Filters
- All Natural Ingredients (1)
- Aloe Vera Gel (2)
- Anti-Inflammatory (3)
- Arthritis (4)
- Arthritis pain (7)
- arthritis pain relief (5)
- Arthritis Pain Relief Cream (4)
- Arthritis Pain Reliever (3)
- Arthritis Treatment (2)
- Back Pain (5)
- Best Arthritis Pain Cream (1)
- glucosamine and chondroitin sulfate (1)
- MSM (2)
- nerve pain (3)
- Nerve Pain Medication (1)
- Osteoarthritis Knee Pain (1)
- powerful antioxidants (1)
- Treat Arthritis (1)
- Treat Fibromyalgia (1)
- Treat Osteoarthritis (1)
- Turmeric (2)
- Muscle Pain (5)
- Muscle Therapy Gel (1)
- Pain Gel (2)
- Relieve Muscle Pain (5)
- Sports Injuries (1)
- Sports Recovery Gel (1)
- Sports Therapy Gel (1)
- Roll On (1)
- Aesthetic Supplies MedSpa Supplies & Cosmetic Surgery Supplies (1)
- anesthesologist (1)
- Anesthetic (6)
- anesthetic spray (2)
- Gebauer (1)
- Gebauer Pain Spray (1)
- Local Anesthetic (2)
- numb pain (1)
- Numb Skin (1)
- Pain ease Spray (1)
- Topical Anesthetic (8)
- 5% Lidocaine (2)
- Adhesive Patches (2)
- Aspercreme (1)
- Aspercreme Pain Relief (2)
- Aspercreme Creme with Lidocaine (1)
- Icy Hot (2)
- Icy Hot Patches (2)
- Pain Patches (2)
- Pain Relief Patches (3)
- Addaprin (1)
- Advil (7)
- Fever Reducer (7)
- ibuprofen (5)
- Ibuprofen Tablets (5)
- Packets (1)
- Pain Reducer (1)
- Unit Dose (1)
- Unit Dose Tablets (1)
- Analgesic (1)
- Cold Patch (1)
- Cold Therapy Pain Relief (1)
- Hot Pain Relief (2)
- Menthol (3)
- Pain Relief Medicine (2)
- topical analgesic (1)
- Topical Pain Relief (1)
- All Day Pain Reliever (2)
- Extra Strength Pain Relief (4)
- Fever Relief (4)
- Relieve Joint Pain (2)
- 20% Benzocaine (4)
- Benzocaine 20 (6)
- Canker Sores (2)
- Dental Work (1)
- Gum Pain (1)
- Mouth Sores (1)
- Oral Pian (1)
- Toothache (2)
- Beutlich Pharmaceutical (1)
- Canker sores (1)
- Fresh Mint (1)
- Hurricane (1)
- Hurricane Anesthetic (1)
- Oral Gel (1)
- Oral Pain (2)
- Oral Topical Anesthetic (1)
- Sore Gums (1)
- Tooth pain (1)
- Aches (1)
- Anti-inflammatory Medication (1)
- Back Pain Relief (1)
- Generic Advil (1)
- Ibuprofen 200 mg (1)
- Joint pain Relief (1)
- menstrual cramp relief (1)
- Motrin (1)
- NSAID (3)
- pain medication (1)
- painkiller (1)
- Toothaches (2)
- Biofreeze (1)
- menthol (1)
- Sore Muscles (1)
- stiff joints (1)
- Camphor (3)
- capsaicin (1)
- Tiger Balm Patches (1)
- benzocaine (1)
- benzodent (1)
- mouth pain (1)
- mouth sores (1)
- oral pain (2)
- Arnica (1)
- Arnica Pain Relief Gel (1)
- Arnicare Pain Relief Cream (1)
- Camphor 11% (1)
- Cassia Oil (1)
- Clove Oil (1)
- Menthol 11% (1)
- Mint Oil (1)
- Relieve joint pain (1)
- Sports Balm (1)
- muscle pain (1)
- salonpas (1)
- Salonpas Lidocaine (1)
- Salonpas Pain Gel (1)
- sore muscles (1)
- Analgesia (1)
- doctor-only (2)
- Intramuscularly (1)
- Ketorolac for Injection (1)
- Ketorolac Shot (1)
- Ketorolac Tromethamine (1)
- ketorolac tromethamine injection (1)
- Moderate to severe pain (1)
- Nonsteroidal anti-inflammatory drugs (NSAIDs) (1)
- Prostaglandins (1)
- Short-term management (1)
- Surgical procedures (1)
- Toradol (1)
- cold sores (2)
- dental pain (1)
- hurricaine (1)
- HurriCaine Oral Gel (1)
- sore throat (2)
- wild cherry (1)
- Heating Pads (1)
- Hot Therapy (1)
- Moist Heating Pad (1)
- Bulk (1)
- bulk bottle (1)
- Arthritis Hot (1)
- Arthritis Relief Gel (1)
- Hot Cream (1)
- methyl salicylate (1)
- First aid antiseptic (1)
- Hurricaine (1)
- Tubes (1)
- Back pain (1)
- Cold therapy (1)
- Cryotherapy (1)
- dura soft back brace (1)
- lower back (1)
- Cherry (1)
- Cherry Flavor (1)
- Cough Drops (1)
- Cough suppressant (1)
- Sore Throat Pain (1)
- Blue Emu (1)
- Deep penetrating (1)
- Emu Oil (1)
- Glucosamine (1)
- muscle stimulator (1)
- r3500 (1)
- russian pain (1)
- Anesthetic Swabs (1)
- Bee Sting (1)
- Insect Bite Relief (1)
- Insect bites (1)
- Jelly Fish Bites (1)
- Mosquito bites (1)
- Still Kill (1)
- After Burn (1)
- Burn Cream (1)
- burn gel (1)
- burn relief (1)
- Burn Relief Gel (1)
- Burns (1)
- Lidocaine Hydrochloride (1)
- minor burns (1)
- Skin Burn (1)
- sunburns (1)
- Treat Burns (1)
- aloe vera (1)
- dermoplast (1)
- lanolin oil (1)
- numbing (1)
- pain anesthetic (1)
- pain spray (1)
- relieve pain (1)
- stop pain (1)
- Topical antiseptic (1)
- Anorectal cream (3)
- Hemorrhoid Cream (2)
- Hemorrhoidal Relief (2)
- Hemorrhoids (2)
- Rectal (2)
- Relieve Hemorrhoids (2)
- Tronolane (1)
- Advil Chewables (1)
- Advil JR (1)
- Advil Junior (1)
- Advil Pain Relief (2)
- children's (1)
- Childrens Aspirin (1)
- cold & flu (1)
- cold and flu (1)
- Cold Cough (1)
- Cold Medication (1)
- Cold Symptom (1)
- cough and cold relief (1)
- Fevers (1)
- Illness (1)
- Nighttime cold medicine (1)
- non drowsy (2)
- Pediatric (1)
- Pediatric Medicine (1)
- Runny Nose (3)
- Sickness (1)
- Advil Migraine (1)
- Capsules (1)
- Headache (3)
- Liquid Filled (1)
- Relieve Migraine Pain (1)
- Finger Cots (1)
- Rectal Pain Relief (2)
- Recticare (1)
- RectiCare Cream (1)
- Rectum (1)
- Anbesol (1)
- canker sore (1)
- Canker Sore Treatment (1)
- Cold Sore (1)
- Cervical Collar (1)
- Heat Pad (1)
- Neck Pain (1)
- Neck Wrap (1)
- Leg Pain (1)
- Mucsle Pain (1)
- Roll on (1)
- Rosemary (1)
- Hydrocortisone Acetate (1)
- Hydrocortisone Cream (1)
- Lidocaine with Hydrocortisone Acetate (1)
- Rectal Cream (1)
- Contains cassia oils (1)
- Pain Relieving Ointment (1)
- Anti itch (1)
- Gold Bond (1)
- Gold Bond Cream (1)
