Filters
- doctor-only (10)
- Fresenius USA (1)
- Hypocalcemia (1)
- hypomagnesemia (1)
- low magnesium (1)
- Magnesium (2)
- Magnesium deficiency (1)
- Magnesium Deficiency Treatment (1)
- magnesium injection (1)
- Magnesium Sulfate 50% (1)
- Magnesium Sulfate for Injection (1)
- Magnesium Sulfate injection (1)
- magnesium sulfate injection side effects (1)
- magnesium sulfate injection uses (1)
- Magnesium Sulfate IV (1)
- Treatment of acute Symptomatic Hypocalcemia (1)
- Connective Tissue (1)
- copper (1)
- Copper Deficiency (1)
- Copper for Injection (1)
- Copper Injection (1)
- Cupric Chloride (1)
- Iron Metabolism (1)
- Malabsorption (1)
- Menkes Disease (1)
- Short Bowel Syndrome (1)
- Total Parenteral Nutrition (2)
- Trace element (3)
- Treat Copper Deficiencies (1)
- 70199-0026-11 (1)
- A Injection (1)
- A Vitamin (1)
- Aquasol A (1)
- Aquasol A Injection (1)
- Aquasol A Parentera (1)
- Cell Growth (1)
- Eye health (1)
- Immune health (1)
- immune system (1)
- Infections (1)
- Intramuscularly (1)
- Malabsorption Disorders (1)
- Palmitate (1)
- Retinol (1)
- Skin health (1)
- TPN Nutrition (1)
- Vision (1)
- Vision Health (1)
- vitamin a (1)
- Vitamin A Deficiency (1)
- Zinc Chloride (2)
- Zinc Chloride Injection (1)
- 64253-0900-91 (1)
- Calcium (1)
- calcium channel blocker overdose (1)
- calcium chloride (1)
- Calcium Chloride 10% (1)
- Calcium Chloride 10% Injection (1)
- Calcium Chloride Injection (1)
- Calcium Injection (1)
- calcium supplementation (1)
- Cardiac arrest (1)
- Cardiac Arrest Drugs (1)
- Crash Cart (1)
- Critical Care Electrolyte (1)
- Critical Care Medicine (1)
- Electrolyte Replacement (1)
- Electrolyte Rescue Medication (1)
- Electrolytes (2)
- Emergency Calcium Injection (1)
- Emergency Drugs (1)
- Emergency Electrolyte Replacement (1)
- Fast-Acting Calcium IV (1)
- Hospital (1)
- Hospital Medication (1)
- Hyperkalemia (1)
- Hypocalcemia Injection (1)
- hypocalcemic (1)
- IV Calcium Chloride (1)
- IV Electrolytes (1)
- IV Medications (1)
- Medefil Calcium (1)
- Paramedic (1)
- Paramedics (1)
- prefilled syringes (1)
- Prefilled Syringes Hospital (1)
- severe hyperkalemia (1)
- Treat bradyasystolic cardiac arrest (1)
- Treat Calcium Deficiency (1)
- Anorexia (1)
- DNA synthesis (1)
- Dysosmia (1)
- Geophagia (1)
- Growth Retardation (1)
- Hepatosplenomegaly (1)
- Hypogeusia (1)
- Hypogonadism (1)
- Immune Function (2)
- Metabolic Function (1)
- Parakeratosis (1)
- Protein Synthesis (1)
- Trace Element supplement (1)
- Treatment of anorexia (1)
- Wound Healing (1)
- zinc (1)
- Zinc deficiency (1)
- Zinc for Injection (1)
- Acid-base Balance (1)
- Electrolyte Additive (1)
- Fluid Balance (1)
- Gastrointestinal issues (1)
- Hydration (1)
- Malnutrition (1)
- Multiple Electrolyte Additive (1)
- Muscle Function (1)
- Nerve Function (1)
- Phosphate (1)
- Potassium (1)
- Severe Dehydration (1)
- TPN Electrolytes (1)
- Blood Sugar Imbalances (1)
- Chromic Chloride (1)
- Chromium (1)
- Chromium for Injection (1)
- Fat Metabolism (1)
- insulin Function (1)
- Mineral Chromium (1)
- antioxidant (1)
- Parenteral nutrition (1)
- Selenious Acid (1)
- Selenious Acid Injection (1)
- Selenium (1)
- Selenium Injection (1)
- Thyroid function (1)
- Treat Selenium Deficiency (1)
- Antioxidant Enzyme (1)
- Bone formation (1)
- Enzymes (1)
- Manganese (1)
- Manganese Chloride (1)
- Manganese deficiency (1)
- Manganese Injection (1)
- metabolism (1)
- Toxicity (1)
- Trace Element Supplement (1)
- Treat Manganese Deficiencies (1)
TPN Electrolyte Injection
TPN Electrolyte Injection
TPN (Total Parenteral Nutrition) Electrolytes is a specialized intravenous solution used in hospital nutrition therapy. It is essentially a concentrated multi-electrolyte injection that is added to a TPN (intravenous nutrition) infusion. In practice, a small volume (e.g. 20 mL) of this electrolyte solution is mixed into each liter of a dextrose/amino‐acid TPN bag to supply essential mineral salts. As the packaging notes, it is a “sterile, … concentrated solution of intra- and extracellular ions for IV infusion after dilution as a maintenance electrolyte replenisher only.”. In other words, it contains key electrolytes (sodium, potassium, calcium, magnesium, acetate, and chloride) and is used only as part of a TPN regimen, not given intravenously by itself.
