Filters
Yeast Infection Treatments, Creams & Medicines to Treat Fungal Meningitis
A yeast infection usually refers to a vaginal yeast infection (vulvovaginal candidiasis), which is an overgrowth of Candida yeast in the vagina. Normally, a small amount of yeast lives in the vagina without causing issues, but factors like taking antibiotics, high stress, pregnancy, or even staying in a wet bathing suit too long can upset the natural balance and let yeast multiply. This leads to classic symptoms: intense itching, redness, swelling of the vulva, a burning sensation (especially during urination or sex), and often a thick, odorless white discharge that looks like cottage cheese. Yeast infections are very common – about 75% of women (and people assigned female at birth) will experience at least one in their lifetime. The good news is that yeast infections are highly treatable. Treatments come in two main forms: antifungal creams or suppositories that you apply directly in the vagina, and oral antifungal medications (pills) that treat the infection from the inside out. There are also some at-home remedies people try, but the most reliable cures are the medicated antifungal treatments.
Treatments for yeast infections primarily involve antifungal medications: either applied directly in the vagina (creams, suppositories) or taken by mouth (pills). Over-the-counter azole antifungals like miconazole or clotrimazole successfully cure most mild yeast infections. For tougher cases, doctors can prescribe stronger or longer therapy – such as fluconazole pills or other new medications – to fully clear the infection. While home remedies might ease things a bit, they’re not proven cures, so it’s best to rely on the antifungal treatments to get rid of the yeast. With proper treatment, most yeast infections improve within a few days and are fully resolved within a week or so If infections keep recurring, talk to a healthcare provider about longer-term strategies to keep the yeast in check. Remember, yeast infections are very common and nothing to be embarrassed about – and with the right approach, they’re very manageable and curable.
-
 Sale 65%
Original price $ 39.95Current price $ 13.95
Sale 65%
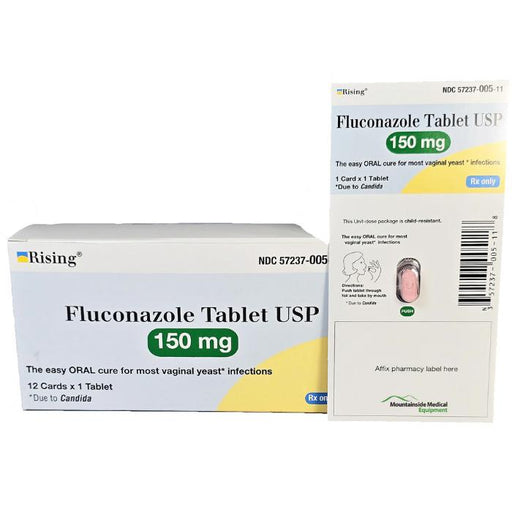
Original price $ 39.95Current price $ 13.95Fluconazole Tablets 150 mg 1 Tablet per Card x 12 Cards per Box (Rx)
Rising Pharmaceuticals1 reviewThe #1 Trusted Prescription Antifungal for Treating Yeast Infection, Vaginal Candidiasis & Thrush Treatment Are you searching for rapid, effect...
View full details🔒 Medical License Required -
 Sale 23%
Original price $ 129.00Current price $ 99.80
Sale 23%
Original price $ 129.00Current price $ 99.80Fluconazole 200 mg Tablets by Glenmark Pharma 30 Count (Rx)
Glenmark PharmaceuticalsNo reviewsFluconazole Tablets 200 mg are used to treat various fungal infections, including those caused by Candida species, such as vaginal yeast infections...
View full details🔒 Medical License Required -
 Sale 19%
Original price $ 85.00Current price $ 69.00
Sale 19%
Original price $ 85.00Current price $ 69.00Fluconazole Tablets 100 mg by Glenmark Pharma 30 Count (RX)
Glenmark PharmaceuticalsNo reviewsFluconazole Tablets 100 mg are primarily used to treat and prevent fungal infections, including those caused by Candida species. These infections c...
