Filters
- airsep (1)
- caire (1)
- Home Concentrator (1)
- Home Oxygen Concentrator (1)
- oxygen concentrator (1)
- Oxygen Machine (2)
- Pure Oxygen (2)
- albuterol (1)
- Albuterol inhalation (2)
- albuterol sulfate (2)
- Albuterol Sulfate HFA (1)
- Ampules (1)
- Asthma Inhaler (3)
- doctor-only (4)
- HFA Inhaler (1)
- Treat Bronchospasm (1)
- Adult Oxygen (1)
- Air Mask (1)
- Elongated Mask (1)
- Elongated Oxygen Mask (1)
- Hudson Rci (1)
- O2 Mask (2)
- Adult Cannula (1)
- Adult Nasal Cannula (5)
- Breathe (2)
- cannula (4)
- Cannula Needles (1)
- Cannulas (3)
- Chronic Obstructive Pulmonary Disease (1)
- COPD (3)
- emphysema (2)
- Nasal cannula (1)
- Oxygen cannula (1)
- Oxygen delivery (3)
- Respiratory (2)
- Respiratory Therapy (4)
- Soft Nasal Cannula (4)
- Tubing (2)
- Aerosol Mask (1)
- Asthma Treatment (4)
- Hudson RCI (9)
- Micro Mist (1)
- Neb Mask (1)
- Nebulizer Mask (1)
- Nebulizer Treatment (3)
- Asthma treatments (3)
- liquid medication (1)
- Medication Jar (1)
- Micromist (2)
- Mouthpiece (3)
- Neb Kit (2)
- Reservoir Tube (1)
- 1040 (1)
- Adult Oxygen mask (4)
- HUD1040 (1)
- o2 mask (1)
- Amsino Nasal Cannula (1)
- AS75080 (1)
- Green Nasal Cannula (1)
- nasal cannula (4)
- oxygen cannula (4)
- soft tubing (1)
- Compressor Nebulizer (1)
- Neb Machine (1)
- nebulizer (4)
- Nebulizer Compressor (1)
- Nebulizer Machine (2)
- Portable Nebulizer (1)
- Portable nebulizer machine (2)
- Resp-O2 (1)
- Non rebreathing oxygen mask (2)
- Pediatric Oxygen Mask (2)
- asthma (1)
- compressor (1)
- compressor nebulizer (1)
- jet nebulizer (1)
- MedNeb (1)
- MedNeb MQ5600 (1)
- MedNeb nebulizer (1)
- MedNeb nebulizer machine (1)
- neb kit (1)
- neb machine (1)
- nebulizer for adults (1)
- nebulizer treatment (1)
- Pediatric nebulizer (1)
- pediatric nebulizer machine (2)
- piston powered (1)
- tabletop nebulizer (1)
- Mask for Trach (1)
- Trach Mask (1)
- Tracheostomy (1)
- Tracheotomy Mask (1)
- Aerosol Inhaler (1)
- Bronchodilators (1)
- Childrens Nebulizer Machine (2)
- Emergency Medical Supplies (1)
- Inhalation (2)
- inhalation Solution (1)
- Nebulizers (1)
- Proventil Nebules (1)
- Asthma Medication (1)
- Asthma Treatment Inhaler (1)
- Kids Nebulizer (1)
- Mouth Piece (1)
- mouthpieces (1)
- Nebulizer Mouthpiece (1)
- Treat Asthma (1)
- Breathing Exerciser (2)
- COPD Recovery (1)
- Deep Breathing Exercise (1)
- Expand Lungs (1)
- Expiatory Practices (1)
- Incentive spirometer (1)
- Large Volume (1)
- Lung Expansion Device (1)
- Postoperative Care (1)
- Voldyne Incentive Spirometer (1)
- Voldyne Volumetric Exerciser 5000 (1)
- extension tubing (1)
- Green Tubing (1)
- o2 tubing (2)
- oxygen supply (1)
- cardiopulmonary resuscitation (1)
- CPR (1)
- CPR Resuscitation (2)
- Manual Resuscitation (2)
- Narcan (1)
- Pocket Mask (1)
- Resuscitation Mask (1)
- Alpha Beta-Adrenergic Agonist (1)
- chronic bronchitis (2)
- Inhalation Solution (2)
- Levalbuterol (1)
- Levlbutrl (1)
- Ambu Bag (1)
- Lifesaver (1)
- Manual Resuscitation Bag (1)
- Manual Resuscitator (1)
- Allergies (1)
- Asthma Nebulizer (1)
- Asthma Relief Medicine (1)
- Cystic Fibrosis (1)
- Emphysema (1)
- nebulizer compressor (1)
- Treat Emphysema (1)
- extenstion tubing (1)
- Long Oxygen Tubing (1)
- oxygen tube (1)
- star tubing (1)
- Pediatric Breathing Excerciser (1)
- airway device (1)
- Airway obstruction (1)
- Airway Tube (1)
- Clear airways (1)
- Medical suction (1)
- Non vented (1)
- Sterile (1)
- Suction instrument (1)
- Suction tip (1)
- Suction tool (1)
- Yankauer (1)
- Abronchodilator (1)
- Antimuscarinic (1)
- Antispasmodic (1)
- Ipratropium bromide (1)
- Mylan (1)
- Oral Inhalation (1)
- Unit Dose (1)
- 1820 (1)
- Softtech (1)
- y adapter (1)
- y splitter (1)
- Nasal Tube (1)
- Over the Ear (1)
- Oxygen Cannula (2)
- Oxygen Supply (2)
- Bacteria Filter (1)
- bacteria filters (1)
- Cabinet (1)
- Filter Pack (1)
- Filters (1)
- HEPA (1)
- HEPA Capsule (1)
- HEPA Filter (1)
- Intake (1)
- Invacare (1)
- Invacare Platinum (1)
- Oxygen Concentrator Parts (2)
- Replacement Filters (1)
- SP1005 (1)
- Christmas Tree Adaptor (1)
- DISS Outlet Fitting (1)
- Green Connector (1)
- Nipple and Nut (1)
- Tubing connector (3)
- Universal Connector (1)
- Continuous Flow (1)
- Curved Prong (1)
- O2 Cannula (1)
- ear cushions (1)
- ear pads (1)
- ez wraps (1)
- Nasal Cannula with Pads (1)
- Adult Mask (2)
- o2 Mask (1)
- Oxygen Therapy (1)
- blood oxygen level (1)
- led display (1)
- meter pulse (1)
- mq3000 (1)
- pulse oximeter (1)
- pulse oximeterfinger tip (1)
- read pulse (1)
- Spo2 (1)
- take pulse (1)
- Airlife (2)
- Male Connector (1)
- Bubble Humidifier (1)
- High Flow (1)
- Oxygen Bottle (1)
- Barrier Mouth Shiled (1)
- Bulk (1)
- CPR Barrier Mask (1)
- CPR Face Shield (1)
- Mouth to Mouth (1)
- Quicksaver (1)
- Resuscitate (1)
- Revive (1)
- Kids Mask (1)
- Oxygen delivery mask (1)
- non rebreather (1)
- Non Rebreathing (1)
- CareFusion AirLife (1)
- Medium concentration Oxygen Mask (1)
- Aspirator (1)
- Aspirator tubing (1)
- Suction Machine (2)
- Tapered (1)
- Tubing Connector (1)
- Universal connector (1)
- Breathing Mask (1)
- Masks (1)
- oxygen tank (3)
- CO2 Oxygen (1)
- CO₂ (1)
- etco2 (1)
- Luer Lock (1)
- Oxygen Lines (1)
- Sampling tubing (1)
- Simultaneous oxygen delivery (1)
- oxygen tanks (2)
- portable oxygen (2)
- Portable Oxygen Tank (2)
- Replacement Oxygen (1)
- Replacement Tank (1)
- Mucas (1)
- Remove Secrections (1)
- Schuco-Vac 330 (1)
- Emergency Oxygen Tank (1)
- twin pack (1)
Respiratory Supplies
Respiratory Supplies
Respiratory supplies are medical devices and protective equipment used to support breathing and protect the lungs in clinical and industrial settings. These include ventilators (mechanical breathing support machines), oxygen delivery systems (tanks, concentrators and related tubing), positive-airway-pressure devices (CPAP/BiPAP for sleep apnea or acute care), medication delivery devices (nebulizers/inhalers), and personal protective respiratory equipment (masks and respirators). For example, mechanical ventilators “help people breathe when they are unable to do so on their own” by pumping oxygen-rich air into the lungs and maintaining airway pressure to prevent alveoli collapse. Similarly, nebulizers convert liquid medication into an aerosol spray delivered to the lungs, treating disorders like asthma or COPD. Oxygen concentrators and cylinders supply supplemental O₂ for patients with low blood oxygen, and spirometers and sensors monitor lung function. Protective gear includes filtering respirators (e.g. N95/FFP2 masks) which “filter at least 95% of airborne particles” when properly fitted. Table-topping “respiratory consumables” – masks, tubing, filters, valves, etc. – are single-use items needed to connect these devices to patients; many hospitals keep inventories of such consumables for normal operations, but demand can surge in crise.
