Nasopharyngeal Tube (nasal) Airway Tube
A nasopharyngeal airway (NPA) – often called a “nasal trumpet” – is a hollow, flexible tube (usually plastic or soft rubber) inserted through the nose into the nasopharynx to maintain an open airway. It extends past the tongue and soft palate, keeping the airway patent by displacing the tongue and soft tissues that can block air flow. Unlike an oropharyngeal airway (which goes through the mouth), an NPA is placed nasally and generally does not trigger the gag reflex. This makes it useful for patients who are semi-conscious or have a strong gag reflex. In practice, a nasopharyngeal airway is used as a short-term adjunct to improve ventilation – for example, when bag-valve-mask ventilation alone is ineffective or when intubation is being prepared. It is a common emergency and anesthesia tool to “bypass” upper airway obstruction in a breathing patient until a more definitive airway (like endotracheal intubation) can be secured.
Indications (When and why it’s used)
Nasopharyngeal airways are indicated in patients who need help keeping their airway open but cannot tolerate an oropharyngeal airway. Typical uses include:
- Airway obstruction in a semi-conscious patient: If a patient is drowsy or intoxicated and the tongue or soft tissues are falling back to block the airway, an NPA can “beat” this obstruction. It is often used when bag-valve-mask ventilation fails to maintain adequate breathing and when intubation is not yet done.
- Intact gag reflex or clenched jaw: Because NPAs usually do not provoke vomiting or gagging, they are preferred over oral airways when the patient has an intact reflex or cannot open their mouth (for example, in seizure activity or jaw injury).
- Emergency airway adjunct: As a temporary measure in emergencies (trauma, resuscitation, airway compromise), an NPA quickly establishes an airway before definitive measures.
In summary, an NPA is a rescue airway device used to improve oxygenation and ventilation in spontaneously breathing patients who are at risk of airway obstruction (e.g. due to tongue fall-back), particularly when an oropharyngeal airway is inappropriate.
Contraindications and Precautions
Care must be taken with NPAs, as there are situations where they should not be used. Absolute contraindications include any suspicion of basal skull fracture or significant facial/nasal trauma – inserting the tube could injure the brain or circulatory structures. Similarly, patients with known midface fractures, nasal bone fractures, or severe head injuries should never receive an NPA. Relative contraindications (use with caution) include: recent nasal or sinus surgery, large nasal polyps, significant nasal septal deviation, coagulopathy or anticoagulation (because of bleeding risk), and severe sinusitis. In a nutshell, do not use a nasopharyngeal tube if there is any doubt about skull or facial integrity, or if the patient has acute nose pathology.
Potential complications of nasopharyngeal airway placement include:
- Nasal bleeding (epistaxis): Trauma to the nasal mucosa is common, so gentle insertion with lube is essential.
- Nasal or turbinate injury: The tube can fracture delicate nasal bones or turbinates if forced.
- Intracranial placement: In rare cases of unrecognized skull base fracture, the tube can enter the cranial vault (a catastrophic complication).
- Other issues: Improper sizing or placement can cause nasal tissue laceration, sinusitis over time, or even channel oxygen/air into the stomach if pushed too far.
In short, a nasopharyngeal (nasal) airway is a soft plastic/rubber tube inserted through the nose to keep the upper airway open. It is often called a “nasal trumpet” and is especially useful when an oral airway cannot be used (e.g. patient has a gag reflex or clenched jaw). When used correctly and sized/lubricated properly, it helps bypass upper airway obstruction by the tongue, improving ventilation in semi-conscious patients. Clinicians must select the correct length (usually measured from nostril to earlobe or angle of the jaw) and use water-based lubricant. It is a temporary measure – once applied, the patient should be closely monitored and planned for definitive airway management as needed. Always remember the contraindications (skull/facial trauma) and use caution due to bleeding risks
Nasopharyngeal Tubes (Nasal Airways) Types & Sizes
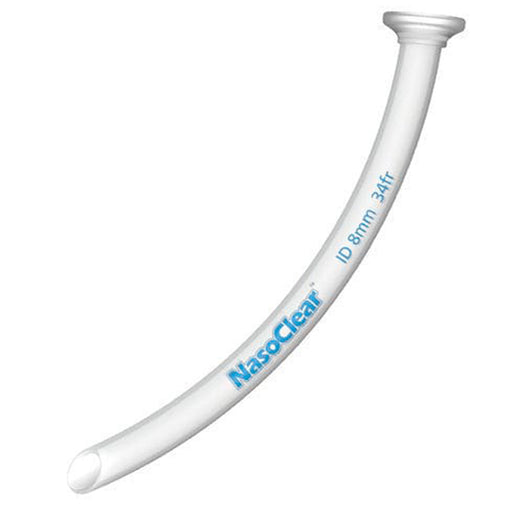
Nasopharyngeal Airway (NPA) – a soft, hollow tube (PVC/silicone or rubber) inserted through the nostril into the posterior pharynx to maintain an open airway. NPAs are often called “nasal trumpets” (or by trade names, e.g. a “Robertazzi” airway). They have a flanged end that prevents over-insertion; the distal tip is beveled and curved to follow the nasal passage.