View full details🔒 Medical License Required -
 Sale 21%
Original price $ 74.95Current price $ 59.00
Sale 21%
Original price $ 74.95Current price $ 59.00Voriconazole Injection 200 mg Powder Vial by Fosun Pharma (RX)
Fosun Pharma USANo reviewsVoriconazole injection is used to treat serious fungal infections, including invasive aspergillosis and certain serious Candida infections. It's ty...
View full details🔒 Medical License Required -
 Sale 31%
Original price $ 23.95Current price $ 16.50
Sale 31%
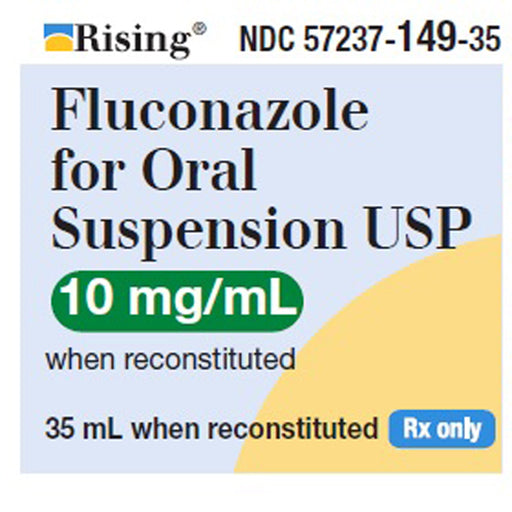
Original price $ 23.95Current price $ 16.50Fluconazole for Oral Suspension 10 mg/mL when Reconstituted 35 mL Bottle by Rising Pharma
Rising PharmaceuticalsNo reviewsFluconazole for Oral Suspension 10 mg/mL is prescribed to treat various fungal infections, notably those caused by Candida species, such as oral th...
View full details🔒 Medical License Required -
 Sale 28%
Original price $ 54.50Current price $ 39.00
Sale 28%
Original price $ 54.50Current price $ 39.00Fluconazole Tablets 50 mg by Glenmark Pharma 30 Count (RX)
Glenmark PharmaceuticalsNo reviewsFluconazole Tablets 50 mg are used to treat minor fungal infections, such as those caused by Candida species, including mild vaginal yeast infectio...
View full details🔒 Medical License Required
People Also Searched For
A yeast infection usually refers to a vaginal yeast infection (vulvovaginal candidiasis), which is an overgrowth of Candida yeast in the vagina. Normally, a small amount of yeast lives in the vagina without causing issues, but factors like taking antibiotics, high stress, pregnancy, or even staying in a wet bathing suit too long can upset the natural balance and let yeast multiply. This leads to classic symptoms: intense itching, redness, swelling of the vulva, a burning sensation (especially during urination or sex), and often a thick, odorless white discharge that looks like cottage cheese. Yeast infections are very common – about 75% of women (and people assigned female at birth) will experience at least one in their lifetime. The good news is that yeast infections are highly treatable. Treatments come in two main forms: antifungal creams or suppositories that you apply directly in the vagina, and oral antifungal medications (pills) that treat the infection from the inside out. There are also some at-home remedies people try, but the most reliable cures are the medicated antifungal treatments.
Treatments for yeast infections primarily involve antifungal medications: either applied directly in the vagina (creams, suppositories) or taken by mouth (pills). Over-the-counter azole antifungals like miconazole or clotrimazole successfully cure most mild yeast infections. For tougher cases, doctors can prescribe stronger or longer therapy – such as fluconazole pills or other new medications – to fully clear the infection. While home remedies might ease things a bit, they’re not proven cures, so it’s best to rely on the antifungal treatments to get rid of the yeast. With proper treatment, most yeast infections improve within a few days and are fully resolved within a week or so If infections keep recurring, talk to a healthcare provider about longer-term strategies to keep the yeast in check. Remember, yeast infections are very common and nothing to be embarrassed about – and with the right approach, they’re very manageable and curable.