-
Composition: The injection contains sodium chloride, potassium chloride, calcium chloride, magnesium chloride and sodium acetate (anhydrous) in fixed proportions. For example, each 20 mL vial provides roughly 35 mEq of sodium (Na⁺), 20 mEq of potassium (K⁺), 4.5 mEq of calcium (Ca²⁺), 5 mEq of magnesium (Mg²⁺), 35 mEq of chloride (Cl⁻) and 29.5 mEq of acetate. (Electrolyte values may vary slightly by manufacturer, but these figures are typical for a “TPN Electrolytes” product.) Notably, no phosphate is included in this solution – phosphate is supplied separately if needed in the TPN mixture. The solution has no added preservatives or buffer agents.
- Indications/Use: This product is indicated only as a supplement to TPN fluids. In practice, it is added to a concentrated dextrose‐amino acid solution (the main TPN infusion) to maintain electrolyte balance. The official prescribing information states that TPN Electrolytes are “indicated for use as a supplement to nutritional solutions containing concentrated dextrose and amino acids delivered by central venous infusion, to help maintain electrolyte homeostasis in adult patients.”. In other words, it helps prevent electrolyte deficiencies in patients getting IV nutrition. Typical dosing is one 20 mL vial per liter of TPN solution, given continuously (e.g. 80–125 mL/hour for 24 hours in an adult). The mixed TPN solution (with dextrose, amino acids, and electrolytes) is usually run through a central venous catheter.
- Administration: The solution comes in a small plastic vial and must be diluted into the TPN fluid before use. It is intended for intravenous use only after thorough mixing. Because it is hypertonic, it should be infused into a high-flow central vein. It is not for subcutaneous or intramuscular use. Health care staff will verify the TPN bag contents (including electrolytes, dextrose, amino acids, vitamins, etc.) before starting the infusion, and will monitor blood electrolyte levels frequently.
- Precautions: As with any electrolyte solution, care is needed in certain conditions. For example, it is contraindicated in patients who already have dangerously high levels of any component (e.g. hyperkalemia, hypernatremia, severe edema) or conditions like complete heart block or severe renal failure. The product label specifically notes it is “Not intended for pediatric use.”. Also note the solution contains acetate, which metabolizes to bicarbonate; clinicians watch acid-base balance when using acetate-containing solutions. In patients with heart failure or renal insufficiency, even normal doses may need adjustment due to sodium or potassium content. (Because it has no preservatives, once mixed it should be used promptly and any unused portion discarded.
In summary, a “TPN Electrolyte injection” is a multi-ion injection solution used as part of total parenteral nutrition. It is essentially a concentrated additive of sodium, potassium, calcium, magnesium, chloride and acetate ions designed to maintain electrolyte balance during IV feeding. It is given by IV infusion (through a central line) along with nutrients. Proper mixing and monitoring are required, and additional phosphate is added separately if needed.
-
 Sale 14%
Original price $ 429.00Current price $ 369.00
Sale 14%
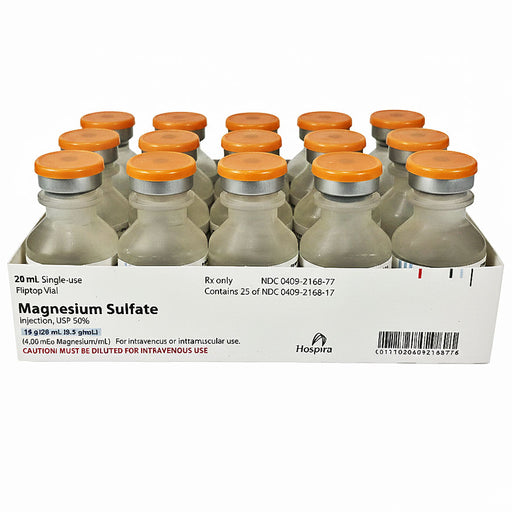
Original price $ 429.00Current price $ 369.00Magnesium Sulfate Injection 50% Single Use Vial 10 gram/20mL (0.5/mL) 20mL , 25/pack (Rx)
Pfizer InjectablesNo reviewsMagnesium Sulfate Injection Magnesium sulfate injection is a sterile, liquid medication that delivers magnesium (in the form of magnesium sulfate) ...
View full details🔒 Medical License Required -
 Sale 36%
Original price $ 2,650.00Current price $ 1,685.00
Sale 36%
Original price $ 2,650.00Current price $ 1,685.00Copper (Cupric Chloride) for Injection 10 mL, 25/Tray by Pfizer (Rx)
Pfizer InjectablesNo reviewsCopper (Cupric Chloride) for Injection is used to treat or prevent copper deficiency in patients who cannot get enough copper through diet alone, o...
