Filters
- Adult Nasal Cannula (7)
- Amsino Nasal Cannula (1)
- AS75080 (1)
- cannula (7)
- Cannulas (4)
- Green Nasal Cannula (1)
- nasal cannula (6)
- oxygen cannula (6)
- Soft (1)
- Soft Nasal Cannula (4)
- soft tubing (1)
- Continuous Flow (1)
- Curved Prong (2)
- Hudson RC (1)
- Hudson RCI (3)
- O2 Cannula (1)
- Oxygen Cannula (3)
- Adult Cannula (1)
- Breathe (1)
- Cannula Needles (1)
- Chronic Obstructive Pulmonary Disease (1)
- COPD (1)
- emphysema (1)
- Nasal cannula (1)
- Oxygen cannula (1)
- Oxygen delivery (1)
- Respiratory (2)
- Respiratory Therapy (2)
- Tubing (2)
- 1600HF Nasal Cannula (1)
- Star Lumen Tubing (1)
- Delivery Oxygen (1)
- Oxygen Supply (2)
- Oxygen Tube (1)
- 1820 (1)
- Softtech (1)
- Nasal Tube (1)
- Over the Ear (1)
- extension tubing (1)
- Green Tubing (1)
- o2 tubing (2)
- oxygen supply (1)
- Connector (3)
- Tubing connector (1)
- ear cushions (2)
- ear pads (2)
- ez wraps (1)
- Nasal Cannula with Pads (1)
- Dyanrex (1)
- Oxygen Therapy (1)
- extenstion tubing (1)
- Long Oxygen Tubing (1)
- oxygen tube (1)
- star tubing (1)
- CO2 Oxygen (1)
- CO₂ (1)
- etco2 (1)
- Luer Lock (1)
- Oxygen Lines (1)
- Sampling tubing (1)
- Simultaneous oxygen delivery (1)
- Aliied Healthcare (1)
- Kids cannula (1)
- Pediatric nasal cannula (1)
- 1016 (1)
- ear irritation (1)
- ear wraps (1)
- foam pams (1)
- Airlife (1)
- White (1)
- Nasal Mask (1)
- diagnostic cannula (1)
- Nasal pressure cannula (1)
- Sleep diagnostics (1)
- Aspirator (1)
- Aspirator tubing (1)
- Suction Machine (1)
- Tapered (1)
- Tubing Connector (1)
- Universal connector (1)
- 1610-7-50 (1)
- Baby Cannula (1)
- Baby nasal cannula (1)
- Infant nasal cannula (1)
- Infants (1)
Nasal Cannulas
Nasal cannulas are medical devices used to deliver supplemental oxygen to people who need help getting enough oxygen. A nasal cannula is a thin, flexible tube that rests on your face and connects to an oxygen source (like an oxygen tank or concentrator). It has a pair of soft prongs (short tips) that fit just inside your nostrils, through which the oxygen flows into your nose.
Here’s what a nasal cannula looks like and how it works:
- The tube typically loops over the ears and under the chin (or around the back of the head) to help it stay in place comfortably. The two prongs at the front sit in your nostrils, and the rest of the tube runs from your nose to the oxygen supply.
- Oxygen travels from the supply, through the tubing, and exits the prongs. You then inhale the oxygen-rich air through your nose (and mouth, if you also breathe through your mouth). This way, the nasal cannula provides extra oxygen while still allowing you to talk, eat, and drink normally – unlike an oxygen mask, which covers the nose and mouth.
- Nasal cannulas are used in many settings: hospitals, clinics, or at home. They’re common for people with respiratory conditions like COPD (chronic obstructive pulmonary disease), pulmonary fibrosis, COVID-19, or heart failure, who might need a little extra oxygen to maintain healthy blood oxygen levels. They’re also used during and after surgery, or anytime a patient needs supplemental oxygen but doesn’t require a more restrictive mask.
- One reason nasal cannulas are popular is they are less intrusive and more comfortable than oxygen masks for long-term use. They cause minimal inconvenience – you can still breathe through your mouth, and you’re not “enclosed” by a mask. This makes them ideal for low to moderate oxygen needs.
Oxygen Flow and Use: A standard nasal cannula typically delivers oxygen at low flow rates, generally between 1 to 6 liters of oxygen per minute (L/min).
-
At 1–2 L/min, you get a small boost of oxygen (often used for people who need just a bit of help, such as some COPD patients at rest).
-
At higher flows like 4–6 L/min, more oxygen is provided. However, standard nasal cannulas usually aren’t used much above 5–6 L/min because at higher flows the oxygen can feel dry or irritating to the nasal passages and the percentage of oxygen delivered (FiO₂) plateaus (meaning you don’t get a much higher oxygen concentration due to room air mixing with it). Often, if someone needs more oxygen than a standard cannula can provide, a face mask or a specialized high-flow cannula is used.
-
Oxygen coming through a nasal cannula can be humidified (moistened) especially at flows above 2–3 L/min, to prevent dryness in the nose. In hospitals, you’ll often see a sterile water bubbler attached to the oxygen source for this purpose.
A nasal cannula is a simple and commonly used device for oxygen therapy, consisting of a lightweight tube with two prongs that sit at the nostrils. It’s used to deliver extra oxygen to people who need it, in a comfortable way that still allows them to talk, eat, and move around. It’s typically used for mild to moderate oxygen needs, at flow rates up to about 5–6 L/min, providing an effective means to improve oxygenation for patients with lung or heart conditions, or anyone temporarily needing a little help with their oxygen intake.
-
 Sale 15%
Original price $ 1.29Current price $ 1.10
Sale 15%
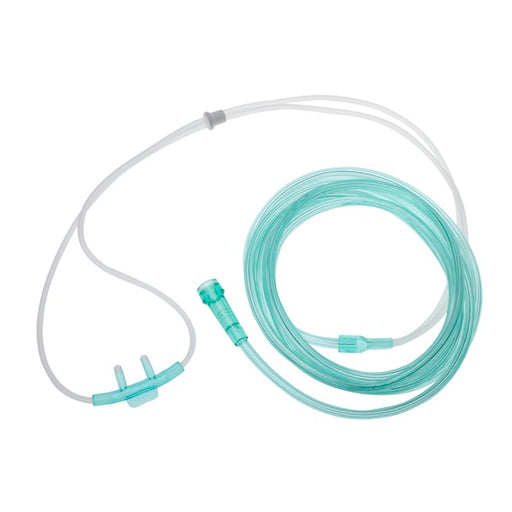
Original price $ 1.29Current price $ 1.10Oxygen Nasal Cannula (Light Green Color) with Super Soft 7 foot Tubing
Amsino55 reviewsAn Oxygen Nasal Cannula is a small tube-like device used to deliver supplemental oxygen to people who can benefit from increased oxygen levels. It ...
View full details -
 Sale 46%
Original price $ 2.35Current price $ 1.28
Sale 46%
Original price $ 2.35Current price $ 1.28Nasal Cannula with Curved Nasal Prongs with 7 Foot Tubing
Medline15 reviewsThe Hudson RCI 1104 Nasal Cannula with Curved Nasal Prongs with 7 Foot Tubing is a great consumable product meant for single-patient use is designe...
View full details -
 Sale 38%
Original price $ 1.05Current price $ 0.65
Sale 38%
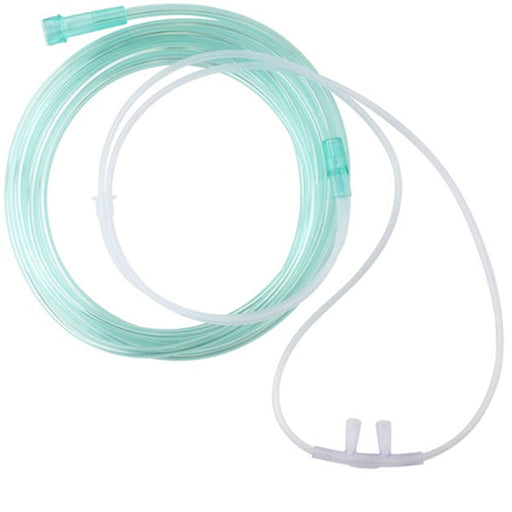
Original price $ 1.05Current price $ 0.65Oxygen Nasal Cannula Adult Size with 7 Foot Tubing
Dynarex10 reviewsA Nasal Cannula is a medical device used to deliver supplemental oxygen to patients. It features two prongs that fit into the nostrils, connected t...
View full details -
 Sale 41%
Original price $ 11.79Current price $ 6.95
Sale 41%
Original price $ 11.79Current price $ 6.95Nasal Cannula High Flow Non-Flared Tip, 7 foot Tubing, Adult by Salter Labs
Sun Med3 reviewsHigh Flow Nasal Cannula is an oxygen delivery device used to provide higher concentrations of oxygen compared to regular nasal cannulas. It supplie...
View full details -
 Sale
$ 1.19
Sale
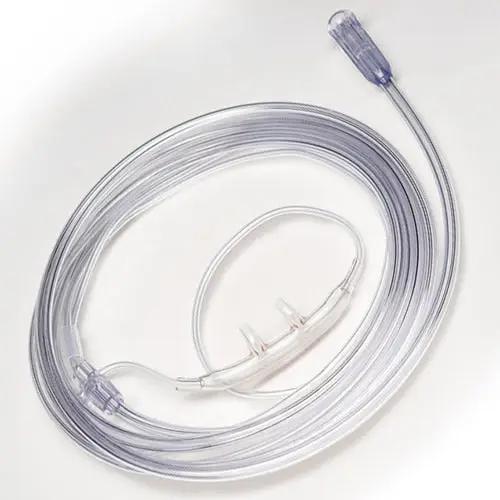
$ 1.19Salter Labs Adult Nasal Cannula with Curved Prongs & 7 foot tubing
Salter Labs28 reviewsSalter-Style 1600-7 Clear Adult Nasal Cannula is a clear, lightweight adult sized nasal cannula designed for comfort and a perfect fit. Complete wi...
View full details -
 Sale 43%
Original price $ 3.95Current price $ 2.25
Sale 43%
Original price $ 3.95Current price $ 2.25Soft-Touch Nasal Cannula with 7 Foot Star Lumen Tubing
Medline Hudson RCI27 reviewsSoft-Touch Nasal Cannula is designed for superior fit and comfort. Made with extra soft tubing, this cannula features an over-the-ear design, a sta...