- Ventilators and BiPAP/CPAP machines: These devices provide assisted ventilation. Invasive ventilators use an endotracheal tube, while non-invasive ventilators and CPAP/BiPAP use masks. Modern ventilators have modes (volume/pressure control, high-frequency ventilation, etc.) tailored to patient needs. CPAP machines deliver continuous positive airway pressure for sleep apnea or emergency support, adjusting pressure in response to breathing patterns.
- Oxygen delivery: Oxygen is delivered via cylinders or concentrators to patients with respiratory failure or chronic hypoxia. Devices like high-flow nasal cannula deliver warmed/humidified oxygen at high flow rates (up to 60–70 L/min) while allowing patient mobility. Accessories include flow regulators, humidifiers, masks, and cannulae.
- Medication delivery devices: Nebulizers and metered-dose inhalers generate aerosolized drugs. For instance, nebulizers “deliver aerosolized medications directly to the lungs” and are essential for treating asthma, COPD, pneumonia, etc.. Spacer chambers and masks are used for bronchodilators and steroids.
- Respiratory protective equipment (RPE): This category covers masks and respirators worn by healthcare workers and others to filter pathogens or particulates. An N95 respirator (NIOSH-approved) tightly seals the face and captures ≥95% of airborne particles. Surgical masks (looser fitting) protect against droplets but are not considered respirators. Powered air-purifying respirators (PAPRs) and elastomeric reusable respirators are also used in high-risk settings. RPE components include filter cartridges and face seals.
-
Consumables and accessories: Tubing, connectors, humidification chambers, endotracheal tubes, mask interfaces, and filters are needed to run ventilators and nebulizers. These are often single-use. For example, a hospital’s respiratory therapy department maintains stock of items like ventilator circuits and CPAP tubing. (Hospitals often list suppliers for these parts to avoid shortages.
Respiratory supplies are critical in many settings: intensive care units (for ARDS and other acute illnesses), emergency medicine, chronic care (COPD, sleep apnea), home care, and occupational safety (e.g. construction, labs). During the COVID-19 pandemic, demand for these supplies exploded. For example, one analysis notes that COVID-related border closures and factory shutdowns turned “PPE, ventilators and associated [respiratory] consumables” into “scarce resources”. A surge in cases led to many countries facing oxygen and ventilator shortages, straining global supply chains. Acute respiratory distress syndrome (ARDS) in COVID patients “commonly requires ventilation support,” which further strained supply – outsourcing ventilator production overseas created a market that was “depleted of supplies that were previously made on a demand basis”. Even normally adequate hospital inventories were swamped by the surge.
Supply chains for respiratory equipment are complex and internationalized. The OECD reports that global trade in medical devices (including respiratory devices) has grown dramatically – roughly 7-fold over the past 30 years, “reaching a total of USD 700 billion in 2022”. While globalization has increased availability, it also means many critical components (e.g. melt-blown filter fabric for N95 masks) come from concentrated regions, creating vulnerability to regional disruptions. In response to past crises, many governments and organizations have bolstered strategic stockpiles of ventilators, oxygen generators, and respirators. For instance, investments in domestic manufacturing (e.g. N95 production facilities) and nimble procurement have been prioritized to build resilience.
The respiratory supplies market is sizable and growing. The global respiratory protection equipment (RPE) market was about US$9.7 billion in 2022 and is forecast to exceed $13.8 billion by 2027. Major PPE manufacturers include 3M, Honeywell, DuPont, Ansell, and Drägerwerk. Similarly, the mechanical ventilator market (ICU and portable ventilators) is valued in the billions (over $1.1 billion in 2024) with major vendors like GE Healthcare, Philips, Draeger, Medtronic, and Fisher & Paykel. The sleep-apnea/CPAP device market is also large (multibillion-dollar globally) driven by prevalence of sleep disorders. Demand is fueled by an aging population and rising prevalence of respiratory diseases.
Current challenges and trends: Supply chains remain a focus of improvement. Efforts include better visibility of inventory, flexible “just-in-case” manufacturing, and international coordination to avoid shortages. Research into new materials and designs (e.g. reuseable elastomeric masks, advanced HEPA filters) is ongoing to balance protection, cost, and sustainability. Digital health integration (smart ventilators/CPAP with remote monitoring) is growing. Meanwhile, guidelines (from CDC/OSHA/NIOSH/WHO) continue to define performance standards – for example, requiring fit testing for N95 respirators to ensure the claimed high filtration efficiency.
In summary, respiratory supplies encompass a wide range of life-support and protective equipment essential for treating and preventing lung problems. Their use spans critical care (ventilators, oxygen), chronic therapy (CPAP, inhalers), and infection control (masks, respirators). The COVID-19 pandemic underscored their importance and the need for robust manufacturing and supply strategies. As healthcare demand grows worldwide, the respiratory supplies sector continues to expand, driven by both medical needs and technological innovation.
Purpose
- Support Healthy Breathing: Deliver oxygen, medication, or humidity to patients with respiratory compromise.
- Manage Chronic Lung Disease: Provide consistent therapy and symptom relief for asthma, chronic bronchitis, COPD, and cystic fibrosis.
- Enable Airway Clearance: Aid in mucus removal, infection control, and post-surgical pulmonary hygiene.
- Emergency & Critical Care: Provide life-saving oxygen, airway management, and acute bronchodilator therapy in urgent settings.
Uses
- Asthma & COPD Management: Daily inhaler/nebulizer therapy, peak flow monitoring, oxygen supplementation.
- Oxygen Therapy: Continuous or pulse oxygen delivery for hypoxemic adults and children, sleep apnea, or home ventilator care.
- Nebulization: Administration of bronchodilators, corticosteroids, antibiotics, and saline for airway disorders or acute symptoms.
- Post-Surgical, ICU & Emergency Care: Supplemental O2, ventilation, chest physiotherapy after surgeries or in critical illness.
- Pediatric Care: Special size masks, spacers, and humidifiers for children with acute bronchiolitis or asthma.
- Infection Control: Disposable masks, viral filters, and airway hygiene products during flu, COVID-19, pneumonia, and TB outbreaks.