View full details🔒 Medical License Required -
 Sale 29%
Original price $ 1,450.00Current price $ 1,025.00
Sale 29%
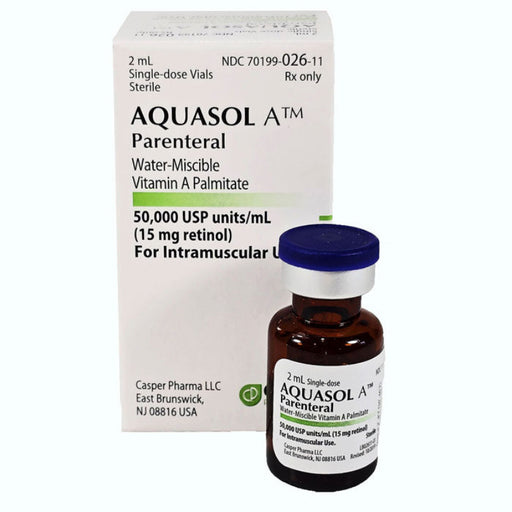
Original price $ 1,450.00Current price $ 1,025.00Aquasol A Vitamin A Injection Deficiency Supplement 50,000 Units 2mL (Rx) *Refrigerated
Casper PharmaNo reviewsFast-Acting, Hospital-Grade Injectable Vitamin A for Deficiency, Malnutrition & Measles Support Aquasol A Vitamin A Injection provides a reliab...
View full details🔒 Medical License Required -
 Sale 26%
Original price $ 1,495.95Current price $ 1,100.00
Sale 26%
Original price $ 1,495.95Current price $ 1,100.00Zinc Chloride Injection Intravenous for Deficiency & Parenteral Nutrition 10 mg/10 mL Vials 10 mL x 25/Pack (RX)
Exela Pharma SciencesNo reviewsThe Gold Standard for IV Zinc Supplementation in Nutritional Support, Hospital, and Critical Care Settings Keep your patients healthy and optimize ...
View full details🔒 Medical License Required -
 Sale 29%
Original price $ 299.95Current price $ 214.00
Sale 29%
Original price $ 299.95Current price $ 214.00Calcium Chloride 10% Prefilled Syringes 1000 mg/10 mL100 mg/mL) 10/Box (Rx)
MedefilNo reviewsEssential IV Electrolyte for Cardiac, Toxicology & Critical Care Emergencies Rapid, Reliable IV Calcium Therapy for Cardiac Arrest, Hyperkalemi...
View full details🔒 Medical License Required -
 Sale 15%
Original price $ 1,750.00Current price $ 1,495.00
Sale 15%
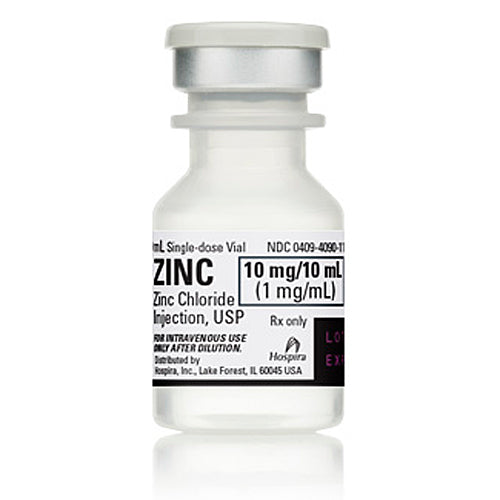
Original price $ 1,750.00Current price $ 1,495.00Zinc Chloride for Injection 1 mg/mL Single Dose 10 mL, 25/Tray
Pfizer InjectablesNo reviewsZinc Chloride Injection is used as a trace element supplement in total parenteral nutrition (TPN) to prevent or treat zinc deficiency. It is essent...
View full details🔒 Medical License Required -
 Sale 21%
Original price $ 599.95Current price $ 475.00
Sale 21%
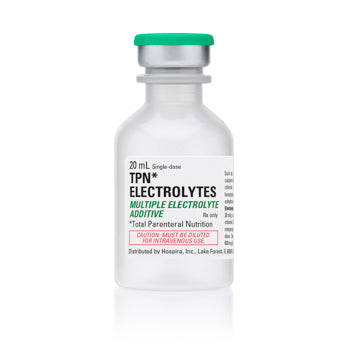
Original price $ 599.95Current price $ 475.00TPN Electrolytes (multiple electrolyte additive) Injection 20 mL SDV Vials x 25/Tray (RX)
Pfizer InjectablesNo reviewsTPN Electrolytes (multiple electrolyte additive) Injection is used in total parenteral nutrition (TPN) to provide essential electrolytes to patient...
View full details🔒 Medical License Required -
 Sale 25%
Original price $ 1,450.00Current price $ 1,085.00
Sale 25%
Original price $ 1,450.00Current price $ 1,085.00Chromium (Chromic Chloride) for Injection 10ml Vials, 25/Tray (RX)
Pfizer InjectablesNo reviewsChromium (Chromic Chloride) for Injection is a medication used to supplement and maintain adequate levels of the mineral chromium in the body. It i...
View full details🔒 Medical License Required -
 Sale 19%
Original price $ 4,559.95Current price $ 3,700.00
Sale 19%
Original price $ 4,559.95Current price $ 3,700.00Selenious Acid Injection (Selenium) 600 mcg/mL SDV 10mL x 5/Box (Rx)
cNo reviewsSelenious Acid Injection (Selenium) 600 mcg is used as a supplement to prevent and treat selenium deficiency, particularly in patients receiving pa...
View full details🔒 Medical License Required -
 Sale 20%
Original price $ 2,250.00Current price $ 1,795.00
Sale 20%
Original price $ 2,250.00Current price $ 1,795.00Manganese Chloride Injection IV Trace Element Supplementation 0.1 mg/mL SDV 10 mL x 25/Tray (RX)
Pfizer InjectablesNo reviewsEssential IV Trace Element Supplement for Parenteral Nutrition, Deficiency Correction, and Total Parenteral Nutrition Protocols Manganese Chloride ...
