Safe IV Fluid Administration
IV therapy carries inherent risks. Proper selection, preparation, infusion technique, and monitoring minimise complications and maximise safety.
Critical Monitoring During IV Infusion
Vital sign changes — Blood pressure, heart rate, respiratory rate, and oxygen saturation must be assessed before, during, and after IV infusion. Rising blood pressure and heart rate may signal hypervolemia (fluid overload); dropping blood pressure may indicate inadequate resuscitation or fluid extravasation (leakage into surrounding tissue).
Intake and output tracking — Documenting IV fluids given and urine output reveals whether kidneys are responding appropriately. Oliguria (low urine output) despite adequate fluid input may signal acute kidney injury or shock.
Serum electrolytes and osmolality — Lab values confirm that IV fluid choice is correcting rather than worsening electrolyte balance. Hyponatremia correction must be monitored closely to ensure gradual change (not more than 10 mEq/L per 24 hours) and prevent cerebral edema.
Catheter site inspection — Redness, swelling, warmth, or patient pain at the IV site suggests infiltration (fluid leaking into tissue), phlebitis (vein inflammation), or early infection. Sites must be assessed at least every 8 hours and immediately if the patient reports pain.
Colloid infusions require special attention — Patients receiving albumin, hetastarch, or dextran must be monitored for increased blood pressure, dyspnea (shortness of breath), and bounding pulse, which signal hypervolemia. These solutions stay in the bloodstream longer than crystalloids and can cause fluid overload if infused too rapidly.
This product is intended for use by qualified healthcare professionals or under the guidance of a licensed medical provider. It is not a substitute for professional medical advice, diagnosis, or treatment.
Contraindications and Cautions by Solution Type
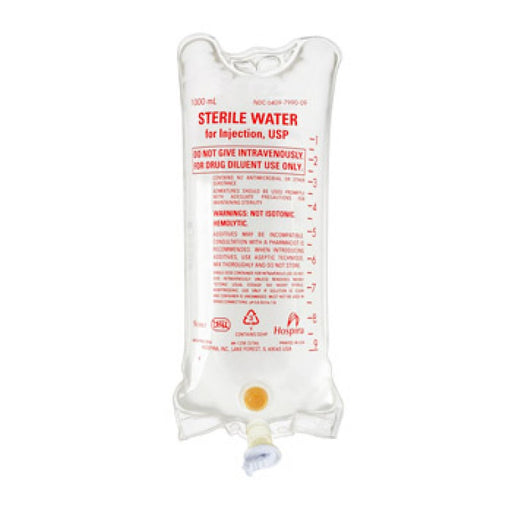
Hypotonic Solutions (0.45% Saline, D5W, Half-Normal Saline)
Contraindicated in:
- Hemorrhagic shock — hypotonic fluid worsens hypovolemia and reduces oxygen delivery
- Head injury or altered mental status — hypotonic fluid can worsen cerebral edema
- Hyperglycemia (in the case of D5W) — dextrose worsens blood glucose in diabetic patients
- Uncontrolled rapid serum sodium correction — can cause osmotic demyelination syndrome
Use with caution in: Patients with SIADH (syndrome of inappropriate antidiuretic hormone) on free water restriction, as hypotonic fluid can dangerously lower serum sodium further.
Hypertonic Solutions (3% Saline, D10W)
Contraindicated in:
- Hypernatremia — worsens serum sodium elevation
- Peripheral IV lines — hypertonic fluid is vesicant and causes tissue necrosis if extravasated; requires central line placement
- Rapid infusion in patients without careful sodium monitoring — can overshoot sodium correction and cause osmotic demyelination
Requires: Central line placement and frequent lab monitoring (every 2–4 hours during active correction). Infusion rates must be controlled to prevent sodium overcorrection.
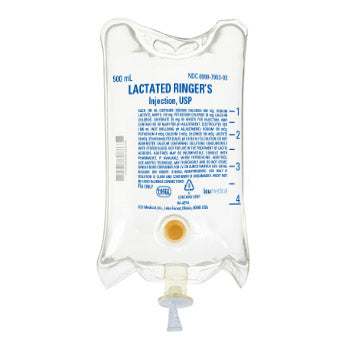
Lactated Ringer's Solution
Contraindicated or used with caution in:
- Severe hyperkalemia — lactate contains potassium (4 mEq/L) and should not be used as primary resuscitation fluid in patients with dangerously elevated serum potassium
- Hepatic failure — lactate metabolism depends on liver function; accumulation can worsen lactic acidosis
- Severe acidosis or certain medications — calcium in LR can precipitate with certain drugs; incompatibility should be checked
Generally preferred for: Trauma, burns, and sepsis where its balanced electrolyte composition and lactate buffering provide advantages over normal saline.
