Filters
- Aesthetic Supplies MedSpa Supplies & Cosmetic Surgery Supplies (13)
- Botox Syringes (1)
- buy insulin syringes (1)
- Easy Touch (1)
- Easy Touch Syringes (1)
- Insulin (14)
- insulin needle (2)
- insulin syringe sizes (1)
- Insulin Syringes Near Me (1)
- Semaglutide Syringes (1)
- U-100 Insulin Syringes (24)
- 31 Gauge (8)
- 31g (2)
- comfort (1)
- Filler Syringes (1)
- Insulin Injection (7)
- Ozempic Syringes (1)
- Pet Insulin Syringes (4)
- Sure Comfort (7)
- Veterinary Insulin Syringe (4)
- 1 cc Syringes (2)
- 29 gauge (7)
- 29 Gauge x ½" (1)
- 511110 (1)
- 8881511110 (1)
- Covidien (1)
- Monoject (1)
- BD Ultra-Fine (2)
- Diabetes Management (2)
- Diabetes Supply (1)
- Disposable Syringes (1)
- Fine Needle (1)
- Insulin Injections (1)
- Small needle (1)
- Sterile Syringes (1)
- Ultrafine Syringes (1)
- 1 mL insulin syringe (2)
- 30 Gauge (4)
- 30 gauge insulin syringe (1)
- 328411 (1)
- BD Insulin Syringes (8)
- best insulin syringes (2)
- blood sugar management (2)
- Diabetes Supplies (6)
- diabetic syringes (2)
- Embecta (7)
- Embecta insulin syringes (1)
- home diabetes care (1)
- insulin needles (2)
- PRP Injections (1)
- safe insulin delivery (1)
- sterile syringe (1)
- ultra-fine needle (2)
- Untra Fine Needle (1)
- 329424 (1)
- Fine Needles (2)
- Micro Fine (1)
- Micro Needle (1)
- Microfine Syringes (1)
- Ultra fine (1)
- 0.5 mL insulin syringe (1)
- disposable insulin syringe (1)
- disposable syringes (1)
- Insulin syringes 31 gauge (2)
- short needle (1)
- short needle insulin syringe (1)
- single-use insulin injection (1)
- sterile diabetic syringes (1)
- subcutaneous insulin syringes (1)
- SureComfort (1)
- 31 gauge insulin needles (1)
- Aesthetic Needles (1)
- Aesthetic Syringes (1)
- Fine Syringe (1)
- Fine Tip (1)
- Fine Tip Syringes (1)
- insulin syringes for diabetes (1)
- Micro Needles (1)
- Ultra Fine Needles (2)
- ultra-fine insulin syringes (1)
- 30 gauge Syringes (1)
- bd syringes (5)
- Ultra Fine Syringes (2)
- 324906 (1)
- BD Needles (2)
- BD Veo (1)
- Ultra Fine Insulin Syringes (1)
- Diabetes Needles (1)
- Diabetes Syringes (3)
- Magellan (1)
- monoject (2)
- 31g insulin needles (1)
- 328418 insulin syringe (1)
- 8mm insulin syringes (1)
- diabetes syringes (1)
- diabetic injection (1)
- ltra-fine insulin injection (1)
- safe insulin shot (1)
- U-100 insulin syringe (1)
- Diabetes Care (3)
- 3/10 mL insulin syringe (1)
- 31 gauge syringes (1)
- 324910 (1)
- Blood Sugar Management (1)
- EasyTouch (1)
- Embecta syringes (1)
- hort needle insulin syringes (1)
- hypoallergenic needle (1)
- Insulin Syringes 31 gauge (1)
- NovoFine (1)
- painless insulin syringe (1)
- safe insulin injection (1)
- True Comfort (1)
- 31 Gauge x 1/2 (1)
- 324911 (1)
- Pen Needles (2)
- doctor-only (1)
- 5/16 (2)
- Short Needle Syringe (3)
- 1 ml (1)
- 1 ml Syringe (1)
- 29-gauge needle (1)
- Insulin therapy (1)
- Subcutaneous injections (1)
- 28 Gauge (1)
- Blood Glucose Levels (1)
- Regular Needle (1)
- Ulticare (1)
- Ulticare Insulin Syringes (1)
- Retractable Needle (1)
- Retractable Syringe (1)
- Stainless Steel Needle (1)
- VanishPoint (1)
- Blood Samples (1)
- Dosage Control (1)
- Fluid Withdrawal (1)
- General Syringes (1)
- Luer Lok Tip (1)
- Medication Delivery (1)
- Patient Safety (1)
- Precise Measurement (1)
- vaccines (1)
- blood lancets (1)
- Diabetic lancets (1)
- Finger Lancets (1)
