Filters
- Adult Oxygen (1)
- Air Mask (1)
- Elongated Mask (2)
- Elongated Oxygen Mask (1)
- Hudson Rci (1)
- O2 Mask (4)
- Hudson RCI (6)
- Kids Mask (1)
- Oxygen delivery mask (1)
- Pediatric Oxygen Mask (3)
- 1040 (1)
- Adult Oxygen mask (6)
- HUD1040 (1)
- o2 mask (1)
- Adult Mask (4)
- o2 Mask (2)
- Tubing (2)
- Non rebreathing oxygen mask (4)
- Airlife (3)
- CareFusion AirLife (1)
- Medium concentration Oxygen Mask (1)
- Breathing Mask (1)
- Masks (1)
- Oxygen Concentrator (1)
- oxygen tank (1)
- Under the Chin (1)
- Venturi Style (1)
- Venturi Style Mask (1)
- Venturi-style Oxygen Mask (1)
- Childs masks (1)
- Non Rebreathing (2)
- Reservoir bag (1)
- Teleflex Medical (1)
- non rebreather (1)
- Oxygen Supply (1)
- extension tubing (1)
- Green Tubing (1)
- o2 tubing (2)
- oxygen supply (1)
- Non rebreather (1)
- extenstion tubing (1)
- Long Oxygen Tubing (1)
- oxygen tube (1)
- star tubing (1)
- Connector (4)
- Tubing connector (2)
- children (1)
- jar (1)
- kids (1)
- kids nebulizer mask (1)
- mask for kids (1)
- neb mask (1)
- nebulizer treatment (1)
- pediatric (1)
- pediatric mask (1)
- Male Connector (1)
- Parts (1)
- Aspirator (1)
- Aspirator tubing (1)
- Suction Machine (1)
- Tapered (1)
- Tubing Connector (1)
- Universal connector (1)
- Mask for Trach (1)
- Trach Mask (1)
- Tracheostomy (1)
- Tracheotomy Mask (1)
- Aerosol Mask (2)
- Asthma Mask (1)
- Nebulizer Mask (1)
- Respiratory (2)
- under the chin (1)
- White (1)
- 1742 (1)
- Aerosol medication (1)
- Air Entrainment Mask (1)
- high humidity entrainment (2)
- Multi-Vent Mask (1)
- Adjustable Mask (1)
- Select a Vent (1)
- Select-A-Vent Mask (1)
Oxygen Masks

An oxygen mask is a medical device that covers the nose and mouth to deliver supplemental oxygen. It connects to an oxygen source (tank or concentrator) and provides higher-than-air oxygen concentrations to the patient’s lungs. Oxygen therapy is used whenever a patient’s blood oxygen levels (SpO₂) are too low (hypoxemia) to safely meet tissue needs. Without enough oxygen, vital organs (brain, heart, kidneys) can suffer damage. Conditions that commonly cause hypoxemia include acute or chronic lung diseases (for example, pneumonia, asthma attacks, COPD exacerbations, pulmonary fibrosis), heart failure with pulmonary congestion, severe anemia, shock, and acute respiratory distress (e.g. ARDS or COVID-19 pneumonia). In all these cases, breathing oxygen helps raise blood oxygen levels and relieve shortness of breath. Oxygen therapy is treated like any medication: it requires a prescription and careful monitoring (via pulse oximetry or arterial blood gases). The goal is to maintain adequate oxygen saturation (usually 94–98% in most adults, or 88–92% in chronic respiratory patients).
Types of Oxygen Masks (and Related Devices)
A variety of masks and interfaces are used depending on how much oxygen the patient needs. Key types include:
-
Nasal Cannula: (Not a mask, but often used first.) This is a simple plastic tube with prongs in the nostrils. It provides low-flow oxygen (1–6 L/min), which raises FiO₂ by roughly 4% per liter (about 24–44% at 6 L/min). Because it is unobtrusive, it allows talking and eating. If flows exceed ~4 L/min, a humidifier is often added to prevent nose/throat dryness.
-
Simple Face Mask: Covers the mouth and nose and has vents on the sides for exhalation. It is used for moderate oxygen needs. Typical flow is 5–10 L/min (never below 5–6, to avoid rebreathing CO₂), delivering about 28–50% FiO₂. The mask has an elastic strap and a moldable nose clip for a better seal.
-
Venturi (Air-Entrainment) Mask: This mask delivers a precise, fixed oxygen concentration. It uses color-coded adapters to “entrain” room air at exact ratios. Depending on the adapter, it can deliver specific FiO₂ values (commonly 24%, 28%, 31%, 35%, 40%, or 50%). The flowmeter is set to the rate indicated by the adapter (the flows are relatively high but fixed by design). Venturi masks are ideal when a controlled FiO₂ is needed – for example, in COPD or other chronic lung disease patients where giving too much oxygen can depress respiratory drive.