View full details -
 Sale 34%
Original price $ 2.10Current price $ 1.39
Sale 34%
Original price $ 2.10Current price $ 1.39Over the Ear Nasal Cannula with 7 Foot Tubing
Teleflex13 reviewsOver-the-Ear 1103 Nasal Cannulas by Hudson RCI is a soft, comfortable cannulas made for the delivery of oxygen. Complete with Hudson's over-the-ear...
View full details -
 Sale 29%
Original price $ 0.79Current price $ 0.56
Sale 29%
Original price $ 0.79Current price $ 0.56Oxygen Supply Extension Tubing 7 Foot
Dynarex15 reviewsOxygen tubing is a clear supply tubing used to deliver therapeutic oxygen to a patients airways. Made with a 5-channel star interior to prevent oxy...
View full details -
 Sale 55%
Original price $ 0.87Current price $ 0.39
Sale 55%
Original price $ 0.87Current price $ 0.39Treaded Oxygen Tubing Connector
Teleflex10 reviewsTreaded Oxygen Tubing Connector is double-male end connector used with nasal cannulas, oxygen masks and other respiratory devices. Unique design, a...
View full details -
 Sale 33%
Original price $ 2.89Current price $ 1.95
Sale 33%
Original price $ 2.89Current price $ 1.95Salter Labs 1600TLC Nasal Cannula with Ear Cushion Pads Sun Med
Salter Labs13 reviewsThe Salter Labs 1600TLC-7 Nasal Cannula with Ear Cushion Pads are ideal for use with patients requiring supplemental oxygen for increased levels of...
View full details -
 Sale 41%
Original price $ 1.05Current price $ 0.62
Sale 41%
Original price $ 1.05Current price $ 0.62Nasal Cannula with 7 foot Oxygen Tubing, Dynarex
Dynarex5 reviewsA Nasal Cannula with 7-foot Oxygen Tubing is used to deliver supplemental oxygen to patients with respiratory conditions. It features prongs that f...
View full details -
 Sale 37%
Original price $ 2.95Current price $ 1.85
Sale 37%
Original price $ 2.95Current price $ 1.85Oxygen Tubing 25 Foot Length
Dynarex20 reviewsOxygen Extension Tubing 25 Foot Length is a star-lumen tubing used with oxygen concentrators, oxygen masks and nasal cannulas to add extra length. ...
View full details -
 Sale 38%
Original price $ 6.95Current price $ 4.29
Sale 38%
Original price $ 6.95Current price $ 4.29Nasal Cannula ETCO2 Sampling Simultaneous O2 CO2 & O2 Lines, 3 Channel Safety Tubing 10' Length
McKesson3 reviewsThe ETCO₂ Nasal Sampling Cannula with O₂ Delivery is designed for precise, continuous respiratory monitoring and effective oxygen therapy in adult ...
View full details -
 Sale
$ 1.99
Sale
$ 1.99Nasal Cannula Low Flow Delivery McKesson Pediatric Curved Prong / NonFlared Tip
McKesson1 reviewMcKesson # 1018188 Manufacturer # 16-331E Brand McKesson Manufacturer McKesson Brand Application Nasal Cannula Color Clear Connectio...
View full details -
 Sale 34%
Original price $ 1.95Current price $ 1.29
Sale 34%
Original price $ 1.95Current price $ 1.29Cannula Ear Protector E-Z Wrap
Salter Labs13 reviewsNasal Cannula Tubing Soft Ear Cushions are a soft, ready-to-use, foam ear wrap used to protect the ear from chafing and irritation of the skin arou...
View full details -
 Sale 30%
Original price $ 19.95Current price $ 14.00
Sale 30%
Original price $ 19.95Current price $ 14.00Oxygen Tubing / Hose Connectors, White 50/Box
Cardinal HealthNo reviewsAirLife Oxygen Tubing Connectors are designed to connects nasal cannula tubing and oxygen masks to extension tubing. Each O2 connector is disposabl...
View full details -
 Sale 23%
Original price $ 3.29Current price $ 2.54
Sale 23%
Original price $ 3.29Current price $ 2.54Westmed BiFlo Nasal Mask with 7' Tubing
WestMed1 reviewWestmed BiFlo Nasal Mask with 7' Tubing eliminiates irritation from rubbing and everyday wear of cannulas. Product Specifications: FiO2 Volumes co...
View full details -
 Sale 14%
Original price $ 124.97Current price $ 107.10
Sale 14%
Original price $ 124.97Current price $ 107.10ThermiSense Sleep Diagnostic Cannula
McKessonNo reviewsThe ThermiSense Sleep Diagnistic Cannula accurately senses the oral/nasal thermal airflow changes as well as the nasal pressure signal when used wi...
View full details -
 Sale 41%
Original price $ 0.59Current price $ 0.35
Sale 41%
Original price $ 0.59Current price $ 0.35Universal Tubing Connector 5-in-1
Cardinal Health2 reviews5-in-1 Universal Medical Tubing Connector is designed for use for oxygen therapy tubing, aspirator suction machine tubing and other medical devices...
View full details -
 Sale 30%
Original price $ 5.59Current price $ 3.89
Sale 30%
Original price $ 5.59Current price $ 3.89Pediatric Nasal Cannula for Babies / Infants with 7 foot tubing
Sun MedNo reviewsSalter Labs 1610 Premature Baby Nasal Cannula is a soft, lightweight over-the-ear style oxygen nasal cannula for oxygen flows up to 3 LPM. This chi...
View full details
People Also Searched For
Nasal cannulas are medical devices used to deliver supplemental oxygen to people who need help getting enough oxygen. A nasal cannula is a thin, flexible tube that rests on your face and connects to an oxygen source (like an oxygen tank or concentrator). It has a pair of soft prongs (short tips) that fit just inside your nostrils, through which the oxygen flows into your nose.
Here’s what a nasal cannula looks like and how it works:
- The tube typically loops over the ears and under the chin (or around the back of the head) to help it stay in place comfortably. The two prongs at the front sit in your nostrils, and the rest of the tube runs from your nose to the oxygen supply.
- Oxygen travels from the supply, through the tubing, and exits the prongs. You then inhale the oxygen-rich air through your nose (and mouth, if you also breathe through your mouth). This way, the nasal cannula provides extra oxygen while still allowing you to talk, eat, and drink normally – unlike an oxygen mask, which covers the nose and mouth.
- Nasal cannulas are used in many settings: hospitals, clinics, or at home. They’re common for people with respiratory conditions like COPD (chronic obstructive pulmonary disease), pulmonary fibrosis, COVID-19, or heart failure, who might need a little extra oxygen to maintain healthy blood oxygen levels. They’re also used during and after surgery, or anytime a patient needs supplemental oxygen but doesn’t require a more restrictive mask.
- One reason nasal cannulas are popular is they are less intrusive and more comfortable than oxygen masks for long-term use. They cause minimal inconvenience – you can still breathe through your mouth, and you’re not “enclosed” by a mask. This makes them ideal for low to moderate oxygen needs.
Oxygen Flow and Use: A standard nasal cannula typically delivers oxygen at low flow rates, generally between 1 to 6 liters of oxygen per minute (L/min).
-
At 1–2 L/min, you get a small boost of oxygen (often used for people who need just a bit of help, such as some COPD patients at rest).
-
At higher flows like 4–6 L/min, more oxygen is provided. However, standard nasal cannulas usually aren’t used much above 5–6 L/min because at higher flows the oxygen can feel dry or irritating to the nasal passages and the percentage of oxygen delivered (FiO₂) plateaus (meaning you don’t get a much higher oxygen concentration due to room air mixing with it). Often, if someone needs more oxygen than a standard cannula can provide, a face mask or a specialized high-flow cannula is used.
-
Oxygen coming through a nasal cannula can be humidified (moistened) especially at flows above 2–3 L/min, to prevent dryness in the nose. In hospitals, you’ll often see a sterile water bubbler attached to the oxygen source for this purpose.
A nasal cannula is a simple and commonly used device for oxygen therapy, consisting of a lightweight tube with two prongs that sit at the nostrils. It’s used to deliver extra oxygen to people who need it, in a comfortable way that still allows them to talk, eat, and move around. It’s typically used for mild to moderate oxygen needs, at flow rates up to about 5–6 L/min, providing an effective means to improve oxygenation for patients with lung or heart conditions, or anyone temporarily needing a little help with their oxygen intake.
What Nasal Cannulas are Used For:
Nasal cannulas are used whenever someone needs a bit of extra oxygen support but doesn’t require a full face mask or more invasive breathing assistance. In practice, this device is commonly used for people who have low blood oxygen levels due to various medical conditions or situations. Here are the primary uses of a nasal cannula:
-
Managing Chronic Respiratory Diseases: One of the most common uses is to provide long-term oxygen therapy for people with chronic lung conditions. For example:
- COPD (Chronic Obstructive Pulmonary Disease): Many patients with COPD, including those with emphysema or chronic bronchitis, use a nasal cannula at home to maintain their oxygen saturations. They might wear it for a set number of hours per day or continuously, depending on the severity of their lung disease. The cannula supplies supplemental oxygen that alleviates shortness of breath, helps them be more active, and protects organs from the effects of chronic low oxygen. For instance, a doctor might prescribe 2 liters per minute of oxygen via nasal cannula for a COPD patient to use during sleep or exercise, or around the clock in advanced cases.
- Pulmonary Fibrosis and Other Interstitial Lung Diseases: These conditions cause scarring of the lungs and reduce oxygen exchange. A nasal cannula is often used to deliver oxygen continuously to such patients, improving their energy levels and organ function. They may need oxygen anytime they exert themselves, or even at rest in later stages of disease.
- Severe Asthma or Cystic Fibrosis: While acute asthma attacks are treated with other measures (like inhalers and sometimes masks for high-flow oxygen), some people with severe, chronic asthma or cystic fibrosis may use nasal cannulas between flare-ups to help with baseline oxygenation.
- Sleep-Related Breathing Disorders: Some individuals with conditions like Chronic Obstructive Sleep Apnea plus COPD (the overlap syndrome) or other hypoventilation syndromes use supplemental oxygen at night via nasal cannula in addition to or instead of CPAP. This ensures their blood oxygen stays stable while sleeping. (However, primary obstructive sleep apnea is usually treated with air pressure devices rather than oxygen.)