- Gold Bond with Lidocaine (1)
- Itch Relief (1)
- Itch Relief Cream (1)
- Itch Relief Treatment (1)
- Itch Skin (1)
- Itching (1)
- Itching Relief (1)
- Relieve itching (1)
- stop itching (1)
- Dual Channel (1)
- Ten Unit (1)
- Tens Unit (2)
- Ultima 3 (1)
- Ultima 3T (1)
- Relieve Back Pain (1)
- Treat Nerve Pain (1)
- Acetaminophen 500mg (1)
- Acetaminophen Pain Relief (1)
- Acetaminophen Pain Reliever (1)
- Fever Reducers (1)
- Headaches (2)
- Tylenol (1)
- Tylenol Extra Strength (1)
- Tylenol pain Relief (1)
- Tylenol Tablets (1)
- Advil Liqui-Gels (1)
- Advil Liqui-Gels Minis (1)
- Advil Liquid gels (1)
- Advil Pain Reliever (1)
- Ibuprofen Capsules (1)
- Liquid Filled Capsules (1)
- Liquid Gel Caps (1)
- Oral Care (1)
- Ethyl Chloride (1)
- Ethyl Chloride Spray (1)
- Gebauer's Ethyl Chloride (1)
- Gebauer’s ethyl chloride (1)
- instant pain relief spray (1)
- IV start numbing spray (1)
- minor procedure anesthetic (1)
- Mist Spray (1)
- Numb Pain (1)
- pre-injection anesthetic (1)
- skin refrigerant spray (1)
- Sports Injury (1)
- back pain (1)
- Trolamine salicylate 10% (1)
- Advil Coated Tablets (1)
- Advil Multisymptom Cold and Flu (1)
- Advil Sinus Congestion and Pain (1)
- All Night Pain Reliever (1)
- Body Aches (1)
- Clear Nasal Passages (1)
- coated tablets (1)
- Complete Respiratory System: Sinus (1)
- Nasal Congestion (1)
- Nasal Congestion Relief (1)
- Nasal decongestant (1)
- Nasal Swelling (1)
- One Tablet Dose (1)
- sinus pressure (1)
- Sinus pressure relief (1)
- Sinus relief (1)
- Treat sinus infections (1)
Pain Management Products, TENS Units, Back, Neck & Arthritis Relief
Pain Management Products
Pain management products are items and therapies used to relieve pain. They include medications (analgesics), topical creams/patches, and devices (like TENS units or braces) that target pain. The right choices depend on pain type (acute injury vs. chronic pain vs. nerve pain) and severity. Below are major categories, uses, and tips.
Over-the-Counter (OTC) Analgesics
- Acetaminophen (Paracetamol): Widely used for mild-to-moderate pain and fever (e.g. headaches, muscle aches). It’s safe at recommended doses (generally ≤3 g per day for adults). Common products include Tylenol. Don’t exceed dosing and be aware that many cold/allergy remedies and prescription pain pills also contain acetaminophen. Overdose can cause serious liver injury, so read labels carefully.
- NSAIDs (Aspirin, Ibuprofen, Naproxen): Nonsteroidal anti-inflammatory drugs treat pain plus inflammation (useful for sprains, arthritis, menstrual cramps). Examples: ibuprofen (Advil/Motrin), naproxen (Aleve), and aspirin. They block pain and reduce swelling. Take them with food or milk to protect the stomach. Long-term or high-dose NSAID use can irritate the stomach lining (ulcers or bleeding) and strain the kidneys. People with ulcers, kidney disease, or certain heart conditions should use NSAIDs cautiously or under doctor’s advice. Aspirin is also a blood thinner, which is why it’s generally not recommended for young children (risk of Reye’s syndrome) and must be used carefully in anyone with bleeding disorders.
- Topical OTC remedies: These include creams, gels, and patches applied directly to the skin. Examples: diclofenac gel (Voltaren), lidocaine patches/creams, capsaicin cream (chili-cream), menthol/analgesic rubs (e.g. Icy Hot). They provide localized relief (e.g. an achy knee or back) with minimal systemic side effects. Use as directed (avoid open wounds or broken skin, and wash hands after application).
Prescription Medications
- Prescription-strength NSAIDs or Acetaminophen combos: Your doctor may prescribe higher doses of NSAIDs or combination analgesics (e.g. acetaminophen plus codeine or hydrocodone) for moderate pain. These offer stronger pain relief but require monitoring for side effects like sedation or constipation.
- Opioids: Drugs like oxycodone (OxyContin), hydrocodone, morphine, and tramadol are very potent painkillers reserved for severe acute pain (post-surgery, cancer pain) or pain unresponsive to other treatments. They act on brain and spinal cord receptors to block pain. While effective, opioids carry significant risks: sedation, respiratory depression, constipation, and dependence/addiction. Current guidelines emphasize maximizing non-opioid therapies first and using opioids only if benefits outweigh risks. Always take opioids exactly as prescribed, never share them, and discuss any risk factors (sleep apnea, COPD, substance history) with your doctor.
- Neuropathic pain agents: When pain is due to nerve damage (e.g. diabetic neuropathy, post-shingles pain, fibromyalgia), certain drugs originally for other uses can help. These include antidepressants (amitriptyline, nortriptyline, duloxetine) and anticonvulsants (gabapentin, pregabalin). They work by altering nerve signal pathways. Your doctor will advise if these are appropriate, as they require a prescription and dose adjustments.
- Muscle Relaxants: Prescription muscle relaxers (e.g. cyclobenzaprine, methocarbamol) can relieve pain from muscle spasms (back strain, injury). They often cause drowsiness or dizziness, so use with caution (avoid driving or alcohol).
Topical & Local Therapies
- Lidocaine Patches/Gels: These numb a local area (similar to numbing cream). Good for back pain, shoulder pain, or nerve pain in a specific spot. Can be very effective with minimal side effects.