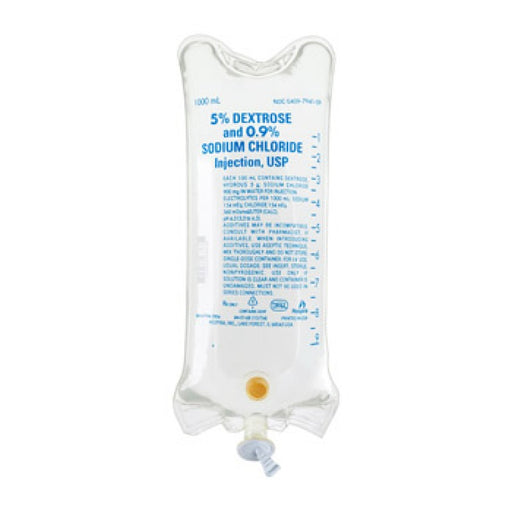
Normal Saline (0.9%)
Contraindicated or used with caution in:
- Hyperchloremic acidosis or chloride-restricted patients — normal saline has high chloride (154 mEq/L) and can worsen metabolic acidosis in large-volume resuscitation
- Patients with baseline metabolic alkalosis — normal saline hyperchloremia can perpetuate alkalosis
Generally safe for: Initial resuscitation, blood transfusions, hyponatremia, and most general IV therapy.
This product is intended for use by qualified healthcare professionals or under the guidance of a licensed medical provider. It is not a substitute for professional medical advice, diagnosis, or treatment.
Common IV Therapy Complications
Infiltration — IV catheter punctures the vein wall, and fluid enters surrounding tissue. Signs: swelling, coolness, and pain at the site. Management: stop infusion immediately, remove catheter, elevate extremity, and apply warm compresses. Extravasation of irritant solutions (potassium, calcium, hypertonic dextrose) can cause tissue necrosis and requires urgent intervention.
Phlebitis — Vein becomes inflamed from mechanical irritation, chemical irritation (acidic or alkaline solutions), or infection. Signs: pain, redness, warmth along the vein. Management: remove catheter, elevate extremity, apply warm compresses. Septic phlebitis (bacteria-caused) requires catheter removal and antibiotics.
Hypervolemia (fluid overload) — Excessive IV fluid causes elevated blood pressure, weight gain, crackles on lung exam, and risk of pulmonary edema (fluid in lungs). Management: slow or stop infusion, elevate head of bed, consider diuretics.
Hypovolemia (inadequate fluid resuscitation) — Insufficient IV fluid leaves the patient in ongoing shock. Signs: tachycardia (fast heart rate), hypotension, altered mental status, decreased urine output. Management: increase infusion rate or switch to more aggressive fluid boluses.
Central line complications — Insertion of central lines carries risks of pneumothorax (collapsed lung), hemothorax (blood in chest cavity), arrhythmias, and catheter-related bloodstream infection (CRBSI). Careful insertion technique, sterile dressing maintenance, and prompt removal when no longer needed reduce risk.
Prevention of Infection and Contamination
IV bags are manufactured as sterile, single-use products. To prevent infection:
- Inspect IV bags for cracks, cloudiness, or particulates before use; discard if damaged
- Use aseptic technique when inserting the IV catheter: hand hygiene, skin antisepsis (alcohol or chlorhexidine), and sterile dressing
- Replace IV dressings if wet, soiled, or loose every 7 days (or per facility protocol)
- Replace peripheral IV catheters every 96 hours to reduce infection risk (though clinical judgment may support earlier replacement if needed)
- Document catheter insertion date and inspect sites regularly for signs of infection
- Remove catheters as soon as no longer needed
Bloodstream infections from contaminated IV fluids or poor catheter care can be life-threatening; prevention through proper technique and monitoring is essential.