-
Acute Medical Situations and Hospital Care: Nasal cannulas are standard in hospitals for patients who need a little oxygen support. For example:
- Pneumonia or COVID-19: If a patient’s oxygen saturation drops due to an infection like pneumonia or COVID-19, the first step is often to apply a nasal cannula with a low to moderate flow of oxygen (say 2-5 liters per minute). This can often raise their oxygen levels enough to relieve symptoms like shortness of breath and prevent more invasive intervention. During surges of COVID-19, many patients on wards were comfortably managed with nasal cannulas unless their condition worsened.
- Post-Surgery Recovery: After anesthesia or surgery, patients sometimes have mildly depressed breathing or low oxygen saturations. A nasal cannula is frequently used in the recovery room and post-op to give a little extra O₂ until the patient is fully awake and their breathing is back to normal. For instance, after abdominal surgery, a person might be on 3 L/min via cannula overnight to ensure their organs get enough oxygen while they’re on pain medication and moving less.
- Heart Failure or Heart Attacks: In acute or chronic heart failure, the heart isn’t pumping efficiently, so tissues may not get adequate oxygen. A nasal cannula can help increase oxygen delivery in these scenarios. In the ER, a patient with chest pain or a suspected heart attack is often given oxygen by nasal cannula (especially if their oxygen saturation is below normal) as a supportive measure.
- Stroke or Shock: In emergency settings, patients with suspected stroke or those in shock (very low blood pressure) may be given supplemental oxygen via cannula to maximize oxygen delivery to vital organs, unless there’s a reason to avoid it. It’s part of the standard “ABCs” (airway, breathing, circulation) to check oxygen and provide support if needed.
- During Procedures with Sedation: If you’re undergoing a procedure with moderate sedation (like an endoscopy, colonoscopy, or minor surgery under IV sedation), clinicians often put a nasal cannula on you. The sedatives can slow breathing, so a little extra oxygen ensures you stay well-oxygenated throughout. Similarly, in dental procedures or plastic surgeries under twilight sedation, nasal cannulas are used because they don’t obstruct access to the mouth/face.
-
Emergency and First Aid Situations: First responders (EMTs, paramedics) commonly use nasal cannulas for patients who are breathing okay on their own but show signs of mild oxygen deprivation.
- For example, an asthma patient who is speaking in full sentences but has an oxygen saturation of 90% might get 4 L/min via cannula while being transported, whereas a more severe case would get a face mask.
- Someone with carbon monoxide poisoning at a scene might initially get high-flow oxygen; if they are stable later, they might wean down to a cannula.
- In wilderness first aid or scenarios at high altitude, a portable oxygen setup with a nasal cannula can be lifesaving for altitude sickness or severe hypoxia until further care is available.
-
Home Oxygen for Other Chronic Conditions: Beyond lung-specific diseases, a nasal cannula might be prescribed in scenarios like:
- Advanced Cancers or Anemia: If someone has a condition causing low oxygen levels (for instance, certain cancers affecting lung function, or very severe anemia where blood can’t carry enough oxygen), doctors might use supplemental oxygen to help alleviate breathlessness.
- Chronic Heart and Lung Combo Issues: Patients with pulmonary hypertension or cor pulmonale (heart issues caused by lung disease) often benefit from continuous oxygen via cannula to reduce strain on the heart.
- Neonatal Care: Infants who are born prematurely or with lung problems (like bronchopulmonary dysplasia) are often given oxygen through tiny nasal cannulas in the neonatal ICU or at home. It helps them grow and thrive until their lungs mature more.
-
High Altitude or Aviation: In unpressurized aircraft or high-altitude climbing, nasal cannulas can be used to deliver oxygen from portable tanks to prevent altitude sickness or hypoxia. For instance, pilots of small aircraft flying above 10,000 feet might use a nasal cannula O₂ system. Mountaineers sometimes carry oxygen (with a mask or cannula) for extreme altitudes above ~26,000 feet (“death zone”) to supplement what little oxygen is in the ambient air. In these contexts, the nasal cannula provides needed oxygen while still allowing for communication and relatively comfortable breathing.
-
COVID-19 Pandemic Note: Nasal cannulas were heavily used during the pandemic for patients with COVID pneumonia. Hospitals would start patients on a nasal cannula at 4-6 L/min and, if that wasn’t sufficient, move to higher flow devices or ventilation. Patients who needed long-term oxygen after recovering from COVID also often went home with nasal cannulas. Some nasal cannulas during COVID were used with humidifiers and flows up to 6 L/min at home. There was also widespread use of high-flow nasal cannula (HFNC) devices in hospitals – which is a specialized use where warmed, humidified oxygen at very high flow rates (e.g., 30-60 L/min) is delivered via larger nasal prongs. This is still a “nasal cannula” in principle, but a more advanced application helping patients avoid intubation in some cases of respiratory failure.
In summary, nasal cannulas are used any time a patient needs supplemental oxygen but does not require intensive breathing support. They are the go-to device for:
- Chronic oxygen therapy in lung and heart disease (improving quality of life and exercise tolerance).
- Acute medical care to treat or prevent hypoxemia (low blood oxygen) in conditions like pneumonia, heart attacks, strokes, etc.
- Emergency response when a person is breathing on their own but oxygen is low.
- Situational needs like high altitude adaptation or procedural sedation.
They’re popular because they’re effective, simple, and patient-friendly – providing the necessary oxygen while still allowing patients to eat, talk, and engage in daily activities with minimal restriction.
Types of nasal cannulas generally refer to the different designs and specialized versions of cannulas used to deliver oxygen. While all nasal cannulas share the basic concept of two prongs in the nostrils and tubing to an oxygen source, there are variations tailored for specific needs. Here are the main types of nasal cannulas:
-
Standard Nasal Cannula: This is the most common type used in hospitals and home oxygen therapy. It’s the familiar design with two small prongs that sit just inside the nostrils and tubing that loops over the ears. Standard cannulas are used for low to moderate oxygen flow rates (typically up to about 5–6 liters per minute). They are made of soft plastic and come in different lengths of tubing (like 4-foot, 7-foot, 25-foot) depending on patient mobility needs. The standard cannula is appropriate for most adults and older children who need supplemental oxygen for conditions like COPD, pulmonary fibrosis, mild pneumonia, etc. It provides an effective means to increase oxygen levels while being relatively comfortable and allowing the patient to talk and eat.
-
Soft-Tip or Comfort Nasal Cannula: This is a variant of the standard cannula designed for improved comfort, especially during long-term use. The prongs and the portion that rests on the upper lip are made of extra-soft, flexible silicone or softer plastic. They often have slightly curved or flared prongs that fit more comfortably in the nostrils. Patients on 24/7 oxygen or who have sensitive skin benefit from these, as they reduce irritation to the nares and ears. Brands like Salter Labs have “soft” cannulas advertised for their gentle feel. In terms of functionality (oxygen delivery), they’re the same as a standard cannula; the difference is mainly patient comfort and reduced friction/pressure sores. Often, patients who find the regular cannula prongs too stiff will switch to a soft-tip cannula for continuous home use.
-
High-Flow Nasal Cannula (HFNC): High-flow nasal cannulas are specialized systems used in hospitals for delivering very high flow rates of oxygen and air (anywhere from 15 up to 60 liters per minute, or more) with added humidification and heating. Physically, the high-flow cannula has larger prongs and is attached to a heated humidifier machine and blender that can deliver precise oxygen concentrations (even up to 100% oxygen) at high flows. This type is often used for patients with severe respiratory distress or acute respiratory failure – for example, patients with COVID-19 pneumonia or acute heart failure may be placed on HFNC as an alternative to intubation. Despite the high flow, because the oxygen is humidified and warmed, it’s more comfortable than blasting cold dry oxygen. The larger-bore tubing and prongs distinguish HFNC from standard cannulas. It’s important to note that HFNC is a whole system (machine + cannula), not just a tubing—so you wouldn’t usually see HFNC used at home; it’s more for critical care or step-down units. There are some intermediate cannulas called “high concentration” cannulas that can handle flows of, say, 6–15 L/min (with external humidifiers) that might be used in ambulances or for short-term boosts, but true HFNC setups are hospital-based.
-
Pediatric and Infant Nasal Cannulas: These are smaller cannulas designed for babies and children. They come in neonatal, infant, pediatric sizes (the prongs and face interface are scaled down). Using an adult cannula on a baby would be impractical and could ulcerate the nostrils, so pediatric cannulas ensure a proper fit. They also deliver appropriate flow rates for little ones (often much lower flows, measured in fractions of a liter for newborns). The tubing is often lighter and designed to minimize pulling on tiny ears and cheeks. In neonatal intensive care units, very small premature babies on low-flow oxygen will wear these delicate cannulas, sometimes secured with a bit of tape. For older children who still need oxygen (like a toddler with bronchopulmonary dysplasia on home oxygen), pediatric cannulas also have soft prongs and a flexible design to allow the child to move around and play. The concept is the same as adult cannulas, just miniaturized and optimized for sensitive skin and small facial features.
-
Reservoir Nasal Cannulas (Oxymizer Cannulas): These are special cannulas that include an oxygen reservoir to increase the efficiency of oxygen delivery. They come in two main designs: a “mustache” Oxymizer (with a small reservoir pouch that sits below the nose and looks a bit like a mustache) or a “pendant” Oxymizer (a reservoir that hangs like a pendant on the chest). These reservoirs store oxygen in between breaths. When the patient inhales, they get a bolus of concentrated oxygen from the reservoir in addition to the continuous flow. This allows a higher effective FiO₂ (oxygen concentration) to reach the lungs without increasing the liter flow. Essentially, a reservoir cannula can deliver the same oxygen benefit at, say, 2 L/min that a standard cannula might at 4 L/min, because it saves oxygen that would otherwise be wasted when exhaling. They are useful for patients who need higher oxygen levels but want to remain on nasal cannula rather than switching to a face mask, or to conserve oxygen from tanks (each breath uses the stored O₂ more efficiently). Some patients with pulmonary fibrosis or severe COPD who need high oxygen might use these so they can ambulate longer on a portable tank.