- Capsaicin Creams: Made from chili peppers, these creams deplete pain-carrying nerve transmitters over time. Used for neuropathic pain or arthritis pain in joints/feet. Some patients find long-term relief with regular use (note a burning sensation when first applied is normal and usually fades).
- Cold Therapy (Ice): For acute injuries (sprains, bumps), ice packs or cold wraps can reduce swelling and numb pain. Apply for 15–20 minutes on the affected area, with a cloth barrier on skin to prevent frostbite. This is often part of the “RICE” regimen (Rest, Ice, Compression, Elevation).
- Heat Therapy: Heat (heating pad, warm bath) relaxes muscles and increases blood flow. It’s helpful for chronic aches or stiff muscles (e.g. sore back or arthritis stiffness). Do not apply heat to a new injury or swelling. Use comfortably warm (not scalding) and never sleep on a heating pad.
Devices & Physical Aids
- TENS Units: Transcutaneous Electrical Nerve Stimulation (TENS) devices are battery-operated gadgets that send mild electrical pulses through the skin via adhesive pads. Many people use TENS for back pain, neck pain, neuropathic pain, etc. When set at a strong but comfortable intensity, TENS can block pain signals and provide short-term relief. In fact, a large 2022 review found that properly used TENS leads to clinically important pain reduction during or immediately after treatment. No major side effects occur with TENS (aside from minor skin irritation), but its effectiveness varies by person and condition. Always follow the device instructions and keep pads on intact skin away from cuts. (Note: People with pacemakers or epilepsy should consult their doctor before using TENS.)
- Braces and Support Garments: Knee braces, wrist splints, lumbar (back) support belts, and compression sleeves can help stabilize joints/tissues and reduce pain during movement. For example, wearing a knee brace during activity can ease arthritis pain. Make sure these fit correctly (not too tight) and are used as directed.
- Compression and Elevation: Elastic wraps or compression stockings can help with swollen limbs (e.g. after sprains). Elevating the limb above the heart when resting can also reduce swelling and pain.
- Assistive Chairs and Cushions: Ergonomic chairs, lumbar cushions, or neck pillows can indirectly relieve pain (especially chronic lower-back or neck pain) by improving posture and reducing stress on affected areas. Even small products like gel seat pads can make a difference for some patients.
Other Therapies & Supplements
- Acupuncture and Massage: These are not “products” per se but are complementary pain management modalities. Many patients find relief from acupuncture (fine needles at pressure points) or therapeutic massage. CDC pain guidelines explicitly list acupuncture and massage among useful non-drug therapies for chronic pain. These should be done by qualified practitioners.
- Biofeedback and Relaxation Aids: Devices like biofeedback monitors or smartphone apps that teach relaxation, breathing exercises, or meditation can help manage pain by reducing stress and muscle tension. While not a quick fix, they are safe and can improve chronic pain over time.
- Supplements: Some people use over-the-counter supplements like glucosamine-chondroitin (for joint pain) or omega-3 fish oil (for inflammation). The evidence is mixed. If you try these, choose reputable brands and inform your doctor (they can interact with medications or have side effects). Supplements are not regulated as strictly as medications, so caution is advised.
- Cannabidiol (CBD) products: CBD oil, creams, and patches are widely marketed for pain relief. Research is still limited. If used, ensure the product is legal in your area, and talk to your doctor about dosing and safety. (Note: CBD can interact with other meds and is not FDA-approved specifically for pain.)
Tips for Safe, Effective Use
- Follow Directions Carefully: Always use pain products as directed. Don’t exceed the recommended dose or frequency. For example, do not take more than 3,000–4,000 mg of acetaminophen per day. If symptoms persist, consult a doctor rather than self-increasing the dose.
- Check Labels: Many combination drugs contain analgesics. Read all ingredient labels to avoid doubling up. For instance, taking plain acetaminophen and also a cold medicine that contains acetaminophen can easily lead to overdose. Similarly, avoid combining multiple NSAIDs (like ibuprofen + aspirin) unless a doctor advises it.
- Use the Lowest Effective Dose: Start with the gentlest option that relieves your pain. For example, try acetaminophen first for a mild headache. If it’s not enough, you might alternate it with an NSAID (as recommended by some guidelines) or move up to prescription therapies for stronger pain. Using the lowest effective dose reduces side effects.
- Protect Your Stomach: Take NSAIDs with food, milk, or an antacid to lower the risk of stomach upset or ulcers. If you have a history of stomach bleeds, ask about COX-2-selective NSAIDs (they are gentler on the gut) or use acetaminophen instead.
- Mind Drug Interactions: Tell your doctor and pharmacist about all medications and supplements you take. Certain drugs (like blood thinners, blood pressure meds, SSRIs) can interact with painkillers. For instance, NSAIDs can raise blood pressure or react with anticoagulants, and some antidepressants can increase bleeding risk if taken with NSAIDs.
- Be Cautious with Addiction-Risk Drugs: If you use prescription opioids, do so only under medical supervision. Never mix opioids with alcohol or other sedatives (like benzodiazepines); this can dangerously depress breathing. Your doctor may prescribe laxatives or stool softeners to prevent constipation from opioids. Also inquire about carrying naloxone (an opioid overdose antidote) if you’re on high doses or have risk factors.
- Rotate Therapies: Combining therapies often gives the best relief. For example, after an acute injury apply ice and take a pain reliever, then use heat or gentle stretching during recovery. If one medication wears off or has side effects, consider switching to another class (e.g. from ibuprofen to acetaminophen) under guidance. This can maintain pain control while minimizing side effects.
- Stay Active and Exercise: Where appropriate, gentle exercise and movement reduce pain over time. Physical therapy, stretching, or low-impact activities (walking, swimming, yoga) strengthen muscles and improve flexibility, easing chronic pain. The CDC notes exercise as a key non-drug therapy for back pain, arthritis, and fibromyalgia. Even short, regular activity often yields significant benefits.
- Mind-Body Techniques: Techniques like deep breathing, meditation, and cognitive-behavioral therapy (CBT) can help manage chronic pain by reducing stress and improving coping. For example, CBT programs have helped many patients alter pain perceptions and improve function. These are safe add-ons that any person in chronic pain should consider.
- Weight Management: If overweight, losing even a few pounds can significantly reduce joint pain (especially in knees and hips). Diet modifications or working with a nutritionist can be an important part of a pain management plan.
- Monitor and Communicate: Keep track of what works and what side effects you get. If a product isn’t helping or is causing problems (new pain, rash, gastrointestinal issues), report this to your healthcare provider. Never ignore severe symptoms like chest pain or difficulty breathing; seek medical help. Also tell your doctor if pain limits daily activities (sleeping, walking, working) despite these products. Effective pain management often requires adjusting the plan over time.