- Insulin Pen Needles (1)
- Insulin Pens (1)
- Safety Lancets (1)
- 1 cc Insulin Syringe (1)
- 31 Gauge Insulin Syringe (1)
- 31 Gauge x 5/16 (1)
- 5/16 Inch Insulin Needles (1)
- Diabetes Insipidus (1)
- Diabetes Insulin Injection (1)
- Painless Insulin Injection (1)
- Safe Insulin Delivery (1)
- Short Needle Insulin Syringe (1)
- Syringe for Diabetes (1)
- 31 gauge x 5/8" (1)
- 56151-1732-01 (1)
- diabetic supplies (1)
- disposable insulin syringes (1)
- glucose control tools (1)
Insulin Syringes
Insulin Syringes
An insulin syringe is a medical syringe specifically designed for injecting insulin – the hormone used to control blood sugar – under the skin. It consists of a small plastic barrel (marked with graduated lines), a plunger, and a very fine needle. The syringe is filled by drawing insulin (from a vial or cartridge) into the barrel, and the plunger is then depressed to inject the insulin into the fatty tissue just under the skin (a subcutaneous injection) to enter the bloodstream. As one source explains, an insulin syringe’s “primary function [is] to draw up and inject insulin subcutaneously (under the skin) to help manage blood sugar levels.”. Because insulin doses are small, these syringes hold very small volumes (typically 1 milliliter or less) and have especially fine needles (usually 28–31 gauge) to minimize pain. The barrel is calibrated in insulin units (not just milliliters), so that each increment corresponds to a precise dose – for example, on a U-100 syringe each “unit” mark equals 0.01 mL of insulin.
Design and Features
Insulin syringes differ from general-purpose syringes mainly in scale and needle size. They come in only very small volumes and have extra fine needles. Common insulin syringe capacities are 0.3 mL, 0.5 mL, and 1.0 mL, corresponding to 30, 50, and 100 “units” of U-100 insulin (U-100 means 100 units per mL). Manufacturers typically color-code or label the plungers or packaging to indicate these sizes (for example, 0.3 mL syringes often have orange markings, 0.5 mL purple, etc.) for easy recognition. The needle is very thin – most often 28-, 29-, 30- or 31-gauge (a larger gauge number means a thinner needle) – and short (typically about 4–12 mm long) because insulin is delivered just under the skin. These dimensions strike a balance between comfort and effective delivery.
- Volume (capacity): Typically 0.3 mL (30 units), 0.5 mL (50 units), or 1.0 mL (100 units). Smaller syringes (e.g. 0.3 mL) are used for low-dose needs; larger (1 mL) for high-dose needs.
- Needle Gauge: Very fine – usually 28–31 gauge. A finer needle causes less discomfort.
- Needle Length: Generally 4–12 mm, just long enough to reach the fatty subcutaneous tissue. Shorter needles reduce the chance of injecting into muscle.
- Calibrations: The barrel is marked in insulin units (each line = 1 unit, etc.) rather than plain milliliters. This ensures that patients can measure out exactly the prescribed number of insulin units.
Because of these features, any two insulin syringes of the same type (e.g. U-100 “1 mL”) are interchangeable in function. In fact, manufacturers note there is “no mechanical difference between children’s and adult’s nebulizers,” and similarly no special “pediatric” insulin syringe – they all work the same, though pediatric syringes may have smaller volume and fun designs.
