Filters
- Asthma (3)
- Asthma Nebulizer (4)
- Asthma Treatment (3)
- Asthma Treatment Inhaler (1)
- Asthma treatments (3)
- Childrens Nebulizer Machine (7)
- Kids Nebulizer (6)
- Neb Machine (3)
- pediatric nebulizer machine (8)
- Penguin (1)
- kids nebulizer mask (7)
- Nebulizer bottle (1)
- Nebulizer Compressor (4)
- Nebulizer Filters (2)
- Nebulizer Machines (9)
- Nebulizer Mouthpiece (3)
- nebulizer parts (1)
- Nebulizer Treatment (5)
- nebulizer treatments (2)
- Nebulizer with Battery (2)
- Pediatric nebulizer (6)
- portable nebulizer (1)
- Portable nebulizer machine (3)
- Pulmo-Aide Nebulizers (1)
- Reusable Nebulizer Cup (1)
- ultrasonic nebulizer (1)
- digger the dog (1)
- Dog Nebulizer (2)
- Dog Nebulizer Machine (1)
- Kids Nebulizer Machine (1)
- Panda bear (1)
- pedicatric nebulizer (1)
- Asthma Medication (2)
- Dogs (1)
- Oxygen Machine (1)
- Puppy (1)
- Respiratory Therapy (2)
- Treat Asthma (2)
- Aerosol Mask (2)
- Aerosol medication (1)
- Bubbles the Fish (1)
- Childrens Mask (1)
- Kids Mask (1)
- Pediatric Mask (1)
- Frog Nebulizer (1)
- children (1)
- jar (1)
- mask for kids (1)
- neb mask (1)
- pediatric mask (1)
- Compressor Nebulizer (1)
- Portable Nebulizer (1)
- Resp-O2 (1)
- Respironics Tucker (1)
- turtle (1)
- Connector (1)
- Tubing connector (1)
- mouthpieces (1)
- Neb Kit 500 (1)
- Red Dog (1)
- Bunny (1)
- Bunny Nebulizer (1)
Pediatric Nebulizers for Kids
Pediatric Nebulizer
A nebulizer is a medical device that converts liquid respiratory medication into a fine mist (aerosol) so it can be inhaled directly into the lungs. In practice, pediatric nebulizer machines are simply nebulizers used for infants, toddlers, and young children. These machines typically include a base unit (often with an air compressor or ultrasonic generator), a small medication cup, and a child-sized mouthpiece or mask. When powered on, the device aerosolizes the liquid medicine and the child breathes it in through the mask or mouthpiece. As one children’s hospital guide explains, “a nebulizer is a device that sprays a fine, liquid mist of medicine” into the air, and the child “breathes in the medicine through the mouthpiece or mask”. In other words, a pediatric nebulizer machine delivers medication by turning it into an inhalable mist so it can reach the lungs effectively.
Pediatric nebulizers are used especially when children cannot use a standard inhaler. Infants and very young children often lack the coordination to inhale properly from a metered-dose inhaler (MDI), even with a spacer. For these patients many sources note that “nebulizers are often used by people who can’t use MDIs. This includes babies [and] young children…”. By contrast, a child simply needs to breathe normally through the mask during a nebulizer treatment (usually lasting 5–15 minutes) while the machine creates the mist. In this way, pediatric nebulizers give an easy, passive way to deliver asthma or other lung medications to children who cannot coordinate inhaler use.
Components and How It Works
A pediatric nebulizer machine has a base unit (compressor or ultrasonic generator), a medication cup, and a delivery mask or mouthpiece. The liquid medicine is placed in the cup, and when the machine is turned on, the base creates an aerosol. In a compressor (jet) nebulizer, compressed air or oxygen is forced through the liquid to form a mist of tiny droplets. In an ultrasonic nebulizer, high-frequency sound waves vibrate the liquid to create aerosol particles. The mask (often made of soft, flexible silicone) fits over the child's nose and mouth and is attached by a small tube to the base unit. The child inhales normally and receives the medication gradually. According to one description, a nebulizer “converts liquid medication into a fine mist that can be inhaled by a child” using precisely these components. Because the mist is inhaled deeply into the lungs, it provides targeted delivery of bronchodilators, steroids, saline or antibiotics right where they are needed.