Key Takeaway: Pain management products range from simple OTC medications (acetaminophen, NSAID pills or gels) to advanced prescription drugs and devices (opioids, nerve stimulators). The “most effective” choice depends on your pain’s cause and severity. For example, NSAIDs are excellent for inflammatory pain (arthritis, sprains), while topical lidocaine or capsaicin may be best for localized nerve or muscle pain. Always use products safely (observe doses, check interactions) and combine them with non-drug measures (ice/heat, movement, stress reduction). If pain is severe, new, or not improving, consult a healthcare provider. With proper use, the right combination of these products can greatly improve comfort and daily functioning.
-
 Sale 33%
Original price $ 29.95Current price $ 19.95
Sale 33%
Original price $ 29.95Current price $ 19.95Arthritis, Joint & Nerve Pain Relief Gel with Turmeric, Arnica, Glucosamine, Tea Tree Oil, Campor, Hyaluronic Acid, Vitamin E & Aloe Vera
53 reviewsMountain Ice is the newest product to hit the pain relief market. It has taken the active ingredient of menthol and combined powerful natural plan...
View full details -
 Sale 21%
Original price $ 29.95Current price $ 23.70
Sale 21%
Original price $ 29.95Current price $ 23.70Sports Recovery Gel for Muscle, Tendon & Ligament Pain Relief Gel
3 reviewsMountain Ice Sports Recovery Gel is specifically formulated for athletes and runners to promote muscle health and provide greater stamina, increase...
View full details -
 Sale 33%
Original price $ 26.95Current price $ 17.95
Sale 33%
Original price $ 26.95Current price $ 17.95Mountain Ice Sports Recovery Muscle Pain Relief Gel Roll-on 3 oz
1 reviewMountain Ice is a clinically recommended topical analgesic that combines the active ingredient of menthol with rich natural plants and extracts to ...
View full details -
 Sale 17%
Original price $ 64.95Current price $ 54.00
Sale 17%
Original price $ 64.95Current price $ 54.00Gebauer's Pain Ease Aerosol Mist Spray 118 mL
26 reviewsGebauer's Pain Ease® instant topical anesthetic skin refrigerant (Vapocoolant) is FDA cleared to temporarily control the pain associated with needl...
View full details -
 Sale 27%
Original price $ 79.95Current price $ 58.00
Sale 27%
Original price $ 79.95Current price $ 58.00Lidocaine 4% Pain Relief Patches Topical Anesthetic Skin Adhesive Patches (30 Count)
No reviewsExperience fast-acting relief with Lidocaine 4% Pain Relief Patches, easing discomfort and enhancing mobility for effective pain management. Lidoca...
View full details -
 Sale 25%
Original price $ 31.95Current price $ 23.99
Sale 25%
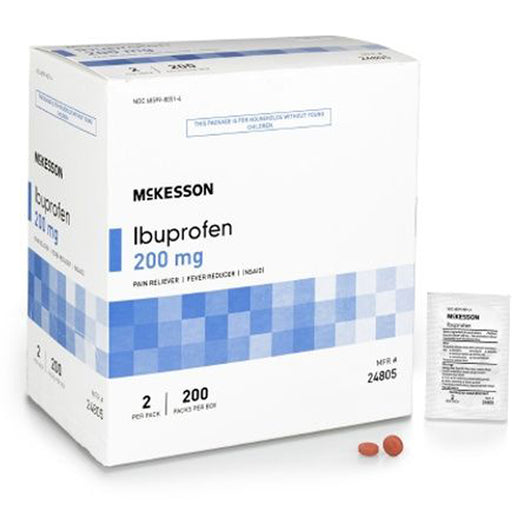
Original price $ 31.95Current price $ 23.99Ibuprofen Unit Dose Packets, 200 mg Strength Tablet (200 packs of 2)
No reviewsIbuprofen Unit Dose Packets 200 mg Strength Tablets 2-Packs can help provide relief from mild to moderate aches, pains, and headaches. Each Ibuprof...
View full details -
 Sale 43%
Original price $ 17.95Current price $ 10.25
Sale 43%
Original price $ 17.95Current price $ 10.25Cold and Hot Medicated Pain Relief Adhesive Patches (5-Pack)
No reviewsRugby Icy Cold and Hot Medicated Pain Relief Adhesive Patches provide temporary relief of minor aches and pains of muscles and joints associated wi...
View full details -
 Sale 40%
Original price $ 4.95Current price $ 2.99
Sale 40%
Original price $ 4.95Current price $ 2.99Naproxen Sodium 220 mg Pain Reliever Tablets All Day Pain Relief, 24 Count (Compare to Aleve)
No reviewsNaproxen Sodium Tablets, 220 mg Pain Reliever, are used to temporarily relieve pain due to minor aches and pains associated with skeletal muscle, b...
View full details -
 Sale 15%
Original price $ 16.95Current price $ 14.35
Sale 15%
Original price $ 16.95Current price $ 14.35Oral Anesthetic Pain Relief Gel Packet, 144/bx
5 reviewsSafetec Oral Pain Relief Packets are convenient for when you’re on-the-go to eliminate your oral irritations. The gel works great for canker sores,...
View full details -
 Sale 27%
Original price $ 16.95Current price $ 12.35
Sale 27%
Original price $ 16.95Current price $ 12.35Hurricane Topical Anesthetic Oral Gel with 20% Benzocaine, Fresh Mint Flavor
11 reviewsBeutlich Hurricane Topical Anesthetic Oral Gel is an over-the-counter solution for those who experience irritability in their mouth. The gel helps ...
View full details -
 Sale 44%
Original price $ 5.89Current price $ 3.29
Sale 44%
Original price $ 5.89Current price $ 3.29Ibuprofen Tablets 200mg Pain Reliever/Fever Reducer 100 Count
5 reviewsFast-Acting, Trusted Over-the-Counter Relief for Pain and Fever Get powerful, long-lasting relief from pain and fever with Ibuprofen Tablets 200mg ...
View full details -
 Sale
$ 13.95
Sale
$ 13.95Biofreeze Pain Relief Gel 4 oz Tube
8 reviewsBiofreeze provides cooling pain relief that temporary treats minor aches and pains of sore muscles and joints associated with arthritis, backaches,...
View full details -
 Sale 30%
Original price $ 9.95Current price $ 6.95
Sale 30%
Original price $ 9.95Current price $ 6.95Tiger Balm Pain Relieving Patches with Capsaicin, Camphor & Menthol (5 Adhesive Patches)
No reviewsTiger Balm Pain Relieving Patches with Capsaicin, Camphor, and Menthol are used to alleviate muscle and joint pain. These patches provide targeted ...