Over-the-Counter Antifungal Treatments (Creams/Suppositories)
For uncomplicated yeast infections, over-the-counter (OTC) antifungal vaginal creams and suppositories are the first choice. You can buy these at pharmacies and supermarkets without a prescription, and they are specifically made to kill yeast in the vagina. These antifungal products typically contain medications from the azole family that are very effective against Candida. Common active ingredients and products include:
- Miconazole – Brand name Monistat, available as 1-day, 3-day, or 7-day treatments. Miconazole is a topical antifungal that you insert into the vagina (either as a cream or ovule suppository) and/or apply around the outside. The numbers (1-day, 3-day, etc.) refer to how many consecutive days you use the medicine. For example, Monistat-7 is a lower dose you use for 7 nights, while Monistat-1 is a single high-dose treatment. All are effective; however, the single-dose (1-day) treatments have a much higher concentration of medication (for instance, 1200 mg of miconazole in one dose vs. about 100 mg per dose in a 7-day treatment). This can sometimes cause more burning or irritation in some women. If you experience irritation with a 1-day treatment, a longer-course (3 or 7-day) regimen might be gentler since the dose per day is lower.
- Clotrimazole – Found in products like Lotrimin AF® Vaginal or Mycelex®. These are often 3-day or 7-day cream treatments. Clotrimazole is another azole antifungal that you apply inside the vagina using an applicator. It’s similarly effective to miconazole. Many generic store-brand yeast infection creams also use clotrimazole as the active ingredient.
- Tioconazole – Found in Vagistat-1®, typically sold as a 1-day ovule (egg-shaped suppository) or ointment. Tioconazole is a potent antifungal and the one-dose treatment is convenient for those who want a short course. As with Monistat-1, some women may feel temporary burning due to the concentrated dose.
- Butoconazole – This one is usually a prescription-strength one-day cream (brand Gynazole-1®), but recently some butoconazole single-dose treatments have become available OTC as well. It’s an alternative azole antifungal used as a vaginal cream, often with an applicator that pre-fills the correct dose.
- Terconazole – Sold under brand name Terazol®, this is a prescription azole cream or suppository. It comes in 3-day or 7-day regimens of various strengths. Terconazole is typically used if OTC treatments haven’t worked or if a doctor prefers to prescribe it for a particular case.
Most OTC yeast infection products are sold in pre-packaged kits that include either a tube of cream with disposable applicators or individually packaged suppositories, plus often a tube of external anti-itch cream. The external cream (often containing a mild antifungal and a soothing ingredient) can be applied to the vulva to alleviate itching of the outside skin, while the internal cream or suppository treats the yeast inside the vagina. Be sure to use the treatment for the full number of days directed, even if you feel better sooner. Many OTC antifungal regimens come in 1-day, 3-day, or 7-day options. Interestingly, these options all have been shown to cure a yeast infection effectively; the difference is just how strong each dose is and how long you treat. Women often choose based on convenience or past experience. If you’re unsure, a 3-day or 7-day course might cause less irritation while still clearing the infection in about a week. With proper use, you should start feeling relief from symptoms like itching and burning after a couple days, but continue the treatment through to the end to fully eradicate the yeast.
How to use vaginal antifungal products: It’s usually best to administer them at bedtime (so the medicine stays inside longer while you lie down). Wash your hands, fill the applicator (if it’s a cream) or unwrap the suppository, and gently insert it into the vagina as far as comfortable, then release the medication. If using a cream, you might want to wear a light panty liner, as there can be some drainage of the cream. Expect some mild burning or discomfort right after application – that can be normal, but it should be temporary. Over the next days, symptoms should gradually improve. If you happen to be on your period, most products say you can still use them (avoid tampons though; use pads and change frequently). Do not douche while treating a yeast infection with these products; douching isn’t recommended in general, as it can upset the vaginal balance further.
OTC antifungal creams and suppositories are quite effective for the majority of yeast infections. However, if your symptoms do not improve after completing an OTC course, or they come back quickly, you should see a doctor. It’s possible you may have a resistant yeast strain or a different problem (like bacterial vaginosis or another kind of infection) that can mimic yeast infection symptoms. Also, if this is your first suspected yeast infection, it’s a good idea to get a medical confirmation. Once a doctor has told you it’s a yeast infection, you can confidently self-treat subsequent mild infections with OTC products. But many vaginal issues are not yeast, so proper diagnosis is key if you’re unsure.