Nebulizers come in three main types, which differ by how they generate the mist:
- Jet nebulizers – These use an air compressor to force air through the medicine, creating an aerosol. They are common and relatively low-cost, but tend to be a bit noisy.
- Ultrasonic nebulizers – These use ultrasonic (high-frequency) vibrations to produce very fine particles. They are quieter and deliver medication quickly, but they may heat the medicine slightly, so not all drugs are suitable.
- Mesh nebulizers – These use a vibrating mesh or membrane with tiny holes to push the liquid through as a mist. They are compact, very quiet, and efficient (with little medication wasted), making them popular for portable or pediatric use.
All these types work on the same principle (turning liquid into inhalable particles) and can be used for children. Importantly, studies and suppliers note no fundamental mechanical difference between “adult” and “pediatric” nebulizers – they operate the same way. The child version usually simply has smaller masks, tubing and a kid-friendly appearance. As one supplier bluntly states, “There are no mechanical differences between children’s nebulizers and adult nebulizers. Both children and adults can use either type of nebulizer. The difference is simply in design. Children’s nebulizers are made to be kid friendly and colorful, often featuring fun animal shapes”. In practice, a doctor could even use a regular nebulizer on a small child (with an appropriate mask); the “pediatric” label just indicates it’s sized and styled for young patients.
Pediatric Design Features
Pediatric nebulizers often include features to help children feel comfortable and get the full treatment. Aside from the smaller mask size, manufacturers frequently use bright colors, cartoon characters, or animal shapes to make the device inviting rather than scary. For example, one pediatric mask design is shaped like “Sami the Seal” or “Tucker the Turtle,” which not only entertains the child but also provides a soft, contoured fit on the face. These elements can keep kids calm and still during the breathing treatment. Other pediatric models sometimes have “interactive” lights or sounds, or handles that children can grip, to make the session more engaging (and to remind them to hold the mask in place). Importantly, however, these are cosmetic or comfort features; the core function – creating the aerosol – is identical to any nebulizer.
In terms of hardware, pediatric nebulizer kits always include masks specifically sized for infants or children. Unlike adult masks that might cover a larger nose and mouth area, pediatric masks are typically small and soft, with straps sized for little heads. Some even come as two-pieces (one for nose, one for mouth) for infants, plus a connecting tube. Parents should ensure a good seal (no big gaps) on the child’s face so that the maximum amount of medication is inhaled. Many source instructions emphasize that a proper fit improves treatment effectiveness.
Modern pediatric nebulizer machines also aim to minimize noise and take less time, since young patients can be restless. For example, mesh nebulizers produce very little sound and can complete a dose faster than old-school compressors. Portable battery-operated models (often mesh-based) exist so that treatment can be done in a car or while traveling. Nevertheless, most home-use pediatric nebulizers still plug into the wall.
Uses and Benefits in Children
Pediatric nebulizers are primarily used for respiratory illnesses in children. Common conditions include:
- Asthma attacks or chronic asthma: Nebulizers deliver direct bronchodilators (like albuterol) and steroids into the airways. They are often used in emergency or clinic settings for wheezing children, as well as at home for daily asthma control when needed.
- Cystic fibrosis or chronic lung disease: In diseases with thick mucus, inhaled saline or medications can help clear airways. Nebulizers are frequently prescribed for cystic fibrosis patients of any age.
- Bronchitis or pneumonia: In some cases, aerosolized antibiotics or bronchodilators are delivered via nebulizer for severe lung infections or inflammation.
- Allergic reactions: If a child has severe allergic asthma, nebulizers can deliver epinephrine or other emergency meds quickly.
By producing an inhalable spray, a nebulizer ensures direct medication delivery to the lungs. As one source notes, “the mist produced by the nebulizer allows the medication to reach the airways directly, providing targeted relief and promoting effective treatment”. This can make the medicine work faster and with fewer systemic side effects than oral drugs. Pediatric nebulizer treatments typically take just a few minutes (often 5–15 minutes per dose) and can deliver the full prescribed dose in one go, which is especially important for young patients.