View full details -
 Sale
$ 5.65
Sale
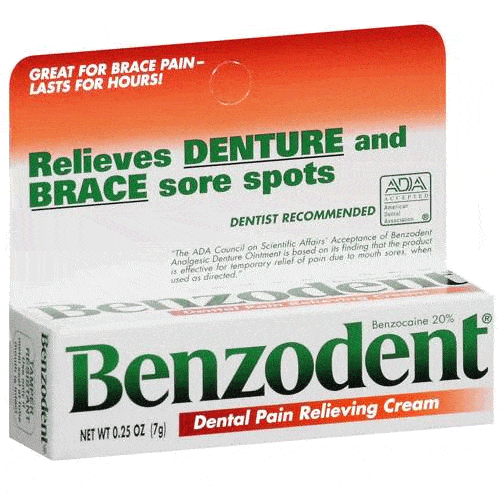
$ 5.65Benzodent Dental Pain Relieving Cream, 0.25 oz
3 reviewsProviding superior relief for oral discomfort caused by things like braces and/or canker sores, Benzodent Dental Pain Relieving Cream is made with ...
View full details -
 Sale 3%
Original price $ 13.95Current price $ 13.50
Sale 3%
Original price $ 13.95Current price $ 13.50Arnicare Arnica Pain Relief Cream
3 reviewsArnicare Arnica cream is a topical cream that is used to relieve pain, inflammation, and swelling. It is made with Arnica montana, a plant that is ...
View full details -
 Sale 25%
Original price $ 19.95Current price $ 14.95
Sale 25%
Original price $ 19.95Current price $ 14.95Tiger Balm Ultra Strength Pain Relieving Ointment 1.7oz
4 reviewsOffering superior relief for joint and muscle strain, Tiger Balm Ultra Strength Pain Relieving Ointment features the strongest combination of herba...
View full details -
 Sale 25%
Original price $ 14.95Current price $ 11.25
Sale 25%
Original price $ 14.95Current price $ 11.25Salonpas Lidocaine Plus Pain Relieving Cream
4 reviewsSalonpas Lidocaine Plus Pain Relieving Cream is a highly effective over-the-counter topical analgesic cream that provides fast and powerful relief ...
View full details -
 Sold out
Original price $ 185.00Current price $ 39.95
Sold out
Original price $ 185.00Current price $ 39.95Ketorolac Tromethamine Injection 60 mg/2 mL Single Dose Vials 2 mL, 25/Tray (Rx)
1 reviewKetorolac Tromethamine Injection 30 mg/2 mL is used for the short-term management of moderate to severe pain, often following surgical procedures. ...
View full details -
 Sale 37%
Original price $ 18.95Current price $ 11.95
Sale 37%
Original price $ 18.95Current price $ 11.95HurriCaine Oral Pain Anesthetic Gel with Wild Cherry Flavor
5 reviewsHurricane Oral Anesthetic Gel is a topical anesthetic that is used to numb the mouth and throat. It comes in a gel form and is applied to the area ...
View full details -
 Sale
$ 51.00
Sale
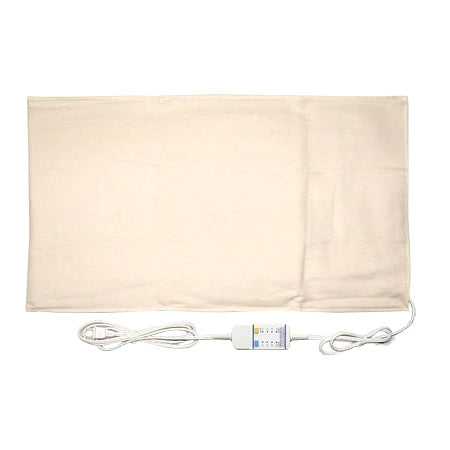
$ 51.00Thermotech Digital Infrared Moist Heating Pad (Medical Grade)
5 reviewsThe Thermotech Infrared Digital Moist Heating Pad is a medical grade heating pad that automatically provides moist heat without the need to add wat...
View full details -
 Sale 30%
Original price $ 19.95Current price $ 13.95
Sale 30%
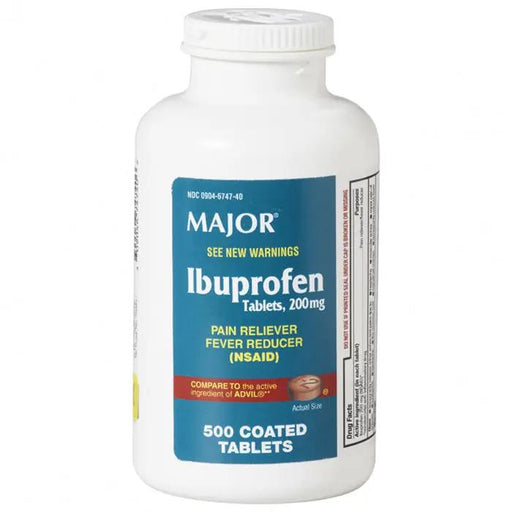
Original price $ 19.95Current price $ 13.95Ibuprofen 200mg Tablets, Coated Bulk Bottle, 500 count
2 reviewsIbuprofen 200mg Brown Coated Tablets in Bulk bottle of 500 tablets refers to a medication that contains 200mg of ibuprofen per tablet and is presen...
View full details -
 Sale 44%
Original price $ 6.95Current price $ 3.89
Sale 44%
Original price $ 6.95Current price $ 3.89Arthritis Hot Pain Relief Cream, Deep Penetrating 85 gram
1 reviewArthritis Hot Deep Penetrating Pain Relief Cream is a topical cream that is designed to provide relief from the pain and inflammation associated wi...
View full details -
 Sale 5%
Original price $ 79.95Current price $ 76.00
Sale 5%
Original price $ 79.95Current price $ 76.00Qfiber Infrared Heat Therapy Body Wrap
No reviewsThe innovatively designed high-tech Qfiber Infrared Heat Therapy Body Wrap provides exceptional levels of relief by deeply penetrating up to 2” int...
View full details -
 Sale 33%
Original price $ 78.95Current price $ 52.95
Sale 33%
Original price $ 78.95Current price $ 52.95HurriCaine Topical Anesthetic Pain Spray Kit with 200 Extension tubes
1 reviewBeutlich HurriCaine Topical Anesthetic Spray used to anesthetize mucosal tissue to elimate pain and discomfort. Can be used on multiple patients. W...
View full details -
 Sale
$ 194.00
Sale
$ 194.00DuraSoft Back Pain Relief Cryotherapy Wrap
No reviewsDonjoy DuraSoft Back Wrap is a cold therapy wrap for back injuries and surgical sites. Made with ultra-wick and antimicrobial fabric technologies, ...
View full details -
 Sale 22%
Original price $ 3.95Current price $ 3.10
Sale 22%
Original price $ 3.95Current price $ 3.10Halls Cough Drops Lozenges Cherry Flavor 30 Count
2 reviewsHalls Cough Drops will help deter your cough and sooth your sore throat. Made with menthol, this cough drop is cherry flavored, fast acting, and co...
View full details -
 Sold out
$ 21.95
Sold out
$ 21.95Blue Emu Super Strength Pain Relief Gel 4oz jar
No reviewsKeep your joints moving and soothe achy muscles with the powerful relief of Blue Emu Super Strength Pain Relief Gel, which features a unique combin...