Prescription Antifungal Medications
If over-the-counter remedies don’t work or if you have a severe yeast infection, your healthcare provider can prescribe stronger treatments. These include both prescription topical azole creams (as mentioned, like terconazole or a stronger dose of butoconazole) and oral antifungal medicines. The most commonly prescribed oral medication for vaginal yeast infection is fluconazole, known by the brand name Diflucan.
-
Fluconazole (Diflucan): This is a single-dose antifungal pill in many cases – you take one 150 mg tablet by mouth to treat a typical yeast infection. It works by circulating through your bloodstream and body tissues to kill yeast wherever it’s growing. Many women find it convenient since you don’t have to deal with creams; symptoms usually start to improve within one to two days after taking the pill. Sometimes, for more stubborn infections, doctors prescribe fluconazole in multiple doses (for example, one pill every 3 days for a total of 2-3 pills). For instance, a common regimen for a tough yeast infection might be to take a dose on day 1, another on day 4, and another on day 7 . If yeast infections are recurrent (happening 4+ times a year), a doctor may recommend a longer course of fluconazole – such as one pill weekly for 6 months – to prevent new infections. Fluconazole is generally safe and very effective; however, it should not be used during pregnancy unless specifically advised by a doctor and it can occasionally cause side effects like stomach upset, headache, or rash. It also can interact with some other medications, so confirm with your doctor or pharmacist if you’re taking other drugs.
-
Ibrexafungerp (Brexafemme): This is a new oral antifungal approved in 2021 for vaginal yeast infections. It’s in a different class (called triterpenoids) and is also taken by mouth. The treatment involves taking a pill twice in one day (one dose in the morning, one in the evening). It works by targeting the fungal cell wall in a unique way. Brexafemme is usually prescribed for infections that might not respond to fluconazole or for women who can’t take azoles. As a newer medication, it can be more expensive and isn’t first-line for an uncomplicated yeast infection, but it’s an important option especially as some Candida strains can develop resistance to fluconazole. Like fluconazole, Brexafemme is not used in pregnancy. Common side effects can include gastrointestinal upset or dizziness.
-
Oteseconazole (Vivjoa): Another new oral antifungal (approved in 2022), but this one is specifically aimed at recurrent yeast infections in certain groups of women. Vivjoa is approved for use in postmenopausal women or those who are permanently infertile (for example, women who have had their uterus and ovaries removed). It’s not allowed for anyone who could become pregnant because of concerns about effects on a fetus. This medication is usually given as a longer course (e.g., daily pills for a couple weeks) to eliminate any resident yeast and then protect against recurrence. It’s an option if other treatments aren’t keeping chronic yeast infections at bay.
-
Boric Acid Suppositories: While not a traditional “medicine” in pill or cream form, boric acid vaginal capsules are a prescription or recommended treatment for recurrent or hard-to-treat yeast infections, especially those caused by non-albicans Candida species. Boric acid is a mild antiseptic that, when inserted as a capsule into the vagina (usually 600 mg), can help clear yeast that isn’t responding to azole antifungals. Typically, a 14-day nightly course is used for an active infection, or a few times a week as maintenance to prevent recurrence. Important: Boric acid is only for vaginal use – never take it by mouth, and keep it away from children. It can cause irritation in some women, but many tolerate it well and find it effective for chronic yeast issues. This treatment is usually guided by a healthcare provider.
Note on Men and Yeast: Yeast infections primarily affect women’s vaginal area, but men can get a form of yeast infection on the penis (called candidal balanitis) or other skin folds. The treatment in men often involves applying a topical antifungal cream (like clotrimazole or miconazole) to the affected area twice daily for a week or two. If a woman has a yeast infection, her male sexual partner doesn’t automatically need treatment unless he has symptoms. But if recurrent infections occur, sometimes both partners treat to prevent ping-pong reinfection.