Uses in Diabetes Management
Insulin syringes are the standard tool for people with diabetes who must inject insulin. As a UK diabetes guide notes, “direct subcutaneous insulin injection remains the most common form of delivery, using a needle and syringe.”. Patients (or caregivers) use them to self-administer insulin at home or in clinics, usually injecting into fatty areas like the abdomen, thigh, buttock or upper arm. Several medical resources emphasize that insulin syringes are engineered for accurate self-dosing: their fine graduations and user-friendly design help patients draw up the exact prescribed dose. For example, one diabetes resource explains that these syringes “allow patients to measure and inject the exact amount of insulin needed,” which makes blood sugar control much more precise. In practice, the user inserts the needle under the skin and slowly depresses the plunger; the insulin mist is then absorbed over minutes, as shown in usage diagrams.
Insulin syringe injections are typically quick (just a few seconds) and almost painless due to the thin needle. Because of their design, patients can reliably administer insulin multiple times a day. This method gives rapid but controlled insulin uptake to match blood glucose needs. Compared to oral medications, injectable insulin via syringe works more quickly to lower blood sugar with minimal systemic side effects. And compared to newer devices like insulin pen injectors or pumps, syringes remain widely used because they are simple, low-cost and readily available. (Patients choosing syringe vs pen or pump often depend on personal preference, age, dexterity, cost and insulin type.)
Care and Safety
Insulin syringes are disposable and sterile. They come individually wrapped and should be discarded after use. Guidelines strongly emphasize safe use: only the intended user should touch the syringe. A diabetes care guide advises that it’s “advisable to use disposable syringes” and never to share one between people. (Some patients may reuse their own syringe up to a few times if needed, but it must never be shared or used by someone else.) After injection, the used syringe should be placed in a proper sharps/needle container for safe disposal – this prevents needlestick injuries or hygiene issues. Practicing good injection technique (rotating sites, using fresh syringes, proper disposal) maximizes the benefits of insulin therapy.
In summary, insulin syringes are essential medical tools for diabetics. They are simply miniature syringes optimized for insulin: very small (≤1 mL), with very fine short needles, and calibrated in insulin units. By turning liquid insulin into a precise, inhalable dose under the skin, they enable people with diabetes to control blood glucose effectively. With correct use and hygiene, insulin syringes provide a safe, convenient, and accurate way to maintain blood sugar control as prescribed by healthcare providers
-
 Sale 23%
Original price $ 19.95Current price $ 15.35
Sale 23%
Original price $ 19.95Current price $ 15.35Insulin Syringes with Needle U-100, All Size Insulin Needles, Easy Touch 100/Box
MHC44 reviewsEasyTouch insulin syringes are simply a branded line of standard “U-100” insulin syringes made by MHC Medical (sold under the EasyTouch name). In o...
View full details -
 Sale 40%
Original price $ 39.95Current price $ 23.95
Sale 40%
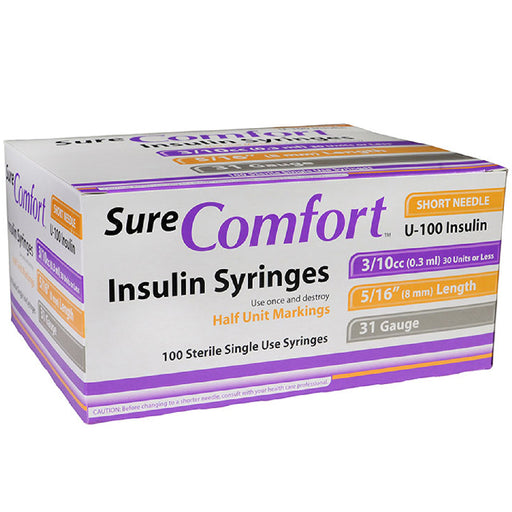
Original price $ 39.95Current price $ 23.95Insulin Syringes 31 Gauge 3/10cc (0.3 ml) with 5/16 Length Sure Comfort 100/Box
Allison Medical1 reviewSure Comfort Insulin Syringes 31 Gauge 3/10CC are designed to allow for quick and easy administration of insulin injections. They are made with hig...
View full details -
 Sale 15%
Original price $ 46.95Current price $ 39.90
Sale 15%
Original price $ 46.95Current price $ 39.9029 Gauge x ½" Monoject 1 mL Insulin Syringes, Safety 1 cc, Permanent Needle, 100/box
Cardinal HealthNo reviewsMonoject 8881511110 1mL Insulin Syringes, 1cc, 29 gauge x ½" Needle are a sterile. safety syringes used to deliver diabetic insulin from a vial in...