-
Curved-Prong Cannulas vs. Straight-Prong Cannulas: This is a minor distinction, but cannulas come with slightly different prong shapes. Curved prong cannulas are anatomically curved to fit the curvature of the nostrils (prongs curve back towards the face). Many people find these more comfortable and they may direct flow a bit better into the nasal passages. Straight prong cannulas have prongs that go straight into the nose; they’re often the basic design. Some brands label their cannulas as “curved, non-flared” or “straight, flared” etc. Flared prongs have a wider opening at the tip to possibly make oxygen dispersion gentler. These design tweaks let clinicians choose a cannula that the patient finds most comfortable and effective. So while not “types” in terms of usage, they’re variants one might encounter.
-
High-Concentration Nasal Cannulas: In some contexts, you may hear of a “high-concentration nasal cannula” which typically refers to a standard cannula used at the upper end of its effective flow range, often with humidification and maybe larger bore tubing. For example, some emergency kits have a larger tubing cannula that can handle 15 L/min (though at that point, a mask is usually more appropriate). This is not a distinct device like HFNC, but rather a beefed-up version of the standard cannula for short-term use when a mask isn’t tolerated.
-
Nasal Prongs for Nasopharyngeal Oxygen: Rarely, there are systems where oxygen is delivered via a thin catheter placed deeper into the nasal passage (near the nasopharynx) – sometimes called “nasopharyngeal catheter” or “nasal prong” in older literature. Before modern cannulas were prevalent, a single thin tube could be inserted deeper into one nostril for oxygen. That provided a bit more direct oxygen delivery than just at the nostril. Nowadays, this method is seldom used because standard and high-flow cannulas cover needs well, but it’s a historical type. It might be considered if a patient can’t tolerate prongs in the nostrils but could handle a soft catheter in one nasal passage.
-
Specialty Cannulas (e.g., for Sleep or Exercise): There are also some proprietary cannulas designed for specific situations. For instance, a “quiet” cannula that reduces the noise of oxygen flow (some patients find the hissing sound annoying at night). Or a split cannula where one side can deliver a slightly different flow than the other (though that’s unusual). By and large, however, the main types are as listed above: standard, soft, high-flow, pediatric, reservoir.
It’s worth noting that while an oxygen mask is not a “nasal cannula,” it is another category of oxygen delivery device. Masks (simple face mask, Venturi mask, non-rebreather mask, etc.) are used when higher oxygen concentrations are needed or if the patient is a mouth-breather who wouldn’t get the full benefit from a cannula. The question, however, is specifically about types of nasal cannulas, so we focus on cannula variations.
In summary, the types of nasal cannulas include:
- Standard cannulas for routine low/mid-range oxygen needs.
- Soft or comfort cannulas for long-term use to minimize irritation.
- High-flow nasal cannula systems for critical care, delivering heated, humidified oxygen at much higher flow rates.
- Pediatric/infant cannulas scaled for children and babies.
- Reservoir (Oxymizer) cannulas that improve oxygen delivery efficiency with built-in reservoirs.
- Other variants like curved vs. straight prongs and nasopharyngeal catheters, which are more about comfort/fit or older techniques.
Healthcare providers will choose the type based on the patient’s oxygen requirements, age/size, comfort considerations, and the clinical setting. Each type is aimed at ensuring the patient gets adequate oxygen in the most comfortable and effective way possible.
Nasal cannula flow rates refer to how many liters of oxygen per minute (L/min) are delivered through a nasal cannula, and each flow rate corresponds to an approximate oxygen concentration that the patient breathes in (the FiO₂, or fraction of inspired oxygen). Here are the typical flow rates for a standard adult nasal cannula and the oxygen percentages they provide:
-
1 L/min: Delivers about 24% oxygen. (Room air is ~21% oxygen, so 1 liter of supplemental O₂ raises the FiO₂ to roughly 24%.)
-
2 L/min: ~28% oxygen. (A general rule of thumb is that each additional liter per minute increases FiO₂ by about 3-4% in a nasal cannula.)
-
3 L/min: ~32% oxygen
-
4 L/min: ~36% oxygen
-
5 L/min: ~40% oxygen
-
6 L/min: ~44% oxygen
These values are approximate. The actual FiO₂ a person receives can vary based on their breathing pattern (how deeply and fast they breathe, which causes mixing of delivered oxygen with room air). But generally:
-
A nasal cannula can provide around 24% to 44% oxygen at flow rates of 1 to 6 L/min. This is sufficient for many patients with mild to moderate oxygen needs.
-
Flow rates above 6 L/min are generally not recommended for a standard nasal cannula. At higher flows, the cannula becomes less effective (much of the oxygen might blow out and not be inhaled) and can be uncomfortable, causing nasal dryness and irritation. If a patient requires more oxygen than ~44% FiO₂ (or more flow than 6 L/min can provide), clinicians typically switch to a different oxygen delivery device:
- For example, a simple face mask can deliver about 40-60% oxygen at 5-10 L/min.
- A non-rebreather mask can deliver 60-90% oxygen at 10-15 L/min.
- Or a Venturi mask can deliver a precise FiO₂ (e.g., 50% at a set flow with an adapter).
- In critical care, a High-Flow Nasal Cannula (HFNC) system (which is different from a regular cannula) can deliver very high flows (up to 60 L/min or more) with close to 100% FiO₂ in a heated, humidified form, But HFNC is a special setup typically used in hospitals for severe respiratory distress.
Humidification: When oxygen is delivered at higher flow rates (generally above 3–4 L/min), it’s often humidified to prevent the nasal passages from drying out. In hospitals and home concentrators, you’ll often see a humidifier bottle attached when flows of 4 L/min or greater are used continuously.
Pediatric Note: For infants and young children, flow rates are much lower. A premature baby might be on 0.1 to 0.5 L/min, an infant on 0.5 to 2 L/min, etc., depending on the need, with appropriately smaller cannulas. The FiO₂ increases similarly in percentage terms, but careful monitoring is required to avoid giving too much oxygen to babies (due to risks like eye damage in preemies).
Relationship between Flow and FiO₂: A common teaching is: For every 1 L/min increase in flow, FiO₂ goes up by ~4%. Starting from 21% at room air:
- 1 L ≈ 24%
- 2 L ≈ 28%
- 3 L ≈ 32%
- 4 L ≈ 36%
- 5 L ≈ 40%
- 6 L ≈ 44%
This rule holds reasonably well in practice for flows 1-6 L/min as long as the patient’s breathing isn’t extremely heavy. If a patient is breathing very rapidly and deeply, the effective FiO₂ might be a bit lower (because they’re pulling in more room air per breath along with the oxygen).
Titration and Use: In clinical practice, doctors and nurses will adjust the nasal cannula flow to achieve target oxygen saturations (SpO₂) in the patient’s blood. For example, they might start at 2 L/min and then check the oximeter; if SpO₂ is still below the goal, they’ll go to 3 L, then 4 L, etc. Many patients at home are given a specific flow rate to use at rest and one for exertion. For instance, “2 L/min at rest, 4 L/min during exercise” if they desaturate with activity.
High-Flow Systems vs. Standard Cannula:
- Standard cannula: 1-6 L/min (some sources allow up to 8 L/min with special high-flow cannula tubing, but beyond 6 L the efficiency drops a lot). Max FiO₂ ~ 40-45%.
- High-Flow Nasal Cannula (HFNC): 10-60+ L/min, with heated humidity. FiO₂ can be 21% to 100%. This is a different apparatus used in ICU/ER for severe cases and is not the typical nasal cannula used at home or on regular hospital floors.
In summary, nasal cannulas deliver oxygen at flow rates typically between 1 and 6 liters per minute, translating to approximately 24% to 44% oxygen being breathed in. Each liter per minute increase raises the delivered oxygen concentration by about 3-4%. If a patient needs more oxygen than what 5-6 L/min via cannula provides, healthcare providers will switch to other oxygen delivery methods (like masks or high-flow devices) to meet the oxygen demand.
Nasal cannulas come in a few different sizes and configurations to fit various patient age groups and needs. Unlike something like IV cannulas which are measured by gauge, nasal cannula “sizes” are generally categorized by patient type (infant, pediatric, adult) and by the length/diameter of the tubing appropriate for different oxygen flow rates. Here are the main types of nasal cannula sizes:
-
Infant (Neonatal) Nasal Cannula: These are the smallest cannulas, designed for newborns and premature babies. They have very tiny, delicate prongs that fit into a baby’s little nostrils without causing trauma. The spacing between the prongs is narrower to match an infant’s nose. The tubing is also narrower and ultra-soft. Infant cannulas deliver low flow rates of oxygen (often measured in fractions of a liter per minute, like 0.1 to 1 L/min) because babies have small tidal volumes. They often come with special securement mechanisms (like gentle head straps or adhesive tabs on the cheeks) to keep them in place on squirmy infants. In hospitals, you might hear terms like “neonatal cannula” or “premature cannula” for the smallest sizes. These ensure that premature infants or newborns needing oxygen (e.g., in neonatal intensive care units or for conditions like bronchiolitis) get the support they need comfortably.
-
Pediatric Nasal Cannula: This is a medium size cannula made for children, typically from toddlers up to pre-teens (though exact breakpoints vary by manufacturer). Pediatric cannulas have prongs that are larger than the infant size but still smaller than adult ones. The distance between prongs and the size of the curved nasal piece are scaled for a child’s face. They are used for kids who need supplemental oxygen for conditions such as pediatric pneumonia, asthma flare-ups, congenital heart or lung issues, etc. The flow rates for pediatric cannulas are usually in the range of 0.5 to 4 L/min, depending on the child’s size and doctor’s prescription. Using an adult cannula on a small child can be uncomfortable or ineffective (the prongs might be too wide and not sit properly), so the pediatric size ensures proper fit and oxygen delivery.
-
Adult Nasal Cannula: The adult size is the standard nasal cannula for adolescents and adults. It has the largest prongs and prong spacing to accommodate adult nostrils and faces. Adult cannulas are typically used for flow rates from 1 to 6 L/min (though some are labeled to handle up to 8 L/min, generally above 6 L the effectiveness plateaus without humidity). Most adult cannulas are designed one-size-fits-most, but some manufacturers offer slight variations such as “Small Adult” or “Large Adult” cannulas; these adjust the prong size/spacing and tubing length a bit for smaller-framed or larger-framed individuals. However, in practice, the standard adult cannula works for the vast majority of adult patients. This is the cannula you’d get in the hospital if you, say, needed oxygen for pneumonia or after surgery, and it’s what home oxygen users wear for COPD or other chronic conditions.