View full details -
 Sold out
Original price $ 179.99Current price $ 167.00
Sold out
Original price $ 179.99Current price $ 167.00Russian Muscle Stimulator 3500
4 reviewsOne of the only portable Russian Stimulators available, the Russian Stim 3500 is a dual channel electro-stimulator with a symmetrical biphasic squa...
View full details -
 Sale 34%
Original price $ 5.99Current price $ 3.95
Sale 34%
Original price $ 5.99Current price $ 3.95Sting Kill Anesthetic Pain Swabs Instant Pain + Itch Relief From Bee Stings and Bug Bites, 5/Pack
1 reviewSting Kill External Anesthetic Swabs are a disposable topical swab used to relieve pain and itching caused from bee, insect and jellyfish stings. S...
View full details -
 Sale 14%
Original price $ 145.99Current price $ 125.99
Sale 14%
Original price $ 145.99Current price $ 125.99Ultima-Neo Tens Advanced Muscle Stimulator with Rechargeable Battery
No reviewsDesigned for ease of use and functionality, the Ultima Neo Advanced Multi-Mode Stimulator is a sophisticated multi-mode electrotherapy stimulator t...
View full details -
 Sale 53%
Original price $ 13.95Current price $ 6.50
Sale 53%
Original price $ 13.95Current price $ 6.50After Burn Serious Burn Treatment Gel with Lidocaine Hydrochloride & Aloe Vera
No reviewsTenders After Burn Gel provides scraps, cuts, sunburns, and other burns the relief they need. The burn gel soothes and reliefs your pain with aloe ...
View full details -
 Sale 28%
Original price $ 13.95Current price $ 9.99
Sale 28%
Original price $ 13.95Current price $ 9.99Dermoplast Pain, Burn & Itching Relief Spray with Aloe vera & Benzocaine 20%
No reviewsDermoplast is an numbing pain anesthetic that provides a “no-touch” application to the skin and makes it easy to get those hard to reach areas. Der...
View full details -
 Sale 20%
Original price $ 11.95Current price $ 9.55
Sale 20%
Original price $ 11.95Current price $ 9.55Tronolane Anesthetic Cream for Pain Relief 1 oz
1 reviewTronolane Anesthetic Cream provides relief from the discomfort caused by minor skin irritations. With a maximum strength non-greasy formula, this f...
View full details -
 Sale 40%
Original price $ 12.95Current price $ 7.75
Sale 40%
Original price $ 12.95Current price $ 7.75Children's Advil Junior Strength Chewable Grape Flavor 100 mg Tablets, 24 Count
No reviewsChildren's Advil Junior Strength Chewable Tablets in Grape Flavor are used to reduce fever and relieve pain in children aged 6 to 11 years. These c...
View full details -
 Sale 30%
Original price $ 8.95Current price $ 6.25
Sale 30%
Original price $ 8.95Current price $ 6.25Advil Migraine Liquid Filled Capsules 20 Count
No reviewsAdvil Migraine Liquid Filled Capsules are a powerful and effective solution for individuals who suffer from recurring migraines. These capsules are...
View full details -
 Sale 32%
Original price $ 49.95Current price $ 33.95
Sale 32%
Original price $ 49.95Current price $ 33.95Recticare Anorectal Cream Hemorrhoid Pain Relief Cream with 10 Finger Cots
No reviewsRecticare Anorectal Cream offers long-lasting and fast-acting relief from symptoms associated with anal and rectal discomfort. It contains the acti...
View full details -
 Sale 32%
Original price $ 9.95Current price $ 6.75
Sale 32%
Original price $ 9.95Current price $ 6.75Anbesol Liquid Oral Anesthetic Pain Reliever for Canker Sores, Toothaches & Denture Pain
1 reviewAnbesol Liquid Oral Pain Reliever in Cool Mint provides instant pain relief for a number of oral ailments. This convenient oral care product featur...
View full details -
 Sale
$ 46.00
Sale
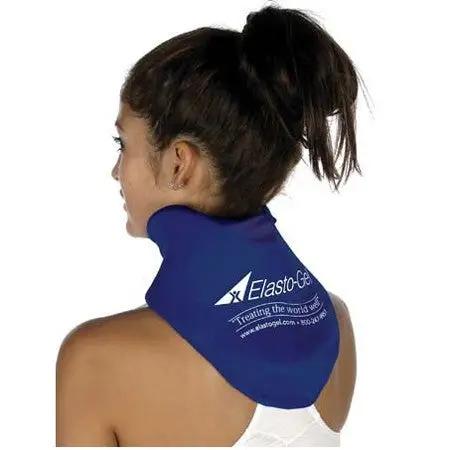
$ 46.00Elasto-Gel Cervical Collar Neck Wrap
1 reviewLeak-free hot and cold therapy is now within reach using the innovative Elasto-Gel Cervical Collar Wrap that conforms easily to various body styles...
View full details -
 Sale 14%
Original price $ 13.95Current price $ 11.95
Sale 14%
Original price $ 13.95Current price $ 11.95Aspercreme Roll-On Lidocaine Pain Relief with Rosemary & Mint No Mess Applicator
No reviewsTemporarily relieve minor pain and enjoy a fresh scent with Aspercreme Lidocaine Topical Pain Relief Liquid With Rosemary & Mint Essential Oils...
View full details -
 Sale 28%
Original price $ 135.00Current price $ 97.50
Sale 28%
Original price $ 135.00Current price $ 97.50Lidocaine HCI 3% with Hydrocortisone Acetate 0.50% Rectal Relief Cream (Rx)
No reviewsLidocaine 2% Hydrocortisone Acetate 3% Relief Cream is a topical cream that is applied to the skin to relieve pain and itching. The cream contains ...
View full details🔒 Medical License Required -
 Sale 26%
Original price $ 9.95Current price $ 7.35
Sale 26%
Original price $ 9.95Current price $ 7.35Tiger Balm Rub Extra Strength Pain Relief Ointment
No reviewsTiger Balm Rub Extra Strength Pain Relief is a uniquely formulated topical analgesic that soothes sore muscles and joints. This pain relief rub fea...
View full details -
 Sale 35%
Original price $ 15.95Current price $ 10.29
Sale 35%
Original price $ 15.95Current price $ 10.29Gold Bond Lidocaine Cream Maximum Strength 4% Pain and Itch Relief
2 reviewsGold Bond Lidocaine Cream offers fast pain relief for muscle aches, sunburn, and minor skin irritations. Gold Bond Lidocaine Cream soothes itching ...
View full details -
 Sale 40%
Original price $ 49.95Current price $ 29.95
Sale 40%
Original price $ 49.95Current price $ 29.95Ultima 3T Plus TENS Unit Dual Channel with Timer
2 reviewsUltima 3T TENS Unit Dual Channel with Timer is a unique pain management system designed to manage chronic muscle pain throughout the body. The TENS...