View full details -
 Sale 28%
Original price $ 89.95Current price $ 65.00
Sale 28%
Original price $ 89.95Current price $ 65.00Insulin Syringe 31 Gauge 5/16 inch, 0.3 mL Ultra-Fine, 100/box
Embecta MedicalNo reviewsShop Insulin Syringes Online for Fast, Accurate Insulin Delivery! Embecta Medical’s Insulin Syringe 31 Gauge 5/16 inch, 0.3 mL Ultra-Fine offers sa...
View full details -
 Sale 24%
Original price $ 105.00Current price $ 79.95
Sale 24%
Original price $ 105.00Current price $ 79.9530 gauge x 1/2" Insulin Syringes 1 mL with Ultra-Fine Needle 1 mL, 100 Count
EmbectaNo reviewsThe Preferred Choice for Safe & Comfortable Insulin Injections Take your diabetes care to the next level with Embecta’s 30 Gauge x 1/2" Insulin...
View full details -
 Sale 34%
Original price $ 67.95Current price $ 45.00
Sale 34%
Original price $ 67.95Current price $ 45.00Insulin Syringes 28 Gauge x 1/2 inch, 1 mL Micro-Fine Needle U-100 Embecta 329424 Sterile 100/Box
Embecta2 reviewsMicrofine U-100 Insulin Syringes 1 mL, 28 Gauge x 1/2 inch have extremely fine, 28-gauge needles that are just 1/2 inch long. This makes them perfe...
View full details -
 Sale 29%
Original price $ 33.95Current price $ 23.95
Sale 29%
Original price $ 33.95Current price $ 23.95Insulin Syringes 31 gauge x 5/16", 0.3 mL by SureComfort 100/Box
Allison MedicalNo reviewsGet Painless, Accurate Insulin Injections – Trusted by Diabetes Care Experts Take control of your diabetes management with SureComfort Insulin Syri...
View full details -
 Sale 17%
Original price $ 99.95Current price $ 83.00
Sale 17%
Original price $ 99.95Current price $ 83.00Ultra-Fine Insulin Syringes 0.3 mL with 8 mm x 31 gauge Insulin Needle 100/box -BD 328438
BD2 reviewsPremium Diabetes Supply for Safe, Accurate Insulin Injection – Trusted, Comfortable, and Painless Delivery Ultra-Fine Insulin Syringes 0.3mL with N...
View full details -
 Sale 25%
Original price $ 99.95Current price $ 75.00
Sale 25%
Original price $ 99.95Current price $ 75.00BD 30 gauge x 1/2" Insulin Syringes 0.3 mL with Ultra-Fine Needle, Non-Safety 100/box
BDNo reviewsBD 328431 Insulin Syringes are designed for injecting insulin into the subcutaneous tissue just under the skin. They are used by people with diabet...
View full details -
 Sale 23%
Original price $ 64.00Current price $ 49.25
Sale 23%
Original price $ 64.00Current price $ 49.25BD Insulin Syringes 31 gauge x 3/10 mL Ultra-Fine Needle 6mm, Sterile 90/box
BD1 reviewThe Ultimate in Comfort, Precision, and Safety for Diabetes Management Achieve accurate, comfortable, and safe insulin injections with the BD Insul...
View full details -
 Sale 43%
Original price $ 38.95Current price $ 22.15
Sale 43%
Original price $ 38.95Current price $ 22.15Monoject Insulin Safety Syringes with 29 Gauge x 1/2" Permanent Needle, 50 Per Box
Cardinal HealthNo reviewsMonoject Magellan Insulin Safety Syringes with 29 Gauge x 1/2" Permanent Needle, 50 Per Box. Monoject™ Magellan™ Insulin Safety Syringes are integr...
View full details -
 Sale 24%
Original price $ 105.00Current price $ 79.95
Sale 24%
Original price $ 105.00Current price $ 79.95Insulin Syringes 31 g x 8 mm, 1 mL with Ultra-Fine Needle 100/box Embecta 328418
Embecta1 reviewBest for Comfortable and Accurate Insulin Injections Insulin Syringes 31g x 8mm, 1 mL Ultra-Fine Needle (SKU: 328418) are the #1 choice for diabeti...