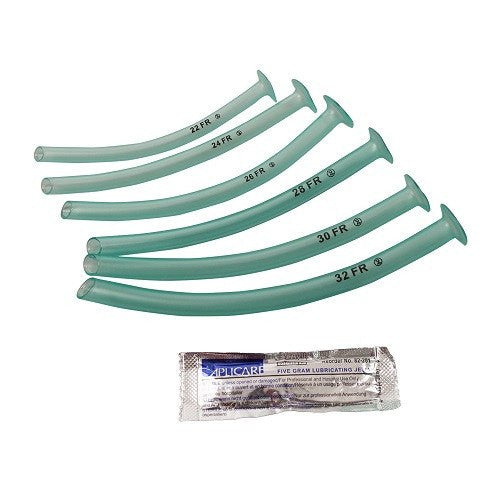
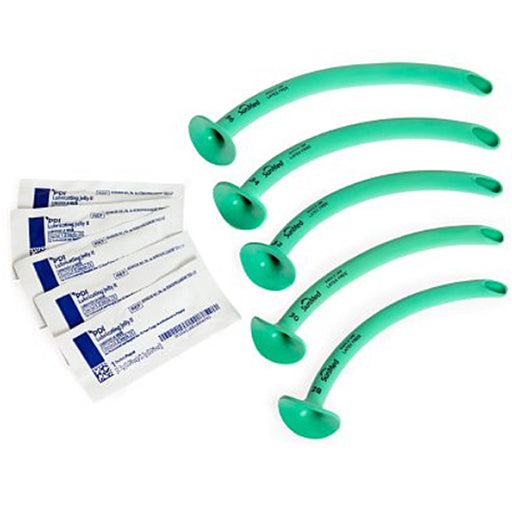
Sizes (adult vs. pediatric): NPAs are sized by internal diameter. Adult NPAs typically range from about 6.0–9.0 mm ID (roughly 18–27 French) with lengths ~6–9 cm. (For example, commercial NPAs come 12F–36F, equal to ~4–12 mm ID.) Pediatric NPAs are much smaller: roughly 3.0 mm ID for neonates, 3.5–4.5 mm for infants, up to ~6.0 mm for older children. A good rule is to pick an NPA about the same size as (or ~0.5 mm larger than) the child’s endotracheal tube.
Variants: Many NPAs have color-coded flanges to indicate size. Some include an adjustable (slidable) flange for fine depth control. They may be made of latex or latex-free materials (modern NPAs are usually PVC or silicone). In practice, adult and pediatric NPAs use different size sets but function identically as nasal airway adjuncts.
Nasopharyngeal tubes, or nasopharyngeal airways (NPAs), come in various sizes to accommodate different patients, ranging from infants to adults. The sizes are typically measured in French (Fr) units, which indicate the tube's outer diameter. Here are some general guidelines:
- Infants: Typically use sizes ranging from 12 Fr to 16 Fr.
- Children: Usually require sizes between 16 Fr and 26 Fr.
- Adults: Commonly use sizes from 26 Fr to 34 Fr.
When selecting the correct size, consider factors such as the patient's age, nasal passage diameter, and purpose of use. The ideal length can also be estimated by measuring from the tip of the patient's nose to the earlobe or the angle of the jaw.
How to Insert Nasopharyngeal Airway (NPA) Tube
A nasopharyngeal airway (NPA) is a soft, flexible tube (a “nasal trumpet”) inserted through a nostril into the posterior pharynx to bypass upper airway obstruction (such as relaxed tongue) in a semi-conscious patient. It is indicated when the patient has an intact gag reflex or difficult mouth opening (trismus), but not if there is suspicion of basal skull fracture or severe nasal/facial trauma. Before insertion, always follow local protocols, obtain consent if possible, and ensure the provider is trained in airway adjuncts.
Equipment and Preparation
- Size the NPA: Choose the correct size by measuring it against the patient’s face. A common method is to measure from the tip of the patient’s nose to the tragus (or earlobe) of their ear – this is the approximate length to reach the hypopharynx. (Tube diameters are usually 6–9 mm for adults.)
- Prepare the patient: Position the patient supine with the head in the “sniffing” position (neck flexed, head extended) if no spinal injury is suspected. If cervical spine injury is possible, leave the head in neutral alignment and use a jaw-thrust. Explain the procedure to a conscious patient.
- Sterile technique: Perform hand hygiene and put on clean gloves. Clear nasal passages of secretions or debris by suction if needed. Select the nostril that appears more patent (wider) — you may gently open and inspect both nares and choose the larger one. Have the patient breathe through the nose if possible, to confirm patency.
- Lubrication: Generously coat the distal 5–7 cm of the NPA with a water-soluble lubricant or lidocaine jelly. This minimizes mucosal injury and eases insertion. If the patient is conscious, topical nasal vasoconstrictor (e.g. phenylephrine) or lidocaine gel can be applied for comfort and to reduce bleeding.
Insertion Steps
- Orient the NPA correctly: Hold the NPA so that the beveled end (pointed end) is facing upward (toward the nasal septum) and the flanged end remains outside. In effect, the tube’s concave side (opening) will face down toward the floor of the nose. This orientation helps avoid scraping the delicate nasal septum – the pointed bevel edge should glide along the lateral wall of the nostril, not the center septum.
- Insert gently along the floor of the nose: Tilt the patient’s head slightly back (unless trauma precautions dictate neutral alignment) and insert the lubricated end of the NPA bevel-first and curving with the anatomy. Aim straight back (posteriorly), parallel to the floor of the nasal passage – not upward. Advance the tube with gentle pressure along the floor of the nasal cavity toward the back of the throat. Do not force the tube upward or with excessive force, as this can cause trauma or passage into the sinuses.
- Advance and rotate if needed: If you encounter resistance (which often means the tube is catching on the turbinates or nasal cartilage), withdraw slightly and rotate the NPA 90–180°, then attempt again. Gentle rotation can allow the bevel to navigate past obstructions. If it still won’t pass, try the other nostril. Never force a tube through resistance.
- Final positioning: Continue to advance until the flange rests against the nostril. At this point the distal tip should lie in the nasopharynx just above the epiglottis. (You can estimate this by having measured correctly; the tube will typically reach to the back of the tongue.) If the NPA is too long it may induce a gag; too short and it won’t bypass obstruction.
- Verify placement: Once inserted, confirm patency. Listen for improved breath sounds or the cessation of stertor/snoring. In a spontaneously breathing patient, there should be more effective airflow and less respiratory effort. If using bag-mask ventilation, you should notice a better mask seal and easier ventilation with less leak when the NPA is in place.
Securing and Monitoring
- Secure the NPA: Tape or otherwise secure the flange to the patient’s cheek or lip to prevent dislodgement. Ensure it remains in the chosen nostril and does not migrate.
- Monitor closely: Check the patient frequently. Watch for complications like nasal bleeding or increased agitation. Align the patient’s head so the NPA remains in position. Perform routine suctioning through the tube if necessary. An NPA can be kept in place as long as needed (even several hours), but it should be removed if there is any change in mental status (risk of gagging/vomiting) or if the airway no longer seems needed.
- Removal: When removing, gently pull the NPA out. If used for an awake patient, warn them of the sensation. Dispose of or clean the tube per protocol.