-
High-Flow Nasal Cannula (Specialized Adult Cannula): While not a different “size” in the traditional sense of patient body size, it’s worth noting that high-flow oxygen delivery systems use a special type of larger cannula. These cannulas have wider bore prongs and tubing to accommodate much higher flow rates (up to 40-60+ L/min) and usually connect to a heated humidifier. They’re used in critical care environments for adults and children in respiratory distress. For example, a high-flow cannula for an adult will have thicker, short prongs that sit in the nostrils (often allowing some leak around them for comfort) and a more secure head strap to keep it in place. So, if you hear “high-flow nasal cannula,” it implies a device that is dimensioned to deliver high volumes of oxygen and is part of a special system – effectively a larger “size” cannula meant for that purpose. They come in sizes too (pediatric high-flow cannulas vs adult high-flow cannulas), but those are specific to the high-flow equipment and are not interchangeable with standard cannulas.
-
Cannula Tubing Lengths: Besides fitting the nose, cannulas differ in tubing length, which isn’t exactly a “size” of the cannula itself but is an important specification:
- Common lengths are 4 feet (1.2 m), 7 feet (2.1 m), 14 feet (4.3 m), 25 feet (7.6 m), and even 50 feet (15 m) for home oxygen users who want to move about their house. In hospitals, you usually see 7-foot cannulas which allow the patient to roll a bit in bed or sit up without yanking the oxygen source. At home, someone may use a 25 or 50-foot cannula connected to their concentrator so they can walk from room to room. The diameter of the tubing may slightly vary with length to ensure adequate oxygen flow to the patient (longer tubing can have more resistance, so some long hoses have a slightly larger internal diameter). But as far as “size,” when ordering cannulas, one would specify the patient size (infant, pediatric, adult) and the desired tubing length.
-
Specialty or Comfort Variations: Some manufacturers produce cannulas labeled as “small adult” or “large adult” for those on the edges of size ranges. For instance, a very petite adult might find a pediatric cannula more comfortable, or a “small adult” version if available. On the flip side, a “large adult” cannula may have slightly bigger prongs or a longer distance between prongs for folks with larger noses or facial features. Additionally, “micro” cannulas exist for cosmetic appeal when patients are out in public (these have extra-thin, less visible tubing and very small prongs, typically still delivering low flow oxygen). And soft cannulas (with softer, pliable silicone prongs) can come in the various sizes above to reduce irritation. These all essentially correspond to the same categorizations (infant, child, adult), just with different materials or slight adjustments.
To summarize by typical labeling:
- Neonate/Infant Cannula: Extremely small prongs, for newborns and babies up to ~1 year. Often used at very low flows (like 0.1 – 1 L/min).
- Pediatric Cannula: Small prongs, for children ~1 year up to early teens, depending on child’s size. Used at low-to-moderate flows (0.5 – 4 L/min).
- Adult Cannula: Standard prongs, fits older teens and adults. Used at flows around 1 – 6 L/min (some up to 8 L/min if humidified).
- (Sometimes subdivided into Small Adult or Large Adult by certain brands, but these are less common).
Each of these is designed to ensure the prongs sit comfortably in the nostrils without stretching or causing sores, and to deliver oxygen effectively for that patient’s typical breathing volumes. When getting oxygen supplies, it’s important to choose the right cannula size: for instance, a pediatric cannula on an adult might not deliver enough oxygen because the prongs are shorter and could easily dislodge, whereas an adult cannula on a toddler would be too big and inefficient. Medical providers or oxygen supply companies will select the appropriate size based on the patient’s age and size, thereby optimizing comfort and oxygen therapy effectiveness.
Oxygen therapy is a treatment that provides you with extra oxygen when you’re not getting enough through normal breathing. In simple terms, it means breathing in air that has a higher concentration of oxygen than the normal atmosphere. This “supplemental oxygen” can help raise the oxygen levels in your blood, which is vital for your organs and tissues to function properly.
People typically need oxygen therapy if their lungs aren’t absorbing enough oxygen on their own. This can happen due to various medical conditions or situations, such as:
- Chronic lung diseases: like COPD (chronic obstructive pulmonary disease), emphysema, or pulmonary fibrosis, where damaged lung tissue can’t extract sufficient oxygen from air.
- Asthma or Pneumonia: during severe flare-ups or infections when airways are narrowed or filled with fluid.
- Heart failure or heart conditions: where poor circulation leads to low oxygen delivery in the body.
- COVID-19 or other acute respiratory infections: that can cause low blood oxygen levels (hypoxemia).
- Sleep apnea or other sleep-related breathing disorders: in some cases, doctors prescribe nighttime oxygen.
- Premature infants with underdeveloped lungs: who may require oxygen support until their lungs mature (often in neonatal intensive care).
How Oxygen Therapy is Delivered: Oxygen is considered a medication, and it’s prescribed by a healthcare provider after determining that your blood oxygen is low (using tests like pulse oximetry or arterial blood gas). The oxygen can come from different sources – large tanks of compressed oxygen gas, liquid oxygen reservoirs, or electric oxygen concentrators that pull oxygen from the air. Once you have a source, the oxygen is most commonly delivered in one of the following ways:
- Nasal Cannula: A small, flexible tube with two prongs that sit in your nostrils. This is one of the most common methods for low to moderate oxygen needs. You’ll see people at home or in the hospital using nasal cannulas, which allow them to talk and eat while getting oxygen. The oxygen flow is measured in liters per minute (for example, 2 liters per minute via cannula is a typical starting dose).
- Oxygen Mask: A mask fits over your nose and mouth and is secured by an elastic strap. Masks are used when a higher concentration of oxygen is needed or if someone is a mouth-breather. There are simple face masks, Venturi masks (which can control the exact oxygen percentage), or non-rebreather masks (for high concentrations in emergencies).
- Oxygen “Tent” or Hood: Mostly used for infants or children, these enclosures can provide a controlled oxygen environment around the head.
- Hyperbaric Oxygen Therapy: A special form of oxygen therapy where you breathe 100% oxygen inside a pressurized chamber. This isn’t for routine low-oxygen situations, but rather for specific conditions like carbon monoxide poisoning, decompression sickness, or difficult wounds. It delivers oxygen at high pressure to super-saturate the blood with oxygen.
- Mechanical Ventilation (in critical care): If someone cannot breathe adequately on their own (for instance, during surgery under general anesthesia or in severe respiratory failure), oxygen is delivered through a ventilator with a tube down the windpipe. This is a form of oxygen therapy in life-support scenarios.
Goals and Benefits of Oxygen Therapy: By increasing the oxygen available to the lungs, oxygen therapy helps:
- Relieve symptoms of low oxygen such as shortness of breath, fatigue, dizziness, or confusion.
- Improve organ function: vital organs like the heart and brain require adequate oxygen. Supplemental oxygen can prevent damage that might occur from prolonged oxygen deprivation.
- Enhance quality of life: People on long-term oxygen often find they have more energy and can be more active. For example, someone with COPD might be able to walk farther or sleep better at night with their oxygen on, because their tissues are getting the oxygen they need.
- Support healing: In acute situations like pneumonia or trauma, giving oxygen buys time and supports the body’s healing process by ensuring tissues aren’t starved of O₂.
- Increase lifespan in chronic conditions: Studies have shown that for patients with chronic lung diseases and chronically low oxygen levels, using oxygen therapy for the prescribed hours each day can help them live longer. It reduces strain on the heart (low oxygen makes the heart pump harder).
Safety and Usage: Oxygen therapy is generally safe, but there are important safety considerations:
- Fire Hazard: Oxygen makes things burn more easily. You must never smoke or have open flames (like candles or gas stoves) in the vicinity of oxygen therapy. “No smoking – oxygen in use” signs are often placed where home oxygen is being used.
- Dryness and Irritation: Oxygen, especially from pressurized tanks or concentrators, can be dry. It may cause dryness in your nose or mouth, or irritation to your skin where the cannula or mask sits. Often, humidifiers are attached to oxygen systems to add moisture, and skin moisturizers (that are oxygen-safe) can help prevent sores where tubing rests on the ears or cheeks.
- Dosage as Prescribed: It’s important to use the flow rate prescribed by your doctor. Using too little might not improve your condition, and using too much can (in some cases) diminish your body’s natural drive to breathe or cause buildup of carbon dioxide. For most people, the doctor will specify a target oxygen saturation (like “keep SpO₂ above 90%”) and the corresponding oxygen flow rate to achieve that. Regular follow-ups ensure you’re on the right amount. Never adjust your oxygen flow rate upwards without medical advice, especially if you have COPD (some COPD patients are sensitive to high oxygen levels).
- Portable Use: Oxygen can be used at home continuously. Portable oxygen concentrators and small tanks allow people to go out, travel, and maintain mobility. For instance, there are lightweight battery-powered concentrators that people can sling over their shoulder, which provide oxygen via nasal cannula on the go. This means oxygen therapy doesn’t necessarily confine someone to a bed or chair; modern solutions aim to keep patients active.
In essence, oxygen therapy (also called supplemental oxygen) is a supportive therapy to ensure the body gets the oxygen it needs when illness or altitude or other factors prevent you from absorbing enough on your own. It’s a common and often life-improving (even life-saving) treatment in both acute medical care and chronic disease management. By breathing in extra oxygen via devices like cannulas or masks, patients can maintain safer oxygen levels, which helps relieve strain on the body and can make them feel much better.
What Nasal Cannulas are Used For:
Nasal cannulas are used whenever someone needs a bit of extra oxygen support but doesn’t require a full face mask or more invasive breathing assistance. In practice, this device is commonly used for people who have low blood oxygen levels due to various medical conditions or situations. Here are the primary uses of a nasal cannula:
-
Managing Chronic Respiratory Diseases: One of the most common uses is to provide long-term oxygen therapy for people with chronic lung conditions. For example:
- COPD (Chronic Obstructive Pulmonary Disease): Many patients with COPD, including those with emphysema or chronic bronchitis, use a nasal cannula at home to maintain their oxygen saturations. They might wear it for a set number of hours per day or continuously, depending on the severity of their lung disease. The cannula supplies supplemental oxygen that alleviates shortness of breath, helps them be more active, and protects organs from the effects of chronic low oxygen. For instance, a doctor might prescribe 2 liters per minute of oxygen via nasal cannula for a COPD patient to use during sleep or exercise, or around the clock in advanced cases.