Nebulizer therapy has both advantages and drawbacks compared to inhalers. Its main advantage in pediatrics is ease of use: the child simply breathes normally, without needing coordination. This often leads to better delivery of medicine for uncooperative or very young children. For instance, academic studies consistently find that nebulizers and pressurized inhalers (with spacers) have similar clinical effectiveness in preschoolers, so nebulizers remain a standard option when inhaler use is not practical. One guideline advises that infants and toddlers “need to use a face mask attached to a metered dose inhaler or a nebulizer to get the correct amount of medicine”. (Indeed, as noted above, metered-dose inhalers require removing a metal canister and inhaling coordination, which is why nebulizers are often preferred when young children are ill.)
Using and Caring for Pediatric Nebulizer
For parents and caregivers, using a pediatric nebulizer involves a simple routine: mix the doctor-prescribed medication in the cup, attach the mask (and tubing), and run the machine while the child breathes normally. Many children hold the mask themselves or watch a favorite video to pass the time. It is important to follow the healthcare provider’s instructions on dosage and solution volume.
Maintenance is crucial. All sources stress that nebulizer components (cup, mask, tubing) should be cleaned or disinfected according to the manufacturer’s instructions after each use. Regular cleaning prevents mold or bacterial growth, which could infect the child’s lungs. For example, Nationwide Children’s Hospital advises: “Clean your inhaler or nebulizer after every use… Always remember to remove the metal canister from your inhaler before cleaning” (when applicable). Some parts may even be disposable or require sterilization in boiling water. Careful maintenance extends the life of the machine and ensures safe treatments.
In summary, pediatric nebulizer machines are essential tools for treating respiratory problems in children. They work exactly like standard nebulizers but come in child-friendly sizes and styles. By turning liquid medication into an inhalable mist, they allow young patients to receive lung treatments easily and effectively. With appropriate use and maintenance, these devices provide a safe and targeted way to deliver asthma and other airway medications directly where they are needed most.
-
 Sale 35%
Original price $ 98.71Current price $ 64.00
Sale 35%
Original price $ 98.71Current price $ 64.00Penguin Pediatric Nebulizer Machine with Neb Kit, Mouthpiece, Mask Tubing and Carry Bag
Drive Medical1 reviewPediatric Penguin Nebulizer is a safe and fun pediatric nebulizer machine compressor used to deliver liquid mist medication for asthma nebulizer tr...
View full details -
 Sale 37%
Original price $ 107.58Current price $ 68.00
Sale 37%
Original price $ 107.58Current price $ 68.00Pediatric Nebulizer Machine with Neb Kit, Mouthpiece, Mask Tubing and Carry Bag
Drive Medical2 reviewsPediatric Fish Compressor Nebulizer is a great way for your kids to take their treatments. It is dishwasher safe and comes with everything you need...
View full details -
 Sale 26%
Original price $ 65.95Current price $ 48.95
Sale 26%
Original price $ 65.95Current price $ 48.95Digger Dog Pediatric Nebulizer Machine with Treatment Supplies
Carex1 reviewDigger Dog Pediatric Nebulizer is designed to make nebulizer treatments more kid-friendly. This nebulizer includes compressor, nebulizer, dog house...
View full details -
 Sale 30%
Original price $ 92.88Current price $ 65.00
Sale 30%
Original price $ 92.88Current price $ 65.00Pediatric Panda Bear Nebulizer Machine
Drive MedicalNo reviewsPanda Bear Pediatric Nebulizer Machine is a child-friendly nebulizer compressor that children love. This pediatric nebulizer comes with the compres...
View full details -
 Sale 34%
Original price $ 49.95Current price $ 33.00
Sale 34%
Original price $ 49.95Current price $ 33.00My Dog Kids Nebulizer Machine with Infant & Child Mask, Mouthpiece and 5 Filters
Dynarex1 reviewGive your child effective and stress-free respiratory care with the My Dog Kids Nebulizer Machine by Dynarex! Specially designed in a fun, kid-frie...