At-Home Remedies and Other Considerations
Because yeast infections are so common, there are many home remedies and over-the-counter “natural” products touted for relief. Examples include using plain yogurt or probiotic suppositories in the vagina (to introduce good bacteria), applying coconut oil or inserting garlic cloves, douching with apple cider vinegar, etc. It’s important to know that while some of these might provide temporary relief or have mild antifungal properties, none of them are proven cures for an active yeast infection.. For instance, lab studies show coconut oil can inhibit candida growth, but it hasn’t been clinically proven to treat vaginal yeast infections in people. Garlic and tea tree oil have antifungal components too, but they can also irritate delicate vaginal tissue and have not been reliably shown to eliminate infection. Baking soda or vinegar baths might soothe itching for some, but won’t eradicate yeast hiding in the vaginal canal. Probiotics (like lactobacillus pills or eating yogurt) may help restore healthy vaginal flora and are a good supportive approach, especially if you’ve been on antibiotics, but during an active infection they are not a stand-alone cure. Essentially, you can try certain gentle home approaches if your symptoms are very mild or you’re just starting to feel an imbalance, but if a true yeast infection has developed, antifungal medications are by far the most effective way to knock it out.
A couple of other points to consider during treatment:
-
Symptomatic Relief: Yeast infections can be miserable with all the itching and burning. While the antifungal is doing its work (which can take a couple days to fully relieve symptoms), you can use some comfort measures. Applying a cool compress to the vulva or sitting in a cool (not hot) bath can calm the itch. The external cream provided in OTC kits often contains an ingredient (like benzocaine or hydrocortisone) to numb or soothe the itch – use it sparingly on the irritated skin outside. Avoid harsh soaps or douches; use plain water or a mild, fragrance-free cleanser for the vulva during this time. And wear loose, breathable cotton underwear and clothing to help keep the area dry and cool; tight or synthetic pants can trap moisture and heat, feeding the yeast.
-
Sex and Yeast Infections: It’s generally advised to avoid sexual intercourse (especially vaginal intercourse) until the yeast infection is fully treated and healed. Not only can it be uncomfortable, but yeast infections can sometimes be passed back and forth. Also, antifungal creams and suppositories can weaken latex condoms or diaphragms, so use alternative protection if needed. If you must have sex, be aware of these issues and consider using condoms made of non-latex materials, but again, ideally wait until treatment is done.
-
When to See a Doctor: If this is your first ever yeast infection, see a healthcare provider to confirm the diagnosis before self-treating – other conditions like bacterial vaginosis or STDs can mimic yeast infection symptoms. Also see a doctor if you keep getting yeast infections (more than 3-4 per year), if symptoms don’t get better after treatment, or if you have unusual symptoms like a foul odor (yeast infections typically do not cause a bad smell; a bad odor could suggest bacterial vaginosis or another issue). Pregnant women should consult a provider for yeast infections; treatment is usually a 7-day topical azole (like Monistat-7 or a prescription azole) – oral fluconazole is not recommended in pregnancy. And of course, if you develop fever, pelvic pain, or very severe symptoms, get medical care as those might indicate a different or more serious problem.
In summary, treatments for yeast infections primarily involve antifungal medications: either applied directly in the vagina (creams, suppositories) or taken by mouth (pills). Over-the-counter azole antifungals like miconazole or clotrimazole successfully cure most mild yeast infections. For tougher cases, doctors can prescribe stronger or longer therapy – such as fluconazole pills or other new medications – to fully clear the infection. While home remedies might ease things a bit, they’re not proven cures, so it’s best to rely on the antifungal treatments to get rid of the yeast. With proper treatment, most yeast infections improve within a few days and are fully resolved within a week or so If infections keep recurring, talk to a healthcare provider about longer-term strategies to keep the yeast in check. Remember, yeast infections are very common and nothing to be embarrassed about – and with the right approach, they’re very manageable and curable.