- Pulmonary Fibrosis and Other Interstitial Lung Diseases: These conditions cause scarring of the lungs and reduce oxygen exchange. A nasal cannula is often used to deliver oxygen continuously to such patients, improving their energy levels and organ function. They may need oxygen anytime they exert themselves, or even at rest in later stages of disease.
- Severe Asthma or Cystic Fibrosis: While acute asthma attacks are treated with other measures (like inhalers and sometimes masks for high-flow oxygen), some people with severe, chronic asthma or cystic fibrosis may use nasal cannulas between flare-ups to help with baseline oxygenation.
- Sleep-Related Breathing Disorders: Some individuals with conditions like Chronic Obstructive Sleep Apnea plus COPD (the overlap syndrome) or other hypoventilation syndromes use supplemental oxygen at night via nasal cannula in addition to or instead of CPAP. This ensures their blood oxygen stays stable while sleeping. (However, primary obstructive sleep apnea is usually treated with air pressure devices rather than oxygen.)
-
Acute Medical Situations and Hospital Care: Nasal cannulas are standard in hospitals for patients who need a little oxygen support. For example:
- Pneumonia or COVID-19: If a patient’s oxygen saturation drops due to an infection like pneumonia or COVID-19, the first step is often to apply a nasal cannula with a low to moderate flow of oxygen (say 2-5 liters per minute). This can often raise their oxygen levels enough to relieve symptoms like shortness of breath and prevent more invasive intervention. During surges of COVID-19, many patients on wards were comfortably managed with nasal cannulas unless their condition worsened.
- Post-Surgery Recovery: After anesthesia or surgery, patients sometimes have mildly depressed breathing or low oxygen saturations. A nasal cannula is frequently used in the recovery room and post-op to give a little extra O₂ until the patient is fully awake and their breathing is back to normal. For instance, after abdominal surgery, a person might be on 3 L/min via cannula overnight to ensure their organs get enough oxygen while they’re on pain medication and moving less.
- Heart Failure or Heart Attacks: In acute or chronic heart failure, the heart isn’t pumping efficiently, so tissues may not get adequate oxygen. A nasal cannula can help increase oxygen delivery in these scenarios. In the ER, a patient with chest pain or a suspected heart attack is often given oxygen by nasal cannula (especially if their oxygen saturation is below normal) as a supportive measure.
- Stroke or Shock: In emergency settings, patients with suspected stroke or those in shock (very low blood pressure) may be given supplemental oxygen via cannula to maximize oxygen delivery to vital organs, unless there’s a reason to avoid it. It’s part of the standard “ABCs” (airway, breathing, circulation) to check oxygen and provide support if needed.
- During Procedures with Sedation: If you’re undergoing a procedure with moderate sedation (like an endoscopy, colonoscopy, or minor surgery under IV sedation), clinicians often put a nasal cannula on you. The sedatives can slow breathing, so a little extra oxygen ensures you stay well-oxygenated throughout. Similarly, in dental procedures or plastic surgeries under twilight sedation, nasal cannulas are used because they don’t obstruct access to the mouth/face.
-
Emergency and First Aid Situations: First responders (EMTs, paramedics) commonly use nasal cannulas for patients who are breathing okay on their own but show signs of mild oxygen deprivation.
- For example, an asthma patient who is speaking in full sentences but has an oxygen saturation of 90% might get 4 L/min via cannula while being transported, whereas a more severe case would get a face mask.
- Someone with carbon monoxide poisoning at a scene might initially get high-flow oxygen; if they are stable later, they might wean down to a cannula.
- In wilderness first aid or scenarios at high altitude, a portable oxygen setup with a nasal cannula can be lifesaving for altitude sickness or severe hypoxia until further care is available.
-
Home Oxygen for Other Chronic Conditions: Beyond lung-specific diseases, a nasal cannula might be prescribed in scenarios like:
- Advanced Cancers or Anemia: If someone has a condition causing low oxygen levels (for instance, certain cancers affecting lung function, or very severe anemia where blood can’t carry enough oxygen), doctors might use supplemental oxygen to help alleviate breathlessness.
- Chronic Heart and Lung Combo Issues: Patients with pulmonary hypertension or cor pulmonale (heart issues caused by lung disease) often benefit from continuous oxygen via cannula to reduce strain on the heart.
- Neonatal Care: Infants who are born prematurely or with lung problems (like bronchopulmonary dysplasia) are often given oxygen through tiny nasal cannulas in the neonatal ICU or at home. It helps them grow and thrive until their lungs mature more.
-
High Altitude or Aviation: In unpressurized aircraft or high-altitude climbing, nasal cannulas can be used to deliver oxygen from portable tanks to prevent altitude sickness or hypoxia. For instance, pilots of small aircraft flying above 10,000 feet might use a nasal cannula O₂ system. Mountaineers sometimes carry oxygen (with a mask or cannula) for extreme altitudes above ~26,000 feet (“death zone”) to supplement what little oxygen is in the ambient air. In these contexts, the nasal cannula provides needed oxygen while still allowing for communication and relatively comfortable breathing.
-
COVID-19 Pandemic Note: Nasal cannulas were heavily used during the pandemic for patients with COVID pneumonia. Hospitals would start patients on a nasal cannula at 4-6 L/min and, if that wasn’t sufficient, move to higher flow devices or ventilation. Patients who needed long-term oxygen after recovering from COVID also often went home with nasal cannulas. Some nasal cannulas during COVID were used with humidifiers and flows up to 6 L/min at home. There was also widespread use of high-flow nasal cannula (HFNC) devices in hospitals – which is a specialized use where warmed, humidified oxygen at very high flow rates (e.g., 30-60 L/min) is delivered via larger nasal prongs. This is still a “nasal cannula” in principle, but a more advanced application helping patients avoid intubation in some cases of respiratory failure.
In summary, nasal cannulas are used any time a patient needs supplemental oxygen but does not require intensive breathing support. They are the go-to device for:
- Chronic oxygen therapy in lung and heart disease (improving quality of life and exercise tolerance).
- Acute medical care to treat or prevent hypoxemia (low blood oxygen) in conditions like pneumonia, heart attacks, strokes, etc.
- Emergency response when a person is breathing on their own but oxygen is low.
- Situational needs like high altitude adaptation or procedural sedation.
They’re popular because they’re effective, simple, and patient-friendly – providing the necessary oxygen while still allowing patients to eat, talk, and engage in daily activities with minimal restriction.
Types of nasal cannulas generally refer to the different designs and specialized versions of cannulas used to deliver oxygen. While all nasal cannulas share the basic concept of two prongs in the nostrils and tubing to an oxygen source, there are variations tailored for specific needs. Here are the main types of nasal cannulas:
-
Standard Nasal Cannula: This is the most common type used in hospitals and home oxygen therapy. It’s the familiar design with two small prongs that sit just inside the nostrils and tubing that loops over the ears. Standard cannulas are used for low to moderate oxygen flow rates (typically up to about 5–6 liters per minute). They are made of soft plastic and come in different lengths of tubing (like 4-foot, 7-foot, 25-foot) depending on patient mobility needs. The standard cannula is appropriate for most adults and older children who need supplemental oxygen for conditions like COPD, pulmonary fibrosis, mild pneumonia, etc. It provides an effective means to increase oxygen levels while being relatively comfortable and allowing the patient to talk and eat.
-
Soft-Tip or Comfort Nasal Cannula: This is a variant of the standard cannula designed for improved comfort, especially during long-term use. The prongs and the portion that rests on the upper lip are made of extra-soft, flexible silicone or softer plastic. They often have slightly curved or flared prongs that fit more comfortably in the nostrils. Patients on 24/7 oxygen or who have sensitive skin benefit from these, as they reduce irritation to the nares and ears. Brands like Salter Labs have “soft” cannulas advertised for their gentle feel. In terms of functionality (oxygen delivery), they’re the same as a standard cannula; the difference is mainly patient comfort and reduced friction/pressure sores. Often, patients who find the regular cannula prongs too stiff will switch to a soft-tip cannula for continuous home use.
-
High-Flow Nasal Cannula (HFNC): High-flow nasal cannulas are specialized systems used in hospitals for delivering very high flow rates of oxygen and air (anywhere from 15 up to 60 liters per minute, or more) with added humidification and heating. Physically, the high-flow cannula has larger prongs and is attached to a heated humidifier machine and blender that can deliver precise oxygen concentrations (even up to 100% oxygen) at high flows. This type is often used for patients with severe respiratory distress or acute respiratory failure – for example, patients with COVID-19 pneumonia or acute heart failure may be placed on HFNC as an alternative to intubation. Despite the high flow, because the oxygen is humidified and warmed, it’s more comfortable than blasting cold dry oxygen. The larger-bore tubing and prongs distinguish HFNC from standard cannulas. It’s important to note that HFNC is a whole system (machine + cannula), not just a tubing—so you wouldn’t usually see HFNC used at home; it’s more for critical care or step-down units. There are some intermediate cannulas called “high concentration” cannulas that can handle flows of, say, 6–15 L/min (with external humidifiers) that might be used in ambulances or for short-term boosts, but true HFNC setups are hospital-based.
-
Pediatric and Infant Nasal Cannulas: These are smaller cannulas designed for babies and children. They come in neonatal, infant, pediatric sizes (the prongs and face interface are scaled down). Using an adult cannula on a baby would be impractical and could ulcerate the nostrils, so pediatric cannulas ensure a proper fit. They also deliver appropriate flow rates for little ones (often much lower flows, measured in fractions of a liter for newborns). The tubing is often lighter and designed to minimize pulling on tiny ears and cheeks. In neonatal intensive care units, very small premature babies on low-flow oxygen will wear these delicate cannulas, sometimes secured with a bit of tape. For older children who still need oxygen (like a toddler with bronchopulmonary dysplasia on home oxygen), pediatric cannulas also have soft prongs and a flexible design to allow the child to move around and play. The concept is the same as adult cannulas, just miniaturized and optimized for sensitive skin and small facial features.