View full details🔒 Medical License Required
People Also Searched For
TPN Electrolyte Injection
TPN (Total Parenteral Nutrition) Electrolytes is a specialized intravenous solution used in hospital nutrition therapy. It is essentially a concentrated multi-electrolyte injection that is added to a TPN (intravenous nutrition) infusion. In practice, a small volume (e.g. 20 mL) of this electrolyte solution is mixed into each liter of a dextrose/amino‐acid TPN bag to supply essential mineral salts. As the packaging notes, it is a “sterile, … concentrated solution of intra- and extracellular ions for IV infusion after dilution as a maintenance electrolyte replenisher only.”. In other words, it contains key electrolytes (sodium, potassium, calcium, magnesium, acetate, and chloride) and is used only as part of a TPN regimen, not given intravenously by itself.
-
Composition: The injection contains sodium chloride, potassium chloride, calcium chloride, magnesium chloride and sodium acetate (anhydrous) in fixed proportions. For example, each 20 mL vial provides roughly 35 mEq of sodium (Na⁺), 20 mEq of potassium (K⁺), 4.5 mEq of calcium (Ca²⁺), 5 mEq of magnesium (Mg²⁺), 35 mEq of chloride (Cl⁻) and 29.5 mEq of acetate. (Electrolyte values may vary slightly by manufacturer, but these figures are typical for a “TPN Electrolytes” product.) Notably, no phosphate is included in this solution – phosphate is supplied separately if needed in the TPN mixture. The solution has no added preservatives or buffer agents.
- Indications/Use: This product is indicated only as a supplement to TPN fluids. In practice, it is added to a concentrated dextrose‐amino acid solution (the main TPN infusion) to maintain electrolyte balance. The official prescribing information states that TPN Electrolytes are “indicated for use as a supplement to nutritional solutions containing concentrated dextrose and amino acids delivered by central venous infusion, to help maintain electrolyte homeostasis in adult patients.”. In other words, it helps prevent electrolyte deficiencies in patients getting IV nutrition. Typical dosing is one 20 mL vial per liter of TPN solution, given continuously (e.g. 80–125 mL/hour for 24 hours in an adult). The mixed TPN solution (with dextrose, amino acids, and electrolytes) is usually run through a central venous catheter.
- Administration: The solution comes in a small plastic vial and must be diluted into the TPN fluid before use. It is intended for intravenous use only after thorough mixing. Because it is hypertonic, it should be infused into a high-flow central vein. It is not for subcutaneous or intramuscular use. Health care staff will verify the TPN bag contents (including electrolytes, dextrose, amino acids, vitamins, etc.) before starting the infusion, and will monitor blood electrolyte levels frequently.
- Precautions: As with any electrolyte solution, care is needed in certain conditions. For example, it is contraindicated in patients who already have dangerously high levels of any component (e.g. hyperkalemia, hypernatremia, severe edema) or conditions like complete heart block or severe renal failure. The product label specifically notes it is “Not intended for pediatric use.”. Also note the solution contains acetate, which metabolizes to bicarbonate; clinicians watch acid-base balance when using acetate-containing solutions. In patients with heart failure or renal insufficiency, even normal doses may need adjustment due to sodium or potassium content. (Because it has no preservatives, once mixed it should be used promptly and any unused portion discarded.
In summary, a “TPN Electrolyte injection” is a multi-ion injection solution used as part of total parenteral nutrition. It is essentially a concentrated additive of sodium, potassium, calcium, magnesium, chloride and acetate ions designed to maintain electrolyte balance during IV feeding. It is given by IV infusion (through a central line) along with nutrients. Proper mixing and monitoring are required, and additional phosphate is added separately if needed.
TPN Electrolyte Injection Types
In total parenteral nutrition (TPN), electrolyte needs can be met either by a combined multi‐electrolyte additive or by individual (single-electrolyte) injections. The main types of IV electrolyte preparations used with TPN or other IV therapy include:
Multi-Electrolyte Additive
- TPN Electrolytes (multiple electrolyte additive): This is a proprietary concentrated mixture designed to be added into a TPN solution (typically 20 mL per liter of dextrose/amino acid infusion). It contains a fixed blend of key electrolytes: roughly 35 mEq sodium, 20 mEq potassium, 4.5 mEq calcium, 5 mEq magnesium, 35 mEq chloride, and 29.5 mEq acetate per 20 mL. (By design, it contains no phosphate.) This multi-ion solution is used exclusively as part of TPN; the manufacturer’s label notes it’s “indicated as a supplement to…concentrated dextrose and amino acids” for maintaining electrolyte balance. In practice, one vial (20 mL) is mixed into each liter of TPN base solution; phosphate (if needed) is added separately to avoid incompatibilities.
Single-Electrolyte Preparations (IV Injections)
Clinicians can also add electrolytes one at a time by using standard IV electrolyte injections. Examples include:
-
Sodium chloride injection (0.9% NS): An IV saline solution used for sodium and volume replacement. A 0.9% NaCl bag contains about 154 mEq/L of Na⁺ and 154 mEq/L of Cl⁻. It may be given alongside TPN or otherwise to provide extra sodium and water as needed.
-
Potassium chloride injection: A concentrated potassium solution for correcting hypokalemia. For example, potassium chloride for injection is supplied as a concentrate (e.g. 20 mEq per 10 mL, or 2 mEq/mL). This must be diluted in IV fluid before administration. When diluted and infused, it serves as an electrolyte replenisher (raising plasma K⁺ levels).