Types of Respiratory Supples
- Nebulizers: Compressor, ultrasonic, mesh; handheld, tabletop, portable
- Inhalers: Metered-dose inhalers (MDI), dry powder inhalers (DPI), soft-mist inhalers
- Oxygen Concentrators & Cylinders: Stationary/home, portable, travel options
- Oxygen Masks, Nasal Cannulas, Reservoir Bags: Adult and pediatric sizes
- CPAP, BiPAP, & Ventilator Supplies: Masks, hoses, filters, humidifiers
- Peak Flow Meters, Spirometers, Pulse Oximeters: Home and professional monitoring
- Tracheostomy Supplies: Tracheostomy tubes, speaking valves, suction catheters
- Resuscitation Bags (BVM), Manual & AED Respiratory Kits
- Suction Machines, Chest Physiotherapy Devices, Incentive Spirometers
- Heat Moisture Exchange Filters (HME), Bacterial/Viral Filters
- Airway Clearance Therapy (vibratory PEP, oscillating devices)
Popular Brands:
- Philips Respironics
- ResMed
- Medline
- Pari
- Drive Medical
- DeVilbiss Healthcare
- Baxter
- 3B Medical
- Invacare
- Sunset Healthcare
- Pulmodyne
- Smiths Medical
- Teleflex
- Hudson RCI
- Omron
- Mallinckrodt
- Salter Labs
- Covidien (Medtronic)
- Fisher & Paykel Healthcare
Trusted by clinics, hospitals, and families worldwide for safe asthma care, COPD therapy, oxygen delivery, recovery, and emergency breathing support. Shop leading brands and all types, from nebulizers and inhalers to oxygen concentrators, masks, and pulse oximeters—order now for guaranteed quality, rapid shipping, and reliable care for every respiratory need!
-
 Sale 20%
Original price $ 875.00Current price $ 699.99
Sale 20%
Original price $ 875.00Current price $ 699.99Home Oxygen Concentrator Machine 5 Liter for COPD, Sleep Apnea, Respiratory Care
No reviewsBreathe Easy with Confidence: The Dynarex Home Oxygen Concentrator Machine 5 Liter delivers powerful and consistent medical-grade oxygen therapy fr...
View full details -
 Sale 13%
Original price $ 79.00Current price $ 68.85
Sale 13%
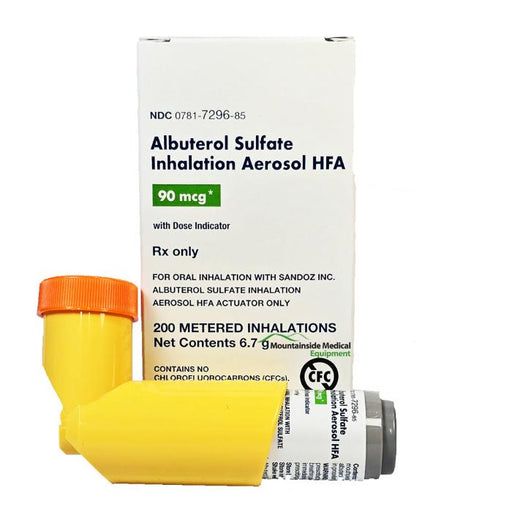
Original price $ 79.00Current price $ 68.85Albuterol Sulfate Inhaler Aerosol HFA 90 mcg 200 Metered Inhalations (RX)
2 reviewsAlbuterol Sulfate Inhaler Aerosol HFA 90 mcg is used to relieve bronchospasm in individuals with reversible obstructive airway diseases, such as as...
View full details🔒 Medical License Required -
 Sale 30%
Original price $ 1.79Current price $ 1.26
Sale 30%
Original price $ 1.79Current price $ 1.26Adult Oxygen Mask with 7 Foot tubing Elongated
24 reviewsAdult Oxygen Mask is a clear, elongated adult oxygen mask used to supply therapeutic oxygen to a person with a respiratory illness. The medium conc...
View full details -
 Sale 38%
Original price $ 1.05Current price $ 0.65
Sale 38%
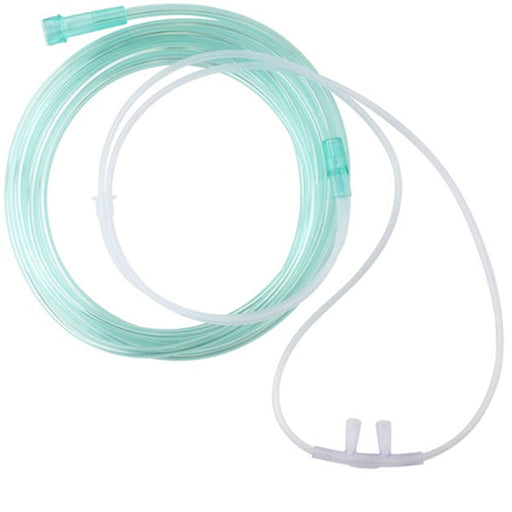
Original price $ 1.05Current price $ 0.65Oxygen Nasal Cannula Adult Size with 7 Foot Tubing
10 reviewsA Nasal Cannula is a medical device used to deliver supplemental oxygen to patients. It features two prongs that fit into the nostrils, connected t...
View full details -
 Sale 35%
Original price $ 3.95Current price $ 2.55
Sale 35%
Original price $ 3.95Current price $ 2.55Nebulizer Mask Micro Mist Elongated Shape, Adult Size with 7 foot Tubing
73 reviewsNebulizer Mask is a clear aerosol mask used to transfer medication in a fine mist to people that have respiratory illnesses. This mask includes 7 f...
View full details -
 Sale 3%
Original price $ 1.95Current price $ 1.89
Sale 3%
Original price $ 1.95Current price $ 1.89Nebulizer Treatment Kit with Mouthpiece and Reservoir Tube
33 reviewsMicro Mist Nebulizer kit used to deliver liquid medication for breathing treatments. Each nebulizer kit is latex free and includes a nebulizer cup,...
View full details -
 Sale
$ 6.50
Sale
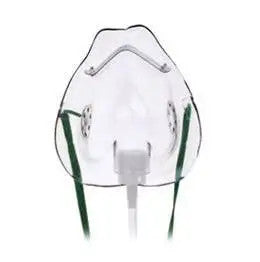
$ 6.50Oxygen Mask, Adult with 7 foot Tubing
6 reviewsHudson RCI 1040 Adult Oxygen Mask is a comfortable and efficient oxygen delivery mask for respiratory patients. This oxygen mask features a medium-...
View full details -
 Sale 15%
Original price $ 1.29Current price $ 1.10
Sale 15%
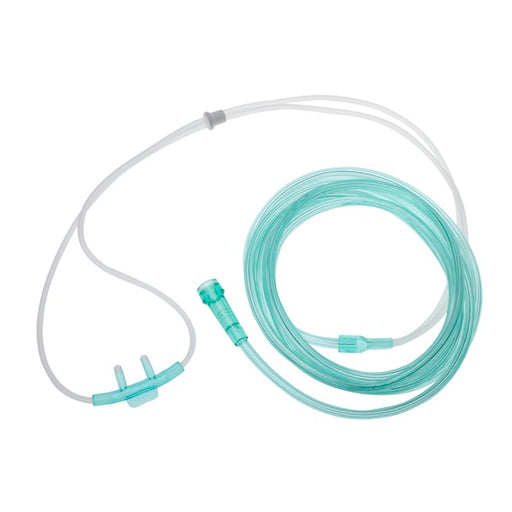
Original price $ 1.29Current price $ 1.10Oxygen Nasal Cannula (Light Green Color) with Super Soft 7 foot Tubing
55 reviewsAn Oxygen Nasal Cannula is a small tube-like device used to deliver supplemental oxygen to people who can benefit from increased oxygen levels. It ...