Precautions and Contraindications
- Skull/base-of-skull injury: Never insert an NPA if you suspect a basilar skull fracture. In such cases there is a risk of intracranial placement. Also avoid if severe facial trauma or really swollen/damaged nares are present.
- Do not force: If the airway will not pass smoothly after a gentle attempt and rotation, leave it out. Forcing it can cause bleeding, further obstruction, or trauma.
- Observe for bleeding: Minor epistaxis can occur. Applying firm gentle external pressure on the nose or topical vasoconstrictors can help. If significant bleeding or a bad reaction occurs, remove the NPA.
- Patient comfort: Even though NPAs are better tolerated than oropharyngeal airways, conscious patients may still feel discomfort. Use of suction, patient reassurance, and allowing the patient to breathe through the nose during insertion can aid tolerance.
How to Use a Nasopharyngeal Airway (Nasal Trumpet)
A nasopharyngeal airway (NPA) is a soft, flexible tube inserted through a nostril into the back of the throat to keep the airway open. It’s often used in semi-conscious or obtunded patients who still have an intact gag reflex (so they can tolerate a nasal tube better than an oral airway). The NPA bypasses obstructions at the base of the tongue or soft palate and allows air to flow freely into the trachea.
Use the NPA only when indicated: Typically, this means the patient is breathing but has partial airway obstruction (e.g. from tongue relaxation) and cannot tolerate an oral airway. Verify no contraindications such as suspected skull-base (cribriform plate) fracture or severe nasal trauma, which could allow the tube to penetrate into the cranial vault.
1. Prepare Equipment and Patient
- Gather supplies: sterile nasopharyngeal airway of various sizes, water‐soluble lubricant (or lidocaine jelly if conscious), gloves, tape (for securing, if needed), and suction ready.
- Measure for size: Choose an NPA length that will extend from the patient’s nostril to the back of the throat (above the epiglottis). A simple guide is to measure from the tip of the patient’s nose to the tragus (ear) on the same side. This ensures the tip will sit just above the epiglottis. (Average adults use roughly 6–7 mm ID for women, 7–8 mm ID for men.)
- Position patient: Place the patient supine. If no neck injury is suspected, a slight “sniffing” position (head tilt–chin lift) will align the airway. If cervical spine injury is possible, maintain neutral alignment (jaw thrust, C-spine precautions). Ensure the patient’s nostrils are clear of secretions (suction if needed). Explain the procedure briefly (if awake) and have suction ready for possible bleeding.
2. Lubricate the Airway
- Generously coat the outside and beveled tip of the NPA with sterile, water‐soluble lubricant. (If the patient is awake/cooperative, a lidocaine‐based jelly can be used to numb the nasal passage.) Lubrication is critical to ease insertion and minimize mucosal injury.
3. Insert the Tube
- Bevel orientation: Place the NPA into a nostril with the bevel (slanted end) forward. Some guides recommend facing the bevel toward the nasal septum (though the most important cue is to follow the natural curvature of the nose).
- Insertion direction: Gently advance the NPA posteriorly (straight back) along the floor of the nasal passage. Aim slightly backward (toward the throat), not upward. The proper trajectory follows the floor of the nose, skirting below the inferior turbinate. This minimizes trauma.
- Technique: Insert slowly and smoothly. Do not force the tube. If you feel significant resistance or the patient shows sudden pain, withdraw slightly and adjust your angle. You may need to rotate the tube slightly toward the midline or try the other nostril.
- Depth: Continue advancing until the flared flange rests against the nostril (outside) and the tip reaches just past the soft palate into the hypopharynx. In practice, the tip should end up roughly at the level of the epiglottis. An inserted NPA should not induce a gag reflex (it sits above the larynx), but you may feel some resistance as it passes the nasopharynx. Stop advancing if the patient gags violently or if bleeding occurs. Forcing the NPA can cause trauma; if the tube will not advance with gentle pressure, remove it and try a smaller size or the other nostril.
4. Confirm and Secure
- Check airway patency: Once inserted, confirm the airway is open. You should see an immediate improvement in breathing effort: airflow and chest rise are more evident, and you can hear or feel breaths moving freely through the tube. If the patient is on a ventilator or bag-mask ventilation, breaths should pass easily through the NPA.
- Maintain head position: You may continue a jaw-thrust or chin-lift if needed to optimize alignment. The mouth can be slightly open. The NPA should prevent the tongue from blocking the airway.
- Secure if necessary: If the NPA will remain in place for an extended period, tape it to the patient’s face. Use adhesive tape across the bridge of the nose and over the end of the airway flange to keep it from slipping out.
- Monitor continuously: Observe the patient’s respiratory rate, oxygen saturation, and chest movement. Be ready to remove or adjust the NPA if it shifts or if the patient’s condition changes. It should relieve upper airway obstruction.
5. Removal and Aftercare
- Remove when appropriate: The NPA is a temporary aid. Remove it if the patient regains consciousness and can maintain their airway independently, or if a more secure airway (e.g. endotracheal intubation) is placed. To remove, lubricate slightly and pull straight out of the nostril.
- Monitor after removal: Ensure the patient continues to breathe well. Prepare to manage airway as needed (e.g. reposition, provide supplemental oxygen).
6. Precautions and Complications
- Contraindications: As noted, avoid NPAs if basal skull fracture is suspected (evidence of raccoon eyes, Battle’s sign, CSF leak) or if severe nasal/facial trauma is present). In these cases, the tube could penetrate through a skull fracture.
- Nasal bleeding: Aspirating or creeping of blood is common. Epistaxis (nosebleed) can occur during insertion. If bleeding happens, withdraw the NPA and apply pressure to the nose. Consider a smaller tube or the other nostril. Use gentle technique to minimize mucosal injury.
- Gagging/vomiting: Because the NPA sits at the back of the throat, it may induce gag reflex in semi‐conscious patients. Insert slowly and stop if the patient gags forcefully. Keep suction ready; if the patient vomits, clear the airway immediately to prevent aspiration.
- Infection: As with any nasal instrument, aseptic technique is used to reduce infection risk. The NPA is not sterile once opened, but it is normally tolerated safely for short‐term use.