-
Calcium injection (gluconate or chloride): Used to treat low blood calcium. Calcium injection is a sterile IV solution of calcium salts. It is “used…to treat low levels of calcium in the body”, and is mixed into IV infusions to increase serum Ca²⁺. (Calcium gluconate is often used in TPN settings if additional calcium is needed.)
-
Magnesium injection (sulfate or chloride): Used for magnesium repletion. For instance, magnesium chloride injection is indicated “to treat or prevent magnesium deficiency”. Doses (e.g. magnesium sulfate 1–2 g) are diluted and infused to correct hypomagnesemia.
-
Phosphate injections: These are sterile solutions of phosphate salts (typically potassium phosphate or sodium phosphate). A common product is Potassium Phosphates in Sodium Chloride injection, labeled as a “phosphorus replacement product” for hypophosphatemia. This provides phosphate along with some K⁺ (and Na⁺) to restore low phosphate levels. (Because the standard multi-electrolyte additive has no phosphate, IV phosphate must be added separately when needed.)
Each of these single-electrolyte solutions is added to the IV fluids (including TPN) as needed, based on lab values. In summary: TPN electrolyte additives come either as a combined “TPN Electrolytes” injection or as individual electrolyte injections (Na⁺, K⁺, Ca²⁺, Mg²⁺, or phosphate) used to correct specific deficiencies. Proper mixing, dilution, and infusion via a central line are crucial for safety.
TPN Electrolyte Composition
Total parenteral nutrition (TPN) must supply all essential electrolytes (“salts”) to meet daily needs. In clinical practice, a TPN admixture is tailored to include sodium, potassium, calcium, magnesium, and phosphate (plus chloride or acetate as counter-ions) in roughly daily amounts that meet the patient’s requirements. Nutrition guidelines express these roughly on a per-kg basis, which for an average adult (≈70 kg) amounts to on the order of:
- Sodium (Na⁺): ≈1–1.5 mmol/kg/day. For a 70-kg adult this is ~70–105 mmol (≈70–105 mEq) of sodium per day. Sodium is usually provided as sodium chloride (NaCl) or sodium acetate.
- Potassium (K⁺): ≈1–1.5 mmol/kg/day (~70–105 mmol). Again, for a 70-kg adult about 70–105 mEq of potassium is typical. Potassium is often given as potassium chloride (KCl) or as potassium phosphate (which also contributes phosphate and potassium).
- Calcium (Ca²⁺): ≈0.10–0.15 mmol/kg/day (≈7–10 mmol). This is roughly 7–10 mEq of calcium per day. In TPN it is usually added as calcium gluconate (or less often calcium chloride), since these formulations are stable.
- Magnesium (Mg²⁺): ≈0.10–0.20 mmol/kg/day (~7–14 mmol). A 70-kg patient would receive on the order of 7–14 mEq of magnesium per day. This is typically supplied as magnesium sulfate.
- Phosphate (HPO₄²⁻): ≈0.50–0.70 mmol/kg/day (≈35–49 mmol). That corresponds to roughly 35–50 mmol of phosphate for a 70-kg person. Phosphate is given as sodium or potassium phosphate salts – often potassium phosphate – so it also adds to the potassium load.
Chloride is not listed above but is implicitly included to balance the cation loads. In practice, sodium and potassium are usually given as chloride salts (NaCl, KCl), and sometimes as acetate salts (Na/K acetate) to provide bicarbonate. The total chloride (plus acetate) content is adjusted so that sodium/potassium charges are balanced and the acid–base status is appropriate.
In summary, a typical adult TPN solution (for ~2–3 L/day) might provisionally contain on the order of about 80–120 mmol Na⁺, 80–100 mmol K⁺, 10–15 mmol Ca²⁺, 8–16 mmol Mg²⁺, and 30–50 mmol phosphate (and a matching amount of Cl⁻) per day. (Exact amounts are individualized by weight, lab values and clinical condition.) These values correspond to standard parenteral electrolyte requirements used in practice.
What is Intravenous Nutrient Therapy (IVNT)?
Intravenous nutrient therapy (IVNT) – often called “IV vitamin therapy” or “IV drips” – is a medical treatment in which vitamins, minerals and other nutrients are delivered directly into the bloodstream via an IV infusion. By bypassing the digestive system, IVNT can achieve higher blood levels of these nutrients than oral supplements. For example, one recent review notes that IV nutrient therapy “has become an increasingly popular method for delivering essential micronutrients directly into the bloodstream, bypassing the gastrointestinal tract”. This allows higher therapeutic doses and rapid replenishment, which can be useful in certain clinical situations (e.g. severe deficiencies or malabsorption).
In practice, IV nutrient formulations contain water-soluble vitamins (like vitamin C or B-complex), minerals (magnesium, zinc, etc.), antioxidants or amino acids – but typically no carbohydrates, fats or protein. (This is in contrast to a full TPN/parenteral nutrition solution, which does include dextrose, lipids and protein.) Because IV nutrient “cocktails” are relatively dilute, they can often be given via a simple peripheral IV line (instead of requiring a central line).