-
Reservoir Nasal Cannulas (Oxymizer Cannulas): These are special cannulas that include an oxygen reservoir to increase the efficiency of oxygen delivery. They come in two main designs: a “mustache” Oxymizer (with a small reservoir pouch that sits below the nose and looks a bit like a mustache) or a “pendant” Oxymizer (a reservoir that hangs like a pendant on the chest). These reservoirs store oxygen in between breaths. When the patient inhales, they get a bolus of concentrated oxygen from the reservoir in addition to the continuous flow. This allows a higher effective FiO₂ (oxygen concentration) to reach the lungs without increasing the liter flow. Essentially, a reservoir cannula can deliver the same oxygen benefit at, say, 2 L/min that a standard cannula might at 4 L/min, because it saves oxygen that would otherwise be wasted when exhaling. They are useful for patients who need higher oxygen levels but want to remain on nasal cannula rather than switching to a face mask, or to conserve oxygen from tanks (each breath uses the stored O₂ more efficiently). Some patients with pulmonary fibrosis or severe COPD who need high oxygen might use these so they can ambulate longer on a portable tank.
-
Curved-Prong Cannulas vs. Straight-Prong Cannulas: This is a minor distinction, but cannulas come with slightly different prong shapes. Curved prong cannulas are anatomically curved to fit the curvature of the nostrils (prongs curve back towards the face). Many people find these more comfortable and they may direct flow a bit better into the nasal passages. Straight prong cannulas have prongs that go straight into the nose; they’re often the basic design. Some brands label their cannulas as “curved, non-flared” or “straight, flared” etc. Flared prongs have a wider opening at the tip to possibly make oxygen dispersion gentler. These design tweaks let clinicians choose a cannula that the patient finds most comfortable and effective. So while not “types” in terms of usage, they’re variants one might encounter.
-
High-Concentration Nasal Cannulas: In some contexts, you may hear of a “high-concentration nasal cannula” which typically refers to a standard cannula used at the upper end of its effective flow range, often with humidification and maybe larger bore tubing. For example, some emergency kits have a larger tubing cannula that can handle 15 L/min (though at that point, a mask is usually more appropriate). This is not a distinct device like HFNC, but rather a beefed-up version of the standard cannula for short-term use when a mask isn’t tolerated.
-
Nasal Prongs for Nasopharyngeal Oxygen: Rarely, there are systems where oxygen is delivered via a thin catheter placed deeper into the nasal passage (near the nasopharynx) – sometimes called “nasopharyngeal catheter” or “nasal prong” in older literature. Before modern cannulas were prevalent, a single thin tube could be inserted deeper into one nostril for oxygen. That provided a bit more direct oxygen delivery than just at the nostril. Nowadays, this method is seldom used because standard and high-flow cannulas cover needs well, but it’s a historical type. It might be considered if a patient can’t tolerate prongs in the nostrils but could handle a soft catheter in one nasal passage.
-
Specialty Cannulas (e.g., for Sleep or Exercise): There are also some proprietary cannulas designed for specific situations. For instance, a “quiet” cannula that reduces the noise of oxygen flow (some patients find the hissing sound annoying at night). Or a split cannula where one side can deliver a slightly different flow than the other (though that’s unusual). By and large, however, the main types are as listed above: standard, soft, high-flow, pediatric, reservoir.
It’s worth noting that while an oxygen mask is not a “nasal cannula,” it is another category of oxygen delivery device. Masks (simple face mask, Venturi mask, non-rebreather mask, etc.) are used when higher oxygen concentrations are needed or if the patient is a mouth-breather who wouldn’t get the full benefit from a cannula. The question, however, is specifically about types of nasal cannulas, so we focus on cannula variations.
In summary, the types of nasal cannulas include:
- Standard cannulas for routine low/mid-range oxygen needs.
- Soft or comfort cannulas for long-term use to minimize irritation.
- High-flow nasal cannula systems for critical care, delivering heated, humidified oxygen at much higher flow rates.
- Pediatric/infant cannulas scaled for children and babies.
- Reservoir (Oxymizer) cannulas that improve oxygen delivery efficiency with built-in reservoirs.
- Other variants like curved vs. straight prongs and nasopharyngeal catheters, which are more about comfort/fit or older techniques.
Healthcare providers will choose the type based on the patient’s oxygen requirements, age/size, comfort considerations, and the clinical setting. Each type is aimed at ensuring the patient gets adequate oxygen in the most comfortable and effective way possible.
Nasal cannula flow rates refer to how many liters of oxygen per minute (L/min) are delivered through a nasal cannula, and each flow rate corresponds to an approximate oxygen concentration that the patient breathes in (the FiO₂, or fraction of inspired oxygen). Here are the typical flow rates for a standard adult nasal cannula and the oxygen percentages they provide:
-
1 L/min: Delivers about 24% oxygen. (Room air is ~21% oxygen, so 1 liter of supplemental O₂ raises the FiO₂ to roughly 24%.)
-
2 L/min: ~28% oxygen. (A general rule of thumb is that each additional liter per minute increases FiO₂ by about 3-4% in a nasal cannula.)
-
3 L/min: ~32% oxygen
-
4 L/min: ~36% oxygen
-
5 L/min: ~40% oxygen
-
6 L/min: ~44% oxygen
These values are approximate. The actual FiO₂ a person receives can vary based on their breathing pattern (how deeply and fast they breathe, which causes mixing of delivered oxygen with room air). But generally:
-
A nasal cannula can provide around 24% to 44% oxygen at flow rates of 1 to 6 L/min. This is sufficient for many patients with mild to moderate oxygen needs.
-
Flow rates above 6 L/min are generally not recommended for a standard nasal cannula. At higher flows, the cannula becomes less effective (much of the oxygen might blow out and not be inhaled) and can be uncomfortable, causing nasal dryness and irritation. If a patient requires more oxygen than ~44% FiO₂ (or more flow than 6 L/min can provide), clinicians typically switch to a different oxygen delivery device:
- For example, a simple face mask can deliver about 40-60% oxygen at 5-10 L/min.
- A non-rebreather mask can deliver 60-90% oxygen at 10-15 L/min.
- Or a Venturi mask can deliver a precise FiO₂ (e.g., 50% at a set flow with an adapter).
- In critical care, a High-Flow Nasal Cannula (HFNC) system (which is different from a regular cannula) can deliver very high flows (up to 60 L/min or more) with close to 100% FiO₂ in a heated, humidified form, But HFNC is a special setup typically used in hospitals for severe respiratory distress.
Humidification: When oxygen is delivered at higher flow rates (generally above 3–4 L/min), it’s often humidified to prevent the nasal passages from drying out. In hospitals and home concentrators, you’ll often see a humidifier bottle attached when flows of 4 L/min or greater are used continuously.
Pediatric Note: For infants and young children, flow rates are much lower. A premature baby might be on 0.1 to 0.5 L/min, an infant on 0.5 to 2 L/min, etc., depending on the need, with appropriately smaller cannulas. The FiO₂ increases similarly in percentage terms, but careful monitoring is required to avoid giving too much oxygen to babies (due to risks like eye damage in preemies).
Relationship between Flow and FiO₂: A common teaching is: For every 1 L/min increase in flow, FiO₂ goes up by ~4%. Starting from 21% at room air:
- 1 L ≈ 24%
- 2 L ≈ 28%
- 3 L ≈ 32%
- 4 L ≈ 36%
- 5 L ≈ 40%
- 6 L ≈ 44%
This rule holds reasonably well in practice for flows 1-6 L/min as long as the patient’s breathing isn’t extremely heavy. If a patient is breathing very rapidly and deeply, the effective FiO₂ might be a bit lower (because they’re pulling in more room air per breath along with the oxygen).
Titration and Use: In clinical practice, doctors and nurses will adjust the nasal cannula flow to achieve target oxygen saturations (SpO₂) in the patient’s blood. For example, they might start at 2 L/min and then check the oximeter; if SpO₂ is still below the goal, they’ll go to 3 L, then 4 L, etc. Many patients at home are given a specific flow rate to use at rest and one for exertion. For instance, “2 L/min at rest, 4 L/min during exercise” if they desaturate with activity.
High-Flow Systems vs. Standard Cannula:
- Standard cannula: 1-6 L/min (some sources allow up to 8 L/min with special high-flow cannula tubing, but beyond 6 L the efficiency drops a lot). Max FiO₂ ~ 40-45%.
- High-Flow Nasal Cannula (HFNC): 10-60+ L/min, with heated humidity. FiO₂ can be 21% to 100%. This is a different apparatus used in ICU/ER for severe cases and is not the typical nasal cannula used at home or on regular hospital floors.
In summary, nasal cannulas deliver oxygen at flow rates typically between 1 and 6 liters per minute, translating to approximately 24% to 44% oxygen being breathed in. Each liter per minute increase raises the delivered oxygen concentration by about 3-4%. If a patient needs more oxygen than what 5-6 L/min via cannula provides, healthcare providers will switch to other oxygen delivery methods (like masks or high-flow devices) to meet the oxygen demand.
Nasal cannulas come in a few different sizes and configurations to fit various patient age groups and needs. Unlike something like IV cannulas which are measured by gauge, nasal cannula “sizes” are generally categorized by patient type (infant, pediatric, adult) and by the length/diameter of the tubing appropriate for different oxygen flow rates. Here are the main types of nasal cannula sizes:
-
Infant (Neonatal) Nasal Cannula: These are the smallest cannulas, designed for newborns and premature babies. They have very tiny, delicate prongs that fit into a baby’s little nostrils without causing trauma. The spacing between the prongs is narrower to match an infant’s nose. The tubing is also narrower and ultra-soft. Infant cannulas deliver low flow rates of oxygen (often measured in fractions of a liter per minute, like 0.1 to 1 L/min) because babies have small tidal volumes. They often come with special securement mechanisms (like gentle head straps or adhesive tabs on the cheeks) to keep them in place on squirmy infants. In hospitals, you might hear terms like “neonatal cannula” or “premature cannula” for the smallest sizes. These ensure that premature infants or newborns needing oxygen (e.g., in neonatal intensive care units or for conditions like bronchiolitis) get the support they need comfortably.
-
Pediatric Nasal Cannula: This is a medium size cannula made for children, typically from toddlers up to pre-teens (though exact breakpoints vary by manufacturer). Pediatric cannulas have prongs that are larger than the infant size but still smaller than adult ones. The distance between prongs and the size of the curved nasal piece are scaled for a child’s face. They are used for kids who need supplemental oxygen for conditions such as pediatric pneumonia, asthma flare-ups, congenital heart or lung issues, etc. The flow rates for pediatric cannulas are usually in the range of 0.5 to 4 L/min, depending on the child’s size and doctor’s prescription. Using an adult cannula on a small child can be uncomfortable or ineffective (the prongs might be too wide and not sit properly), so the pediatric size ensures proper fit and oxygen delivery.