- Discomfort: Patients who are awake may find the NPA uncomfortable. Lubrication and possibly topical anesthetic can help. Explain the process and proceed gently.
In summary: To use an NPA, select the correct size, lubricate it, and gently insert the beveled end into a patent nostril aiming along the nasal floor. Advance until you meet slight resistance—at that point the tip should be in the nasopharynx (just above the soft palate). Confirm improved airflow and secure the tube. Always use caution (do not force in cases of resistance or contraindication). By following these steps, a nasopharyngeal airway can safely bypass upper airway obstruction and help maintain effective breathing in an emergency or pre‐hospital setting.
Medical Airway Management
Airway management is the set of measures used to keep a patient’s airway open and clear so that breathing (ventilation) and oxygen delivery can occur. In other words, it encompasses “all actions aimed at ensuring the patency of the airways and guaranteeing sufficient spontaneous breathing or external ventilation”. Effective airway management is fundamental in emergency and operative medicine – failure to establish a free airway can quickly lead to life-threatening hypoxia. Indeed, a blocked airway and resulting oxygen deficiency is the single most important anesthesia-related cause of serious injury or perioperative death. In practice, airway management ranges from quick bedside maneuvers (head-tilt, jaw-thrust) to advanced interventions (intubation, surgical airway) to protect the airway and support breathing.
Key goals: Securing a clear, “patent” airway so that adequate ventilation and oxygenation occur. This often requires assessing the airway first (checking consciousness, obstructions, breathing – “look, listen, feel”), then opening or securing it with appropriate techniques, and finally supporting breathing (with oxygen, bag-mask ventilation, or mechanical ventilation). Continuous monitoring (pulse oximetry, capnography, vital signs) is essential throughout to confirm that the airway remains open and the patient is oxygenating effectively.
Indications for Airway Management
Airway management is indicated whenever a patient cannot protect or maintain their own airway. Common scenarios include:
- Respiratory failure or insufficiency: The patient cannot maintain adequate oxygenation (hypoxemia) or ventilation (hypercapnia). Examples include severe asthma/COPD exacerbation, respiratory arrest, or neurologic depression of breathing.
- Unconsciousness or depressed mental status: A comatose or heavily sedated patient often loses airway tone (tongue falls back) and cannot breathe on their own. Such patients need their airway opened (e.g. via head-tilt) and usually need assisted ventilation.
- High risk of obstruction/aspiration: Situations like vomiting, facial/neck trauma, burns or swelling, or ingestion of large foreign bodies can acutely block the airway. Airway management (positioning, suction, intubation, etc.) prevents airway obstruction by vomitus, blood or other debris..
- Planned anesthesia or sedation: Patients undergoing surgery or procedures under general anesthesia are intubated to control the airway and breathing. (Even routine induction of anesthesia is a form of airway management.)
- Cardiac arrest or CPR: During resuscitation, an open airway is critical. Standard protocols begin with opening the airway and ventilating (by bag-mask ventilation or intubation) to restore oxygen delivery.
Basic Airway Maneuvers
Initial airway management in an unconscious or unresponsive patient relies on simple maneuvers to open the airway. The patient is placed supine, and the clinician checks if the mouth/throat are clear. Common maneuvers include:
- Head-tilt–Chin-lift: Gently tilt the head back and lift the chin up, which lifts the tongue away from the back of the throat. This often restores an airway if the tongue is the only obstruction. (This is contraindicated if there is suspected neck injury.)
- Jaw-thrust: If cervical spine injury is possible, the jaw-thrust is used instead. The provider grasps the angles of the lower jaw and lifts it forward without moving the neck, tenting the tongue and opening the airway while keeping neck alignment.
- Recovery (lateral) position: For a breathing-but-unconscious patient, placing them on their side helps drain secretions and keeps the tongue from occluding the airway.
During these maneuvers, the provider uses a “look, listen, and feel” approach to assess breathing: look for chest rise, listen/feel for air at the mouth, and feel for breathing on your cheek. If airway obstruction is obvious (food, dentures, vomit), it should be removed manually if possible. Back blows or Heimlich maneuvers are used in choking victims with a foreign body in the hypopharynx. Throughout, one provides oxygen by mask if available.
Airway Adjuncts
When basic positioning is not enough, airway adjunct devices can help keep the airway open. These are placed into the mouth or nose to prevent tongue or soft tissues from occluding the airway. Common adjuncts include:
- Oropharyngeal airway (OPA): A curved plastic device inserted through the patient’s open mouth to keep the tongue from falling back. OPAs are used only in unresponsive patients without a gag reflex (since it would provoke gagging or vomiting otherwise).
- Nasopharyngeal airway (NPA): A soft rubber or plastic tube inserted through the nostril into the pharynx. NPAs can be used even if the patient is semi-conscious (some gagging is tolerated) and are useful when oral access is difficult. However, avoid NPAs in midface trauma or suspected skull-base fracture.
These adjuncts do not guarantee ventilation, but they maintain patency as you prepare for more definitive measures. Along with adjunct placement, suctioning any secretions or debris from the oropharynx is essential.
Ventilation and Oxygenation Support
Once the airway is open or secured, breathing must be supported. Supplemental oxygen is given as soon as possible (via nasal cannula or face mask). If the patient isn’t breathing adequately, ventilation is assisted:
- Bag-valve-mask (BVM) ventilation: A self-inflating bag attached to a face mask is squeezed to force breaths into the lungs. Proper mask seal and head positioning (often jaw-thrust) are needed. BVM is a fundamental backup for apneic patients before definitive airway placement.
- Mechanical ventilation: In hospital settings, the patient may be intubated and connected to a ventilator to control respiratory rate and volume. This provides precise breathing support in ICU or during surgery.
These interventions help maintain oxygen (O₂) levels and remove carbon dioxide (CO₂) once any airway device is in place. Adequate ventilation (tidal volume, rate) is monitored by chest rise and capnography.