IVNT is used in two main ways: as a medical intervention and as a wellness/service treatment. Medically, it can benefit patients who cannot absorb nutrients normally (for example, severe malabsorption, short bowel, or certain critically ill patients). It can rapidly correct known vitamin/mineral deficiencies or support recovery when oral intake is inadequate. In the wellness world, trendy IV drip clinics offer customized infusions (e.g. “hydration drips,” vitamin cocktails, glutathione, etc.) aiming to boost energy, immunity, or recovery from hangovers and fatigue.
Key points: IV nutrient therapy simply means giving vitamins and minerals by IV infusion. It does not replace a meal or serve as full nutrition (no calories from protein/fat/carbs). Instead, it’s a way to ensure rapid delivery of micronutrients. By expert definition, it involves “sterile solutions of vitamins, minerals and other naturally occurring nutritive substances” infused into the blood. Proponents cite benefits like quicker repletion and higher bioavailability. Patients typically tolerate it well, but doctors note that many vitamins are water-soluble (excess is excreted) and stress proper medical oversight. In sum, IV nutrient therapy is an established medical practice (and increasingly a commonly marketed wellness service) for delivering nutrients directly into the bloodstream
What is a Electrolyte Imbalance?
Electrolytes are charged minerals (such as sodium, potassium, calcium, chloride, phosphate and magnesium) present in your blood and other body fluids. These ions are essential for many body functions: they help balance water and acid–base (pH) levels, and enable proper nerve and muscle activity (including the heartbeat). An electrolyte imbalance occurs when the concentration of one or more of these minerals becomes abnormally high or low. In other words, if salt or electrolyte levels in the body rise above or fall below the normal range, the body is in an electrolyte imbalance. For example, the Cleveland Clinic explains an electrolyte imbalance “occurs when certain mineral levels in your blood get too high or too low”. Such imbalances can disrupt normal cell function and often indicate an underlying problem (for instance, kidney or endocrine disease).
Role of Electrolytes
Major electrolytes include sodium (Na⁺), potassium (K⁺), calcium (Ca²⁺), magnesium (Mg²⁺), chloride (Cl⁻) and phosphate (PO₄³⁻). Electrolytes carry an electric charge, which allows them to:
- Balance the amount of water in body tissues.
- Maintain normal blood pH (acid–base balance).
- Conduct nerve impulses and enable muscle contractions (including the heartbeat).
- Transport nutrients into cells and waste out of cells.
Because electrolytes control these vital processes, even slight imbalances can cause symptoms. (Doctors detect any imbalance by ordering a blood electrolyte panel, which measures levels of sodium, potassium, etc.).
Causes of Electrolyte Imbalance
Electrolyte levels can change whenever fluid balance or organ function is altered. Common causes include:
- Fluid loss (dehydration): Vomiting, diarrhea, heavy sweating, fever or inadequate fluid intake can wash out electrolytes from the body.
- Overhydration: Drinking excessive water (water intoxication) can dilute blood electrolytes (especially sodium) below normal levels.
- Kidney or liver disorders: The kidneys and liver normally regulate electrolytes; diseases like kidney failure or liver cirrhosis can impair this balance.
- Medications: Certain drugs – for example some antibiotics, chemotherapy agents or corticosteroids – may alter electrolyte levels. (Potassium-sparing or losing diuretics are also common causes, although not listed in these sources.)
- Other conditions: Endocrine disorders (like Addison’s disease), eating disorders, and severe burns or trauma can also lead to electrolyte disturbances.
Any condition that shifts large amounts of fluid in or out of cells, or impairs kidney/urological function, can upset electrolyte balance.
Symptoms and Complications
Signs of an electrolyte imbalance vary with severity and which electrolytes are affected. Mild imbalances may cause little or no noticeable symptoms, but larger disturbances can affect many body systems. Possible symptoms include:
- Confusion, irritability or headache.
- Fatigue or weakness.
- Muscle cramps, spasms or general weakness.
- Irregular heartbeat (arrhythmia).
- Nausea, vomiting or diarrhea.
- Numbness or tingling in the hands, feet or around the mouth.
For example, low sodium (hyponatremia) can cause confusion, seizures or coma, while high potassium (hyperkalemia) can cause dangerous heart rhythms. Severe electrolyte imbalances can thus be life-threatening. As one review notes, “very high or very low levels” of electrolytes can disrupt cell functions and lead to serious, even life-threatening complications. In clinical practice, doctors check blood electrolytes when patients have symptoms like muscle cramps, weakness, palpitations, or altered mental status, since correcting the balance is critical for recovery.
In summary, an electrolyte imbalance is simply an abnormal level of one or more charged minerals in the body. Maintaining the right electrolyte balance is essential for health, and significant imbalances usually require medical attention.
TPN Electrolyte Injection Types
In total parenteral nutrition (TPN), electrolyte needs can be met either by a combined multi‐electrolyte additive or by individual (single-electrolyte) injections. The main types of IV electrolyte preparations used with TPN or other IV therapy include:
Multi-Electrolyte Additive
- TPN Electrolytes (multiple electrolyte additive): This is a proprietary concentrated mixture designed to be added into a TPN solution (typically 20 mL per liter of dextrose/amino acid infusion). It contains a fixed blend of key electrolytes: roughly 35 mEq sodium, 20 mEq potassium, 4.5 mEq calcium, 5 mEq magnesium, 35 mEq chloride, and 29.5 mEq acetate per 20 mL. (By design, it contains no phosphate.) This multi-ion solution is used exclusively as part of TPN; the manufacturer’s label notes it’s “indicated as a supplement to…concentrated dextrose and amino acids” for maintaining electrolyte balance. In practice, one vial (20 mL) is mixed into each liter of TPN base solution; phosphate (if needed) is added separately to avoid incompatibilities.