-
Non-Rebreather (NRB) Mask: This mask has a reservoir bag and one-way valves so that the patient inhales almost pure oxygen and exhales into the mask vents (not the reservoir). It can deliver very high oxygen concentrations (up to 60–90% FiO₂) when flow is set correctly. The typical flow is 10–15 L/min, and importantly, the reservoir bag must never fully collapse (it should stay at least 1/3–1/2 full between breaths. NRB masks are used in emergencies or very severe hypoxia (e.g. in shock, major trauma, or acute severe asthma), where maximal oxygen is needed immediately. (Note: If oxygen flow ceases or valves fail, there’s a risk of suffocation, so one must never remove the mask until it’s safe to do so.)
-
Partial Rebreather Mask: Similar to a non-rebreather but without one-way valves. It also has a reservoir bag but allows the patient to rebreathe some of the exhaled air. It typically requires 10–15 L/min flow and delivers around 35–50% FiO₂. Partial rebreathers are less common today but may be used when high-flow half-rich oxygen is acceptable.
-
Pediatric Oxygen Masks: Children and infants use scaled-down versions of the masks above (simple, Venturi, NRB) to fit their faces safely. For tiny infants, an oxygen hood (a transparent dome) or flowy oxygen tent may be used instead of a mask.
-
Noninvasive Ventilation Masks: (CPAP/BiPAP) These are tight-fitting masks connected to machines that provide pressurized oxygen or air (for example, in respiratory failure). Though not simple “masks” for passive O₂, they are important to mention as advanced oxygen-delivery devices.
-
Bag-Valve Mask (Resuscitator): In emergency situations, a hand-held bag-mask (Ambu bag) delivers oxygen or room air when the patient is not breathing adequately or at all. This is a specialized usage beyond routine oxygen therapy.
When Is Oxygen Mask Therapy Needed?
Oxygen masks are used for hypoxemia – when blood oxygen is dangerously low. Nurses and doctors typically look at the patient’s oxygen saturation (SpO₂): fall below ~90–92% on room air (or show signs of respiratory distress), and it’s time for oxygen. Situations include:
- Respiratory diseases: e.g. Pneumonia (bacterial or viral) – the inflamed lungs don’t exchange O₂ well; Asthma exacerbations – airway constriction leads to hypoxia; Chronic Obstructive Pulmonary Disease (COPD) flare-ups – long-term lung damage causes chronically low O₂; Pulmonary fibrosis or other interstitial lung disease; etc.
- Cardiac/vascular causes: e.g. Acute heart failure (fluid in lungs), pulmonary embolism, or shock – when blood isn’t getting to the lungs or lungs are flooded.
- High Altitude or Decompression: Low environmental oxygen.
- Anemia: Very low hemoglobin can cause low oxygen delivery; O₂ can help while fixing the anemia.
- During or after surgery/trauma: Anesthesia or injury can impair breathing; oxygen is often given prophylactically or therapeutically.
- Toxic exposures: Carbon monoxide poisoning and smoke inhalation victims are given 100% O₂.
- Emergency resuscitation: Any respiratory arrest or arrest situation zones in on high-oxygen support.
In all cases, indications for giving oxygen are signs or measurements of inadequate oxygenation (fast breathing, confusion or deterioration, low SpO₂). Nurses often have standing orders allowing them to start O₂ if saturations are below a threshold (commonly <92–94%). Once started, oxygen is titrated to keep SpO₂ in the target range (normally ≥94%, or 88–92% in certain COPD patients).
How to Apply Oxygen Masks
Preparing: Confirm the order (e.g. “O₂ at 6 L by mask”) and gather supplies: the correct mask type, oxygen source, and connecting tubing. Check the flowmeter and regulator, and ensure oxygen is flowing (with no kinks or leaks). If using a reservoir (NRB/partial), squeeze it to partially inflate before placement.
Placement: Secure the mask on the patient. For face masks, place it over the nose and mouth; loop the elastic band around the back of the head. Pinch the nose piece for a tight fit. For a nasal cannula, insert prongs into nostrils and drape tubing over the ears, tightening the slider under the chin. Ensure the mask seats well: watch for leaks around the edges or a floppy cannula. The patient should breathe normally; you may need to instruct them gently because having a mask on can be unsettling at first.
Flow Settings: Adjust the flowmeter to the prescribed setting. Typical flows:
- Simple face mask: 6–10 L/min (this yields about 28–50% O₂).