View full details -
 Sale 38%
Original price $ 4.79Current price $ 2.95
Sale 38%
Original price $ 4.79Current price $ 2.95Pari Bubbles the Fish II Pediatric Aerosol Nebulizer Mask
Pari2 reviewsThe Pari Respiratory Bubbles the Fish II Pediatric Aerosol Mask is a cute and fun aerosol medication delivery mask designed for use by children. Th...
View full details -
 Sale 28%
Original price $ 67.95Current price $ 48.95
Sale 28%
Original price $ 67.95Current price $ 48.95Frog Pediatric Nebulizer Machine with Mask and Tubing Included
CarexNo reviewsFrog Pediatric nebulizer machine with mask and tubing included is a medical device used for delivering medication directly into the respiratory sys...
View full details -
 Sale 20%
Original price $ 3.87Current price $ 3.08
Sale 20%
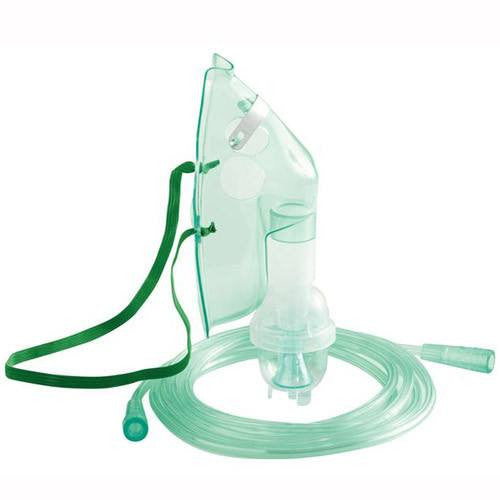
Original price $ 3.87Current price $ 3.08Pediatric Nebulizer Mask with Tubing and Medication Jar
Teleflex22 reviewsHudson RCI 1886 Pediatric Nebulizer mask is used to deliver aerosol mist medication to patients while using a Nebulizer machine. Product includes m...
View full details -
 Sale 45%
Original price $ 59.95Current price $ 33.00
Sale 45%
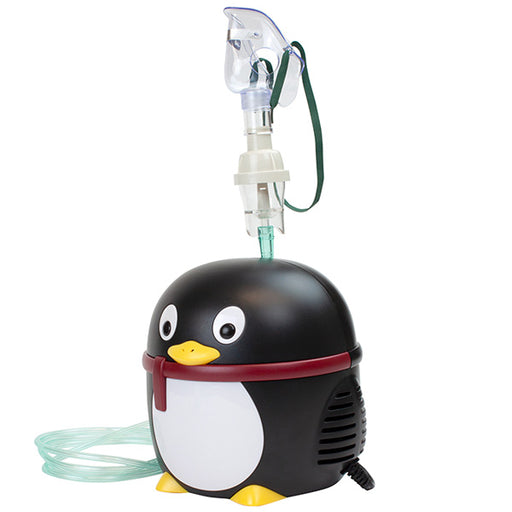
Original price $ 59.95Current price $ 33.00Penguin Pediatric Nebulizer Machine Compressor with Mask and Tubing
DynarexNo reviewsPenguin Pediatric Nebulizer Machine Compressor with Mask and Tubing is a medical device used to convert liquid medication into a mist that can be i...
View full details -
 Sale 31%
Original price $ 39.95Current price $ 27.50
Sale 31%
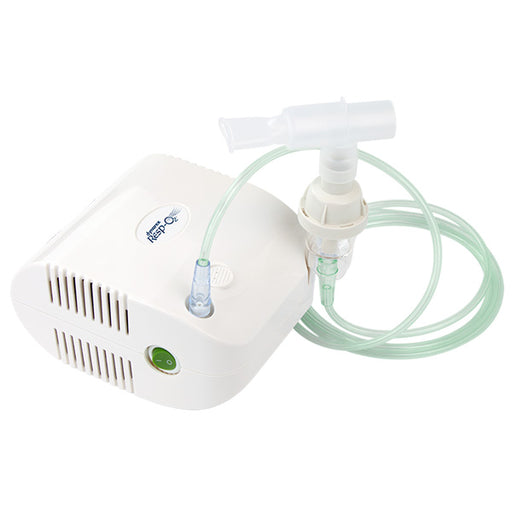
Original price $ 39.95Current price $ 27.50Nebulizer Machine Compressor for Respiratory Therapy
Dynarex103 reviewsThe Ultra light portable nebulizer machine compressor is highly effective for respiratory treatments related to asthma, allergies, and a variety of...