Single-Electrolyte Preparations (IV Injections)
Clinicians can also add electrolytes one at a time by using standard IV electrolyte injections. Examples include:
-
Sodium chloride injection (0.9% NS): An IV saline solution used for sodium and volume replacement. A 0.9% NaCl bag contains about 154 mEq/L of Na⁺ and 154 mEq/L of Cl⁻. It may be given alongside TPN or otherwise to provide extra sodium and water as needed.
-
Potassium chloride injection: A concentrated potassium solution for correcting hypokalemia. For example, potassium chloride for injection is supplied as a concentrate (e.g. 20 mEq per 10 mL, or 2 mEq/mL). This must be diluted in IV fluid before administration. When diluted and infused, it serves as an electrolyte replenisher (raising plasma K⁺ levels).
-
Calcium injection (gluconate or chloride): Used to treat low blood calcium. Calcium injection is a sterile IV solution of calcium salts. It is “used…to treat low levels of calcium in the body”, and is mixed into IV infusions to increase serum Ca²⁺. (Calcium gluconate is often used in TPN settings if additional calcium is needed.)
-
Magnesium injection (sulfate or chloride): Used for magnesium repletion. For instance, magnesium chloride injection is indicated “to treat or prevent magnesium deficiency”. Doses (e.g. magnesium sulfate 1–2 g) are diluted and infused to correct hypomagnesemia.
-
Phosphate injections: These are sterile solutions of phosphate salts (typically potassium phosphate or sodium phosphate). A common product is Potassium Phosphates in Sodium Chloride injection, labeled as a “phosphorus replacement product” for hypophosphatemia. This provides phosphate along with some K⁺ (and Na⁺) to restore low phosphate levels. (Because the standard multi-electrolyte additive has no phosphate, IV phosphate must be added separately when needed.)
Each of these single-electrolyte solutions is added to the IV fluids (including TPN) as needed, based on lab values. In summary: TPN electrolyte additives come either as a combined “TPN Electrolytes” injection or as individual electrolyte injections (Na⁺, K⁺, Ca²⁺, Mg²⁺, or phosphate) used to correct specific deficiencies. Proper mixing, dilution, and infusion via a central line are crucial for safety.
TPN Electrolyte Composition
Total parenteral nutrition (TPN) must supply all essential electrolytes (“salts”) to meet daily needs. In clinical practice, a TPN admixture is tailored to include sodium, potassium, calcium, magnesium, and phosphate (plus chloride or acetate as counter-ions) in roughly daily amounts that meet the patient’s requirements. Nutrition guidelines express these roughly on a per-kg basis, which for an average adult (≈70 kg) amounts to on the order of:
- Sodium (Na⁺): ≈1–1.5 mmol/kg/day. For a 70-kg adult this is ~70–105 mmol (≈70–105 mEq) of sodium per day. Sodium is usually provided as sodium chloride (NaCl) or sodium acetate.
- Potassium (K⁺): ≈1–1.5 mmol/kg/day (~70–105 mmol). Again, for a 70-kg adult about 70–105 mEq of potassium is typical. Potassium is often given as potassium chloride (KCl) or as potassium phosphate (which also contributes phosphate and potassium).
- Calcium (Ca²⁺): ≈0.10–0.15 mmol/kg/day (≈7–10 mmol). This is roughly 7–10 mEq of calcium per day. In TPN it is usually added as calcium gluconate (or less often calcium chloride), since these formulations are stable.
- Magnesium (Mg²⁺): ≈0.10–0.20 mmol/kg/day (~7–14 mmol). A 70-kg patient would receive on the order of 7–14 mEq of magnesium per day. This is typically supplied as magnesium sulfate.
- Phosphate (HPO₄²⁻): ≈0.50–0.70 mmol/kg/day (≈35–49 mmol). That corresponds to roughly 35–50 mmol of phosphate for a 70-kg person. Phosphate is given as sodium or potassium phosphate salts – often potassium phosphate – so it also adds to the potassium load.
Chloride is not listed above but is implicitly included to balance the cation loads. In practice, sodium and potassium are usually given as chloride salts (NaCl, KCl), and sometimes as acetate salts (Na/K acetate) to provide bicarbonate. The total chloride (plus acetate) content is adjusted so that sodium/potassium charges are balanced and the acid–base status is appropriate.
In summary, a typical adult TPN solution (for ~2–3 L/day) might provisionally contain on the order of about 80–120 mmol Na⁺, 80–100 mmol K⁺, 10–15 mmol Ca²⁺, 8–16 mmol Mg²⁺, and 30–50 mmol phosphate (and a matching amount of Cl⁻) per day. (Exact amounts are individualized by weight, lab values and clinical condition.) These values correspond to standard parenteral electrolyte requirements used in practice.
What is Intravenous Nutrient Therapy (IVNT)?
Intravenous nutrient therapy (IVNT) – often called “IV vitamin therapy” or “IV drips” – is a medical treatment in which vitamins, minerals and other nutrients are delivered directly into the bloodstream via an IV infusion. By bypassing the digestive system, IVNT can achieve higher blood levels of these nutrients than oral supplements. For example, one recent review notes that IV nutrient therapy “has become an increasingly popular method for delivering essential micronutrients directly into the bloodstream, bypassing the gastrointestinal tract”. This allows higher therapeutic doses and rapid replenishment, which can be useful in certain clinical situations (e.g. severe deficiencies or malabsorption).