- Venturi mask: Set flow according to the adaptor (usually 4–15 L/min) to achieve the ordered FiO₂ (24–60%).
- Non-rebreather: 10–15 L/min (the bag must stay inflated).
- Nasal cannula: 1–6 L/min (each liter adds ~4% FiO₂.
Always verify the patient’s SpO₂ after a few minutes to ensure adequate response. If the saturation remains low, follow protocols to increase flow or change device, and notify the provider.
Ongoing Care: The patient may remove the mask briefly to eat unless otherwise instructed (provide a nasal cannula if needed). Remind them not to adjust the dial themselves – oxygen is not self-regulated. Nurses should intermittently check the mask fit, patency of tubing, and comfort level. Document the oxygen device, flow, and patient’s SpO₂ and respiratory status in the chart. When it’s time to wean, gradually reduce flow while monitoring saturation and work of breathing.
Helpful Tips and Important Safety Information
-
Oxygen “Fuel” Hazard: Oxygen greatly accelerates fires. Never smoke or allow open flames around oxygen equipment. Maintain a 6–10 foot “no-smoking” zone. Keep electrical appliances and heaters at a safe distance. Check that electrical devices and bulbs are functioning properly, as sparks could ignite enriched oxygen. Store oxygen cylinders upright and secure them to prevent tipping. In the home setting, install working smoke detectors and have a fire extinguisher available.
-
No Grease or Petroleum: Do not use oily or petroleum-based products (like Vaseline) on or near your face, lips, or inside the nostrils while on oxygen. Such substances can spontaneously ignite in the presence of concentrated oxygen. Use only approved water-based or saline moisturizers for dry nasal passages.
-
Humidification and Comfort: High-flow oxygen can dry out the mucous membranes. If the patient complains of dryness or thick secretions, a humidifier attachment (sterile water) may be indicated. Encourage the patient to drink plenty of fluids to stay hydrated (as this thins secretions). Warm, moist compresses or nasal saline sprays can also relieve dryness (never use petroleum jelly).
-
Skin and Comfort: Check the skin around masks and cannulas regularly. Irritation can occur at pressure points (over the nose or behind ears). Use gauze padding under straps or nasal prongs if needed. Adjust straps for comfort – the mask should seal but not painfully pinch. If the patient feels claustrophobic, reassure them and allow short breaks if oxygenation permits.
-
Monitoring: Nurses should continuously monitor respiratory rate and SpO₂. Improvement (saturation rising into target range, slower breathing, mental clarity) indicates therapy is working. Watch for signs of oxygen toxicity or carbon dioxide retention: headache, confusion, or lethargy may mean the flow is too high for certain patients (especially those with COPD). Follow orders for regular ABGs if the patient’s condition requires it.
-
Prescribed Therapy: Oxygen is essentially a medication. Never increase or decrease the flow without a doctor’s order (or standing protocol). Even though it seems helpful, giving “too much” oxygen can actually cause harm (hyperoxia), just as too little causes hypoxia. Target saturations are set for a reason. For example, nurses commonly give O₂ if SpO₂ falls below ~92% but hold off if it is ≥ 94–96%.
-
Patient Education: Teach the patient about using their device (especially at home). Show them how to read the flowmeter, and stress that only prescribed settings are allowed. If they have portable oxygen, instruct them on checking tank levels (gauge) and ensuring the cannula/mask is properly secured. Emphasize never to smoke near the device and to keep it upright. If any new symptoms occur (worsening breathlessness, dizziness, etc.), they should tell a healthcare provider promptly.
-
Travel/Home Safety: If the patient is on home oxygen, ensure they have enough supply (portable tank or concentrator batteries) before going out to avoid running out of oxygen. Store cylinders safely, and have an emergency plan. Remind everyone: in case of fire, turn off the oxygen source and evacuate immediately.
By following these guidelines, oxygen masks can be used effectively and safely. In summary, oxygen masks deliver needed oxygen directly to improve blood oxygen levels in patients with respiratory compromise. Proper device selection (simple mask, Venturi, NRB, etc.) depends on how much O₂ the patient needs, and strict safety measures (no smoking, correct flow, monitoring) protect the patient and caregivers. When applied and monitored correctly, oxygen mask therapy can greatly relieve hypoxia in many lung, heart, and critical illnesses.
-
 Sale 30%
Original price $ 1.79Current price $ 1.26
Sale 30%
Original price $ 1.79Current price $ 1.26Adult Oxygen Mask with 7 Foot tubing Elongated
24 reviewsAdult Oxygen Mask is a clear, elongated adult oxygen mask used to supply therapeutic oxygen to a person with a respiratory illness. The medium conc...