Over-the-Counter Antifungal Treatments (Creams/Suppositories)
For uncomplicated yeast infections, over-the-counter (OTC) antifungal vaginal creams and suppositories are the first choice. You can buy these at pharmacies and supermarkets without a prescription, and they are specifically made to kill yeast in the vagina. These antifungal products typically contain medications from the azole family that are very effective against Candida. Common active ingredients and products include:
- Miconazole – Brand name Monistat, available as 1-day, 3-day, or 7-day treatments. Miconazole is a topical antifungal that you insert into the vagina (either as a cream or ovule suppository) and/or apply around the outside. The numbers (1-day, 3-day, etc.) refer to how many consecutive days you use the medicine. For example, Monistat-7 is a lower dose you use for 7 nights, while Monistat-1 is a single high-dose treatment. All are effective; however, the single-dose (1-day) treatments have a much higher concentration of medication (for instance, 1200 mg of miconazole in one dose vs. about 100 mg per dose in a 7-day treatment). This can sometimes cause more burning or irritation in some women. If you experience irritation with a 1-day treatment, a longer-course (3 or 7-day) regimen might be gentler since the dose per day is lower.
- Clotrimazole – Found in products like Lotrimin AF® Vaginal or Mycelex®. These are often 3-day or 7-day cream treatments. Clotrimazole is another azole antifungal that you apply inside the vagina using an applicator. It’s similarly effective to miconazole. Many generic store-brand yeast infection creams also use clotrimazole as the active ingredient.
- Tioconazole – Found in Vagistat-1®, typically sold as a 1-day ovule (egg-shaped suppository) or ointment. Tioconazole is a potent antifungal and the one-dose treatment is convenient for those who want a short course. As with Monistat-1, some women may feel temporary burning due to the concentrated dose.
- Butoconazole – This one is usually a prescription-strength one-day cream (brand Gynazole-1®), but recently some butoconazole single-dose treatments have become available OTC as well. It’s an alternative azole antifungal used as a vaginal cream, often with an applicator that pre-fills the correct dose.
- Terconazole – Sold under brand name Terazol®, this is a prescription azole cream or suppository. It comes in 3-day or 7-day regimens of various strengths. Terconazole is typically used if OTC treatments haven’t worked or if a doctor prefers to prescribe it for a particular case.
Most OTC yeast infection products are sold in pre-packaged kits that include either a tube of cream with disposable applicators or individually packaged suppositories, plus often a tube of external anti-itch cream. The external cream (often containing a mild antifungal and a soothing ingredient) can be applied to the vulva to alleviate itching of the outside skin, while the internal cream or suppository treats the yeast inside the vagina. Be sure to use the treatment for the full number of days directed, even if you feel better sooner. Many OTC antifungal regimens come in 1-day, 3-day, or 7-day options. Interestingly, these options all have been shown to cure a yeast infection effectively; the difference is just how strong each dose is and how long you treat. Women often choose based on convenience or past experience. If you’re unsure, a 3-day or 7-day course might cause less irritation while still clearing the infection in about a week. With proper use, you should start feeling relief from symptoms like itching and burning after a couple days, but continue the treatment through to the end to fully eradicate the yeast.
How to use vaginal antifungal products: It’s usually best to administer them at bedtime (so the medicine stays inside longer while you lie down). Wash your hands, fill the applicator (if it’s a cream) or unwrap the suppository, and gently insert it into the vagina as far as comfortable, then release the medication. If using a cream, you might want to wear a light panty liner, as there can be some drainage of the cream. Expect some mild burning or discomfort right after application – that can be normal, but it should be temporary. Over the next days, symptoms should gradually improve. If you happen to be on your period, most products say you can still use them (avoid tampons though; use pads and change frequently). Do not douche while treating a yeast infection with these products; douching isn’t recommended in general, as it can upset the vaginal balance further.