-
Adult Nasal Cannula: The adult size is the standard nasal cannula for adolescents and adults. It has the largest prongs and prong spacing to accommodate adult nostrils and faces. Adult cannulas are typically used for flow rates from 1 to 6 L/min (though some are labeled to handle up to 8 L/min, generally above 6 L the effectiveness plateaus without humidity). Most adult cannulas are designed one-size-fits-most, but some manufacturers offer slight variations such as “Small Adult” or “Large Adult” cannulas; these adjust the prong size/spacing and tubing length a bit for smaller-framed or larger-framed individuals. However, in practice, the standard adult cannula works for the vast majority of adult patients. This is the cannula you’d get in the hospital if you, say, needed oxygen for pneumonia or after surgery, and it’s what home oxygen users wear for COPD or other chronic conditions.
-
High-Flow Nasal Cannula (Specialized Adult Cannula): While not a different “size” in the traditional sense of patient body size, it’s worth noting that high-flow oxygen delivery systems use a special type of larger cannula. These cannulas have wider bore prongs and tubing to accommodate much higher flow rates (up to 40-60+ L/min) and usually connect to a heated humidifier. They’re used in critical care environments for adults and children in respiratory distress. For example, a high-flow cannula for an adult will have thicker, short prongs that sit in the nostrils (often allowing some leak around them for comfort) and a more secure head strap to keep it in place. So, if you hear “high-flow nasal cannula,” it implies a device that is dimensioned to deliver high volumes of oxygen and is part of a special system – effectively a larger “size” cannula meant for that purpose. They come in sizes too (pediatric high-flow cannulas vs adult high-flow cannulas), but those are specific to the high-flow equipment and are not interchangeable with standard cannulas.
-
Cannula Tubing Lengths: Besides fitting the nose, cannulas differ in tubing length, which isn’t exactly a “size” of the cannula itself but is an important specification:
- Common lengths are 4 feet (1.2 m), 7 feet (2.1 m), 14 feet (4.3 m), 25 feet (7.6 m), and even 50 feet (15 m) for home oxygen users who want to move about their house. In hospitals, you usually see 7-foot cannulas which allow the patient to roll a bit in bed or sit up without yanking the oxygen source. At home, someone may use a 25 or 50-foot cannula connected to their concentrator so they can walk from room to room. The diameter of the tubing may slightly vary with length to ensure adequate oxygen flow to the patient (longer tubing can have more resistance, so some long hoses have a slightly larger internal diameter). But as far as “size,” when ordering cannulas, one would specify the patient size (infant, pediatric, adult) and the desired tubing length.
-
Specialty or Comfort Variations: Some manufacturers produce cannulas labeled as “small adult” or “large adult” for those on the edges of size ranges. For instance, a very petite adult might find a pediatric cannula more comfortable, or a “small adult” version if available. On the flip side, a “large adult” cannula may have slightly bigger prongs or a longer distance between prongs for folks with larger noses or facial features. Additionally, “micro” cannulas exist for cosmetic appeal when patients are out in public (these have extra-thin, less visible tubing and very small prongs, typically still delivering low flow oxygen). And soft cannulas (with softer, pliable silicone prongs) can come in the various sizes above to reduce irritation. These all essentially correspond to the same categorizations (infant, child, adult), just with different materials or slight adjustments.
To summarize by typical labeling:
- Neonate/Infant Cannula: Extremely small prongs, for newborns and babies up to ~1 year. Often used at very low flows (like 0.1 – 1 L/min).
- Pediatric Cannula: Small prongs, for children ~1 year up to early teens, depending on child’s size. Used at low-to-moderate flows (0.5 – 4 L/min).
- Adult Cannula: Standard prongs, fits older teens and adults. Used at flows around 1 – 6 L/min (some up to 8 L/min if humidified).
- (Sometimes subdivided into Small Adult or Large Adult by certain brands, but these are less common).
Each of these is designed to ensure the prongs sit comfortably in the nostrils without stretching or causing sores, and to deliver oxygen effectively for that patient’s typical breathing volumes. When getting oxygen supplies, it’s important to choose the right cannula size: for instance, a pediatric cannula on an adult might not deliver enough oxygen because the prongs are shorter and could easily dislodge, whereas an adult cannula on a toddler would be too big and inefficient. Medical providers or oxygen supply companies will select the appropriate size based on the patient’s age and size, thereby optimizing comfort and oxygen therapy effectiveness.
Oxygen therapy is a treatment that provides you with extra oxygen when you’re not getting enough through normal breathing. In simple terms, it means breathing in air that has a higher concentration of oxygen than the normal atmosphere. This “supplemental oxygen” can help raise the oxygen levels in your blood, which is vital for your organs and tissues to function properly.
People typically need oxygen therapy if their lungs aren’t absorbing enough oxygen on their own. This can happen due to various medical conditions or situations, such as:
- Chronic lung diseases: like COPD (chronic obstructive pulmonary disease), emphysema, or pulmonary fibrosis, where damaged lung tissue can’t extract sufficient oxygen from air.
- Asthma or Pneumonia: during severe flare-ups or infections when airways are narrowed or filled with fluid.
- Heart failure or heart conditions: where poor circulation leads to low oxygen delivery in the body.
- COVID-19 or other acute respiratory infections: that can cause low blood oxygen levels (hypoxemia).
- Sleep apnea or other sleep-related breathing disorders: in some cases, doctors prescribe nighttime oxygen.
- Premature infants with underdeveloped lungs: who may require oxygen support until their lungs mature (often in neonatal intensive care).
How Oxygen Therapy is Delivered: Oxygen is considered a medication, and it’s prescribed by a healthcare provider after determining that your blood oxygen is low (using tests like pulse oximetry or arterial blood gas). The oxygen can come from different sources – large tanks of compressed oxygen gas, liquid oxygen reservoirs, or electric oxygen concentrators that pull oxygen from the air. Once you have a source, the oxygen is most commonly delivered in one of the following ways:
- Nasal Cannula: A small, flexible tube with two prongs that sit in your nostrils. This is one of the most common methods for low to moderate oxygen needs. You’ll see people at home or in the hospital using nasal cannulas, which allow them to talk and eat while getting oxygen. The oxygen flow is measured in liters per minute (for example, 2 liters per minute via cannula is a typical starting dose).
- Oxygen Mask: A mask fits over your nose and mouth and is secured by an elastic strap. Masks are used when a higher concentration of oxygen is needed or if someone is a mouth-breather. There are simple face masks, Venturi masks (which can control the exact oxygen percentage), or non-rebreather masks (for high concentrations in emergencies).
- Oxygen “Tent” or Hood: Mostly used for infants or children, these enclosures can provide a controlled oxygen environment around the head.
- Hyperbaric Oxygen Therapy: A special form of oxygen therapy where you breathe 100% oxygen inside a pressurized chamber. This isn’t for routine low-oxygen situations, but rather for specific conditions like carbon monoxide poisoning, decompression sickness, or difficult wounds. It delivers oxygen at high pressure to super-saturate the blood with oxygen.
- Mechanical Ventilation (in critical care): If someone cannot breathe adequately on their own (for instance, during surgery under general anesthesia or in severe respiratory failure), oxygen is delivered through a ventilator with a tube down the windpipe. This is a form of oxygen therapy in life-support scenarios.
Goals and Benefits of Oxygen Therapy: By increasing the oxygen available to the lungs, oxygen therapy helps:
- Relieve symptoms of low oxygen such as shortness of breath, fatigue, dizziness, or confusion.
- Improve organ function: vital organs like the heart and brain require adequate oxygen. Supplemental oxygen can prevent damage that might occur from prolonged oxygen deprivation.
- Enhance quality of life: People on long-term oxygen often find they have more energy and can be more active. For example, someone with COPD might be able to walk farther or sleep better at night with their oxygen on, because their tissues are getting the oxygen they need.
- Support healing: In acute situations like pneumonia or trauma, giving oxygen buys time and supports the body’s healing process by ensuring tissues aren’t starved of O₂.
- Increase lifespan in chronic conditions: Studies have shown that for patients with chronic lung diseases and chronically low oxygen levels, using oxygen therapy for the prescribed hours each day can help them live longer. It reduces strain on the heart (low oxygen makes the heart pump harder).
Safety and Usage: Oxygen therapy is generally safe, but there are important safety considerations:
- Fire Hazard: Oxygen makes things burn more easily. You must never smoke or have open flames (like candles or gas stoves) in the vicinity of oxygen therapy. “No smoking – oxygen in use” signs are often placed where home oxygen is being used.
- Dryness and Irritation: Oxygen, especially from pressurized tanks or concentrators, can be dry. It may cause dryness in your nose or mouth, or irritation to your skin where the cannula or mask sits. Often, humidifiers are attached to oxygen systems to add moisture, and skin moisturizers (that are oxygen-safe) can help prevent sores where tubing rests on the ears or cheeks.
- Dosage as Prescribed: It’s important to use the flow rate prescribed by your doctor. Using too little might not improve your condition, and using too much can (in some cases) diminish your body’s natural drive to breathe or cause buildup of carbon dioxide. For most people, the doctor will specify a target oxygen saturation (like “keep SpO₂ above 90%”) and the corresponding oxygen flow rate to achieve that. Regular follow-ups ensure you’re on the right amount. Never adjust your oxygen flow rate upwards without medical advice, especially if you have COPD (some COPD patients are sensitive to high oxygen levels).
- Portable Use: Oxygen can be used at home continuously. Portable oxygen concentrators and small tanks allow people to go out, travel, and maintain mobility. For instance, there are lightweight battery-powered concentrators that people can sling over their shoulder, which provide oxygen via nasal cannula on the go. This means oxygen therapy doesn’t necessarily confine someone to a bed or chair; modern solutions aim to keep patients active.
In essence, oxygen therapy (also called supplemental oxygen) is a supportive therapy to ensure the body gets the oxygen it needs when illness or altitude or other factors prevent you from absorbing enough on your own. It’s a common and often life-improving (even life-saving) treatment in both acute medical care and chronic disease management. By breathing in extra oxygen via devices like cannulas or masks, patients can maintain safer oxygen levels, which helps relieve strain on the body and can make them feel much better.




