Advanced Airway Techniques
If basic measures fail or are insufficient, more advanced airway interventions are used. These require trained providers and often special equipment. Key advanced techniques include:
- Endotracheal intubation (ETI): Inserting a cuffed tube through the mouth (or nose) past the vocal cords into the trachea. ETI creates a definitive airway and seals the lungs from upper airway contamination. Intubation requires visualization of the cords (direct laryngoscopy or video laryngoscopy) and usually muscle relaxation/medication. Once the tube is in place, its position is confirmed (listening for bilateral breath sounds, capnography).
- Supraglottic airway (SGA) devices: These include laryngeal mask airways (LMAs), i-gels, combitubes, etc. SGAs sit above the vocal cords and allow ventilation without being in the trachea. They are easier to place than a tube and are often used as a bridge or in cases where intubation may be difficult.
- Surgical airway: When intubation and mask ventilation both fail and the airway must be secured urgently, an emergency cricothyrotomy or tracheostomy is performed. This creates a direct hole in the trachea below the larynx. Surgical airway is a last resort for “can’t intubate, can’t ventilate” situations.
In all cases, airway management is a continuous process: if an advanced airway is in place, it must be secured (taped or tied), and the patient must be ventilated with oxygen. For intubated patients, end-tidal CO₂ monitors and repeat chest exams help confirm and maintain placement.
Monitoring and Reassessment
Throughout airway management, continuous monitoring is essential. This includes:
- Pulse oximetry: Monitors oxygen saturation, alerting for hypoxemia.
- End-tidal CO₂ (capnography): Confirms tube placement in the trachea (presence of CO₂ with breaths) and helps gauge ventilation.
- Clinical signs: Watch chest rise, breathing effort, skin color, and vital signs (heart rate, blood pressure) for signs of respiratory distress or improvement.
- Repeat assessment: Continuously re-check airway patency after each intervention. If obstruction recurs or oxygen drops, be prepared to reposition, suction, or advance to the next airway step.
Effective airway management depends on prompt recognition of problems and quick action. It is not a one-time procedure but a dynamic process of assessment and adjustment to ensure adequate breathing.
Common Airway Obstructions and Special Cases
Common causes of airway compromise include tongue collapse (in unconsciousness), Foreign Body Airway Obstruction (choking on food or objects), swelling of tissues (e.g. tongue or epiglottis from allergic reaction or infection), and trauma-related deformities. Management must be tailored accordingly: e.g. suction or back blows for choking, and cricothyrotomy if swelling completely blocks traditional intubation. Trauma patients deserve special care: always assume a cervical spine injury and use jaw-thrust instead of head-tilt.
Pediatric airways are anatomically different (smaller, more anterior, larger occiput), so airway maneuvers and devices are adjusted (smaller tubes, head positioning aids). In obstetrics, a pregnant patient has increased aspiration risk; therefore a rapid-sequence induction and intubation is often done to protect the airway during surgery. Each context has nuance, but the core principles of keeping the airway open remain the same.
Note: Airway management is a critical skill traditionally taught in medical, paramedic, and nursing training. If you are not a healthcare provider, you should not attempt advanced airway procedures on a real patient. However, even basic knowledge (calling for help, placing someone in the recovery position, performing the Heimlich maneuver for choking, or beginning CPR) can save lives in an emergency.
This overview is for informational purposes only and not a substitute for professional medical training or advice. Clinicians should follow established protocols and guidelines (e.g. ACLS/PALS/ATLS) in airway management.
Nasopharyngeal Tubes (Nasal Airways) Types & Sizes
Nasopharyngeal Airway (NPA) – a soft, hollow tube (PVC/silicone or rubber) inserted through the nostril into the posterior pharynx to maintain an open airway. NPAs are often called “nasal trumpets” (or by trade names, e.g. a “Robertazzi” airway). They have a flanged end that prevents over-insertion; the distal tip is beveled and curved to follow the nasal passage.
Sizes (adult vs. pediatric): NPAs are sized by internal diameter. Adult NPAs typically range from about 6.0–9.0 mm ID (roughly 18–27 French) with lengths ~6–9 cm. (For example, commercial NPAs come 12F–36F, equal to ~4–12 mm ID.) Pediatric NPAs are much smaller: roughly 3.0 mm ID for neonates, 3.5–4.5 mm for infants, up to ~6.0 mm for older children. A good rule is to pick an NPA about the same size as (or ~0.5 mm larger than) the child’s endotracheal tube.
Variants: Many NPAs have color-coded flanges to indicate size. Some include an adjustable (slidable) flange for fine depth control. They may be made of latex or latex-free materials (modern NPAs are usually PVC or silicone). In practice, adult and pediatric NPAs use different size sets but function identically as nasal airway adjuncts.
Nasopharyngeal tubes, or nasopharyngeal airways (NPAs), come in various sizes to accommodate different patients, ranging from infants to adults. The sizes are typically measured in French (Fr) units, which indicate the tube's outer diameter. Here are some general guidelines:
- Infants: Typically use sizes ranging from 12 Fr to 16 Fr.
- Children: Usually require sizes between 16 Fr and 26 Fr.
- Adults: Commonly use sizes from 26 Fr to 34 Fr.
When selecting the correct size, consider factors such as the patient's age, nasal passage diameter, and purpose of use. The ideal length can also be estimated by measuring from the tip of the patient's nose to the earlobe or the angle of the jaw.
How to Insert Nasopharyngeal Airway (NPA) Tube
A nasopharyngeal airway (NPA) is a soft, flexible tube (a “nasal trumpet”) inserted through a nostril into the posterior pharynx to bypass upper airway obstruction (such as relaxed tongue) in a semi-conscious patient. It is indicated when the patient has an intact gag reflex or difficult mouth opening (trismus), but not if there is suspicion of basal skull fracture or severe nasal/facial trauma. Before insertion, always follow local protocols, obtain consent if possible, and ensure the provider is trained in airway adjuncts.
Equipment and Preparation
- Size the NPA: Choose the correct size by measuring it against the patient’s face. A common method is to measure from the tip of the patient’s nose to the tragus (or earlobe) of their ear – this is the approximate length to reach the hypopharynx. (Tube diameters are usually 6–9 mm for adults.)
- Prepare the patient: Position the patient supine with the head in the “sniffing” position (neck flexed, head extended) if no spinal injury is suspected. If cervical spine injury is possible, leave the head in neutral alignment and use a jaw-thrust. Explain the procedure to a conscious patient.