In practice, IV nutrient formulations contain water-soluble vitamins (like vitamin C or B-complex), minerals (magnesium, zinc, etc.), antioxidants or amino acids – but typically no carbohydrates, fats or protein. (This is in contrast to a full TPN/parenteral nutrition solution, which does include dextrose, lipids and protein.) Because IV nutrient “cocktails” are relatively dilute, they can often be given via a simple peripheral IV line (instead of requiring a central line).
IVNT is used in two main ways: as a medical intervention and as a wellness/service treatment. Medically, it can benefit patients who cannot absorb nutrients normally (for example, severe malabsorption, short bowel, or certain critically ill patients). It can rapidly correct known vitamin/mineral deficiencies or support recovery when oral intake is inadequate. In the wellness world, trendy IV drip clinics offer customized infusions (e.g. “hydration drips,” vitamin cocktails, glutathione, etc.) aiming to boost energy, immunity, or recovery from hangovers and fatigue.
Key points: IV nutrient therapy simply means giving vitamins and minerals by IV infusion. It does not replace a meal or serve as full nutrition (no calories from protein/fat/carbs). Instead, it’s a way to ensure rapid delivery of micronutrients. By expert definition, it involves “sterile solutions of vitamins, minerals and other naturally occurring nutritive substances” infused into the blood. Proponents cite benefits like quicker repletion and higher bioavailability. Patients typically tolerate it well, but doctors note that many vitamins are water-soluble (excess is excreted) and stress proper medical oversight. In sum, IV nutrient therapy is an established medical practice (and increasingly a commonly marketed wellness service) for delivering nutrients directly into the bloodstream
What is a Electrolyte Imbalance?
Electrolytes are charged minerals (such as sodium, potassium, calcium, chloride, phosphate and magnesium) present in your blood and other body fluids. These ions are essential for many body functions: they help balance water and acid–base (pH) levels, and enable proper nerve and muscle activity (including the heartbeat). An electrolyte imbalance occurs when the concentration of one or more of these minerals becomes abnormally high or low. In other words, if salt or electrolyte levels in the body rise above or fall below the normal range, the body is in an electrolyte imbalance. For example, the Cleveland Clinic explains an electrolyte imbalance “occurs when certain mineral levels in your blood get too high or too low”. Such imbalances can disrupt normal cell function and often indicate an underlying problem (for instance, kidney or endocrine disease).
Role of Electrolytes
Major electrolytes include sodium (Na⁺), potassium (K⁺), calcium (Ca²⁺), magnesium (Mg²⁺), chloride (Cl⁻) and phosphate (PO₄³⁻). Electrolytes carry an electric charge, which allows them to:
- Balance the amount of water in body tissues.
- Maintain normal blood pH (acid–base balance).
- Conduct nerve impulses and enable muscle contractions (including the heartbeat).
- Transport nutrients into cells and waste out of cells.
Because electrolytes control these vital processes, even slight imbalances can cause symptoms. (Doctors detect any imbalance by ordering a blood electrolyte panel, which measures levels of sodium, potassium, etc.).
Causes of Electrolyte Imbalance
Electrolyte levels can change whenever fluid balance or organ function is altered. Common causes include:
- Fluid loss (dehydration): Vomiting, diarrhea, heavy sweating, fever or inadequate fluid intake can wash out electrolytes from the body.
- Overhydration: Drinking excessive water (water intoxication) can dilute blood electrolytes (especially sodium) below normal levels.
- Kidney or liver disorders: The kidneys and liver normally regulate electrolytes; diseases like kidney failure or liver cirrhosis can impair this balance.
- Medications: Certain drugs – for example some antibiotics, chemotherapy agents or corticosteroids – may alter electrolyte levels. (Potassium-sparing or losing diuretics are also common causes, although not listed in these sources.)
- Other conditions: Endocrine disorders (like Addison’s disease), eating disorders, and severe burns or trauma can also lead to electrolyte disturbances.
Any condition that shifts large amounts of fluid in or out of cells, or impairs kidney/urological function, can upset electrolyte balance.
Symptoms and Complications
Signs of an electrolyte imbalance vary with severity and which electrolytes are affected. Mild imbalances may cause little or no noticeable symptoms, but larger disturbances can affect many body systems. Possible symptoms include:
- Confusion, irritability or headache.
- Fatigue or weakness.
- Muscle cramps, spasms or general weakness.
- Irregular heartbeat (arrhythmia).
- Nausea, vomiting or diarrhea.
- Numbness or tingling in the hands, feet or around the mouth.
For example, low sodium (hyponatremia) can cause confusion, seizures or coma, while high potassium (hyperkalemia) can cause dangerous heart rhythms. Severe electrolyte imbalances can thus be life-threatening. As one review notes, “very high or very low levels” of electrolytes can disrupt cell functions and lead to serious, even life-threatening complications. In clinical practice, doctors check blood electrolytes when patients have symptoms like muscle cramps, weakness, palpitations, or altered mental status, since correcting the balance is critical for recovery.
In summary, an electrolyte imbalance is simply an abnormal level of one or more charged minerals in the body. Maintaining the right electrolyte balance is essential for health, and significant imbalances usually require medical attention.










