Naltrexone
Naltrexone is a prescription medication used to help people recover from opioid or alcohol addiction. It belongs to the drug class opioid antagonists, meaning it binds to opioid receptors in the brain but does not activate them By occupying these receptors, naltrexone blocks the effects of opioid drugs (heroin, prescription painkillers, etc.) – patients feel no euphoria or sedation if they use opioids while on naltrexone. This blockade also extends to opioid-like effects of alcohol, which can help reduce alcohol craving and use. Naltrexone itself has no abuse potential or sedative effect and is not addictive. Importantly, it does not relieve withdrawal symptoms and should only be started once a person is fully detoxified. (Starting naltrexone too soon can trigger acute withdrawal on someone who still has opioids in their system.)
Naltrexone works by blocking brain opioid receptors. This competitive antagonism prevents opioids from producing reward or sedation. Unlike opioid drugs, naltrexone does not activate these receptors, so it causes no “high,” no physical dependence, and no withdrawal when discontinued. If a patient takes opioid medication while on naltrexone, the opioid has little to no effect – this property helps break the cycle of addiction. Because naltrexone has very high affinity for the mu-opioid receptor, it must be used after withdrawal: patients typically wait about 7–10 days after their last short-acting opioid (or 10–14 days after a long-acting opioid) before beginning naltrexone.
Uses and Administration
Naltrexone is FDA-approved to support abstinence in both opioid use disorder (OUD) and alcohol use disorder (AUD). It is always used with counseling and support services as part of a comprehensive treatment program. Common clinical uses include:
-
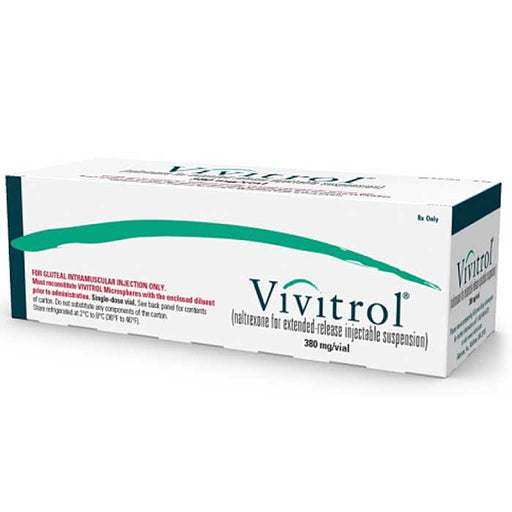
Opioid use disorder: After medically supervised detox from opioids, patients receive naltrexone to prevent relapse. The long-acting injectable form (380 mg intramuscular once monthly) is approved for this purpose. Naltrexone blocks any opioids taken, so it removes the incentive to use. Patients must have gone 1–2 weeks without opioids before starting.
-
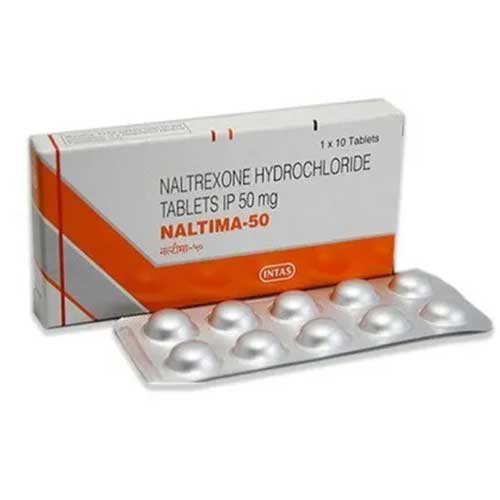
Alcohol use disorder: Naltrexone (usually 50 mg by mouth daily) helps people who have recently stopped drinking to avoid relapse. It reduces the rewarding effects of alcohol and diminishes cravings. Unlike disulfiram or some other medications, naltrexone does not punish drinking with sickness – instead it simply blunts the “high” from alcohol.
-
Weight management (obesity): In combination with bupropion, naltrexone is approved (as the brand Contrave) to aid in weight loss for obese patients. This use exploits naltrexone’s effect on reward pathways and appetite. (This is a different indication than addiction treatment.)
Naltrexone is available in two main formulations. The oral tablet (50 mg) is taken daily, typically under the brand names ReVia or Depade. This form is often used for alcohol dependence. The extended-release injection (380 mg once every 4 weeks) is given by a healthcare provider (brand name Vivitrol) and is approved for both opioid and alcohol dependence. In all cases, naltrexone is only effective when the patient is already abstinent from the abused substance. It is not useful for detoxification itself or for people who are still actively using alcohol or opioids.
Naltrexone Side Effects
Naltrexone is generally well tolerated, but it can cause side effects (often mild to moderate). Common side effects include:
-
Gastrointestinal: nausea, vomiting, stomach cramps or gas, loss of appetite.
-
Neurologic: headache, dizziness, sleep disturbances (insomnia or fatigue).
-
Psychiatric/Mood: anxiety, nervousness, irritability or mood swings.
Because of these effects, patients are advised to take it with food or a snack if stomach upset occurs. Rare but serious side effects can include liver damage. Naltrexone, especially in high doses, can cause hepatotoxicity, so clinicians monitor liver enzymes. Anyone with acute hepatitis or severe liver disease should not take naltrexone. Other rare reactions (e.g. severe allergic reactions, confusion or hallucinations) have been reported.
Important precautions: Patients must completely stop opioids (and often alcohol) before starting naltrexone. Using naltrexone in someone who still has opioids in their system precipitates immediate withdrawal. Patients should avoid opioid painkillers, illicit opioids, or sedative drugs while on naltrexone, since these will have no effect and may be unsafe. Similarly, heavy drinking is discouraged when taking naltrexone for alcohol use disorder. Naltrexone is not recommended for those under 18 years old or for people with acute addiction or other unstable medical conditions.
Finally, an important clinical note: naltrexone reduces opioid tolerance. If a patient stops naltrexone (or misses doses) and then relapses to opioid use, even a previously normal dose of opioid can cause overdose, because their tolerance has dropped during abstinence on naltrexone. Patients are always warned about this risk and advised to be cautious if opioid use is resumed.
Naltrexone is an opioid-receptor blocker used to prevent relapse in opioid or alcohol addiction. It comes as a daily pill or a monthly injection, and works by eliminating the pleasurable effects of opioids/alcohol, thereby helping people maintain sobriety. It is non-addictive and does not cause withdrawal on its own, but requires careful medical supervision due to its effects on liver function and potentials for precipitated withdrawal.