View full details -
 Sale 25%
Original price $ 2.59Current price $ 1.94
Sale 25%
Original price $ 2.59Current price $ 1.94Pediatric Oxygen Mask with 7 Foot Tubing
2 reviewsKids Pediatric Oxygen Mask is a soft, medium concentration supply mask with 7 foot tubing that delivers therapeutic oxygen to children with respira...
View full details -
 Sale
$ 6.50
Sale
$ 6.50Oxygen Mask, Adult with 7 foot Tubing
6 reviewsHudson RCI 1040 Adult Oxygen Mask is a comfortable and efficient oxygen delivery mask for respiratory patients. This oxygen mask features a medium-...
View full details -
 Sale 16%
Original price $ 1.65Current price $ 1.39
Sale 16%
Original price $ 1.65Current price $ 1.39Oxygen Mask, Adult with 7 foot Tubing
6 reviewsAdult Vinyl Oxygen Mask 7 ft, Medium Concentration, Latex-free, is a disposable o2 mask used for oxygen delivery to a patient. This oxygen mask fea...
View full details -
 Sale 46%
Original price $ 2.59Current price $ 1.40
Sale 46%
Original price $ 2.59Current price $ 1.40Pediatric Oxygen Mask Non-Rebreather Style with 7 foot tubing and Safety Vent
3 reviewsDynarex Pediatric Oxygen Mask with Non Rebreather Bag is specifically designed to provide high-concentration oxygen delivery to pediatric patients....
View full details -
 Sale 38%
Original price $ 1.59Current price $ 0.98
Sale 38%
Original price $ 1.59Current price $ 0.98Oxygen Mask, Adult Elongated with 7 foot Tubing
3 reviewsDynarex Adult Oxygen Mask is an effective method for medium concentration delivery of oxygen to respiratory patients. This oxygen mask features hig...
View full details -
 Sale 28%
Original price $ 1.95Current price $ 1.40
Sale 28%
Original price $ 1.95Current price $ 1.40Non-Rebreather Oxygen Mask, Elongated Shape, Adult Size with 7 foot Tubing & Safety Vent
4 reviewsNon-Rebreathing Oxygen Masks are used to deliver high concentrations of oxygen to patients in need of significant respiratory support. They feature...
View full details -
 Sale 46%
Original price $ 8.99Current price $ 4.89
Sale 46%
Original price $ 8.99Current price $ 4.89Venturi-Style Oxygen Mask with U Connect-It Tubing by AirLife
2 reviewsVenturi-Style Oxygen Mask with U Connect-It Tubing is a type of oxygen mask that is designed to deliver a specific oxygen concentration to a patien...
View full details -
 Sale
$ 5.55
Sale
$ 5.55Pediatric Non Rebreathing Oxygen Mask, Salter Labs
No reviewsSalter Labs 1130 Oxygen Mask is a high-concentration, non-rebreathing oxygen face mask used for respiratory care on pediatric patients. This oxygen...
View full details -
 Sold out
Original price $ 1.29Current price $ 0.79
Sold out
Original price $ 1.29Current price $ 0.79Oxygen Mask, Adult Elongated with 7 Foot Tubing
3 reviewsDynarex disposable oxygen mask has a soft vinyl plastic that conforms and contours to the shape of your face. Made with latex free materials for pe...
View full details -
 Sale 41%
Original price $ 5.25Current price $ 3.10
Sale 41%
Original price $ 5.25Current price $ 3.10Non-Rebreathing Oxygen Mask, Adult with 7foot tubing, Universal Connector and vent
1 reviewHudson Adult Non-Rebreathing Oxygen Mask with 7' tubing and Universal Connector is a low-resistance check valve prevents rebreathing and allows exh...
View full details -
 Sale
$ 4.95
Sale
$ 4.95Elongated Non Rebreathing Oxygen Mask SunMed Salter Labs
2 reviewsSalter Labs 8130 Elongated Non-Rebreathing Mask is an oxygen mask, designed for high-concentration oxygen delivery. This non-rebreathing oxygen mas...
View full details -
 Sale 29%
Original price $ 0.79Current price $ 0.56
Sale 29%
Original price $ 0.79Current price $ 0.56Oxygen Supply Extension Tubing 7 Foot
15 reviewsOxygen tubing is a clear supply tubing used to deliver therapeutic oxygen to a patients airways. Made with a 5-channel star interior to prevent oxy...