View full details -
 Sale
$ 29.95
Sale
$ 29.95TENS Unit, Transcutaneous Nerve Stimulation
No reviewsTranscutaneous electrical nerve stimulation (TENS) therapy is the most common form of electrical stimulation used for pain management. This small, ...
View full details -
 Sale 20%
Original price $ 19.95Current price $ 15.95
Sale 20%
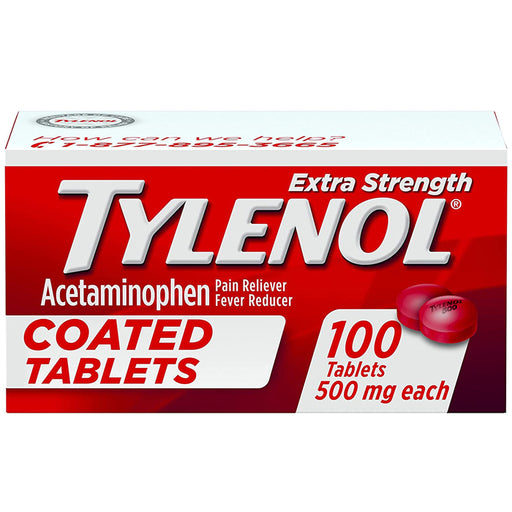
Original price $ 19.95Current price $ 15.95Tylenol Extra Strength 500mg Pain Reliever Fever Reducer Coated Tablets, 100 Count
No reviewsTylenol Extra Strength Coated Tablets are an over-the-counter pain reliever used to temporarily relieve minor aches and pains and temporarily reduc...
View full details -
 Sale 28%
Original price $ 9.95Current price $ 7.15
Sale 28%
Original price $ 9.95Current price $ 7.15Advil Liqui-Gel Minis Pain Reliever and Fever Reducer Ibuprofen 200mg 20 Count
No reviewsAdvil Liqui-Gel Minis are used for pain relief and to reduce inflammation and fever. Containing ibuprofen, these mini capsules quickly alleviate he...
View full details -
 Sale 25%
Original price $ 78.95Current price $ 59.00
Sale 25%
Original price $ 78.95Current price $ 59.00Gebauer's Ethyl Chloride Skin Refrigerant Spray Mist Topical Anesthetic (Ground Shipping Only)
29 reviewsTopical Anesthetic for Instant Pain Relief, Minor Procedures, and Sports Injuries Discover rapid pain relief and numbing power with the leading top...
View full details -
 Sale
$ 8.59
Sale
$ 8.59Mobisyl Pain Relieving Creme with Trolamine salicylate 10%, 3.5 oz
2 reviewsMobisyl Pain Relieving Creme is a special analgesic in the Mobisyl formula penetrates deep through tissue to deliver relief directly to painful mu...
View full details
People Also Searched For
Pain Management Products
Pain management products are items and therapies used to relieve pain. They include medications (analgesics), topical creams/patches, and devices (like TENS units or braces) that target pain. The right choices depend on pain type (acute injury vs. chronic pain vs. nerve pain) and severity. Below are major categories, uses, and tips.
Over-the-Counter (OTC) Analgesics
- Acetaminophen (Paracetamol): Widely used for mild-to-moderate pain and fever (e.g. headaches, muscle aches). It’s safe at recommended doses (generally ≤3 g per day for adults). Common products include Tylenol. Don’t exceed dosing and be aware that many cold/allergy remedies and prescription pain pills also contain acetaminophen. Overdose can cause serious liver injury, so read labels carefully.
- NSAIDs (Aspirin, Ibuprofen, Naproxen): Nonsteroidal anti-inflammatory drugs treat pain plus inflammation (useful for sprains, arthritis, menstrual cramps). Examples: ibuprofen (Advil/Motrin), naproxen (Aleve), and aspirin. They block pain and reduce swelling. Take them with food or milk to protect the stomach. Long-term or high-dose NSAID use can irritate the stomach lining (ulcers or bleeding) and strain the kidneys. People with ulcers, kidney disease, or certain heart conditions should use NSAIDs cautiously or under doctor’s advice. Aspirin is also a blood thinner, which is why it’s generally not recommended for young children (risk of Reye’s syndrome) and must be used carefully in anyone with bleeding disorders.
- Topical OTC remedies: These include creams, gels, and patches applied directly to the skin. Examples: diclofenac gel (Voltaren), lidocaine patches/creams, capsaicin cream (chili-cream), menthol/analgesic rubs (e.g. Icy Hot). They provide localized relief (e.g. an achy knee or back) with minimal systemic side effects. Use as directed (avoid open wounds or broken skin, and wash hands after application).
Prescription Medications
- Prescription-strength NSAIDs or Acetaminophen combos: Your doctor may prescribe higher doses of NSAIDs or combination analgesics (e.g. acetaminophen plus codeine or hydrocodone) for moderate pain. These offer stronger pain relief but require monitoring for side effects like sedation or constipation.
- Opioids: Drugs like oxycodone (OxyContin), hydrocodone, morphine, and tramadol are very potent painkillers reserved for severe acute pain (post-surgery, cancer pain) or pain unresponsive to other treatments. They act on brain and spinal cord receptors to block pain. While effective, opioids carry significant risks: sedation, respiratory depression, constipation, and dependence/addiction. Current guidelines emphasize maximizing non-opioid therapies first and using opioids only if benefits outweigh risks. Always take opioids exactly as prescribed, never share them, and discuss any risk factors (sleep apnea, COPD, substance history) with your doctor.
- Neuropathic pain agents: When pain is due to nerve damage (e.g. diabetic neuropathy, post-shingles pain, fibromyalgia), certain drugs originally for other uses can help. These include antidepressants (amitriptyline, nortriptyline, duloxetine) and anticonvulsants (gabapentin, pregabalin). They work by altering nerve signal pathways. Your doctor will advise if these are appropriate, as they require a prescription and dose adjustments.
- Muscle Relaxants: Prescription muscle relaxers (e.g. cyclobenzaprine, methocarbamol) can relieve pain from muscle spasms (back strain, injury). They often cause drowsiness or dizziness, so use with caution (avoid driving or alcohol).
Topical & Local Therapies
- Lidocaine Patches/Gels: These numb a local area (similar to numbing cream). Good for back pain, shoulder pain, or nerve pain in a specific spot. Can be very effective with minimal side effects.
- Capsaicin Creams: Made from chili peppers, these creams deplete pain-carrying nerve transmitters over time. Used for neuropathic pain or arthritis pain in joints/feet. Some patients find long-term relief with regular use (note a burning sensation when first applied is normal and usually fades).
- Cold Therapy (Ice): For acute injuries (sprains, bumps), ice packs or cold wraps can reduce swelling and numb pain. Apply for 15–20 minutes on the affected area, with a cloth barrier on skin to prevent frostbite. This is often part of the “RICE” regimen (Rest, Ice, Compression, Elevation).