View full details -
 Sale 31%
Original price $ 39.95Current price $ 27.70
Sale 31%
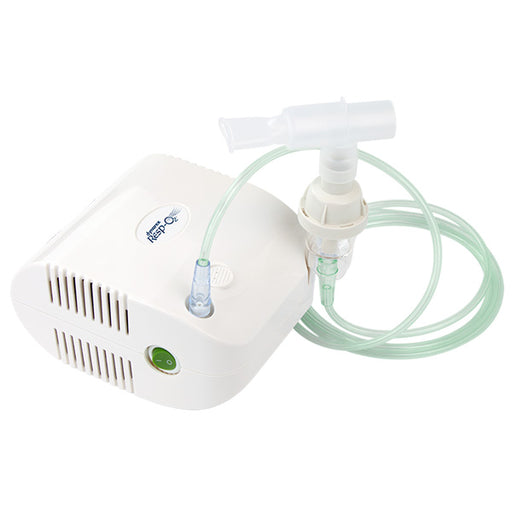
Original price $ 39.95Current price $ 27.70Nebulizer Machine Compressor for Respiratory Therapy
103 reviewsThe Ultra light portable nebulizer machine compressor is highly effective for respiratory treatments related to asthma, allergies, and a variety of...
View full details -
 Sale 46%
Original price $ 2.59Current price $ 1.40
Sale 46%
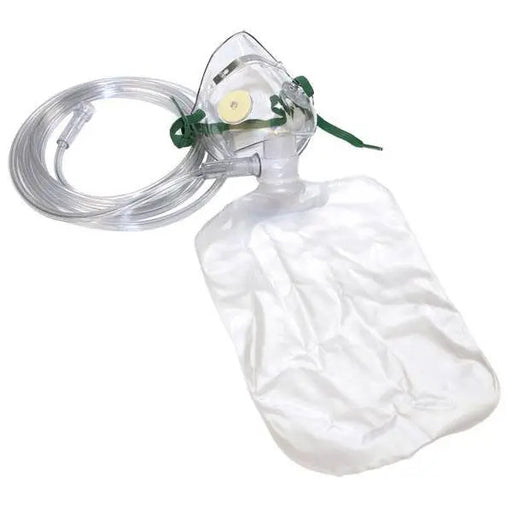
Original price $ 2.59Current price $ 1.40Pediatric Oxygen Mask Non-Rebreather Style with 7 foot tubing and Safety Vent
3 reviewsDynarex Pediatric Oxygen Mask with Non Rebreather Bag is specifically designed to provide high-concentration oxygen delivery to pediatric patients....
View full details -
 Sale 35%
Original price $ 57.95Current price $ 37.95
Sale 35%
Original price $ 57.95Current price $ 37.95Nebulizer Machine For Adults & Kids for COPD & Asthma Relief
106 reviewsNebulizer Machine MedNeb MQ5600 A nebulizer is a small medical device that turns liquid medication into a breathable mist that enters the lungs. Th...
View full details -
 Sale 40%
Original price $ 2.99Current price $ 1.79
Sale 40%
Original price $ 2.99Current price $ 1.79Tracheostomy Mask, Adult
2 reviewsA Tracheotomy Mask is a medical device specifically designed for those who need additional oxygen. These masks provide a safe and secure seal over ...
View full details -
 Sale 38%
Original price $ 29.95Current price $ 18.50
Sale 38%
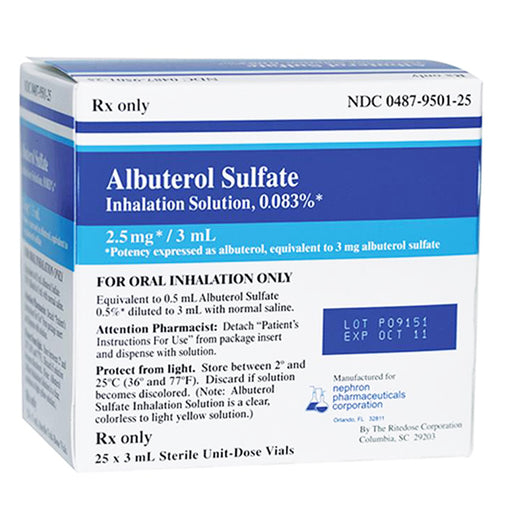
Original price $ 29.95Current price $ 18.50Albuterol Sulfate 0.083% Inhalation Nebulizer Solution 2.5 mg/3 ml by Ritedose 25/Box (Rx)
96 reviewsFast-Acting Relief for Asthma, COPD, and Bronchospasm – Professional-Grade Albuterol Nebulizer Solution Breathe easier and faster with Albuterol Su...
View full details🔒 Medical License Required -
 Sale 23%
Original price $ 2.95Current price $ 2.27
Sale 23%
Original price $ 2.95Current price $ 2.27MicroMist Nebulizer Kit with Mouthpiece, Med cup and Tubing
74 reviewsTeleflex Micro Mist Nebulizer Kit 1882 with med cup, tubing and Mouthpiece. Made to transfer liquid asthma medications into a fine micro mist aero...
View full details -
 Sale 20%
Original price $ 9.95Current price $ 7.99
Sale 20%
Original price $ 9.95Current price $ 7.99Voldyne Incentive Spirometer Breathing Exerciser 4000 mL
4 reviewsTake control of your respiratory health with the Voldyne Incentive Spirometer Breathing Exerciser 4000 mL by Medline. Specifically engineered for e...
View full details -
 Sale 29%
Original price $ 0.79Current price $ 0.56
Sale 29%
Original price $ 0.79Current price $ 0.56Oxygen Supply Extension Tubing 7 Foot
15 reviewsOxygen tubing is a clear supply tubing used to deliver therapeutic oxygen to a patients airways. Made with a 5-channel star interior to prevent oxy...
View full details -
 Sale 35%
Original price $ 11.95Current price $ 7.80
Sale 35%
Original price $ 11.95Current price $ 7.80CPR Mask with 1 Way Valve, Orange Case (Fits Adult & Pediatric Patents)
10 reviewsCPR Mask with Hard Case is pocket-sized resuscitator mask made with a high-efficiency and low resistance one-way valve to help minimize the possibi...
View full details -
 Sale 29%
Original price $ 59.95Current price $ 42.80
Sale 29%
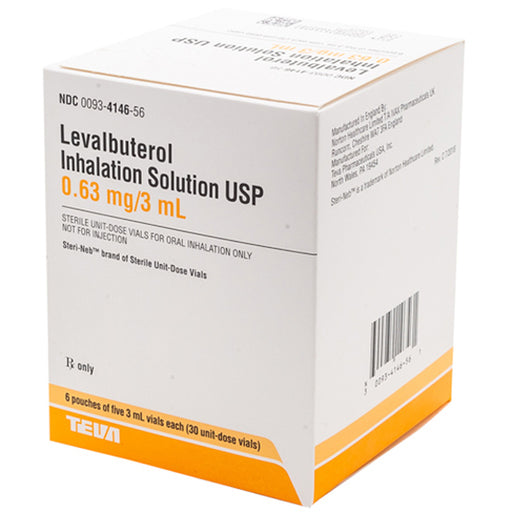
Original price $ 59.95Current price $ 42.80Levalbuterol Inhalation Solution 0.63mg Nebulizer Vial 3 mL x 30/Box - Teva (Rx)
No reviewsLevalbuterol inhalation solution 0.63mg treats and prevents bronchospasm in adults and children 4 years of age and older with reversible obstructiv...