OTC antifungal creams and suppositories are quite effective for the majority of yeast infections. However, if your symptoms do not improve after completing an OTC course, or they come back quickly, you should see a doctor. It’s possible you may have a resistant yeast strain or a different problem (like bacterial vaginosis or another kind of infection) that can mimic yeast infection symptoms. Also, if this is your first suspected yeast infection, it’s a good idea to get a medical confirmation. Once a doctor has told you it’s a yeast infection, you can confidently self-treat subsequent mild infections with OTC products. But many vaginal issues are not yeast, so proper diagnosis is key if you’re unsure.
Prescription Antifungal Medications
If over-the-counter remedies don’t work or if you have a severe yeast infection, your healthcare provider can prescribe stronger treatments. These include both prescription topical azole creams (as mentioned, like terconazole or a stronger dose of butoconazole) and oral antifungal medicines. The most commonly prescribed oral medication for vaginal yeast infection is fluconazole, known by the brand name Diflucan.
-
Fluconazole (Diflucan): This is a single-dose antifungal pill in many cases – you take one 150 mg tablet by mouth to treat a typical yeast infection. It works by circulating through your bloodstream and body tissues to kill yeast wherever it’s growing. Many women find it convenient since you don’t have to deal with creams; symptoms usually start to improve within one to two days after taking the pill. Sometimes, for more stubborn infections, doctors prescribe fluconazole in multiple doses (for example, one pill every 3 days for a total of 2-3 pills). For instance, a common regimen for a tough yeast infection might be to take a dose on day 1, another on day 4, and another on day 7 . If yeast infections are recurrent (happening 4+ times a year), a doctor may recommend a longer course of fluconazole – such as one pill weekly for 6 months – to prevent new infections. Fluconazole is generally safe and very effective; however, it should not be used during pregnancy unless specifically advised by a doctor and it can occasionally cause side effects like stomach upset, headache, or rash. It also can interact with some other medications, so confirm with your doctor or pharmacist if you’re taking other drugs.
-
Ibrexafungerp (Brexafemme): This is a new oral antifungal approved in 2021 for vaginal yeast infections. It’s in a different class (called triterpenoids) and is also taken by mouth. The treatment involves taking a pill twice in one day (one dose in the morning, one in the evening). It works by targeting the fungal cell wall in a unique way. Brexafemme is usually prescribed for infections that might not respond to fluconazole or for women who can’t take azoles. As a newer medication, it can be more expensive and isn’t first-line for an uncomplicated yeast infection, but it’s an important option especially as some Candida strains can develop resistance to fluconazole. Like fluconazole, Brexafemme is not used in pregnancy. Common side effects can include gastrointestinal upset or dizziness.
-
Oteseconazole (Vivjoa): Another new oral antifungal (approved in 2022), but this one is specifically aimed at recurrent yeast infections in certain groups of women. Vivjoa is approved for use in postmenopausal women or those who are permanently infertile (for example, women who have had their uterus and ovaries removed). It’s not allowed for anyone who could become pregnant because of concerns about effects on a fetus. This medication is usually given as a longer course (e.g., daily pills for a couple weeks) to eliminate any resident yeast and then protect against recurrence. It’s an option if other treatments aren’t keeping chronic yeast infections at bay.
-
Boric Acid Suppositories: While not a traditional “medicine” in pill or cream form, boric acid vaginal capsules are a prescription or recommended treatment for recurrent or hard-to-treat yeast infections, especially those caused by non-albicans Candida species. Boric acid is a mild antiseptic that, when inserted as a capsule into the vagina (usually 600 mg), can help clear yeast that isn’t responding to azole antifungals. Typically, a 14-day nightly course is used for an active infection, or a few times a week as maintenance to prevent recurrence. Important: Boric acid is only for vaginal use – never take it by mouth, and keep it away from children. It can cause irritation in some women, but many tolerate it well and find it effective for chronic yeast issues. This treatment is usually guided by a healthcare provider.
Note on Men and Yeast: Yeast infections primarily affect women’s vaginal area, but men can get a form of yeast infection on the penis (called candidal balanitis) or other skin folds. The treatment in men often involves applying a topical antifungal cream (like clotrimazole or miconazole) to the affected area twice daily for a week or two. If a woman has a yeast infection, her male sexual partner doesn’t automatically need treatment unless he has symptoms. But if recurrent infections occur, sometimes both partners treat to prevent ping-pong reinfection.