- Sterile technique: Perform hand hygiene and put on clean gloves. Clear nasal passages of secretions or debris by suction if needed. Select the nostril that appears more patent (wider) — you may gently open and inspect both nares and choose the larger one. Have the patient breathe through the nose if possible, to confirm patency.
- Lubrication: Generously coat the distal 5–7 cm of the NPA with a water-soluble lubricant or lidocaine jelly. This minimizes mucosal injury and eases insertion. If the patient is conscious, topical nasal vasoconstrictor (e.g. phenylephrine) or lidocaine gel can be applied for comfort and to reduce bleeding.
Insertion Steps
- Orient the NPA correctly: Hold the NPA so that the beveled end (pointed end) is facing upward (toward the nasal septum) and the flanged end remains outside. In effect, the tube’s concave side (opening) will face down toward the floor of the nose. This orientation helps avoid scraping the delicate nasal septum – the pointed bevel edge should glide along the lateral wall of the nostril, not the center septum.
- Insert gently along the floor of the nose: Tilt the patient’s head slightly back (unless trauma precautions dictate neutral alignment) and insert the lubricated end of the NPA bevel-first and curving with the anatomy. Aim straight back (posteriorly), parallel to the floor of the nasal passage – not upward. Advance the tube with gentle pressure along the floor of the nasal cavity toward the back of the throat. Do not force the tube upward or with excessive force, as this can cause trauma or passage into the sinuses.
- Advance and rotate if needed: If you encounter resistance (which often means the tube is catching on the turbinates or nasal cartilage), withdraw slightly and rotate the NPA 90–180°, then attempt again. Gentle rotation can allow the bevel to navigate past obstructions. If it still won’t pass, try the other nostril. Never force a tube through resistance.
- Final positioning: Continue to advance until the flange rests against the nostril. At this point the distal tip should lie in the nasopharynx just above the epiglottis. (You can estimate this by having measured correctly; the tube will typically reach to the back of the tongue.) If the NPA is too long it may induce a gag; too short and it won’t bypass obstruction.
- Verify placement: Once inserted, confirm patency. Listen for improved breath sounds or the cessation of stertor/snoring. In a spontaneously breathing patient, there should be more effective airflow and less respiratory effort. If using bag-mask ventilation, you should notice a better mask seal and easier ventilation with less leak when the NPA is in place.
Securing and Monitoring
- Secure the NPA: Tape or otherwise secure the flange to the patient’s cheek or lip to prevent dislodgement. Ensure it remains in the chosen nostril and does not migrate.
- Monitor closely: Check the patient frequently. Watch for complications like nasal bleeding or increased agitation. Align the patient’s head so the NPA remains in position. Perform routine suctioning through the tube if necessary. An NPA can be kept in place as long as needed (even several hours), but it should be removed if there is any change in mental status (risk of gagging/vomiting) or if the airway no longer seems needed.
- Removal: When removing, gently pull the NPA out. If used for an awake patient, warn them of the sensation. Dispose of or clean the tube per protocol.
Precautions and Contraindications
- Skull/base-of-skull injury: Never insert an NPA if you suspect a basilar skull fracture. In such cases there is a risk of intracranial placement. Also avoid if severe facial trauma or really swollen/damaged nares are present.
- Do not force: If the airway will not pass smoothly after a gentle attempt and rotation, leave it out. Forcing it can cause bleeding, further obstruction, or trauma.
- Observe for bleeding: Minor epistaxis can occur. Applying firm gentle external pressure on the nose or topical vasoconstrictors can help. If significant bleeding or a bad reaction occurs, remove the NPA.
- Patient comfort: Even though NPAs are better tolerated than oropharyngeal airways, conscious patients may still feel discomfort. Use of suction, patient reassurance, and allowing the patient to breathe through the nose during insertion can aid tolerance.
How to Use a Nasopharyngeal Airway (Nasal Trumpet)
A nasopharyngeal airway (NPA) is a soft, flexible tube inserted through a nostril into the back of the throat to keep the airway open. It’s often used in semi-conscious or obtunded patients who still have an intact gag reflex (so they can tolerate a nasal tube better than an oral airway). The NPA bypasses obstructions at the base of the tongue or soft palate and allows air to flow freely into the trachea.
Use the NPA only when indicated: Typically, this means the patient is breathing but has partial airway obstruction (e.g. from tongue relaxation) and cannot tolerate an oral airway. Verify no contraindications such as suspected skull-base (cribriform plate) fracture or severe nasal trauma, which could allow the tube to penetrate into the cranial vault.
1. Prepare Equipment and Patient
- Gather supplies: sterile nasopharyngeal airway of various sizes, water‐soluble lubricant (or lidocaine jelly if conscious), gloves, tape (for securing, if needed), and suction ready.
- Measure for size: Choose an NPA length that will extend from the patient’s nostril to the back of the throat (above the epiglottis). A simple guide is to measure from the tip of the patient’s nose to the tragus (ear) on the same side. This ensures the tip will sit just above the epiglottis. (Average adults use roughly 6–7 mm ID for women, 7–8 mm ID for men.)
- Position patient: Place the patient supine. If no neck injury is suspected, a slight “sniffing” position (head tilt–chin lift) will align the airway. If cervical spine injury is possible, maintain neutral alignment (jaw thrust, C-spine precautions). Ensure the patient’s nostrils are clear of secretions (suction if needed). Explain the procedure briefly (if awake) and have suction ready for possible bleeding.
2. Lubricate the Airway
- Generously coat the outside and beveled tip of the NPA with sterile, water‐soluble lubricant. (If the patient is awake/cooperative, a lidocaine‐based jelly can be used to numb the nasal passage.) Lubrication is critical to ease insertion and minimize mucosal injury.
3. Insert the Tube
- Bevel orientation: Place the NPA into a nostril with the bevel (slanted end) forward. Some guides recommend facing the bevel toward the nasal septum (though the most important cue is to follow the natural curvature of the nose).
- Insertion direction: Gently advance the NPA posteriorly (straight back) along the floor of the nasal passage. Aim slightly backward (toward the throat), not upward. The proper trajectory follows the floor of the nose, skirting below the inferior turbinate. This minimizes trauma.
