 and 2 are rare; only 1% of the total population is estimated to have them. However, these genes account for 10 to 15% of all breast cancers. While most breast and ovarian cancers occur sporadically, without known cause, the possibility of carrying mutations in these genes should be regarded seriously.
Other Genes: Although tumor suppressor genes make up the bulk of inherited cancers, other genes may be responsible for other incidences, both inherited and sporadic. These include:
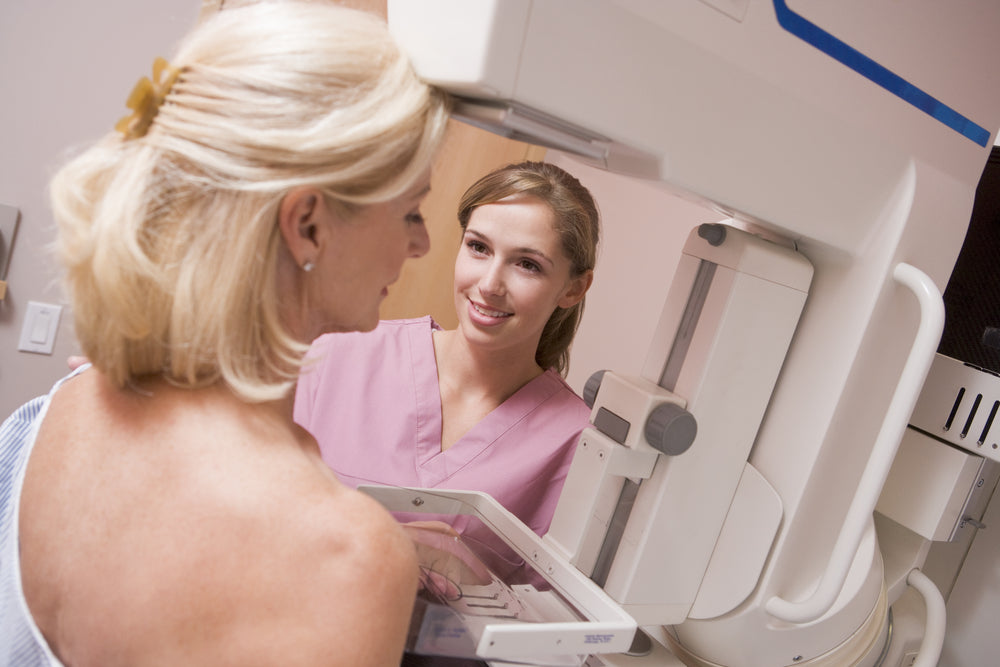
Identifying Risk: The first step in understanding your inherited cancer risk level is a study of your family history, possibly with the guidance of a genetic counselor. Increased incidence of cancer, particularly specific cancers on the same side of the family, may be an indication that genetic testing should be done.
When possible, try to collect the following information about your family's cancer history:
This isn't quite a complete list, as family and personal health circumstances can vary greatly. Any family history of cancer should be looked at closely for unusually high incidence or recurrence, among other atypical occurrences. Knowing your family history is vital in protecting yourself.

Women with mutations associated with hereditary breast cancer face many increased cancer risks compared to other women, including other types such as ovarian cancer. Some of these risks include:
Men with inherited mutations also show increased risk for various cancers, including:
Triple negative breast cancer: Not all breast cancers function or grow in the same way. A triple negative form of breast cancer has cells that test negative for the presence of receptors for the hormones estrogen or progesterone, or for the gene HER2. Estrogen and progesterone do not help these cancers grow; neither does the presence of excessive HER2 receptors. This means that these cancers don't respond to hormonal therapies, or ones that target HER2 receptors. About 10% to 20% of breast cancers are triple negative. This type of breast cancer also can indicate the presence of specific mutations:

Finding out that you have a gene mutation or a family history of breast cancer can be distressing, but you can mitigate the risks of developing a cancer in numerous ways.
Lifestyle Changes: Adopting healthy practices in your lifestyle can reduce the risk of cancer for both those with inherited mutations and family histories, and even those without preexisting risks. Among these changes:
Hormonal Therapy and Other Medications: Medications that lower the production of estrogen or block estrogen receptors reduce the risk of hormone-receptor-positive breast cancer. Additionally, birth control pills may lower the risk in women with abnormal BRCA1 and BRCA2 genes.
Protective Surgery: Prophylactic, or protective, surgery, involves removing most of the breast tissue to prevent cancer from forming in the future. It can also be used on other organs or glands in high-risk patients. This extremely aggressive prevention method can reduce risk of breast cancer by up to 97%. Women with BRCA1 or BRCA2 mutations can also reduce cancer risk by 50% by removing their ovaries or Fallopian tubes before the onset of menopause.
More Frequent Screening: A healthcare professional and genetic counselor are invaluable guides to developing a useful and timely screening schedule, which may include:
A thorough and well-structured screening plan can not only detect cancer early, potentially saving your life, but can also be a strong foundation for coping with the possibility of breast cancer. Learning about an inherited condition can cause anxiety, frustration, and grief. But regular screenings can help reduce these fears, and a close relationship with a doctor, genetic counselor, or other healthcare professional can be an immense source of comfort. The importance of being open about your fears with your doctor cannot be overstated, and managing fear will help you better manage your own health.
Leave a comment