View full details🔒 Medical License Required -
 Sale
$ 43.00
Sale
$ 43.00LifeSaver Bag Valve Mask Adult Resuscitation Bag
15 reviewsManual Resuscitation Bags are an essential tool in first aid and emergency response. They are devices which allow for manual ventilation and oxygen...
View full details -
 Sale 32%
Original price $ 49.95Current price $ 33.95
Sale 32%
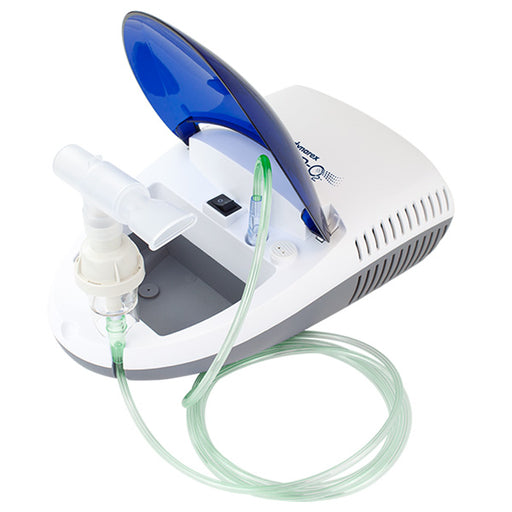
Original price $ 49.95Current price $ 33.95Elite Nebulizer Machine with Mask & Mouthpiece Included
22 reviewsDynarex Elite Nebulizer Machine is used for the treatment of: bronchial asthma, acute bronchitis, emphysema, cystic fibrosis, COPD, tracheitis, pul...
View full details -
 Sale 37%
Original price $ 2.95Current price $ 1.85
Sale 37%
Original price $ 2.95Current price $ 1.85Oxygen Tubing 25 Foot Length
20 reviewsOxygen Extension Tubing 25 Foot Length is a star-lumen tubing used with oxygen concentrators, oxygen masks and nasal cannulas to add extra length. ...
View full details -
 Sale 34%
Original price $ 13.00Current price $ 8.60
Sale 34%
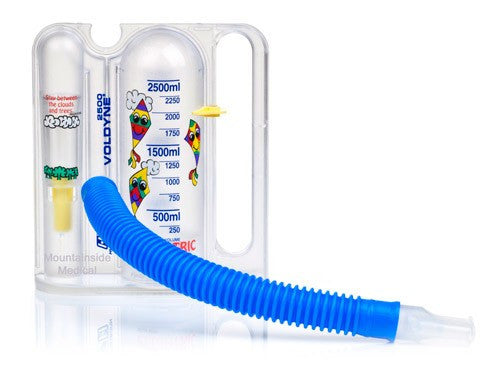
Original price $ 13.00Current price $ 8.60Pediatric Voldyne Volumetric Incentive Spirometer Breathing Exerciser 2500ml
1 reviewPediatric Voldyne Volumetric Exerciser 2500 mL is specifically designed for children, and is used for exercising the lungs and increasing the amou...
View full details -
 Sale 32%
Original price $ 0.95Current price $ 0.65
Sale 32%
Original price $ 0.95Current price $ 0.65Yankauer Suction Tube Handle, Sterile
12 reviewsYankauer Suction A Yankauer is a rigid, curved suction tip (often called a “tonsil tip”) connected to a suction machine. It’s designed for orophary...
View full details -
 Sale 22%
Original price $ 35.80Current price $ 27.95
Sale 22%
Original price $ 35.80Current price $ 27.95Ipratropium Bromide 0.02% Inhalation Solution 0.5 mg Per 2.5 mL Vials, 30 Count (Rx)
No reviewsIpratropium Bromide Inhalation Solution 0.02% is a bronchodilator used to treat respiratory conditions such as chronic obstructive pulmonary diseas...
View full details🔒 Medical License Required -
 Sale 27%
Original price $ 67.00Current price $ 49.00
Sale 27%
Original price $ 67.00Current price $ 49.00Soft-Touch Nasal Cannula with 7 Foot Star Lumen Tubing, 50/case
27 reviewsSoft-Touch Nasal Cannula is designed for superior fit and comfort. Made with extra soft tubing, this cannula features an over-the-ear design, a sta...
View full details -
 Sale
$ 2.49
Sale
$ 2.49Kink-Free Swivel Oxygen Tubing Connector w/ Security Clip, White
17 reviewsSalter Labs 1220-0 Kink-Free Swivel Oxygen Tubing Connector with Security Clip is designed to eliminate the tangling, twisting, and kinking of oxyg...
View full details -
 Sale
$ 1.89
Sale
$ 1.89Y Connector for Oxygen Tubing
7 reviewsUniversal Y Connector to Spilt Oxygen Lines 1/4” and 3/8” sizes are unique oxygen connectors used to spilt oxygen lines from tanks and concentrator...
View full details -
 Sale 34%
Original price $ 2.10Current price $ 1.39
Sale 34%
Original price $ 2.10Current price $ 1.39Over the Ear Nasal Cannula with 7 Foot Tubing
13 reviewsOver-the-Ear 1103 Nasal Cannulas by Hudson RCI is a soft, comfortable cannulas made for the delivery of oxygen. Complete with Hudson's over-the-ear...
View full details -
 Sale 27%
Original price $ 19.95Current price $ 14.50
Sale 27%
Original price $ 19.95Current price $ 14.50Hepa Filter for Invacare Platinum 5 and 10 Liter Oxygen Concentrators
7 reviewsThe HEPA filter for Invacare Platinum 5 and 10 Liter Oxygen Concentrators is designed to provide enhanced air purification by trapping airborne par...
View full details -
 Sale 42%
Original price $ 1.19Current price $ 0.69
Sale 42%
Original price $ 1.19Current price $ 0.69Nut and Nipple Universal Oxygen Adapter, Green Christmas Tree
7 reviewsOxygen Concentrator Tubing Adaptor for DISS Outlet Fitting is a barbed oxygen concentrator adaptor made with a hex screw used to connect oxygen tub...
View full details -
 Sale 46%
Original price $ 2.35Current price $ 1.28
Sale 46%
Original price $ 2.35Current price $ 1.28Nasal Cannula with Curved Nasal Prongs with 7 Foot Tubing
15 reviewsThe Hudson RCI 1104 Nasal Cannula with Curved Nasal Prongs with 7 Foot Tubing is a great consumable product meant for single-patient use is designe...
View full details -
 Sale 55%
Original price $ 0.87Current price $ 0.39
Sale 55%
Original price $ 0.87Current price $ 0.39Treaded Oxygen Tubing Connector
10 reviewsTreaded Oxygen Tubing Connector is double-male end connector used with nasal cannulas, oxygen masks and other respiratory devices. Unique design, a...
View full details -
 Sale 33%
Original price $ 2.89Current price $ 1.95
Sale 33%
Original price $ 2.89Current price $ 1.95Salter Labs 1600TLC Nasal Cannula with Ear Cushion Pads Sun Med
13 reviewsThe Salter Labs 1600TLC-7 Nasal Cannula with Ear Cushion Pads are ideal for use with patients requiring supplemental oxygen for increased levels of...
View full details -
 Sale 16%
Original price $ 1.65Current price $ 1.39
Sale 16%
Original price $ 1.65Current price $ 1.39Oxygen Mask, Adult with 7 foot Tubing
6 reviewsAdult Vinyl Oxygen Mask 7 ft, Medium Concentration, Latex-free, is a disposable o2 mask used for oxygen delivery to a patient. This oxygen mask fea...