- Technique: Insert slowly and smoothly. Do not force the tube. If you feel significant resistance or the patient shows sudden pain, withdraw slightly and adjust your angle. You may need to rotate the tube slightly toward the midline or try the other nostril.
- Depth: Continue advancing until the flared flange rests against the nostril (outside) and the tip reaches just past the soft palate into the hypopharynx. In practice, the tip should end up roughly at the level of the epiglottis. An inserted NPA should not induce a gag reflex (it sits above the larynx), but you may feel some resistance as it passes the nasopharynx. Stop advancing if the patient gags violently or if bleeding occurs. Forcing the NPA can cause trauma; if the tube will not advance with gentle pressure, remove it and try a smaller size or the other nostril.
4. Confirm and Secure
- Check airway patency: Once inserted, confirm the airway is open. You should see an immediate improvement in breathing effort: airflow and chest rise are more evident, and you can hear or feel breaths moving freely through the tube. If the patient is on a ventilator or bag-mask ventilation, breaths should pass easily through the NPA.
- Maintain head position: You may continue a jaw-thrust or chin-lift if needed to optimize alignment. The mouth can be slightly open. The NPA should prevent the tongue from blocking the airway.
- Secure if necessary: If the NPA will remain in place for an extended period, tape it to the patient’s face. Use adhesive tape across the bridge of the nose and over the end of the airway flange to keep it from slipping out.
- Monitor continuously: Observe the patient’s respiratory rate, oxygen saturation, and chest movement. Be ready to remove or adjust the NPA if it shifts or if the patient’s condition changes. It should relieve upper airway obstruction.
5. Removal and Aftercare
- Remove when appropriate: The NPA is a temporary aid. Remove it if the patient regains consciousness and can maintain their airway independently, or if a more secure airway (e.g. endotracheal intubation) is placed. To remove, lubricate slightly and pull straight out of the nostril.
- Monitor after removal: Ensure the patient continues to breathe well. Prepare to manage airway as needed (e.g. reposition, provide supplemental oxygen).
6. Precautions and Complications
- Contraindications: As noted, avoid NPAs if basal skull fracture is suspected (evidence of raccoon eyes, Battle’s sign, CSF leak) or if severe nasal/facial trauma is present). In these cases, the tube could penetrate through a skull fracture.
- Nasal bleeding: Aspirating or creeping of blood is common. Epistaxis (nosebleed) can occur during insertion. If bleeding happens, withdraw the NPA and apply pressure to the nose. Consider a smaller tube or the other nostril. Use gentle technique to minimize mucosal injury.
- Gagging/vomiting: Because the NPA sits at the back of the throat, it may induce gag reflex in semi‐conscious patients. Insert slowly and stop if the patient gags forcefully. Keep suction ready; if the patient vomits, clear the airway immediately to prevent aspiration.
- Infection: As with any nasal instrument, aseptic technique is used to reduce infection risk. The NPA is not sterile once opened, but it is normally tolerated safely for short‐term use.
- Discomfort: Patients who are awake may find the NPA uncomfortable. Lubrication and possibly topical anesthetic can help. Explain the process and proceed gently.
In summary: To use an NPA, select the correct size, lubricate it, and gently insert the beveled end into a patent nostril aiming along the nasal floor. Advance until you meet slight resistance—at that point the tip should be in the nasopharynx (just above the soft palate). Confirm improved airflow and secure the tube. Always use caution (do not force in cases of resistance or contraindication). By following these steps, a nasopharyngeal airway can safely bypass upper airway obstruction and help maintain effective breathing in an emergency or pre‐hospital setting.
Medical Airway Management
Airway management is the set of measures used to keep a patient’s airway open and clear so that breathing (ventilation) and oxygen delivery can occur. In other words, it encompasses “all actions aimed at ensuring the patency of the airways and guaranteeing sufficient spontaneous breathing or external ventilation”. Effective airway management is fundamental in emergency and operative medicine – failure to establish a free airway can quickly lead to life-threatening hypoxia. Indeed, a blocked airway and resulting oxygen deficiency is the single most important anesthesia-related cause of serious injury or perioperative death. In practice, airway management ranges from quick bedside maneuvers (head-tilt, jaw-thrust) to advanced interventions (intubation, surgical airway) to protect the airway and support breathing.
Key goals: Securing a clear, “patent” airway so that adequate ventilation and oxygenation occur. This often requires assessing the airway first (checking consciousness, obstructions, breathing – “look, listen, feel”), then opening or securing it with appropriate techniques, and finally supporting breathing (with oxygen, bag-mask ventilation, or mechanical ventilation). Continuous monitoring (pulse oximetry, capnography, vital signs) is essential throughout to confirm that the airway remains open and the patient is oxygenating effectively.
Indications for Airway Management
Airway management is indicated whenever a patient cannot protect or maintain their own airway. Common scenarios include:
- Respiratory failure or insufficiency: The patient cannot maintain adequate oxygenation (hypoxemia) or ventilation (hypercapnia). Examples include severe asthma/COPD exacerbation, respiratory arrest, or neurologic depression of breathing.
- Unconsciousness or depressed mental status: A comatose or heavily sedated patient often loses airway tone (tongue falls back) and cannot breathe on their own. Such patients need their airway opened (e.g. via head-tilt) and usually need assisted ventilation.
- High risk of obstruction/aspiration: Situations like vomiting, facial/neck trauma, burns or swelling, or ingestion of large foreign bodies can acutely block the airway. Airway management (positioning, suction, intubation, etc.) prevents airway obstruction by vomitus, blood or other debris..
- Planned anesthesia or sedation: Patients undergoing surgery or procedures under general anesthesia are intubated to control the airway and breathing. (Even routine induction of anesthesia is a form of airway management.)
- Cardiac arrest or CPR: During resuscitation, an open airway is critical. Standard protocols begin with opening the airway and ventilating (by bag-mask ventilation or intubation) to restore oxygen delivery.