View full details -
 Sale 25%
Original price $ 99.95Current price $ 75.00
Sale 25%
Original price $ 99.95Current price $ 75.00BD 328466 Insulin Syringes 0.5 mL with Ultra-Fine Needle 12.7mm x 30 Gauge, 100/box
EmbectaNo reviewsSimplify your diabetes management with BD 328466 Insulin Syringes. Expertly crafted by BD, each 0.5 mL syringe features an Ultra-Fine 12.7mm x 30G ...
View full details -
 Sale 19%
Original price $ 89.95Current price $ 72.95
Sale 19%
Original price $ 89.95Current price $ 72.95Insulin Syringes 31 gauge x 3/10 mL with Ultra-Fine Needle 6mm x 31 G by Embecta 100/box
EmbectaNo reviews#1 Doctor-Recommended Insulin Syringes for Safe, Comfortable, and Accurate Insulin Injections Looking for the best insulin syringes for diabetes ma...
View full details -
 Sale 21%
Original price $ 99.95Current price $ 78.90
Sale 21%
Original price $ 99.95Current price $ 78.90BD Insulin Syringes 31 Gauge x 1/2" with Ultra-Fine Needle 6mm Sterile (10-Packs) 100/box
EmbectaNo reviewsOptimize your insulin administration with BD Veo Insulin Syringes by Embecta. Featuring a 0.5 mL capacity and an Ultra-Fine 6mm x 31G needle, these...
View full details -
 Sale 24%
Original price $ 109.95Current price $ 84.00
Sale 24%
Original price $ 109.95Current price $ 84.00BD Ultra-Fine Original Pen Needles 12.7mm x 29G, 100/box
BDNo reviewsBD 328203 Ultra-Fine Original Pen Needles 12.7mm x 29 gauge are great for those on injectable medication. It is the premium choice sought after by ...
View full details -
 Sale 24%
Original price $ 59.95Current price $ 45.75
Sale 24%
Original price $ 59.95Current price $ 45.75BD Microfine Insulin Syringe 27 Gauge x 5/8 Inch, 1 mL, 100/Box
EmbectaNo reviewsBD 329412 Microfine Insulin Syringe 27 Gauge x 5/8 Inch is a highly effective and widely used tool in the world of diabetes management. This top of...
View full details🔒 Medical License Required -
 Sale 39%
Original price $ 38.95Current price $ 23.95
Sale 39%
Original price $ 38.95Current price $ 23.95Insulin Syringes 30 g x 5/16" 0.5 mL, Sterile by Sure Comfort 100/Box
Allison Medical2 reviewsAllison Medical 22-6005 Sure Comfort Insulin Syringes are medical devices used for injecting insulin into the body for diabetes management. These s...
View full details -
 Sale 27%
Original price $ 32.95Current price $ 23.95
Sale 27%
Original price $ 32.95Current price $ 23.95Insulin Syringes 30g x 5/16", 1 mL Sterile by Sure Comfort 100/Box
Allison MedicalNo reviewsAllison Medical 22-6010 Sure Comfort Insulin Syringes 30g x 5/16" 1 mL are a type of syringe specifically designed for use with insulin injections....
View full details -
 Sale 20%
Original price $ 29.95Current price $ 23.95
Sale 20%
Original price $ 29.95Current price $ 23.95Sure Comfort Insulin Syringes 29 gauge x 1/2" 0.3 mL (100/Count)
Allison MedicalNo reviewsAllison Medical 22-9003 Sure Comfort Insulin Syringes 29 gauge x 1/2" 0.3 mL. Allison Medical 22-9003 Sure Comfort Insulin Syringes are used for ad...
View full details -
 Sale 35%
Original price $ 36.95Current price $ 23.95
Sale 35%
Original price $ 36.95Current price $ 23.95Insulin Syringes 29 gauge x 1/2" 0.5 mL Sure Comfort (100/Count)
Allison Medical1 reviewSure Comfort Insulin Syringes 29 gauge x 1/2" 0.5 mL are designed for the precise and comfortable administration of insulin to individuals with dia...
View full details -
 Sale 20%
Original price $ 29.95Current price $ 23.95
Sale 20%
Original price $ 29.95Current price $ 23.95Sure Comfort Insulin Syringes 29 gauge x 1/2" 1 mL (100/Count)
Allison MedicalNo reviewsAllison Medical 22-9010 Sure Comfort Insulin Syringes 29 gauge x 1/2" 1 mL. Allison Medical 22-9010 Sure Comfort Insulin Syringes are syringes used...