View full details -
 Sale 33%
Original price $ 5.95Current price $ 3.98
Sale 33%
Original price $ 5.95Current price $ 3.98CareFusion AirLife™ Inline Water Trap
9 reviewsInline Water Trap that catches moisture between bubble humidifier bottles before getting to patients nasal cannula or oxygen make. Ideal for patien...
View full details -
 Sale 41%
Original price $ 1.05Current price $ 0.62
Sale 41%
Original price $ 1.05Current price $ 0.62Nasal Cannula with 7 foot Oxygen Tubing, Dynarex
6 reviewsA Nasal Cannula with 7-foot Oxygen Tubing is used to deliver supplemental oxygen to patients with respiratory conditions. It features prongs that f...
View full details -
 Sale 27%
Original price $ 49.00Current price $ 35.90
Sale 27%
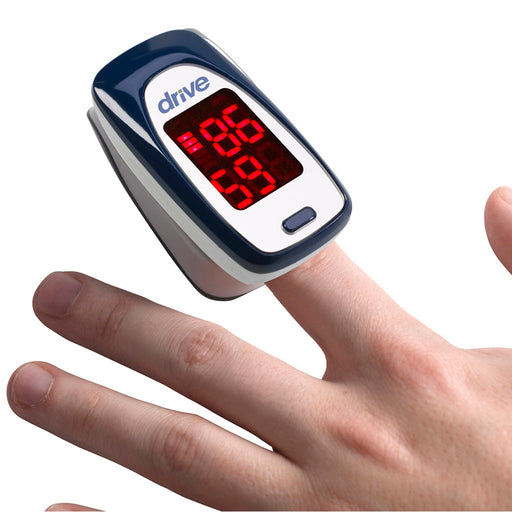
Original price $ 49.00Current price $ 35.90Finger Pulse Oximeter Easy-Slide
6 reviewsMQ3000 Finger Pulse Oximeter is a non-invasive spot-check fingertip pulse oximeter. Made to accommodates a wide range of finger sizes for pediatric...
View full details -
 Sale 52%
Original price $ 3.95Current price $ 1.90
Sale 52%
Original price $ 3.95Current price $ 1.90Oxygen Tubing Connector, White - Pack of 5
2 reviewsAirLife Oxygen Tubing Connectors are designed to connect tubing with a diameter between 5 mm and 7 mm. Each O2 connector is disposable and latex f...
View full details -
 Sale
$ 5.35
Sale
$ 5.35Salter Labs High Flow Bubble Humidifier Bottle 6 to 15 LPM with 6 PSI
2 reviewsSalter labs High Flow Humidifier Bottle is a oxygen mist water bottle that works with high capacity output oxygen concentrators and devices. High f...
View full details -
 Sale 34%
Original price $ 1.29Current price $ 0.85
Sale 34%
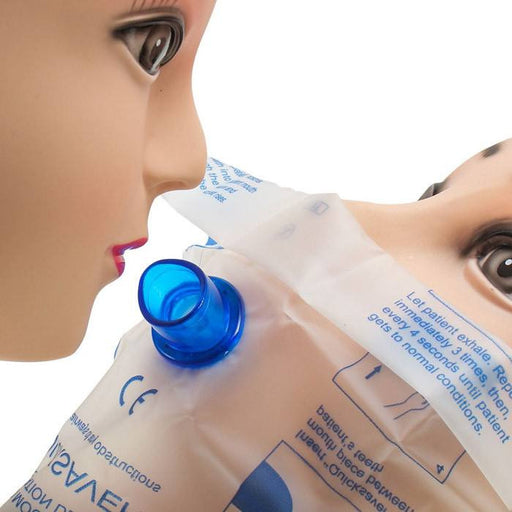
Original price $ 1.29Current price $ 0.85QuickSaver CPR Face Shield Barrier
18 reviewsCPR Mask - QuickSaver CPR Face Shields bulk barrier for mouth to mouth resuscitation and saves you from coming in direct contact with the individua...
View full details -
 Sale 25%
Original price $ 2.59Current price $ 1.94
Sale 25%
Original price $ 2.59Current price $ 1.94Pediatric Oxygen Mask with 7 Foot Tubing
2 reviewsKids Pediatric Oxygen Mask is a soft, medium concentration supply mask with 7 foot tubing that delivers therapeutic oxygen to children with respira...
View full details -
 Sale
$ 4.95
Sale
$ 4.95Elongated Non Rebreathing Oxygen Mask SunMed Salter Labs
2 reviewsSalter Labs 8130 Elongated Non-Rebreathing Mask is an oxygen mask, designed for high-concentration oxygen delivery. This non-rebreathing oxygen mas...
View full details -
 Sold out
Original price $ 1.29Current price $ 0.79
Sold out
Original price $ 1.29Current price $ 0.79Oxygen Mask, Adult Elongated with 7 Foot Tubing
3 reviewsDynarex disposable oxygen mask has a soft vinyl plastic that conforms and contours to the shape of your face. Made with latex free materials for pe...
View full details -
 Sale 38%
Original price $ 1.59Current price $ 0.98
Sale 38%
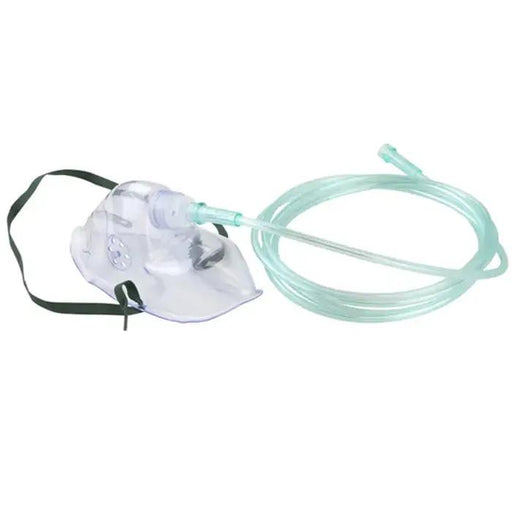
Original price $ 1.59Current price $ 0.98Oxygen Mask, Adult Elongated with 7 foot Tubing
3 reviewsDynarex Adult Oxygen Mask is an effective method for medium concentration delivery of oxygen to respiratory patients. This oxygen mask features hig...
View full details -
 Sale 41%
Original price $ 0.59Current price $ 0.35
Sale 41%
Original price $ 0.59Current price $ 0.35Universal Tubing Connector 5-in-1
2 reviews5-in-1 Universal Medical Tubing Connector is designed for use for oxygen therapy tubing, aspirator suction machine tubing and other medical devices...
View full details -
 Sale 28%
Original price $ 1.95Current price $ 1.40
Sale 28%
Original price $ 1.95Current price $ 1.40Non-Rebreather Oxygen Mask, Elongated Shape, Adult Size with 7 foot Tubing & Safety Vent
4 reviewsNon-Rebreathing Oxygen Masks are used to deliver high concentrations of oxygen to patients in need of significant respiratory support. They feature...
View full details -
 Sale 38%
Original price $ 6.95Current price $ 4.29
Sale 38%
Original price $ 6.95Current price $ 4.29Nasal Cannula ETCO2 Sampling Simultaneous O2 CO2 & O2 Lines, 3 Channel Safety Tubing 10' Length
3 reviewsThe ETCO₂ Nasal Sampling Cannula with O₂ Delivery is designed for precise, continuous respiratory monitoring and effective oxygen therapy in adult ...
View full details -
 Sold out
Original price $ 149.95Current price $ 119.00
Sold out
Original price $ 149.95Current price $ 119.00Replacement Oxygen Tank for Allied Healthcare Lif-O-Gen System
No reviewsAllied Healthcare Lif-O-Gen Replacement Oxygen tank cylinders for the EmergencyOxygen Kit. This tank is lightweight and can help you make sure you ...