View full details -
 Sold out
$ 2.95
Sold out
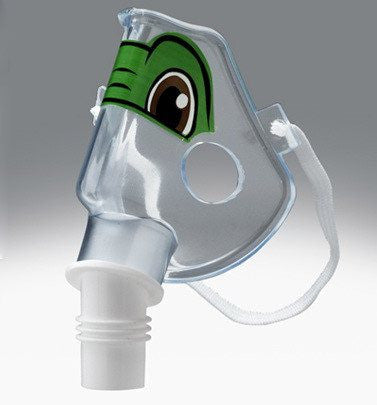
$ 2.95Tucker the Turtle Pediatric Aerosol Mask
Philips RespironicsNo reviewsRespironics Tucker the Turtle Pediatric Aerosol Medication Mask is a cute, kid-friendly face mask for use with nebulizer breathing treatments. This...
View full details -
 Sale 55%
Original price $ 0.87Current price $ 0.39
Sale 55%
Original price $ 0.87Current price $ 0.39Treaded Oxygen Tubing Connector
Teleflex10 reviewsTreaded Oxygen Tubing Connector is double-male end connector used with nasal cannulas, oxygen masks and other respiratory devices. Unique design, a...
View full details -
 Sale 39%
Original price $ 72.38Current price $ 43.95
Sale 39%
Original price $ 72.38Current price $ 43.95Compressor Nebulizer Machine for Aerosol Medication Therapy
Drive Medical2 reviewsCompressor Nebulizer Machine for Aerosol Medication Therapy. This nebulizer Comes with a dishwasher safe reusable JetNeb Plus The MQ5900 also come...
View full details -
 Sale 37%
Original price $ 3.95Current price $ 2.49
Sale 37%
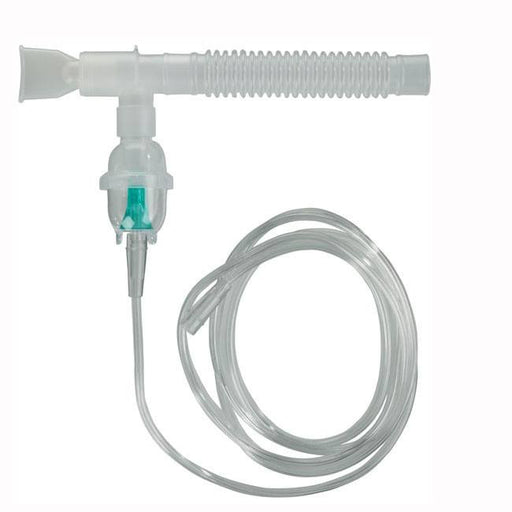
Original price $ 3.95Current price $ 2.49Nebulizer Treatment Kit with Cup, Mouthpiece and 7 foot Tubing
Drive Medical7 reviewsDrive Medical Nebulizer Treatment Kit with Cup, Corrugated Mouthpiece and seven foot Tubing. Transforms medication into a fine micro mist for eas...
View full details -
 Sale 17%
Original price $ 47.95Current price $ 39.95
Sale 17%
Original price $ 47.95Current price $ 39.95Pete the Dog Pediatric Nebulizer Machine Compressor for Asthma and COPD Treatments
LeaderNo reviewsPete the Dog Pediatric Nebulizer Machine Compressor is a medical device used for administering medication through inhaled mist to treat asthma and ...
View full details -
 Sale 26%
Original price $ 67.95Current price $ 49.95
Sale 26%
Original price $ 67.95Current price $ 49.95Bunny Pediatric Nebulizer Machine with Mask, Tubing and Carrying Bag
CarexNo reviewsBunny Pediatric Nebulizer Machine is a medical device used to administer medication directly to the lungs of infants and young children. The machin...