View full details -
 Sale 25%
Original price $ 31.95Current price $ 23.95
Sale 25%
Original price $ 31.95Current price $ 23.95Insulin Syringes 30 g x 1/2", 0.3 mL, Sterile by Sure Comfort 100/Box
Allison MedicalNo reviews#1 Best Seller for Comfort, Accuracy, and Safety Control your diabetes with confidence! The Sure Comfort Insulin Syringes 30 gauge x 1/2 inch, 0.3 ...
View full details -
 Sale 23%
Original price $ 38.95Current price $ 29.95
Sale 23%
Original price $ 38.95Current price $ 29.95Insulin Syringes 28 gauge x 1/2"(12.7 mm) 0.5 mL Regular Needle by Ulticare 100/Box
Uti MedNo reviewsUlticare Insulin Syringes 28 gauge x 1/2" (12.7 mm) 0.5 mL Regular Needle are designed for the precise administration of insulin in individuals wit...
View full details -
 Sale 25%
Original price $ 145.95Current price $ 109.00
Sale 25%
Original price $ 145.95Current price $ 109.00VanishPoint 29 gauge x 5/16 inch Retractable Insulin Syringe with Needle 1 mL, Regular Wall, 100/Box
Retractable TechnologiesNo reviewsVanishPoint Safety Syringe is a type of syringe that is designed with a retractable needle. This feature allows the needle to retract into the syri...
View full details -
 Sale 33%
Original price $ 45.00Current price $ 29.95
Sale 33%
Original price $ 45.00Current price $ 29.95BD Plastipak 3 mL General Purpose Syringe with Luer Lok Tip Without Safety 200/Box
BDNo reviewsExperience precision with BD Plastipak 3 mL Syringe, featuring a Luer Lok Tip for secure connections. Essential for safe and accurate healthcare us...
View full details -
 Sale 25%
Original price $ 129.95Current price $ 97.00
Sale 25%
Original price $ 129.95Current price $ 97.00Insulin Pen Needles Ultra-Fine 31 gauge x 5mm (100/box) BD 320119
EmbectaNo reviewsThe BD Ultra-Fine Mini pen needle is 31 gauge, 5 mm (3/16"). It's the shortest insulin pen needle in the world, and no insulin pen needle is thinne...
View full details -
 Sale 29%
Original price $ 24.95Current price $ 17.59
Sale 29%
Original price $ 24.95Current price $ 17.59Insulin Syringes 31 Gauge x 5/16", 1 cc Individually Wrapped, 100/box
DynarexNo reviewsTake control of diabetes care with Insulin Syringes 31 Gauge x 5/16", 1 cc (100/box, Individually Wrapped) – the trusted choice for comfortable, ac...
View full details -
 Sale 24%
Original price $ 19.95Current price $ 15.25
Sale 24%
Original price $ 19.95Current price $ 15.25Insulin Syringes 31 gauge x 5/8", 0.5 mL by Leader 100/Box
LeaderNo reviewsFast, Safe & Accurate Insulin Injection Leader Insulin Syringes 31 gauge x 5/8", 0.5 mL provide precise and comfortable insulin delivery for di...
View full details
People Also Searched For
Insulin Syringes
An insulin syringe is a medical syringe specifically designed for injecting insulin – the hormone used to control blood sugar – under the skin. It consists of a small plastic barrel (marked with graduated lines), a plunger, and a very fine needle. The syringe is filled by drawing insulin (from a vial or cartridge) into the barrel, and the plunger is then depressed to inject the insulin into the fatty tissue just under the skin (a subcutaneous injection) to enter the bloodstream. As one source explains, an insulin syringe’s “primary function [is] to draw up and inject insulin subcutaneously (under the skin) to help manage blood sugar levels.”. Because insulin doses are small, these syringes hold very small volumes (typically 1 milliliter or less) and have especially fine needles (usually 28–31 gauge) to minimize pain. The barrel is calibrated in insulin units (not just milliliters), so that each increment corresponds to a precise dose – for example, on a U-100 syringe each “unit” mark equals 0.01 mL of insulin.