Basic Airway Maneuvers
Initial airway management in an unconscious or unresponsive patient relies on simple maneuvers to open the airway. The patient is placed supine, and the clinician checks if the mouth/throat are clear. Common maneuvers include:
- Head-tilt–Chin-lift: Gently tilt the head back and lift the chin up, which lifts the tongue away from the back of the throat. This often restores an airway if the tongue is the only obstruction. (This is contraindicated if there is suspected neck injury.)
- Jaw-thrust: If cervical spine injury is possible, the jaw-thrust is used instead. The provider grasps the angles of the lower jaw and lifts it forward without moving the neck, tenting the tongue and opening the airway while keeping neck alignment.
- Recovery (lateral) position: For a breathing-but-unconscious patient, placing them on their side helps drain secretions and keeps the tongue from occluding the airway.
During these maneuvers, the provider uses a “look, listen, and feel” approach to assess breathing: look for chest rise, listen/feel for air at the mouth, and feel for breathing on your cheek. If airway obstruction is obvious (food, dentures, vomit), it should be removed manually if possible. Back blows or Heimlich maneuvers are used in choking victims with a foreign body in the hypopharynx. Throughout, one provides oxygen by mask if available.
Airway Adjuncts
When basic positioning is not enough, airway adjunct devices can help keep the airway open. These are placed into the mouth or nose to prevent tongue or soft tissues from occluding the airway. Common adjuncts include:
- Oropharyngeal airway (OPA): A curved plastic device inserted through the patient’s open mouth to keep the tongue from falling back. OPAs are used only in unresponsive patients without a gag reflex (since it would provoke gagging or vomiting otherwise).
- Nasopharyngeal airway (NPA): A soft rubber or plastic tube inserted through the nostril into the pharynx. NPAs can be used even if the patient is semi-conscious (some gagging is tolerated) and are useful when oral access is difficult. However, avoid NPAs in midface trauma or suspected skull-base fracture.
These adjuncts do not guarantee ventilation, but they maintain patency as you prepare for more definitive measures. Along with adjunct placement, suctioning any secretions or debris from the oropharynx is essential.
Ventilation and Oxygenation Support
Once the airway is open or secured, breathing must be supported. Supplemental oxygen is given as soon as possible (via nasal cannula or face mask). If the patient isn’t breathing adequately, ventilation is assisted:
- Bag-valve-mask (BVM) ventilation: A self-inflating bag attached to a face mask is squeezed to force breaths into the lungs. Proper mask seal and head positioning (often jaw-thrust) are needed. BVM is a fundamental backup for apneic patients before definitive airway placement.
- Mechanical ventilation: In hospital settings, the patient may be intubated and connected to a ventilator to control respiratory rate and volume. This provides precise breathing support in ICU or during surgery.
These interventions help maintain oxygen (O₂) levels and remove carbon dioxide (CO₂) once any airway device is in place. Adequate ventilation (tidal volume, rate) is monitored by chest rise and capnography.
Advanced Airway Techniques
If basic measures fail or are insufficient, more advanced airway interventions are used. These require trained providers and often special equipment. Key advanced techniques include:
- Endotracheal intubation (ETI): Inserting a cuffed tube through the mouth (or nose) past the vocal cords into the trachea. ETI creates a definitive airway and seals the lungs from upper airway contamination. Intubation requires visualization of the cords (direct laryngoscopy or video laryngoscopy) and usually muscle relaxation/medication. Once the tube is in place, its position is confirmed (listening for bilateral breath sounds, capnography).
- Supraglottic airway (SGA) devices: These include laryngeal mask airways (LMAs), i-gels, combitubes, etc. SGAs sit above the vocal cords and allow ventilation without being in the trachea. They are easier to place than a tube and are often used as a bridge or in cases where intubation may be difficult.
- Surgical airway: When intubation and mask ventilation both fail and the airway must be secured urgently, an emergency cricothyrotomy or tracheostomy is performed. This creates a direct hole in the trachea below the larynx. Surgical airway is a last resort for “can’t intubate, can’t ventilate” situations.
In all cases, airway management is a continuous process: if an advanced airway is in place, it must be secured (taped or tied), and the patient must be ventilated with oxygen. For intubated patients, end-tidal CO₂ monitors and repeat chest exams help confirm and maintain placement.
Monitoring and Reassessment
Throughout airway management, continuous monitoring is essential. This includes:
- Pulse oximetry: Monitors oxygen saturation, alerting for hypoxemia.
- End-tidal CO₂ (capnography): Confirms tube placement in the trachea (presence of CO₂ with breaths) and helps gauge ventilation.
- Clinical signs: Watch chest rise, breathing effort, skin color, and vital signs (heart rate, blood pressure) for signs of respiratory distress or improvement.
- Repeat assessment: Continuously re-check airway patency after each intervention. If obstruction recurs or oxygen drops, be prepared to reposition, suction, or advance to the next airway step.
Effective airway management depends on prompt recognition of problems and quick action. It is not a one-time procedure but a dynamic process of assessment and adjustment to ensure adequate breathing.
Common Airway Obstructions and Special Cases
Common causes of airway compromise include tongue collapse (in unconsciousness), Foreign Body Airway Obstruction (choking on food or objects), swelling of tissues (e.g. tongue or epiglottis from allergic reaction or infection), and trauma-related deformities. Management must be tailored accordingly: e.g. suction or back blows for choking, and cricothyrotomy if swelling completely blocks traditional intubation. Trauma patients deserve special care: always assume a cervical spine injury and use jaw-thrust instead of head-tilt.
Pediatric airways are anatomically different (smaller, more anterior, larger occiput), so airway maneuvers and devices are adjusted (smaller tubes, head positioning aids). In obstetrics, a pregnant patient has increased aspiration risk; therefore a rapid-sequence induction and intubation is often done to protect the airway during surgery. Each context has nuance, but the core principles of keeping the airway open remain the same.
Note: Airway management is a critical skill traditionally taught in medical, paramedic, and nursing training. If you are not a healthcare provider, you should not attempt advanced airway procedures on a real patient. However, even basic knowledge (calling for help, placing someone in the recovery position, performing the Heimlich maneuver for choking, or beginning CPR) can save lives in an emergency.
This overview is for informational purposes only and not a substitute for professional medical training or advice. Clinicians should follow established protocols and guidelines (e.g. ACLS/PALS/ATLS) in airway management.