View full details
People Also Searched For
Respiratory Supplies
Respiratory supplies are medical devices and protective equipment used to support breathing and protect the lungs in clinical and industrial settings. These include ventilators (mechanical breathing support machines), oxygen delivery systems (tanks, concentrators and related tubing), positive-airway-pressure devices (CPAP/BiPAP for sleep apnea or acute care), medication delivery devices (nebulizers/inhalers), and personal protective respiratory equipment (masks and respirators). For example, mechanical ventilators “help people breathe when they are unable to do so on their own” by pumping oxygen-rich air into the lungs and maintaining airway pressure to prevent alveoli collapse. Similarly, nebulizers convert liquid medication into an aerosol spray delivered to the lungs, treating disorders like asthma or COPD. Oxygen concentrators and cylinders supply supplemental O₂ for patients with low blood oxygen, and spirometers and sensors monitor lung function. Protective gear includes filtering respirators (e.g. N95/FFP2 masks) which “filter at least 95% of airborne particles” when properly fitted. Table-topping “respiratory consumables” – masks, tubing, filters, valves, etc. – are single-use items needed to connect these devices to patients; many hospitals keep inventories of such consumables for normal operations, but demand can surge in crise.
- Ventilators and BiPAP/CPAP machines: These devices provide assisted ventilation. Invasive ventilators use an endotracheal tube, while non-invasive ventilators and CPAP/BiPAP use masks. Modern ventilators have modes (volume/pressure control, high-frequency ventilation, etc.) tailored to patient needs. CPAP machines deliver continuous positive airway pressure for sleep apnea or emergency support, adjusting pressure in response to breathing patterns.
- Oxygen delivery: Oxygen is delivered via cylinders or concentrators to patients with respiratory failure or chronic hypoxia. Devices like high-flow nasal cannula deliver warmed/humidified oxygen at high flow rates (up to 60–70 L/min) while allowing patient mobility. Accessories include flow regulators, humidifiers, masks, and cannulae.
- Medication delivery devices: Nebulizers and metered-dose inhalers generate aerosolized drugs. For instance, nebulizers “deliver aerosolized medications directly to the lungs” and are essential for treating asthma, COPD, pneumonia, etc.. Spacer chambers and masks are used for bronchodilators and steroids.
- Respiratory protective equipment (RPE): This category covers masks and respirators worn by healthcare workers and others to filter pathogens or particulates. An N95 respirator (NIOSH-approved) tightly seals the face and captures ≥95% of airborne particles. Surgical masks (looser fitting) protect against droplets but are not considered respirators. Powered air-purifying respirators (PAPRs) and elastomeric reusable respirators are also used in high-risk settings. RPE components include filter cartridges and face seals.
-
Consumables and accessories: Tubing, connectors, humidification chambers, endotracheal tubes, mask interfaces, and filters are needed to run ventilators and nebulizers. These are often single-use. For example, a hospital’s respiratory therapy department maintains stock of items like ventilator circuits and CPAP tubing. (Hospitals often list suppliers for these parts to avoid shortages.
Respiratory supplies are critical in many settings: intensive care units (for ARDS and other acute illnesses), emergency medicine, chronic care (COPD, sleep apnea), home care, and occupational safety (e.g. construction, labs). During the COVID-19 pandemic, demand for these supplies exploded. For example, one analysis notes that COVID-related border closures and factory shutdowns turned “PPE, ventilators and associated [respiratory] consumables” into “scarce resources”. A surge in cases led to many countries facing oxygen and ventilator shortages, straining global supply chains. Acute respiratory distress syndrome (ARDS) in COVID patients “commonly requires ventilation support,” which further strained supply – outsourcing ventilator production overseas created a market that was “depleted of supplies that were previously made on a demand basis”. Even normally adequate hospital inventories were swamped by the surge.
Supply chains for respiratory equipment are complex and internationalized. The OECD reports that global trade in medical devices (including respiratory devices) has grown dramatically – roughly 7-fold over the past 30 years, “reaching a total of USD 700 billion in 2022”. While globalization has increased availability, it also means many critical components (e.g. melt-blown filter fabric for N95 masks) come from concentrated regions, creating vulnerability to regional disruptions. In response to past crises, many governments and organizations have bolstered strategic stockpiles of ventilators, oxygen generators, and respirators. For instance, investments in domestic manufacturing (e.g. N95 production facilities) and nimble procurement have been prioritized to build resilience.
The respiratory supplies market is sizable and growing. The global respiratory protection equipment (RPE) market was about US$9.7 billion in 2022 and is forecast to exceed $13.8 billion by 2027. Major PPE manufacturers include 3M, Honeywell, DuPont, Ansell, and Drägerwerk. Similarly, the mechanical ventilator market (ICU and portable ventilators) is valued in the billions (over $1.1 billion in 2024) with major vendors like GE Healthcare, Philips, Draeger, Medtronic, and Fisher & Paykel. The sleep-apnea/CPAP device market is also large (multibillion-dollar globally) driven by prevalence of sleep disorders. Demand is fueled by an aging population and rising prevalence of respiratory diseases.
Current challenges and trends: Supply chains remain a focus of improvement. Efforts include better visibility of inventory, flexible “just-in-case” manufacturing, and international coordination to avoid shortages. Research into new materials and designs (e.g. reuseable elastomeric masks, advanced HEPA filters) is ongoing to balance protection, cost, and sustainability. Digital health integration (smart ventilators/CPAP with remote monitoring) is growing. Meanwhile, guidelines (from CDC/OSHA/NIOSH/WHO) continue to define performance standards – for example, requiring fit testing for N95 respirators to ensure the claimed high filtration efficiency.
In summary, respiratory supplies encompass a wide range of life-support and protective equipment essential for treating and preventing lung problems. Their use spans critical care (ventilators, oxygen), chronic therapy (CPAP, inhalers), and infection control (masks, respirators). The COVID-19 pandemic underscored their importance and the need for robust manufacturing and supply strategies. As healthcare demand grows worldwide, the respiratory supplies sector continues to expand, driven by both medical needs and technological innovation.
Purpose
- Support Healthy Breathing: Deliver oxygen, medication, or humidity to patients with respiratory compromise.
- Manage Chronic Lung Disease: Provide consistent therapy and symptom relief for asthma, chronic bronchitis, COPD, and cystic fibrosis.
- Enable Airway Clearance: Aid in mucus removal, infection control, and post-surgical pulmonary hygiene.
- Emergency & Critical Care: Provide life-saving oxygen, airway management, and acute bronchodilator therapy in urgent settings.
Uses
- Asthma & COPD Management: Daily inhaler/nebulizer therapy, peak flow monitoring, oxygen supplementation.
- Oxygen Therapy: Continuous or pulse oxygen delivery for hypoxemic adults and children, sleep apnea, or home ventilator care.
- Nebulization: Administration of bronchodilators, corticosteroids, antibiotics, and saline for airway disorders or acute symptoms.
- Post-Surgical, ICU & Emergency Care: Supplemental O2, ventilation, chest physiotherapy after surgeries or in critical illness.
- Pediatric Care: Special size masks, spacers, and humidifiers for children with acute bronchiolitis or asthma.
- Infection Control: Disposable masks, viral filters, and airway hygiene products during flu, COVID-19, pneumonia, and TB outbreaks.