Design and Features
Insulin syringes differ from general-purpose syringes mainly in scale and needle size. They come in only very small volumes and have extra fine needles. Common insulin syringe capacities are 0.3 mL, 0.5 mL, and 1.0 mL, corresponding to 30, 50, and 100 “units” of U-100 insulin (U-100 means 100 units per mL). Manufacturers typically color-code or label the plungers or packaging to indicate these sizes (for example, 0.3 mL syringes often have orange markings, 0.5 mL purple, etc.) for easy recognition. The needle is very thin – most often 28-, 29-, 30- or 31-gauge (a larger gauge number means a thinner needle) – and short (typically about 4–12 mm long) because insulin is delivered just under the skin. These dimensions strike a balance between comfort and effective delivery.
- Volume (capacity): Typically 0.3 mL (30 units), 0.5 mL (50 units), or 1.0 mL (100 units). Smaller syringes (e.g. 0.3 mL) are used for low-dose needs; larger (1 mL) for high-dose needs.
- Needle Gauge: Very fine – usually 28–31 gauge. A finer needle causes less discomfort.
- Needle Length: Generally 4–12 mm, just long enough to reach the fatty subcutaneous tissue. Shorter needles reduce the chance of injecting into muscle.
- Calibrations: The barrel is marked in insulin units (each line = 1 unit, etc.) rather than plain milliliters. This ensures that patients can measure out exactly the prescribed number of insulin units.
Because of these features, any two insulin syringes of the same type (e.g. U-100 “1 mL”) are interchangeable in function. In fact, manufacturers note there is “no mechanical difference between children’s and adult’s nebulizers,” and similarly no special “pediatric” insulin syringe – they all work the same, though pediatric syringes may have smaller volume and fun designs.
Uses in Diabetes Management
Insulin syringes are the standard tool for people with diabetes who must inject insulin. As a UK diabetes guide notes, “direct subcutaneous insulin injection remains the most common form of delivery, using a needle and syringe.”. Patients (or caregivers) use them to self-administer insulin at home or in clinics, usually injecting into fatty areas like the abdomen, thigh, buttock or upper arm. Several medical resources emphasize that insulin syringes are engineered for accurate self-dosing: their fine graduations and user-friendly design help patients draw up the exact prescribed dose. For example, one diabetes resource explains that these syringes “allow patients to measure and inject the exact amount of insulin needed,” which makes blood sugar control much more precise. In practice, the user inserts the needle under the skin and slowly depresses the plunger; the insulin mist is then absorbed over minutes, as shown in usage diagrams.
Insulin syringe injections are typically quick (just a few seconds) and almost painless due to the thin needle. Because of their design, patients can reliably administer insulin multiple times a day. This method gives rapid but controlled insulin uptake to match blood glucose needs. Compared to oral medications, injectable insulin via syringe works more quickly to lower blood sugar with minimal systemic side effects. And compared to newer devices like insulin pen injectors or pumps, syringes remain widely used because they are simple, low-cost and readily available. (Patients choosing syringe vs pen or pump often depend on personal preference, age, dexterity, cost and insulin type.)
Care and Safety
Insulin syringes are disposable and sterile. They come individually wrapped and should be discarded after use. Guidelines strongly emphasize safe use: only the intended user should touch the syringe. A diabetes care guide advises that it’s “advisable to use disposable syringes” and never to share one between people. (Some patients may reuse their own syringe up to a few times if needed, but it must never be shared or used by someone else.) After injection, the used syringe should be placed in a proper sharps/needle container for safe disposal – this prevents needlestick injuries or hygiene issues. Practicing good injection technique (rotating sites, using fresh syringes, proper disposal) maximizes the benefits of insulin therapy.
In summary, insulin syringes are essential medical tools for diabetics. They are simply miniature syringes optimized for insulin: very small (≤1 mL), with very fine short needles, and calibrated in insulin units. By turning liquid insulin into a precise, inhalable dose under the skin, they enable people with diabetes to control blood glucose effectively. With correct use and hygiene, insulin syringes provide a safe, convenient, and accurate way to maintain blood sugar control as prescribed by healthcare providers





