View full details -
 Sale 19%
Original price $ 7.35Current price $ 5.98
Sale 19%
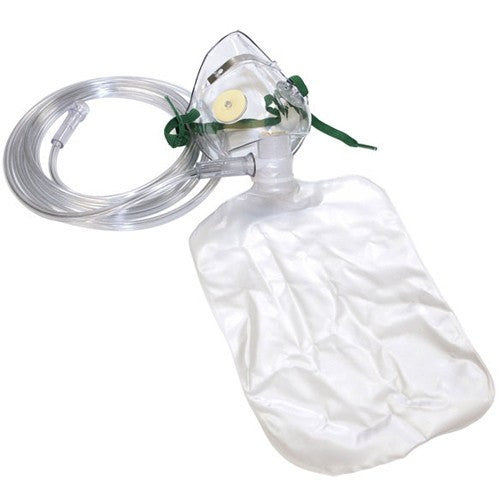
Original price $ 7.35Current price $ 5.98Salter Labs Non-Rebreather Adult Oxygen Mask with 7 foot tubing
10 reviewsSalter 8140 High Concentration Oxygen Mask is a non-rebreather adult oxygen mask designed to handle concentartion levels of therapeutic medical oxy...
View full details -
 Sale 37%
Original price $ 2.95Current price $ 1.85
Sale 37%
Original price $ 2.95Current price $ 1.85Oxygen Tubing 25 Foot Length
20 reviewsOxygen Extension Tubing 25 Foot Length is a star-lumen tubing used with oxygen concentrators, oxygen masks and nasal cannulas to add extra length. ...
View full details -
 Sale
$ 2.49
Sale
$ 2.49Kink-Free Swivel Oxygen Tubing Connector w/ Security Clip, White
17 reviewsSalter Labs 1220-0 Kink-Free Swivel Oxygen Tubing Connector with Security Clip is designed to eliminate the tangling, twisting, and kinking of oxyg...
View full details -
 Sale 55%
Original price $ 0.87Current price $ 0.39
Sale 55%
Original price $ 0.87Current price $ 0.39Treaded Oxygen Tubing Connector
10 reviewsTreaded Oxygen Tubing Connector is double-male end connector used with nasal cannulas, oxygen masks and other respiratory devices. Unique design, a...
View full details -
 Sale 11%
Original price $ 3.87Current price $ 3.45
Sale 11%
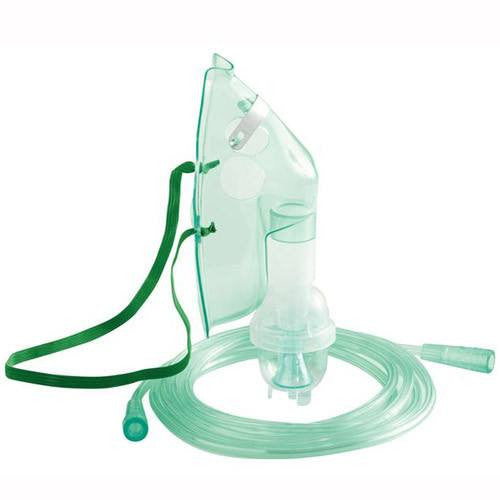
Original price $ 3.87Current price $ 3.45Pediatric Nebulizer Mask with 7 foot Tubing and Medication Jar
22 reviewsHudson RCI 1886 Pediatric Nebulizer mask is used to deliver aerosol mist medication to patients while using a Nebulizer machine. Product includes m...
View full details -
 Sale 52%
Original price $ 3.95Current price $ 1.90
Sale 52%
Original price $ 3.95Current price $ 1.90Oxygen Tubing Connector, White - Pack of 5
2 reviewsAirLife Oxygen Tubing Connectors are designed to connect tubing with a diameter between 5 mm and 7 mm. Each O2 connector is disposable and latex f...
View full details -
 Sale 41%
Original price $ 0.59Current price $ 0.35
Sale 41%
Original price $ 0.59Current price $ 0.35Universal Tubing Connector 5-in-1
2 reviews5-in-1 Universal Medical Tubing Connector is designed for use for oxygen therapy tubing, aspirator suction machine tubing and other medical devices...
View full details -
 Sale 40%
Original price $ 2.99Current price $ 1.79
Sale 40%
Original price $ 2.99Current price $ 1.79Tracheostomy Mask, Adult
2 reviewsA Tracheotomy Mask is a medical device specifically designed for those who need additional oxygen. These masks provide a safe and secure seal over ...
View full details -
 Sale 14%
Original price $ 0.79Current price $ 0.68
Sale 14%
Original price $ 0.79Current price $ 0.68Aerosol Mask, Under-the-Chin Style
1 reviewDynarex Aerosol Masks made with flexible, soft vinyl.. Adult elongated mask used for aerosol treatments. Dynarex Aerosol masks are excellent for en...