View full details
People Also Searched For
Pediatric Nebulizer
A nebulizer is a medical device that converts liquid respiratory medication into a fine mist (aerosol) so it can be inhaled directly into the lungs. In practice, pediatric nebulizer machines are simply nebulizers used for infants, toddlers, and young children. These machines typically include a base unit (often with an air compressor or ultrasonic generator), a small medication cup, and a child-sized mouthpiece or mask. When powered on, the device aerosolizes the liquid medicine and the child breathes it in through the mask or mouthpiece. As one children’s hospital guide explains, “a nebulizer is a device that sprays a fine, liquid mist of medicine” into the air, and the child “breathes in the medicine through the mouthpiece or mask”. In other words, a pediatric nebulizer machine delivers medication by turning it into an inhalable mist so it can reach the lungs effectively.
Pediatric nebulizers are used especially when children cannot use a standard inhaler. Infants and very young children often lack the coordination to inhale properly from a metered-dose inhaler (MDI), even with a spacer. For these patients many sources note that “nebulizers are often used by people who can’t use MDIs. This includes babies [and] young children…”. By contrast, a child simply needs to breathe normally through the mask during a nebulizer treatment (usually lasting 5–15 minutes) while the machine creates the mist. In this way, pediatric nebulizers give an easy, passive way to deliver asthma or other lung medications to children who cannot coordinate inhaler use.
Components and How It Works
A pediatric nebulizer machine has a base unit (compressor or ultrasonic generator), a medication cup, and a delivery mask or mouthpiece. The liquid medicine is placed in the cup, and when the machine is turned on, the base creates an aerosol. In a compressor (jet) nebulizer, compressed air or oxygen is forced through the liquid to form a mist of tiny droplets. In an ultrasonic nebulizer, high-frequency sound waves vibrate the liquid to create aerosol particles. The mask (often made of soft, flexible silicone) fits over the child's nose and mouth and is attached by a small tube to the base unit. The child inhales normally and receives the medication gradually. According to one description, a nebulizer “converts liquid medication into a fine mist that can be inhaled by a child” using precisely these components. Because the mist is inhaled deeply into the lungs, it provides targeted delivery of bronchodilators, steroids, saline or antibiotics right where they are needed.
Nebulizers come in three main types, which differ by how they generate the mist:
- Jet nebulizers – These use an air compressor to force air through the medicine, creating an aerosol. They are common and relatively low-cost, but tend to be a bit noisy.
- Ultrasonic nebulizers – These use ultrasonic (high-frequency) vibrations to produce very fine particles. They are quieter and deliver medication quickly, but they may heat the medicine slightly, so not all drugs are suitable.
- Mesh nebulizers – These use a vibrating mesh or membrane with tiny holes to push the liquid through as a mist. They are compact, very quiet, and efficient (with little medication wasted), making them popular for portable or pediatric use.
All these types work on the same principle (turning liquid into inhalable particles) and can be used for children. Importantly, studies and suppliers note no fundamental mechanical difference between “adult” and “pediatric” nebulizers – they operate the same way. The child version usually simply has smaller masks, tubing and a kid-friendly appearance. As one supplier bluntly states, “There are no mechanical differences between children’s nebulizers and adult nebulizers. Both children and adults can use either type of nebulizer. The difference is simply in design. Children’s nebulizers are made to be kid friendly and colorful, often featuring fun animal shapes”. In practice, a doctor could even use a regular nebulizer on a small child (with an appropriate mask); the “pediatric” label just indicates it’s sized and styled for young patients.
Pediatric Design Features
Pediatric nebulizers often include features to help children feel comfortable and get the full treatment. Aside from the smaller mask size, manufacturers frequently use bright colors, cartoon characters, or animal shapes to make the device inviting rather than scary. For example, one pediatric mask design is shaped like “Sami the Seal” or “Tucker the Turtle,” which not only entertains the child but also provides a soft, contoured fit on the face. These elements can keep kids calm and still during the breathing treatment. Other pediatric models sometimes have “interactive” lights or sounds, or handles that children can grip, to make the session more engaging (and to remind them to hold the mask in place). Importantly, however, these are cosmetic or comfort features; the core function – creating the aerosol – is identical to any nebulizer.