Types of Respiratory Supples
- Nebulizers: Compressor, ultrasonic, mesh; handheld, tabletop, portable
- Inhalers: Metered-dose inhalers (MDI), dry powder inhalers (DPI), soft-mist inhalers
- Oxygen Concentrators & Cylinders: Stationary/home, portable, travel options
- Oxygen Masks, Nasal Cannulas, Reservoir Bags: Adult and pediatric sizes
- CPAP, BiPAP, & Ventilator Supplies: Masks, hoses, filters, humidifiers
- Peak Flow Meters, Spirometers, Pulse Oximeters: Home and professional monitoring
- Tracheostomy Supplies: Tracheostomy tubes, speaking valves, suction catheters
- Resuscitation Bags (BVM), Manual & AED Respiratory Kits
- Suction Machines, Chest Physiotherapy Devices, Incentive Spirometers
- Heat Moisture Exchange Filters (HME), Bacterial/Viral Filters
- Airway Clearance Therapy (vibratory PEP, oscillating devices)
Popular Brands:
- Philips Respironics
- ResMed
- Medline
- Pari
- Drive Medical
- DeVilbiss Healthcare
- Baxter
- 3B Medical
- Invacare
- Sunset Healthcare
- Pulmodyne
- Smiths Medical
- Teleflex
- Hudson RCI
- Omron
- Mallinckrodt
- Salter Labs
- Covidien (Medtronic)
- Fisher & Paykel Healthcare
Trusted by clinics, hospitals, and families worldwide for safe asthma care, COPD therapy, oxygen delivery, recovery, and emergency breathing support. Shop leading brands and all types, from nebulizers and inhalers to oxygen concentrators, masks, and pulse oximeters—order now for guaranteed quality, rapid shipping, and reliable care for every respiratory need!
Common Types of Respiratory Supplies
-
Ventilators: Mechanical breathing machines that move air in and out of the lungs for a patient. Ventilators can fully or partially take over the work of breathing for someone who is unable to breathe adequately on their own. They are commonly used in critical care settings (and sometimes for home care) to deliver life-sustaining breaths to patients in respiratory failure or during surgery.
-
Oxygen Therapy Equipment: Devices that provide supplemental oxygen to patients who have low blood oxygen levels. This category includes oxygen concentrators (machines that extract and concentrate oxygen from room air) and oxygen cylinders/tanks (containers of compressed oxygen). These supplies are used for conditions like chronic obstructive pulmonary disease (COPD), pulmonary fibrosis, or other lung disorders where extra oxygen is needed. The oxygen is delivered to the patient through nasal cannulas or oxygen masks.
-
CPAP and BiPAP Machines: These are Positive Airway Pressure devices used mainly to treat sleep apnea and other conditions that cause breathing difficulty during sleep. CPAP (Continuous Positive Airway Pressure) provides a steady, continuous stream of pressurized air to keep the airways open, while BiPAP (Bilevel Positive Airway Pressure) provides two levels of pressure (a higher pressure when inhaling and lower when exhaling. Both devices require masks and tubing to connect to the user and maintain airflow throughout the night.
-
Nebulizers and Inhalers: Devices for delivering respiratory medication in the form of an aerosol or mist that can be inhaled into the lungs. A nebulizer is a machine that turns liquid medicine (like bronchodilators or steroids) into a fine mist for inhalation, often used by people with asthma or other lung diseases. Inhalers, such as metered-dose inhalers or dry powder inhalers, are handheld devices that deliver a specific dose of medication (like albuterol for asthma) directly to the airways. Both nebulizers and inhalers help in opening airways and reducing inflammation to improve breathing.
-
Masks, Tubing, and Other Accessories: These are the components that connect patients to the above devices and ensure effective delivery of air or medication. Examples include oxygen masks, nasal cannulas (small tubes for the nostrils), CPAP/BiPAP masks (which can cover the nose, or nose and mouth), and various tubing and filters. Such accessories are considered part of respiratory supplies because they are necessary for using ventilators, oxygen systems, CPAP machines, and nebulizers safely and hygienically. Many of these items are disposable or require regular replacement to maintain cleanliness and function.
Who Uses Respiratory Supplies?
People with a variety of respiratory conditions or needs rely on these supplies. For example, individuals with sleep apnea, COPD, asthma, or other chronic lung diseases often use respiratory equipment at home to breathe easier and maintain their oxygen levels. In acute care, patients suffering from pneumonia, COVID-19, or other forms of respiratory failure may need ventilators or high-flow oxygen devices in the hospital. Even in emergency situations, manual resuscitator bags (a type of respiratory supply) are used by first responders to assist with breathing. In summary, respiratory supplies include a range of devices and supportive tools – from ventilators, oxygen and medication delivery systems to masks and tubing – all aimed at helping patients breathe effectively and maintain healthy oxygen levels.
Common Types of Respiratory Supplies
-
Ventilators: Mechanical breathing machines that move air in and out of the lungs for a patient. Ventilators can fully or partially take over the work of breathing for someone who is unable to breathe adequately on their own. They are commonly used in critical care settings (and sometimes for home care) to deliver life-sustaining breaths to patients in respiratory failure or during surgery.
-
Oxygen Therapy Equipment: Devices that provide supplemental oxygen to patients who have low blood oxygen levels. This category includes oxygen concentrators (machines that extract and concentrate oxygen from room air) and oxygen cylinders/tanks (containers of compressed oxygen). These supplies are used for conditions like chronic obstructive pulmonary disease (COPD), pulmonary fibrosis, or other lung disorders where extra oxygen is needed. The oxygen is delivered to the patient through nasal cannulas or oxygen masks.
-
CPAP and BiPAP Machines: These are Positive Airway Pressure devices used mainly to treat sleep apnea and other conditions that cause breathing difficulty during sleep. CPAP (Continuous Positive Airway Pressure) provides a steady, continuous stream of pressurized air to keep the airways open, while BiPAP (Bilevel Positive Airway Pressure) provides two levels of pressure (a higher pressure when inhaling and lower when exhaling. Both devices require masks and tubing to connect to the user and maintain airflow throughout the night.
-
Nebulizers and Inhalers: Devices for delivering respiratory medication in the form of an aerosol or mist that can be inhaled into the lungs. A nebulizer is a machine that turns liquid medicine (like bronchodilators or steroids) into a fine mist for inhalation, often used by people with asthma or other lung diseases. Inhalers, such as metered-dose inhalers or dry powder inhalers, are handheld devices that deliver a specific dose of medication (like albuterol for asthma) directly to the airways. Both nebulizers and inhalers help in opening airways and reducing inflammation to improve breathing.
-
Masks, Tubing, and Other Accessories: These are the components that connect patients to the above devices and ensure effective delivery of air or medication. Examples include oxygen masks, nasal cannulas (small tubes for the nostrils), CPAP/BiPAP masks (which can cover the nose, or nose and mouth), and various tubing and filters. Such accessories are considered part of respiratory supplies because they are necessary for using ventilators, oxygen systems, CPAP machines, and nebulizers safely and hygienically. Many of these items are disposable or require regular replacement to maintain cleanliness and function.
Who Uses Respiratory Supplies?
People with a variety of respiratory conditions or needs rely on these supplies. For example, individuals with sleep apnea, COPD, asthma, or other chronic lung diseases often use respiratory equipment at home to breathe easier and maintain their oxygen levels. In acute care, patients suffering from pneumonia, COVID-19, or other forms of respiratory failure may need ventilators or high-flow oxygen devices in the hospital. Even in emergency situations, manual resuscitator bags (a type of respiratory supply) are used by first responders to assist with breathing. In summary, respiratory supplies include a range of devices and supportive tools – from ventilators, oxygen and medication delivery systems to masks and tubing – all aimed at helping patients breathe effectively and maintain healthy oxygen levels.
















