View full details -
 Sale 40%
Original price $ 1.75Current price $ 1.05
Sale 40%
Original price $ 1.75Current price $ 1.05CareFusion AirLife Baxter Pediatric Aerosol Mask
No reviewsDesigned for anatomical compatibility, the CareFusion AirLife Baxter Pediatric Aerosol Mask reduces irritation points to maximize patient comfort. ...
View full details -
 Sale 30%
Original price $ 19.95Current price $ 14.00
Sale 30%
Original price $ 19.95Current price $ 14.00Oxygen Tubing / Hose Connectors, White 50/Box
No reviewsAirLife Oxygen Tubing Connectors are designed to connects nasal cannula tubing and oxygen masks to extension tubing. Each O2 connector is disposabl...
View full details -
 Sold out
Original price $ 4.89Current price $ 3.59
Sold out
Original price $ 4.89Current price $ 3.59Aerosol Drainage Bag System with Wye Adaptor
No reviewsHudson RCI 1742 Aerosol Drainage Bag System with Wye adaptor is a drainage system for respiratory therapy. This respiratory device features a wye a...
View full details -
 Sale 27%
Original price $ 4.99Current price $ 3.65
Sale 27%
Original price $ 4.99Current price $ 3.65Multi-Vent Air Entrainment Mask Elongated Style Adult with Adjustable Head Strap & Nose Clip
No reviewsMulti-VENT® Air Entrainment Masks with color-coded, air-entrainment low and medium concentration diluters are intended for utilization by healthcar...
View full details -
 Sale 24%
Original price $ 3.95Current price $ 2.99
Sale 24%
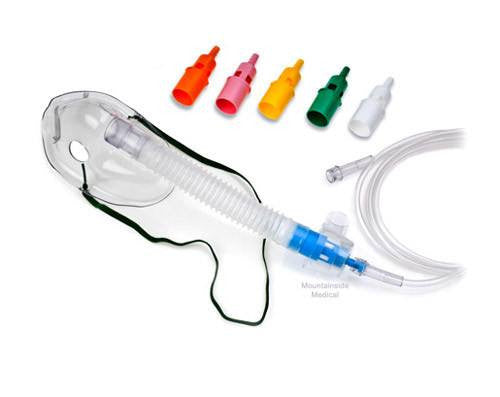
Original price $ 3.95Current price $ 2.99SELECT-A-VENT Mask Kit
No reviewsThe Teleflex 1098 Select-A-Vent Mask Kit provides patients with superior comfort and an effective seal. It comes with a clear, anatomically shaped,...
View full details
People Also Searched For

An oxygen mask is a medical device that covers the nose and mouth to deliver supplemental oxygen. It connects to an oxygen source (tank or concentrator) and provides higher-than-air oxygen concentrations to the patient’s lungs. Oxygen therapy is used whenever a patient’s blood oxygen levels (SpO₂) are too low (hypoxemia) to safely meet tissue needs. Without enough oxygen, vital organs (brain, heart, kidneys) can suffer damage. Conditions that commonly cause hypoxemia include acute or chronic lung diseases (for example, pneumonia, asthma attacks, COPD exacerbations, pulmonary fibrosis), heart failure with pulmonary congestion, severe anemia, shock, and acute respiratory distress (e.g. ARDS or COVID-19 pneumonia). In all these cases, breathing oxygen helps raise blood oxygen levels and relieve shortness of breath. Oxygen therapy is treated like any medication: it requires a prescription and careful monitoring (via pulse oximetry or arterial blood gases). The goal is to maintain adequate oxygen saturation (usually 94–98% in most adults, or 88–92% in chronic respiratory patients).
Types of Oxygen Masks (and Related Devices)
A variety of masks and interfaces are used depending on how much oxygen the patient needs. Key types include:
-
Nasal Cannula: (Not a mask, but often used first.) This is a simple plastic tube with prongs in the nostrils. It provides low-flow oxygen (1–6 L/min), which raises FiO₂ by roughly 4% per liter (about 24–44% at 6 L/min). Because it is unobtrusive, it allows talking and eating. If flows exceed ~4 L/min, a humidifier is often added to prevent nose/throat dryness.
-
Simple Face Mask: Covers the mouth and nose and has vents on the sides for exhalation. It is used for moderate oxygen needs. Typical flow is 5–10 L/min (never below 5–6, to avoid rebreathing CO₂), delivering about 28–50% FiO₂. The mask has an elastic strap and a moldable nose clip for a better seal.