In terms of hardware, pediatric nebulizer kits always include masks specifically sized for infants or children. Unlike adult masks that might cover a larger nose and mouth area, pediatric masks are typically small and soft, with straps sized for little heads. Some even come as two-pieces (one for nose, one for mouth) for infants, plus a connecting tube. Parents should ensure a good seal (no big gaps) on the child’s face so that the maximum amount of medication is inhaled. Many source instructions emphasize that a proper fit improves treatment effectiveness.
Modern pediatric nebulizer machines also aim to minimize noise and take less time, since young patients can be restless. For example, mesh nebulizers produce very little sound and can complete a dose faster than old-school compressors. Portable battery-operated models (often mesh-based) exist so that treatment can be done in a car or while traveling. Nevertheless, most home-use pediatric nebulizers still plug into the wall.
Uses and Benefits in Children
Pediatric nebulizers are primarily used for respiratory illnesses in children. Common conditions include:
- Asthma attacks or chronic asthma: Nebulizers deliver direct bronchodilators (like albuterol) and steroids into the airways. They are often used in emergency or clinic settings for wheezing children, as well as at home for daily asthma control when needed.
- Cystic fibrosis or chronic lung disease: In diseases with thick mucus, inhaled saline or medications can help clear airways. Nebulizers are frequently prescribed for cystic fibrosis patients of any age.
- Bronchitis or pneumonia: In some cases, aerosolized antibiotics or bronchodilators are delivered via nebulizer for severe lung infections or inflammation.
- Allergic reactions: If a child has severe allergic asthma, nebulizers can deliver epinephrine or other emergency meds quickly.
By producing an inhalable spray, a nebulizer ensures direct medication delivery to the lungs. As one source notes, “the mist produced by the nebulizer allows the medication to reach the airways directly, providing targeted relief and promoting effective treatment”. This can make the medicine work faster and with fewer systemic side effects than oral drugs. Pediatric nebulizer treatments typically take just a few minutes (often 5–15 minutes per dose) and can deliver the full prescribed dose in one go, which is especially important for young patients.
Nebulizer therapy has both advantages and drawbacks compared to inhalers. Its main advantage in pediatrics is ease of use: the child simply breathes normally, without needing coordination. This often leads to better delivery of medicine for uncooperative or very young children. For instance, academic studies consistently find that nebulizers and pressurized inhalers (with spacers) have similar clinical effectiveness in preschoolers, so nebulizers remain a standard option when inhaler use is not practical. One guideline advises that infants and toddlers “need to use a face mask attached to a metered dose inhaler or a nebulizer to get the correct amount of medicine”. (Indeed, as noted above, metered-dose inhalers require removing a metal canister and inhaling coordination, which is why nebulizers are often preferred when young children are ill.)
Using and Caring for Pediatric Nebulizer
For parents and caregivers, using a pediatric nebulizer involves a simple routine: mix the doctor-prescribed medication in the cup, attach the mask (and tubing), and run the machine while the child breathes normally. Many children hold the mask themselves or watch a favorite video to pass the time. It is important to follow the healthcare provider’s instructions on dosage and solution volume.
Maintenance is crucial. All sources stress that nebulizer components (cup, mask, tubing) should be cleaned or disinfected according to the manufacturer’s instructions after each use. Regular cleaning prevents mold or bacterial growth, which could infect the child’s lungs. For example, Nationwide Children’s Hospital advises: “Clean your inhaler or nebulizer after every use… Always remember to remove the metal canister from your inhaler before cleaning” (when applicable). Some parts may even be disposable or require sterilization in boiling water. Careful maintenance extends the life of the machine and ensures safe treatments.
In summary, pediatric nebulizer machines are essential tools for treating respiratory problems in children. They work exactly like standard nebulizers but come in child-friendly sizes and styles. By turning liquid medication into an inhalable mist, they allow young patients to receive lung treatments easily and effectively. With appropriate use and maintenance, these devices provide a safe and targeted way to deliver asthma and other airway medications directly where they are needed most.
