At-Home Remedies and Other Considerations
Because yeast infections are so common, there are many home remedies and over-the-counter “natural” products touted for relief. Examples include using plain yogurt or probiotic suppositories in the vagina (to introduce good bacteria), applying coconut oil or inserting garlic cloves, douching with apple cider vinegar, etc. It’s important to know that while some of these might provide temporary relief or have mild antifungal properties, none of them are proven cures for an active yeast infection.. For instance, lab studies show coconut oil can inhibit candida growth, but it hasn’t been clinically proven to treat vaginal yeast infections in people. Garlic and tea tree oil have antifungal components too, but they can also irritate delicate vaginal tissue and have not been reliably shown to eliminate infection. Baking soda or vinegar baths might soothe itching for some, but won’t eradicate yeast hiding in the vaginal canal. Probiotics (like lactobacillus pills or eating yogurt) may help restore healthy vaginal flora and are a good supportive approach, especially if you’ve been on antibiotics, but during an active infection they are not a stand-alone cure. Essentially, you can try certain gentle home approaches if your symptoms are very mild or you’re just starting to feel an imbalance, but if a true yeast infection has developed, antifungal medications are by far the most effective way to knock it out.
A couple of other points to consider during treatment:
-
Symptomatic Relief: Yeast infections can be miserable with all the itching and burning. While the antifungal is doing its work (which can take a couple days to fully relieve symptoms), you can use some comfort measures. Applying a cool compress to the vulva or sitting in a cool (not hot) bath can calm the itch. The external cream provided in OTC kits often contains an ingredient (like benzocaine or hydrocortisone) to numb or soothe the itch – use it sparingly on the irritated skin outside. Avoid harsh soaps or douches; use plain water or a mild, fragrance-free cleanser for the vulva during this time. And wear loose, breathable cotton underwear and clothing to help keep the area dry and cool; tight or synthetic pants can trap moisture and heat, feeding the yeast.
-
Sex and Yeast Infections: It’s generally advised to avoid sexual intercourse (especially vaginal intercourse) until the yeast infection is fully treated and healed. Not only can it be uncomfortable, but yeast infections can sometimes be passed back and forth. Also, antifungal creams and suppositories can weaken latex condoms or diaphragms, so use alternative protection if needed. If you must have sex, be aware of these issues and consider using condoms made of non-latex materials, but again, ideally wait until treatment is done.
-
When to See a Doctor: If this is your first ever yeast infection, see a healthcare provider to confirm the diagnosis before self-treating – other conditions like bacterial vaginosis or STDs can mimic yeast infection symptoms. Also see a doctor if you keep getting yeast infections (more than 3-4 per year), if symptoms don’t get better after treatment, or if you have unusual symptoms like a foul odor (yeast infections typically do not cause a bad smell; a bad odor could suggest bacterial vaginosis or another issue). Pregnant women should consult a provider for yeast infections; treatment is usually a 7-day topical azole (like Monistat-7 or a prescription azole) – oral fluconazole is not recommended in pregnancy. And of course, if you develop fever, pelvic pain, or very severe symptoms, get medical care as those might indicate a different or more serious problem.
In summary, treatments for yeast infections primarily involve antifungal medications: either applied directly in the vagina (creams, suppositories) or taken by mouth (pills). Over-the-counter azole antifungals like miconazole or clotrimazole successfully cure most mild yeast infections. For tougher cases, doctors can prescribe stronger or longer therapy – such as fluconazole pills or other new medications – to fully clear the infection. While home remedies might ease things a bit, they’re not proven cures, so it’s best to rely on the antifungal treatments to get rid of the yeast. With proper treatment, most yeast infections improve within a few days and are fully resolved within a week or so If infections keep recurring, talk to a healthcare provider about longer-term strategies to keep the yeast in check. Remember, yeast infections are very common and nothing to be embarrassed about – and with the right approach, they’re very manageable and curable.