-
Venturi (Air-Entrainment) Mask: This mask delivers a precise, fixed oxygen concentration. It uses color-coded adapters to “entrain” room air at exact ratios. Depending on the adapter, it can deliver specific FiO₂ values (commonly 24%, 28%, 31%, 35%, 40%, or 50%). The flowmeter is set to the rate indicated by the adapter (the flows are relatively high but fixed by design). Venturi masks are ideal when a controlled FiO₂ is needed – for example, in COPD or other chronic lung disease patients where giving too much oxygen can depress respiratory drive.
-
Non-Rebreather (NRB) Mask: This mask has a reservoir bag and one-way valves so that the patient inhales almost pure oxygen and exhales into the mask vents (not the reservoir). It can deliver very high oxygen concentrations (up to 60–90% FiO₂) when flow is set correctly. The typical flow is 10–15 L/min, and importantly, the reservoir bag must never fully collapse (it should stay at least 1/3–1/2 full between breaths. NRB masks are used in emergencies or very severe hypoxia (e.g. in shock, major trauma, or acute severe asthma), where maximal oxygen is needed immediately. (Note: If oxygen flow ceases or valves fail, there’s a risk of suffocation, so one must never remove the mask until it’s safe to do so.)
-
Partial Rebreather Mask: Similar to a non-rebreather but without one-way valves. It also has a reservoir bag but allows the patient to rebreathe some of the exhaled air. It typically requires 10–15 L/min flow and delivers around 35–50% FiO₂. Partial rebreathers are less common today but may be used when high-flow half-rich oxygen is acceptable.
-
Pediatric Oxygen Masks: Children and infants use scaled-down versions of the masks above (simple, Venturi, NRB) to fit their faces safely. For tiny infants, an oxygen hood (a transparent dome) or flowy oxygen tent may be used instead of a mask.
-
Noninvasive Ventilation Masks: (CPAP/BiPAP) These are tight-fitting masks connected to machines that provide pressurized oxygen or air (for example, in respiratory failure). Though not simple “masks” for passive O₂, they are important to mention as advanced oxygen-delivery devices.
-
Bag-Valve Mask (Resuscitator): In emergency situations, a hand-held bag-mask (Ambu bag) delivers oxygen or room air when the patient is not breathing adequately or at all. This is a specialized usage beyond routine oxygen therapy.
When Is Oxygen Mask Therapy Needed?
Oxygen masks are used for hypoxemia – when blood oxygen is dangerously low. Nurses and doctors typically look at the patient’s oxygen saturation (SpO₂): fall below ~90–92% on room air (or show signs of respiratory distress), and it’s time for oxygen. Situations include:
- Respiratory diseases: e.g. Pneumonia (bacterial or viral) – the inflamed lungs don’t exchange O₂ well; Asthma exacerbations – airway constriction leads to hypoxia; Chronic Obstructive Pulmonary Disease (COPD) flare-ups – long-term lung damage causes chronically low O₂; Pulmonary fibrosis or other interstitial lung disease; etc.
- Cardiac/vascular causes: e.g. Acute heart failure (fluid in lungs), pulmonary embolism, or shock – when blood isn’t getting to the lungs or lungs are flooded.
- High Altitude or Decompression: Low environmental oxygen.
- Anemia: Very low hemoglobin can cause low oxygen delivery; O₂ can help while fixing the anemia.
- During or after surgery/trauma: Anesthesia or injury can impair breathing; oxygen is often given prophylactically or therapeutically.
- Toxic exposures: Carbon monoxide poisoning and smoke inhalation victims are given 100% O₂.
- Emergency resuscitation: Any respiratory arrest or arrest situation zones in on high-oxygen support.
In all cases, indications for giving oxygen are signs or measurements of inadequate oxygenation (fast breathing, confusion or deterioration, low SpO₂). Nurses often have standing orders allowing them to start O₂ if saturations are below a threshold (commonly <92–94%). Once started, oxygen is titrated to keep SpO₂ in the target range (normally ≥94%, or 88–92% in certain COPD patients).
How to Apply Oxygen Masks
Preparing: Confirm the order (e.g. “O₂ at 6 L by mask”) and gather supplies: the correct mask type, oxygen source, and connecting tubing. Check the flowmeter and regulator, and ensure oxygen is flowing (with no kinks or leaks). If using a reservoir (NRB/partial), squeeze it to partially inflate before placement.
Placement: Secure the mask on the patient. For face masks, place it over the nose and mouth; loop the elastic band around the back of the head. Pinch the nose piece for a tight fit. For a nasal cannula, insert prongs into nostrils and drape tubing over the ears, tightening the slider under the chin. Ensure the mask seats well: watch for leaks around the edges or a floppy cannula. The patient should breathe normally; you may need to instruct them gently because having a mask on can be unsettling at first.