- Heat Therapy: Heat (heating pad, warm bath) relaxes muscles and increases blood flow. It’s helpful for chronic aches or stiff muscles (e.g. sore back or arthritis stiffness). Do not apply heat to a new injury or swelling. Use comfortably warm (not scalding) and never sleep on a heating pad.
Devices & Physical Aids
- TENS Units: Transcutaneous Electrical Nerve Stimulation (TENS) devices are battery-operated gadgets that send mild electrical pulses through the skin via adhesive pads. Many people use TENS for back pain, neck pain, neuropathic pain, etc. When set at a strong but comfortable intensity, TENS can block pain signals and provide short-term relief. In fact, a large 2022 review found that properly used TENS leads to clinically important pain reduction during or immediately after treatment. No major side effects occur with TENS (aside from minor skin irritation), but its effectiveness varies by person and condition. Always follow the device instructions and keep pads on intact skin away from cuts. (Note: People with pacemakers or epilepsy should consult their doctor before using TENS.)
- Braces and Support Garments: Knee braces, wrist splints, lumbar (back) support belts, and compression sleeves can help stabilize joints/tissues and reduce pain during movement. For example, wearing a knee brace during activity can ease arthritis pain. Make sure these fit correctly (not too tight) and are used as directed.
- Compression and Elevation: Elastic wraps or compression stockings can help with swollen limbs (e.g. after sprains). Elevating the limb above the heart when resting can also reduce swelling and pain.
- Assistive Chairs and Cushions: Ergonomic chairs, lumbar cushions, or neck pillows can indirectly relieve pain (especially chronic lower-back or neck pain) by improving posture and reducing stress on affected areas. Even small products like gel seat pads can make a difference for some patients.
Other Therapies & Supplements
- Acupuncture and Massage: These are not “products” per se but are complementary pain management modalities. Many patients find relief from acupuncture (fine needles at pressure points) or therapeutic massage. CDC pain guidelines explicitly list acupuncture and massage among useful non-drug therapies for chronic pain. These should be done by qualified practitioners.
- Biofeedback and Relaxation Aids: Devices like biofeedback monitors or smartphone apps that teach relaxation, breathing exercises, or meditation can help manage pain by reducing stress and muscle tension. While not a quick fix, they are safe and can improve chronic pain over time.
- Supplements: Some people use over-the-counter supplements like glucosamine-chondroitin (for joint pain) or omega-3 fish oil (for inflammation). The evidence is mixed. If you try these, choose reputable brands and inform your doctor (they can interact with medications or have side effects). Supplements are not regulated as strictly as medications, so caution is advised.
- Cannabidiol (CBD) products: CBD oil, creams, and patches are widely marketed for pain relief. Research is still limited. If used, ensure the product is legal in your area, and talk to your doctor about dosing and safety. (Note: CBD can interact with other meds and is not FDA-approved specifically for pain.)
Tips for Safe, Effective Use
- Follow Directions Carefully: Always use pain products as directed. Don’t exceed the recommended dose or frequency. For example, do not take more than 3,000–4,000 mg of acetaminophen per day. If symptoms persist, consult a doctor rather than self-increasing the dose.
- Check Labels: Many combination drugs contain analgesics. Read all ingredient labels to avoid doubling up. For instance, taking plain acetaminophen and also a cold medicine that contains acetaminophen can easily lead to overdose. Similarly, avoid combining multiple NSAIDs (like ibuprofen + aspirin) unless a doctor advises it.
- Use the Lowest Effective Dose: Start with the gentlest option that relieves your pain. For example, try acetaminophen first for a mild headache. If it’s not enough, you might alternate it with an NSAID (as recommended by some guidelines) or move up to prescription therapies for stronger pain. Using the lowest effective dose reduces side effects.
- Protect Your Stomach: Take NSAIDs with food, milk, or an antacid to lower the risk of stomach upset or ulcers. If you have a history of stomach bleeds, ask about COX-2-selective NSAIDs (they are gentler on the gut) or use acetaminophen instead.
- Mind Drug Interactions: Tell your doctor and pharmacist about all medications and supplements you take. Certain drugs (like blood thinners, blood pressure meds, SSRIs) can interact with painkillers. For instance, NSAIDs can raise blood pressure or react with anticoagulants, and some antidepressants can increase bleeding risk if taken with NSAIDs.
- Be Cautious with Addiction-Risk Drugs: If you use prescription opioids, do so only under medical supervision. Never mix opioids with alcohol or other sedatives (like benzodiazepines); this can dangerously depress breathing. Your doctor may prescribe laxatives or stool softeners to prevent constipation from opioids. Also inquire about carrying naloxone (an opioid overdose antidote) if you’re on high doses or have risk factors.
- Rotate Therapies: Combining therapies often gives the best relief. For example, after an acute injury apply ice and take a pain reliever, then use heat or gentle stretching during recovery. If one medication wears off or has side effects, consider switching to another class (e.g. from ibuprofen to acetaminophen) under guidance. This can maintain pain control while minimizing side effects.
- Stay Active and Exercise: Where appropriate, gentle exercise and movement reduce pain over time. Physical therapy, stretching, or low-impact activities (walking, swimming, yoga) strengthen muscles and improve flexibility, easing chronic pain. The CDC notes exercise as a key non-drug therapy for back pain, arthritis, and fibromyalgia. Even short, regular activity often yields significant benefits.
- Mind-Body Techniques: Techniques like deep breathing, meditation, and cognitive-behavioral therapy (CBT) can help manage chronic pain by reducing stress and improving coping. For example, CBT programs have helped many patients alter pain perceptions and improve function. These are safe add-ons that any person in chronic pain should consider.
- Weight Management: If overweight, losing even a few pounds can significantly reduce joint pain (especially in knees and hips). Diet modifications or working with a nutritionist can be an important part of a pain management plan.
- Monitor and Communicate: Keep track of what works and what side effects you get. If a product isn’t helping or is causing problems (new pain, rash, gastrointestinal issues), report this to your healthcare provider. Never ignore severe symptoms like chest pain or difficulty breathing; seek medical help. Also tell your doctor if pain limits daily activities (sleeping, walking, working) despite these products. Effective pain management often requires adjusting the plan over time.
Key Takeaway: Pain management products range from simple OTC medications (acetaminophen, NSAID pills or gels) to advanced prescription drugs and devices (opioids, nerve stimulators). The “most effective” choice depends on your pain’s cause and severity. For example, NSAIDs are excellent for inflammatory pain (arthritis, sprains), while topical lidocaine or capsaicin may be best for localized nerve or muscle pain. Always use products safely (observe doses, check interactions) and combine them with non-drug measures (ice/heat, movement, stress reduction). If pain is severe, new, or not improving, consult a healthcare provider. With proper use, the right combination of these products can greatly improve comfort and daily functioning.
















