Flow Settings: Adjust the flowmeter to the prescribed setting. Typical flows:
- Simple face mask: 6–10 L/min (this yields about 28–50% O₂).
- Venturi mask: Set flow according to the adaptor (usually 4–15 L/min) to achieve the ordered FiO₂ (24–60%).
- Non-rebreather: 10–15 L/min (the bag must stay inflated).
- Nasal cannula: 1–6 L/min (each liter adds ~4% FiO₂.
Always verify the patient’s SpO₂ after a few minutes to ensure adequate response. If the saturation remains low, follow protocols to increase flow or change device, and notify the provider.
Ongoing Care: The patient may remove the mask briefly to eat unless otherwise instructed (provide a nasal cannula if needed). Remind them not to adjust the dial themselves – oxygen is not self-regulated. Nurses should intermittently check the mask fit, patency of tubing, and comfort level. Document the oxygen device, flow, and patient’s SpO₂ and respiratory status in the chart. When it’s time to wean, gradually reduce flow while monitoring saturation and work of breathing.
Helpful Tips and Important Safety Information
-
Oxygen “Fuel” Hazard: Oxygen greatly accelerates fires. Never smoke or allow open flames around oxygen equipment. Maintain a 6–10 foot “no-smoking” zone. Keep electrical appliances and heaters at a safe distance. Check that electrical devices and bulbs are functioning properly, as sparks could ignite enriched oxygen. Store oxygen cylinders upright and secure them to prevent tipping. In the home setting, install working smoke detectors and have a fire extinguisher available.
-
No Grease or Petroleum: Do not use oily or petroleum-based products (like Vaseline) on or near your face, lips, or inside the nostrils while on oxygen. Such substances can spontaneously ignite in the presence of concentrated oxygen. Use only approved water-based or saline moisturizers for dry nasal passages.
-
Humidification and Comfort: High-flow oxygen can dry out the mucous membranes. If the patient complains of dryness or thick secretions, a humidifier attachment (sterile water) may be indicated. Encourage the patient to drink plenty of fluids to stay hydrated (as this thins secretions). Warm, moist compresses or nasal saline sprays can also relieve dryness (never use petroleum jelly).
-
Skin and Comfort: Check the skin around masks and cannulas regularly. Irritation can occur at pressure points (over the nose or behind ears). Use gauze padding under straps or nasal prongs if needed. Adjust straps for comfort – the mask should seal but not painfully pinch. If the patient feels claustrophobic, reassure them and allow short breaks if oxygenation permits.
-
Monitoring: Nurses should continuously monitor respiratory rate and SpO₂. Improvement (saturation rising into target range, slower breathing, mental clarity) indicates therapy is working. Watch for signs of oxygen toxicity or carbon dioxide retention: headache, confusion, or lethargy may mean the flow is too high for certain patients (especially those with COPD). Follow orders for regular ABGs if the patient’s condition requires it.
-
Prescribed Therapy: Oxygen is essentially a medication. Never increase or decrease the flow without a doctor’s order (or standing protocol). Even though it seems helpful, giving “too much” oxygen can actually cause harm (hyperoxia), just as too little causes hypoxia. Target saturations are set for a reason. For example, nurses commonly give O₂ if SpO₂ falls below ~92% but hold off if it is ≥ 94–96%.
-
Patient Education: Teach the patient about using their device (especially at home). Show them how to read the flowmeter, and stress that only prescribed settings are allowed. If they have portable oxygen, instruct them on checking tank levels (gauge) and ensuring the cannula/mask is properly secured. Emphasize never to smoke near the device and to keep it upright. If any new symptoms occur (worsening breathlessness, dizziness, etc.), they should tell a healthcare provider promptly.
-
Travel/Home Safety: If the patient is on home oxygen, ensure they have enough supply (portable tank or concentrator batteries) before going out to avoid running out of oxygen. Store cylinders safely, and have an emergency plan. Remind everyone: in case of fire, turn off the oxygen source and evacuate immediately.
By following these guidelines, oxygen masks can be used effectively and safely. In summary, oxygen masks deliver needed oxygen directly to improve blood oxygen levels in patients with respiratory compromise. Proper device selection (simple mask, Venturi, NRB, etc.) depends on how much O₂ the patient needs, and strict safety measures (no smoking, correct flow, monitoring) protect the patient and caregivers. When applied and monitored correctly, oxygen mask therapy can greatly relieve hypoxia in many lung, heart, and critical illnesses.



























